International Journal of Anesthetics and Anesthesiology
Need of Ultrasound in Emergency Department for Suprapubic Catheterization
Prerana N. Shah* , Vaishali P Chaskar, Pradeep Rathod, Anand Komawar and Barakha Gadpale
Department of Anaesthesiology, GSMC & KEMH, India
*Corresponding author: Prerana N. Shah, Professor, Department of Anaesthesiology, Seth GSMC & KEMH, Mumbai 400012, Maharashtra, India, Tel: 09869117027, E-mail: pps@kem.edu
Int J Anesthetic Anesthesiol, IJAA-1-014, (Volume 1, Issue 3), Case Report; ISSN: 2377-4630
Received: September 12, 2014 | Accepted: November 16, 2014 | Published: November 20, 2014
Citation: Shah PN, Chaskar VP, Rathod P, Komawar A, Gadpale B (2014) Need of Ultrasound in Emergency Department for Suprapubic Catheterization. Int J Anesthetic Anesthesiol 1:014. 10.23937/2377-4630/1/3/1014
Copyright: © 2014 Shah PN, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Acute retention of urine is a medical emergency which needs immediate intervention. Urethral catheterization is a common procedure in the emergency department. Repeated unsuccessful attempts for urethral catheterization demand alternative procedure like suprapubic catheterization.
Traditionlly, anatomical landmarks are used to achieve suprapubic catheterization. The confirmation of successful catheterization by ultrasound is recommended. Often due to its unavailability, complications like bowel injury, bleeding etc are reported.
We report a case of gastric perforation caused by such a blind suprapubic catheter (SPC) insertion procedure.
Key words
Gastric perforation, Suprapubic catheterization, Ultrasound modality.
Introduction
Acute urinary retention is a common medical emergency for which early evaluation and intervention is needed. Quick and proper history and clinical examination helps the emergency physician to diagnose the cause. Sometimes atypical presentation or multifactorial causes confuses the physician for confirmed diagnosis. This ultimately leads to delay in initiating the treatment.
Bedside ultrasound might be helpful for diagnosis and during invasive procedures like internal jugular vein (IJV) cannulation, suprapubic catheterization etc. It gives added advantages of confirmation of catheter tip position and prevention of the complications like bowel injury and bleeding. Our case report explains the need of bedside ultrasound during suprapubic catheterization.
Case Description
We discuss a case report of iatrogenic gastric perforation in a 38 year old man. He was posted for emergency laparotomy due to detected gas under diaphragm on X ray abdomen. The patient was a known chronic alcoholic since 20 years. History of seizures without any medication for the past two years was obtained. History of anuria for two days. In the emergency ward, urethral catheterization was attempted twice. However, as there was no urine in the catheter, it was assumed that uretheral cathererization was faulty or a false tract had been created and urology resident was called for intervention and insertion of supra pubic catheter (SPC). Even after assumed successful insertion of SPC, urine was not seen in the bag. He then underwent radiological investigations that revealed gastric obstruction with Foleys cathter in the stomach.
On examination, he was conscious, awake and well oriented. There was no significant finding on examination of cardiac and respiratory systems. The abdomen was distended. Nasogastric tube and per urethral Foleys catheter were in situ with no urine in bag. Interestingly SPC showed stomach contents. Peripheral and central venous catheters were already inserted earlier. Heart rate was 120 beats per minute and blood pressure was 90/60 mm of Hg. Platelet count was 60,000/cmm. All other laboratory investigations were normal. Ultrasonography report was suggestive of duodenal obstruction with SPC wrongly inserted into stomach. There was moderate amount of free fluid in pelvis suggestive of perforation with collapsed urinary bladder. Same findings were noted on CT abdomen report. Thus the indication of insertion of SPC due to absence of urine after urethral catheterization was wrong as the patient had anuria probably due to obstruction.
An informed written consent was obtained from patient. After confirming the availability of platelets and packed cells, patient was wheeled in the operating room for exploratory laparotomy. All standard monitors like cardio scope, noninvasive blood pressure, pulse oximetry and capnograph were attached. Rapid sequence intubation using fentanyl, propofol and rocuronium was done. After endotracheal intubation, maintenance was provided with isoflurane levels of 0.6-1 MAC, O2 and air in ratio of 50:50. Six units of platelet were transfused during surgery. Intraoperatively, after administration of about 1 litre of fluid, 100 ml urine came through urethral catheter. Hence, failure to get urine via urethral catheter was not due to false tract, but it was because of hypovolaemia.
