Clinical Medical
Reviews and Case Reports
Descending Necrotizing Mediastinitis due to the Third Branchial Sinus: A Case Report
Jiang Xiuwen, Shao Jinyan, Hou Tiening, He Lina and Tang Jianguo*
Department of Otolaryngology-Head and Neck Surgery, Sir Run Run Shaw Hospital, Medical College of Zhejiang University, China
*Corresponding author: Tang Jianguo, Department of Otolaryngology-Head and Neck Surgery, Sir Run Run Shaw Hospital, Medical College of Zhejiang University, Hangzhou 310016, China, E-mail: jgtang_srrsh@163.com
Clin Med Rev Case Rep, CMRCR-2-037, (Volume 2, Issue 6), Case Report; ISSN: 2378-3656
Received: April 06, 2015 | Accepted: June 22, 2015 | Published: June 25, 2015
Citation: Xiuwen J, Jinyan S, Tiening H, Lina H, Jianguo T (2015) Descending Necrotizing Mediastinitis due to the Third Branchial Sinus: A Case Report. Clin Med Rev Case Rep 2:037. 10.23937/2378-3656/1410037
Copyright: © 2015 Xiuwen J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Descending Necrotizing Mediastinitis (DNM) is uncommon infection of mediastinum arising from neck or oral cavity. Despite improvements in diagnostic imaging and treatment, its mortality rate remains relatively high. We describe a unique case of descending necrotizing mediastinitis secondary to the third branchial sinus. The patient was successfully treated with antibiotics and transcervical surgical drainage. The tract was removed in second staged procedure after that descending necrotizing mediastinitis was cured.
Keywords
Descending necrotizing mediastinitis, Branchial sinus
Introduction
As a rare form of mediastinitis, Descending Necrotizing Mediastinitis (DNM) is a highly lethal complication of cervical or oral cavity infection that spreads into the mediastinum through cervical spaces and the mortality rate is reported as high as 40% [1]. The third branchial sinus is rare and usually presents as a lateral neck mass, or abscess. We report a unique case of a 34-year-old man with DNM that originating from a neck abscess caused by the third branchial sinus.
Case Report
A 34-year-old man who had been suffering from odynophagia and moderate fever for one week was admitted to the emergency department of our hospital. He was diagnosed as having acute pharyngitis and treated with antibiotics at a local hospital. His condition was aggravated by dysphagia and backache that transpired for four days; thus, the patient was transferred to our hospital. Upon admission, the physical examination showed the following vital signs: blood pressure, 124/75mmHg; temperature, 38.6℃; heart rate, 101 beats per minute; and respiratory rate, 20 breaths per minute. No palpable neck mass or stiffness was observed. Fibro-laryngoscopy was performed, which revealed infra-pharyngeal congestion and ischesis of the bilateral pyriform fossa. No dental infection was found. Laboratory studies showed that peripheral white blood cell count was 17,900/mm3 (91.5% polymorphonuclear leukocytes), and erythrocyte sedimentation rate was 64mm/hr (range, M, 1-15mm/hr). The chest X-ray did not show any significant alterations. Radiography with esophageal barium swallow was performed, and the sinus tract of the left pyriform fossa was demonstrated (Figure 1). The contrast-enhanced Computed Tomography (CT) scan of the neck and thorax showed an extensive mediastinum abscess with air collection in the neck (Figures 2A,2B). Thus, the patient was diagnosed with DNM secondary to the third branchial sinus infection.
.
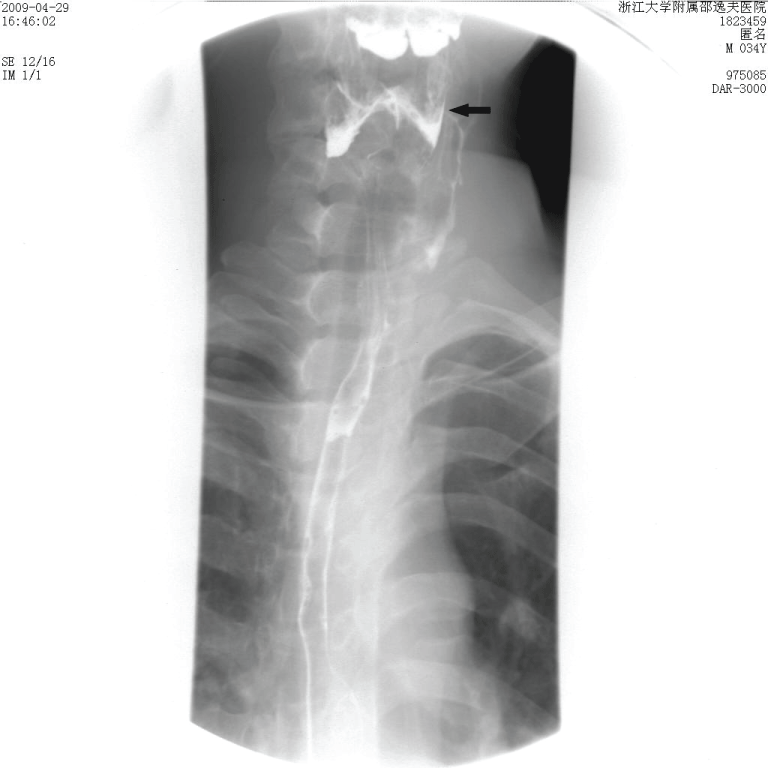
Figure 1: Barium esophagography shows a sinus tract (arrow) that originates from the cephalad of the left pyriform fossa.
