Clinical Medical
Reviews and Case Reports
Lymphoma or Pseudolymphoma, that is the Question
Yasar Albushra Ahmed1* and Mohamed Fatani2
1Medical oncology Department, Sligo Regional Hospital, Ireland
2Internal Medicine Resident, King Faisal Specialist Hospital & Research center, Saudi Arabia
*Corresponding author: Yasar Albushra Ahmed, Sligo Regional Hospital, The Mall, Sligo, Ireland, Tel: +3531022059, E-mail: drhammor@gmail.com
Clin Med Rev Case Rep, CMRCR-2-035, (Volume 2, Issue 6), Case Report; ISSN: 2378-3656
Received: April 19, 2015 | Accepted: June 20, 2015 | Published: June 23, 2015
Citation: Ahmed YA, Fatani M (2015) Lymphoma or Pseudolymphoma, that is the Question. Clin Med Rev Case Rep 2:035. 10.23937/2378-3656/1410035
Copyright: © 2015 Ahmed YA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Drug-induced pseudolymphoma syndrome refers to a benign, drug-induced lymphocytic infiltrate in the skin that mimics malignant lymphoma histologically, clinically, or both. At times, exposure to medication may result in cutaneous inflammatory patterns that resemble lymphoma. These pseudolymphomatous drug eruptions may resemble either T-cell or B-cell lymphomas.
Introduction
We describe the case of a 15-year-old man with history of resected astrocytoma and seizure disorder. The patient presented with pyrexia of unknown origin, lymphadenopathy and generalized pruritic and confluent maculopapular eruption. His history of lymphadenopathy and skin lesions was concordant with medication and resolved after discontinuation. However, microscopic examination and immunohistochemical was suggestive of T-cell lymphoma (diffuse proliferation of large lymphoid cells). But clonal population of T-cells could not be detected in a pathologic specimen obtained from an excisional biopsy of one of the patient's cervical lymph nodes, such finding argues against lymphoma. This experience demonstrates that combining clinical history, histological and immunohistochemical findings is crucial for a definite diagnosis of pseudolymphoma syndrome.
Case Report
A 15-year-old man, a sufferer of seizure disorder secondary to resected astrorocytoma, received regular medical attention (Phenytoin and Valproic acid) in a tertiary hospital center in western Saudi Arabia. Due to an episode of fever, night sweats, and Odynophagia, he was admitted to the hospital.
On admission, her vital signs were a blood pressure of 110/70mmHg, heart rate of 78 beats/min, respiratory rate of 18 breaths/ min, and body temperature of 38.8�C.
A physical examination conducted at presentation revealed multiple, firm, tender cervical lymph nodes mainly on the right side and measured 1.5cm to 1.0cm in diameter.
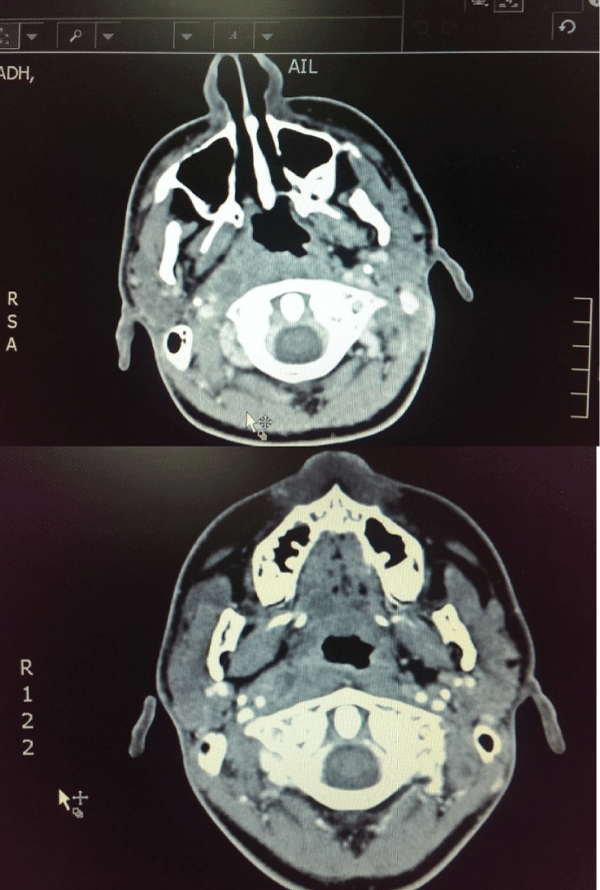
Laboratory tests results were as follows: initially normal blood count, renal and liver function tests. C-reactive protein (CRP) was 164mg/dl (0-10mg/dL). Blood urine and throat Culture came back negative. Chest x-ray and Brain Computed tomography (CT) were unremarkable. CT neck, chest, abdomen and pelvis showed right-sided parapharyngeal abscess (Figure 1).