On laparotomy the stomach was found to be distended with the tip and balloon of Foleys catheter in it. There was no evidence of any injury on posterior wall of stomach or to any other intra abdominal organ. It was diagnosed to be a case of benign gastric outlet obstruction with a hugely distended stomach. Site of narrowing was at junction of third and fourth parts of duodenum. The site of gastric injury was closed primarily and a wide posterior gastojejunostomy was performed. In perioperative period, vitals were stable. Intravenous fluids were given as per requirement. After reversal, patient was extubated. The patient was shifted to the postoperative ward (Figure 1,2).
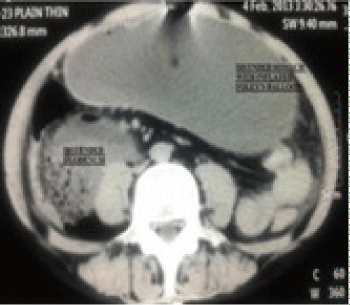
Figure 1: CT abdomen showing distended stomach, duodenum & tip of
catheter seen in stomach along with inflated balloon.
View Figure 1
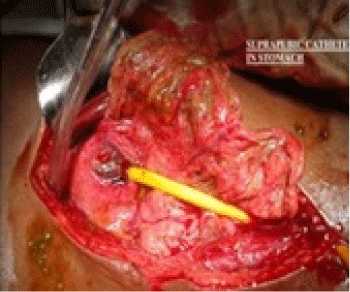
Figure 2: Tip of catheter tip in stomach.
View Figure 2
Discussion
Modern medical technology has given us several advanced monitoring tools. We should apply them for benefit of various types of patients to give appropriate treatment and to minimize iatrogenic complications.
The conventional 'blind' technique for SPC insertion requires distended urinary bladder. This distended bladder and head low position keeps bowel away from needle puncture. Though this is generally considered a safe procedure, the risk of bowel injury is estimated at up to 2.4% with a mortality rate of 1.8%. most of studies in eastern regions showed gastroduodenal perforation constitutes most common cause of peritonitis [1,2]. Incidence of gastric perforation is very low during suprapubic catheterization due to lower puncture site. However, there are few cases showing life threatening bowel injury [3]. The procedure involves insertion of a sharp trocar into the bladder percutaneously, usually by palpation, percussion or cystoscopy for guidance.
In our patient as there were no features suggestive of obstruction, possibility of distension of stomach was not thought of. Portable bedside USG machines help to visualize abdominal organs. Such rare but severe complications can be avoided if the trocar is inserted using sonography [2,4,5]. Retrospectively, in our patient, ultrasound would have been beneficial to diagnose cause of anuria. SPC was not necessary and perforation would not have occurred. Recently published British Association of Urological Surgeons (BAUS) guidelines recommend that ultrasonography (USG) may be helpful to identify bowel loops and recommends its usage whenever possible [6].
We recommend availability and usage of bedside USG in emergency departments. It can also be used for procedures like IJV canulation, suprapubic catheterization and for diagnosis [7].
We conclude that in absence of specialist services like urologist and interventional radiologist, ultrasound should be used in procedures like SPC insertion to minimize complications and improve efficacy of medical services in emergency departments.
References
-
Stokes S, Wu D (2004) Suprapubic bladder catheterization. In: Reichman E, Simon R eds. Emergency Medicine Procedures. New York: McGraw-Hill: 1134-4.
-
Halder SK, Khan I, Mukhopadhyay P, Paira SK (2012) Inadvertent suprapubic gastrostomy: Report of a unique complication of blind percutaneous suprapubic trocar cystostomy. Indian J Urol 28: 445-446.
-
Rees M, Joseph AE (1981) Ultrasound guided suprapubic puncture-a new, simple way of releasing a blocked Foley balloon. Br J Urol 53: 196.
-
WMM Lee, KL Tsui, CW Kam (2005) Trans-abdominal ultrasound-guided suprapubic puncture of a nondeflating Foley catheter balloon. Hong Kong Journal of Emergency Medicine 12: 42-45.
-
Aguilera PA, Choi T, Durham BA (2004) Ultrasound-guided suprapubic cystostomy catheter placement in the emergency department. J Emerg Med 26: 319-321.
-
Jacob P, Rai BP, Todd AW (2012) Suprapubic catheter insertion using an ultrasound-guided technique and literature review. BJU Int 110: 779-784.
-
Robin Guillory, Marc de Moya (2011) Use of ultrasound in the ICU Critcal Care. Luca M Bigatello, Hassan Alam, Ree M Allain, Edward A.Bittner. Handbook of the Massachusetts General Hospital (5th edn). Wolter Kluwer Pvt. Ltd 3: 39-49.