View Figure 1
.
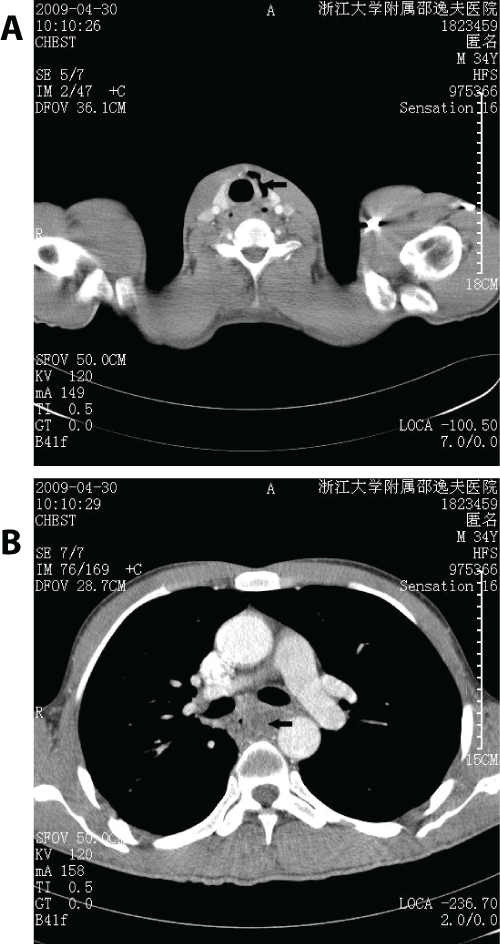
Figure 2: Contrast-enhanced CT scan of the chest and neck reveals a septic process with abundant air collection (arrow) at the left side of the neck (A) with extension (arrow) at the posterior mediastinum (B).
View Figure 2
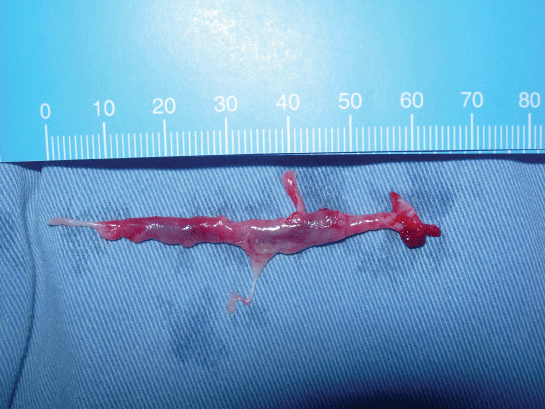
Drainage of the neck and mediastinum was performed with an incision along the anterior edge of the left sternocleidomastoid muscle. Abundant pus flowed out from the vomica of the neck and mediastinum. The vomica, about 33cm in length, was near the trachea. It was about 12cm in length from the left clavicular head to the top of the vomica, and about 21cm in length to the bottom. Meanwhile, esophagoscopy was performed and a tract opening was found at the cephalad posterolateral wall of the left pyriform fossa, with purulent secretions overflowing. The vomica was washed repeatedly and drainage tubes were inserted into the cavities. We used one negative pressure drainage tube for the neck and another negative pressure drainage tube with one washing pipe in the mediastinum. The patient was transferred to the ICU after surgery. Irrigation and drainage of the mediastinum were conducted daily. Cultures of purulent secretions yielded no organisms. Empiric antibiotic therapy consisting of panipenemetamipron 0.5g q 8h, vancomycin 1.0g q 12h, and tinidazole 0.8g once daily was administered. On the first post-operative day, the temperature fell to normal (36.7℃) and peripheral white blood cell count was 10.2*109/L (86.5% polymorphonuclear leukocytes). The patient's clinical conditions steadily improved. On the third post-operative day, the CT scan of the thorax showed an obvious reduction of the mediastinum abscess. The patient was then transferred to the general ward (Figure 3). On the 13th post-operative day, the CT scan of the thorax showed that the mediastinum abscess had disappeared; thus, the drainage tubes were removed. A week later, cervical sinus resection was performed. During the surgical dissection of the tract, we found the tract passing through the inferior constrictor into the pyriform fossa, superior to the superior laryngeal nerve traveling laterally to the recurrent laryngeal nerve. The tract was resected in a retrograde fashion and ligated at the pyriform fossa (Figure 4). Histopathologic examination showed that the tract covered with squamous epithelial lining confirms the diagnosis of branchial anomaly. The patient was discharged on day 35. A 36-month follow up showed no late complications or recurrence.