.
Figure 1: Contrast-enhanced CT scan of the neck demonstrating a right-sided parapharyngeal abscess anterior to the right carotid artery measuring 1.3cm x 1.5cm with elongated retropharyngeal abscess extension measuring 9cm cranio-caudally and 6 mm in thickness
View Figure 1
Empiric intravenous antibiotics was started without improvement so incision and drainage were done and there was no abscess found but only necrotic tissue and necrotic cervical lymph node so biopsy was taken and sent for histopathology. The fever continued despite good coverage of antibiotics. An extension workup was carried out including viral serology for Epstein-Barr virus (EBV), Cytomegalovirus (CMV), hepatitis, Human Immunodeficiency Virus (HIV), herpes and dengue fever. Toxoplasmosis, malaria, brucella, additional bacterial and fungal blood cultures and screening for autoimmune diseases and immunodeficiency, drug levels for acetaminophen, phenytoinand valproic acid were also done and all these came back normal.
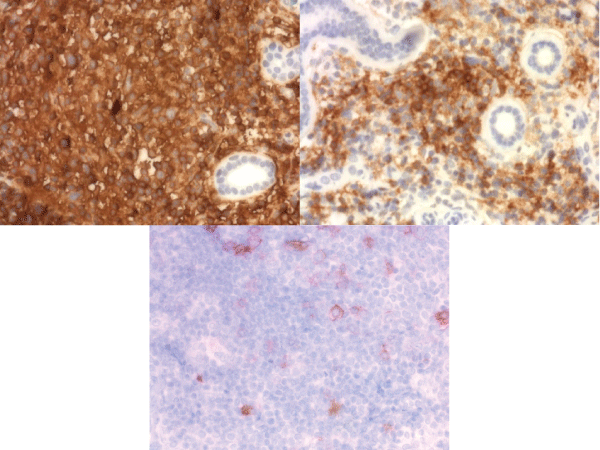
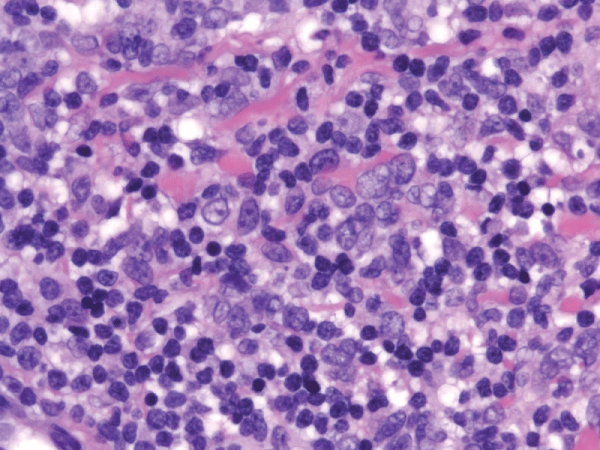
The Histopathological assessment of the cervical lymph node was highly suggestive of lymphoma. It showed diffuse proliferation of various size atypical lymphocytes (Figure 2). The immunophenotype show an exclusive T-Cell population of the infiltrate with the B cells limited to the follicles. The large atypical lymphocytes are positive for CD45, CD3, CD5, CD2, CD4 and CD8. CD7 is diminished. Also, positive for CD30 and Granzyme B. CD56 is focally positive. Alk-1 is negative. The large atypical cells are negative for CD20, PAX-5 and CD21.
