International Journal of Anesthetics and Anesthesiology
Endotracheal Repair of an Iatrogenic Tracheal Laceration in A 83-Year-Old Critically Ill Woman with Aspiration Pneumonitis and Sepsis
Stefan Welter1* , Danjouma Cheufou1, Thomas Ehmann2, Sandra Kampe3 and Peter Scharmann4
1Department of Thoracic Surgery and Endoscopy, Ruhrlandklinik, West German Lung Centre, University of Duisburg-Essen, Germany
2Department of Visceral and General Surgery, Niederberg Clinic, Germany
3Division of Anaesthesiology, Ruhrlandklinik, West German Lung Centre, University of Duisburg-Essen, Germany
4Institute of Anaesthesiology, Operative Intensive Care Medicine and Pain Therapy, Niederberg Clinic, Germany
*Corresponding author: Stefan Welter, Department of Thoracic Surgery and Endoscopy, Ruhrlandklinik, Tuschener Weg 40, 45239 Essen, Germany, Tel: 492014334012, Fax: 492014334019,
E-mail: Stefan.welter@ruhrlandklinik.uk-essen.de
Int J Anesthetic Anesthesiol, IJAA-1-015, (Volume 1, Issue 3), Case Report; ISSN: 2377-4630
Received: November 01, 2014 | Accepted: November 20, 2014 | Published: November 24, 2014
Citation: Welter S, Cheufou D, Ehmann T, Kampe S, Scharmann P (2014) Endotracheal Repair of an Iatrogenic Tracheal Laceration in A 83-Year-Old Critically Ill Woman with Aspiration Pneumonitis and Sepsis .Int J Anesthetic Anesthesiol 1:015. 10.23937/2377-4630/1/3/1015
Copyright: © 2014 Welter S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Tracheal laceration is a rare complication of emergency intubation. The treatment decision depends on severity of accompanying problems, available resources, condition and perspectives of the patient and experience of the responsible intensivist and surgeon. The life saving application of endotracheal suture in a disastrous situation is demonstrated in this report. We present the case of a 83-year-old woman who presented with an acute abdomen and septicaemia. A heavy aspiration occured during insertion of a central venous line. The emergency intubation led to a 6 cm rupture of the posterior tracheal wall with a consecutive mediastinal and subcutaneous emphysema. During the Hartmann's operation intermittent tube obstruction caused critically impaired ventilation. The tracheal suture was performed in manifest septicaemia and later allowed regular ventilation, extubation, tracheostomy and weaning. The rupture healed primarily. We think that endotracheal suture of iatrogenic lacerations is a valuable treatment option, even in very difficult situations.
Introduction
Treatment of full thickness iatrogenic tracheal membrane laceration (TML) is a matter of current debate. Some authors favour conservative treatment based on the suspected increased risk of open tracheal repair [1]. To date, there are only case reports and small retrospective series of 10 to 40 cases published [2-4]. It is very difficult to compare treatment results because every case is unique, with regard to the length and depth of the rupture, circumstance and mechanism of the injury, severity of mediastinal emphysema, pneumothorax and the available options to maintain adequate ventilation and the condition of the patient. We recently described the endotracheal running suture as a new method to repair posterior wall injuries without the morbidity of a separate surgical incision [5]. The endotracheal running suture of a longitudinal full thickness laceration of the posterior tracheal membrane is atraumatic. This case report shall demonstrate that endotracheal repair can be applied even in the most critical situations with aspiration and sepsis to avoid further troubles with tube dislocation, mediastinal emphysema or long-term instability of the trachea.
Methods
We describe the successful closure of a 6cm full thickness TML with an endotracheal running suture in an 83-year-old obese woman (BMI 35 kg/m2) in a life-threatening critical situation. She had a massive mediastinal emphysema and repeated obstruction of the endotracheal tube due to dislocation of the tube tip into the mediastinum. She was admitted to a neighbouring hospital with severe dyspnoea and abdominal pain. Further investigations revealed the beginning of multiorgan failure with an acute abdomen. She was then admitted to the ICU. During the insertion of a central venous line, massive vomiting and aspiration occurred resulting in severe hypoxaemia. Emergency intubation was performed with bronchoscopy and bronchial clearance. After stabilizing the septic patient (HR 120, catecholamine-dependent circulatory depression, leukocytosis 25.000/nl, E. coli revealed in the first blood culture) the following laparotomy revealed a small bowel obstruction caused by a severe inflammatory tumour consisting of ileum and a ruptured sigmoid tumour. The operation included a small bowel segmental resection and a Hartman`s procedure to remove the sigmoid colon. The final pathology showed a sigmoid cancer pT4, pN1, RO, G2.