.
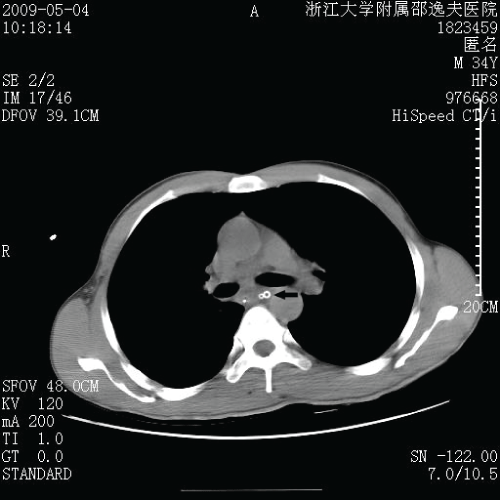
Figure 3: Thoracic computed tomographic scan demonstrates that posterior mediastinal pus is decreased obviously on the 3rd day after drainage operation. A nasogastric feeding tube and mediastinal drains (drainage tube and wash tube) (arrow) are also identified.
View Figure 3
Discussion
DNM mainly involves adults around the fourth or fifth decade but can affect all age groups including children [1,2]. There is also a marked male predominance in DNM [2,3]. Branchial sinus of the pyriform fossa refers to a persistent embryologic third or fourth pharyngeal pouch, which typically presents as a congenital sinus tract that originates from the pyriform fossa. The tract of the third branchial sinus passes deep into the platysma, ascending along the common carotid sheath, and passing behind the common and internal carotid artery. The tract crosses the hypoglossal nerve, but does not ascend above the glossopharyngeal nerve or the stylopharyngeus muscle, and is superficial to the superior laryngeal nerve [4]. The internal opening is in the pyriform fossa. The fourth branchial sinus also originates from the pyriform fossa, but follows a path inferior to the superior laryngeal nerve. Although the pathways of these sinuses are widely referred to in literature, case reports matching these descriptions are rare [5]. James retrospectively analyzed 17 cases of third and fourth branchial anomalies; however, no lesions following the classical course of either the third or fourth branchial anomaly were identified [6]. An alternative embryologic process was proposed to better fit the presentation of these lesions; this approach is based on the supposition that these tracts represent an embryologic derivation of the thymopharyngeal duct, which is formed as the thymus descends during fetal development [7]. The origin of the third branchial pouch sinus is the persistence of the thymopharyngeal canal. The tract never loops around the hypoglossal nerve or carotid arteries and never descends into the mediastinum [3]. During surgical dissection of this tract, we found that the tract passed through the inferior constrictor into the cephalad posterolateral wall of the left pyriform fossa, superior to the superior laryngeal nerve traveling laterally to the recurrent laryngeal nerve. The tract was relative to neither the hypoglossal nerve nor the carotid arteries. It was resected in a retrograde fashion, and ligated at the left pyriform fossa.
The patient had been misdiagnosed with acute pharyngitis before admission. The dysphagia and backache indicated the need to perform radiography with esophageal barium swallow. The fistula of the left pyriform fossa suggested the occurrence of a special disease. The CT scan of the neck and thorax showed a left cervical abscess and a severe abscess in the mediastinum. Imaging and surgical findings confirmed a final diagnosis of DNM secondary to the third branchial sinus infection.
The sensitivity of barium-swallow imaging is as high as 80% in diagnosing a branchial sinus of the pyriform fossa [8]. Furthermore, ultrasonography can show the presence of gas within the area, which is pathognomonic for a pyriform fossa fistula. In difficult cases, both CT and MR studies are advocated, but CT is the preferred method. A chest CT scan is known to be the best tool for the diagnosis of DNM [9]. In our case, the barium esophagography showed a sinus tract that originates from the cephalad of left pyriform fossa. Falcone M reported a patient with DNM and a fistula in the hypopharynx, which was formed as the result of the neck infection and contributed to the successful outcome of the patient [10]. However, why did we consider it as a congenital orificium fistula? The esophagoscopy revealed that the location of orificium fistula was coincident with the third branchial sinus; meanwhile the surrounding mucosa of the hole was intact and not swelling. The surgical findings and the histopathologic examination confirmed the presence of the third branchial sinus. So, we suggest that the congenital disease should not be forgotten if the primary lesion is difficult to be found for DNM.