.
Figure 2: from the right cervical lymph node demonstrating effaced nodal architecture with paracortical Section expansion of atypical lymphoid infiltrate ranging from small to large cells. The infiltrate extends to the medullary region of the lymph node. The atypical infiltrate composed of small, medium and large lymphocytes (HE, 100x)
View Figure 2
During hospitalization he developed confluent maculopapular eruptions with pruritus on the trunk and all four limbs in addition to hepatosplenomegaly. Hepatic function panel revealed an elevated aspartate aminotransferase of 220U/L (8-48U/L)and increased alkaline phosphatase levels of 426U/L (45-115U/L) and high International Normalized Ratio (INR) of 1.6 (0.8 to 1.2).
The patient was started on IV hydrocortisone after which the fever and rash started to resolve. Phenytoin and valproic were stopped and he was started on keppra as anticonvulsat.
For a definitive diagnosis, a molecular study on the rearrangement of the T-cell receptor (TCR)-gamma gene was performed and showed polyclonality. The T-cell receptor gene rearrangement clonality study and the EBV in-situ hybridization were negative (Figure 3).
He was monitored for signs of clinical recovery. Two days later his fever subsides. Rash, hepatosplenomegally and transaminitis had substantially resolved in day 7. Based on the patient's history of lymphadenopathy, phenytoin exposure, and inability to demonstrate a clonal population of T cells in the affected lymph node, a diagnosis of phenytoin-induced pseudolymphoma syndrome was rendered and phenytoin was identified as the offending drug. The steroid was discontinued after 2 weeks of treatment. No recurrence of symptoms occurred in the 3-month follow-up period.
Discussion
Lymphadenopathy in association with the use of hydantoin derivatives such as phenytoin was first described in 1940. Pseudolymphoma is a rare but interesting phenomenon because of its diagnostic and therapeutic implications. It consists of a triad of fever, generalized rash and lymphadenopathy.
The minimum clinical criteria for the diagnosis include: (i) Exposure to drugs as stated earlier; (ii) Triad of fever, generalized rash and lymphadenopathy; and (iii) Improvement on stopping the offending drug [1-3]. Clinical features of drug-induced pseudolymphomas are not well known but generally may include generalized skin eruption, lymphadenopathy fever, arthralgia hepatosplenomegaly, eosinophilia and transaminitis [3-6].
Phenytoin is said to be the commonest drug causing this syndrome. It occurs in about 1% of patients receiving the drug. Other drugs known to cause this syndrome are Carbamazepine, mephytoin, trimethadone, mexiletine (antiarrhythmics), thioridazine and butabarbital [6].
In contrast to classic drug eruptions, which develop minutes to days from drug ingestion and quickly resolve with drug discontinuation, the time course of drug-induced pseudolymphoma syndrome is prolonged and suggests a distinct biologic mechanism. Some postulate that drug-induced immune-dysregulation results in the lymphoproliferative process [7]. Abnormally functioning lymphocytes may proliferate in response to an antigen from the drug itself, an antigen unmasked by drug metabolism, or another non pharmacologic antigen. Supporting this theory, alterations in immune function have been demonstrated in vivo or in vitro for many of the causative agents [3].
Usually, drug-induced pseudolymphoma is a T-cell proliferation, but occasional B-cell-predominant forms have been reported. In general, evidence of T- or B-cell clonality (by polymerase chain reaction analysis of T-cell receptor or immunoglobulin H gene rearrangement or immunohistochemical light chain analysis) supports true lymphoma, whereas polyclonality supports a pseudolymphomatous proliferation [1].
The emerging consensus is that pseudolymphomatous and lymphomatous proliferations represent 2 ends of a spectrum [1,2]. Supporting this theory are examples of antigen-driven lymphoproliferation and progression to lymphoma in other organ systems (i.e., Helicobacter pylori -related gastric mucosa-associated lymphoid tissue [MALT] lymphoma). Transformation of drug-induced cutaneous lymphocytic infiltrates to malignant lymphoma has been reported with phenytoin; however, many of these cases predate the availability of current diagnostic standards and may have represented cases that would now be classified as hypersensitivity syndrome [8,9].