Immediately after the emergency intubation, a severe mediastinal and subcutaneous emphysema appeared and a tracheal laceration was diagnosed by bronchoscopy. The tube was placed distally of the lesion but could not prevent further progression of subcutaneous emphysema. Catecholamines and broad spectrum antibiotics were started. Based on repeated tube dislocations and difficulties to maintain adequate oxygenation, the decision was taken to repair the trachea. Nine hours after intubation and 4 hours after laparotomy, this woman was transferred to our hospital while intubated, with catecholamines and blurry infiltrates in both lungs seen on the chest X-ray (Figure 1a). A rigid bronchoscopy was done to exactly investigate the injury. It demonstrated a 6 cm full thickness rupture in the middle of the membraneous posterior wall, full of cloudy gastric contents (Figure 1b). With short interruptions of the jet ventilation, the complete rupture was washed and cleaned using normal saline >100ml. The rigid bronchoscopy was now changed with a 14mm rigid tracheaoscope. A running endotracheal suture with a 2/0 Vicryl thread (UCLX needle, Ethicon, Germany) was then applied with the optical needle holder (Karl Storz Endoscopes, Tuttlingen, Germany) (Figure 1c) as described earlier [5].
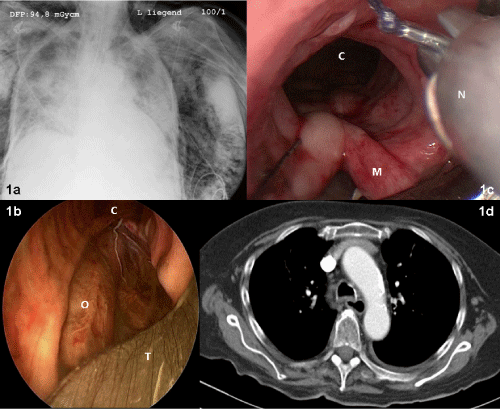
Figure 1a-d: Endobronchial findings and chest X-rays in the course of the treatment
View Figure 1
Results
The woman needed lung protective ventilation for 7 more days for a severe aspiration pneumonitis before she could be extubated. No further episode of tube obstruction occurred. After 5 days with repeated bronchoscopies for retention of secretions, she was exhausted and needed reintubation and early surgical tracheostomy. Despite the fact that the whole bronchial system was severely inflamed, the posterior tracheal wall healed primarily with no relevant fluid collection in the mediastinum (Figure 1d). The enteral nutrition was applied via nasogastric tube and later via percutaneous endoscopic gastrostomy. After 23 days, weaning from the ventilator was successful and the tracheostomy cannula could be removed at day 26. She was discharged in a home for elderly residents on day 47 and is fully mobile without complaints eight months later.
Discussion
Posterior tracheal wall lacerations are most frequently observed during emergency intubations in critical situations and this differentiates it from tracheal wall laceration due to other causes. The broad communication of the tracheal lumen with the mediastinum can result in severe complications such as progressive mediastinal emphysema, right-sided pneumothorax [1], massive air leak along the tube [6], dislocation of the tube tip into the rupture by small movements of the patient's head, continous bleeding and late sequelae with posterior wall instability [7]. Therefore, early treatment of the injury is mandatory. In the past, open repair via posterolateral thoracotomy or cervicotomy with open repair of the lesion was performed by many surgeons [2-4]. A review from Minambres et al. (2009) observed that thoracotomy in such critical situations increases mortality, and therefore some authors recommend conservative treatment for most patients with ongoing ventilatory support [4]. We first described the new method of complete endoluminal repair [5] and subsequently gathered further experience in 14 such cases. This is the first published report of a successful endotracheal repair in a septic patient with severe aspiration pneumonitis. The aim was to stabilize the central airways and avoid further dislocation of the endotracheal tube.
Conclusion
This case demonstrates that endoluminal repair of full thickness TML without the trauma of a separate incision is feasible even in disastrous situations and may prevent early and late complications as mentioned above. The method is worth being established in specialized major units.
Acknowledgement
We thank Prof. Georgios Stamatis1 for his critical discussion of the case and the encouragement to publish this promising treatment option.
Author Contribution
S.W. and P.S. contributed substantially to the conception and design of the study and the acquisition of data.
D.C. and T. E. drafted or provided critical revision of the article.
S.K. provided final approval of the version to publish
References
-
Stokes S, Wu D (2004) Suprapubic bladder catheterization. In: Reichman E, Simon R eds. Emergency Medicine Procedures. New York: McGraw-Hill: 1134-4.
-
Halder SK, Khan I, Mukhopadhyay P, Paira SK (2012) Inadvertent suprapubic gastrostomy: Report of a unique complication of blind percutaneous suprapubic trocar cystostomy. Indian J Urol 28: 445-446.
-
Rees M, Joseph AE (1981) Ultrasound guided suprapubic puncture-a new, simple way of releasing a blocked Foley balloon. Br J Urol 53: 196.
-
WMM Lee, KL Tsui, CW Kam (2005) Trans-abdominal ultrasound-guided suprapubic puncture of a nondeflating Foley catheter balloon. Hong Kong Journal of Emergency Medicine 12: 42-45.
-
Aguilera PA, Choi T, Durham BA (2004) Ultrasound-guided suprapubic cystostomy catheter placement in the emergency department. J Emerg Med 26: 319-321.
-
Jacob P, Rai BP, Todd AW (2012) Suprapubic catheter insertion using an ultrasound-guided technique and literature review. BJU Int 110: 779-784.
-
Robin Guillory, Marc de Moya (2011) Use of ultrasound in the ICU Critcal Care. Luca M Bigatello, Hassan Alam, Ree M Allain, Edward A.Bittner. Handbook of the Massachusetts General Hospital (5th edn). Wolter Kluwer Pvt. Ltd 3: 39-49.