The standard treatment for DNM consists of surgical drainage combined with the administration of antibiotics. However, the optimal surgical approach remains controversial. Four standard surgical approaches to mediastinal drainage have been described: (1) Transcervical, (2) Standard posterolateral thoracotomy, (3) Median sternotomy and (4) Transthoracic via the subxiphoid [11]. Estrera et al. recommended transthoracic surgery for any infection extending below the T4 plane (at the tracheal bifurcation) because mediastinitis below this level tends to lead to pleural empyema [12]. In the present study, the abscess extended mainly at the upper mediastinum and posterior mediastinum. The vomica was large and required drainage; thus, the patient was treated with transcervical drainage of the cervical and mediastinal abscess. The condition was improved promptly on the first post-operative day, and the abscess was clearly reduced by the third post-operative day.
In managing the third branchial sinus, James recommended that surgical excision involve ipsilateral thyroidectomy as the lesion passes through the thyroid gland [6]. Honzumi et al. reported that high ligation of the fistula and its complete excision without thyroid lobectomy would suffice [13]. We found no relationship between the lesion and thyroid gland; thus, the thyroid was kept intact.
In conclusion, we have described a unique case of DNM secondary to the third branchial sinus infection. Odontogenic infection is the most common cause of DNM. Other infrequent causes are peritonsillar and retropharyngeal abscesses, cervical trauma, epiglottitis, sinusitis, and lymphadenitis of the neck. Nonetheless, congenital branchial anomalies should not be disregarded, even if the patient has no history of recurrent cervical masses. We should maintain a high index of suspicion for this disease when treating patients with odynophagia and backache.
References
-
Wheatley MJ, Stirling MC, Kirsh MM, Gago O, Orringer MB (1990) Descending necrotizing mediastinitis: transcervical drainage is not enough. Ann Thorac Surg 49: 780-784.
-
Ridder GJ, Maier W, Kinzer S, Teszler CB, Boedeker CC, et al. (2010) Descending necrotizing mediastinitis: contemporary trends in etiology, diagnosis, management, and outcome. Ann Surg 251: 528-534.
-
Marty-Ane CH, Berthet JP, Alric P, Pegis JD, Rouvière P, et al. (1999) Management of descending necrotizing mediastinitis: an aggressive treatment for an aggressive disease. Ann Thorac Surg 68: 212-217.
-
Godin MS, Kearns DB, Pransky SM, Seid AB, Wilson DB (1990) Fourth branchial pouch sinus: principles of diagnosis and management. Laryngoscope 100: 174-178.
-
Miyauchi A, Matsuzaka F, Takai S, Kuma K, Kosaki G (1981) Pyriform sinus fistula: a route of infection in acute suppurative thyroiditis. Arch Surg 116: 66-69.
-
James A, Stewart C, Warrick P, Tzifa C, Forte V (2007) Branchial sinus of the pyriform fossa: reappraisal of third and fourth branchial anomalies. Laryngoscope 117: 1920-1924.
-
Ford GR, Balakrishnan A, Evans JN, Bailey CM (1992) Branchial cleft and pouch anomalies. J Laryngol Otol 106: 137-143.
-
Bar-Ziv J (1996) Pyogenic thyroiditis in children due to a fourth branchial pouch fistula. Pediatr Radiol 26: 88-90.
-
Makeieff M, Gresillon N, Berthet JP, Garrel R, Crampette L, et al. (2004) Management of descending necrotizing mediastinitis. Laryngoscope 114: 772-775.
-
Falcone M, Pompeo ME, Pavoni GL, Fusconi M, Soldo P, et al. (2005) Successful conservative treatment of descending necrotizing mediastinitis with fistula formation in the hypopharynx. Infectious Diseases in Clinical Practice 13: 36-38.
-
Mihos P, Potaris K, Gakidis I, Papadakis D, Rallis G (2004) Management of descending necrotizing mediastinitis. J Oral Maxillofac Surg 62: 966-972.
-
Estrera AS, Landay MJ, Grisham JM, Sinn DP, Platt MR (1983) Descending necrotizing mediastinitis. Surg Gynecol Obstet 157: 545-552.
-
Honzumi M, Suzuki H, Tsukamoto Y (1993) Surgical resection for pyriform sinus fistula. J Pediatr Surg 28: 877-879.