Generally there are no hematological or biochemical abnormalities. Transaminitis has been reported; however, it confers a worse prognosis, with one study reporting 10-50% mortality with severe hepatitis [10]. Immunohistochemical stains are usually required to facilitate differentiation between pseudolymphomatous eruptions and lymphoma. In drug induced pseudolymphoma they confirm a polymorphic infiltrate including CD3-positive T lymphocytes, CD20-positive B lymphocytes and CD68-positive histiocytes.
Molecular biology and chromosome studies have become the definitive basis differentiating pseudolymphoma from malignant lymphoma in patients receiving chronic Phenytoin therapy [11].
Discontinuation of the offending drug is the most important therapeutic step. It is unclear whether steroids can significantly alter the disease process, although they are widely used in the acute phase of disease. Symptomatic therapies for fever with antipyretics should be prescribed with caution to avoid aggravating liver toxicity. Topical steroids and antihistamines could be prescribed for cutaneous rash and pruritus [9-11].
Conclusion
In conclusion, it has been a known fact that Phenytoin poses wide range of clinical syndromes. Phenytoin induced psedulymphoma is a unique phenomenon that mimic lymphoma clinically. In some cases of, the possibility of lymphoma cannot be excluded by histologic analysis and immunostaining. In such cases, analysis for immunoglobulin or T-cell receptor gene rearrangements may provide additional helpful information.
Our experience of this case cautions physicians that lymph node biopsy results suggestive of lymphoma in the situation of drug-induced pseudolymphoma should be an interpretation of the biopsy before deciding on the optimal treatment.
References
-
Albrecht J, Fine LA, Piette W (2007) Drug-associated lymphoma and pseudolymphoma: recognition and management. Dermatol Clin 25: 233-244
-
Magro CM, Crowson AN (1996) Drug-induced immune dysregulation as a cause of atypical cutaneous lymphoid infiltrates: a hypothesis. Hum Pathol 27: 125-132.
-
Magro CM, Crowson AN, Kovatich AJ, Burns F (2003) Drug-induced reversible lymphoid dyscrasia: a clonal lymphomatoid dermatitis of memory and activated T cells. Hum Pathol 34: 119-129
-
Sueki H, Sasaki M, Kamiyama T, Ohtoshi S, Watanabe H, et al. (2014) Drug-induced hypersensitivity syndrome/drug reaction with eosinophilia and systemic symptoms with histologic features mimicking cutaneous pseudolymphoma. J Dermatol 41: 856-857.
-
Ahronowitz I, Fox L (2014) Severe drug-induced dermatoses. Semin Cutan Med Surg 33: 49-58.
-
Breathnach SM (1992) Drug reaction. In: Champion RH, Burton JL, Ebling FJG (ed) Textbook of Dermatology. (5th edn), Oxford, Blackwell Scientific Publication 2961-3035
-
Ploysangam T, Breneman DL, Mutasim DF (1998) Cutaneous pseudolymphomas.J Am Acad Dermatol 38: 877-895.
-
Welsh JP, Ko C, Hsu WT (2008) Lymphomatoid drug reaction secondary to methylphenidate hydrochloride. Cutis 81: 61-64.
-
Camilot D, Arnez ZM, Luzar B, Pizem J, Zgavec B, Falconieri G (2011)Cutaneous Pseudolymphoma Following Tattoo Application: Report of Two New Cases of a Potential Lymphoma Mimicker.Int J Surg Pathol 20: 311-315
-
Choi TS, Doh KS, Kim SH, Jang MS, Suh KS, Kim ST (2003) Clinicopathological and genotypic aspects of anticonvulsant-induced pseudolymphoma syndrome. Br J Dermatol 148: 730-736.
-
Zhang B, Beck AH, Taube JM, Kohler S, Seo K, et al. (2010) Combined use of PCR-based TCRG and TCRB clonality tests on paraffin-embedded skin tissue in the differential diagnosis of mycosis fungoides and inflammatory dermatoses. J Mol Diagn 12: 320.