International Journal of Anesthetics and Anesthesiology
Airway Management following Facial Trauma Caused by a Pit Bull Attack
Jaime Ortiz1* and Kelly A. Frew2
1Department of Anesthesiology, Baylor College of Medicine, USA
2Department of Anesthesiology, Greater Houston Anesthesiology, USA
*Corresponding author: Jaime Ortiz, MD, Department of Anesthesiology, Baylor College of Medicine, MS: BCM120, Houston, Texas 77030, USA, Tel: 713-873-2860, E-mail: jaimeo@bcm.edu
Int J Anesthetic Anesthesiol, IJAA-1-021, (Volume 2, Issue 1), Case Report; ISSN: 2377-4630
Received: February 20, 2015 | Accepted: February 26, 2015 | Published: February 28, 2015
Citation: Ortiz J, Frew KA (2015) Airway Management following Facial Trauma Caused by a Pit Bull Attack. Int J Anesthetic Anesthesiol 2:021. 10.23937/2377-4630/2/1/1021
Copyright: © 2015 Ortiz J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Airway management of patients following facial trauma poses many challenges to the acute care team. An 80 year old male presented following a pit bull attack with massive trauma to his face, scalp and extremities. After carefully considering the options available, we were able to safely secure his airway by utilizing a WuScope. We confirm that the WuScope is a useful tool for airway management in a case of severe facial trauma.
Keywords
Trauma, Airway, Wuscope, Fiber optic
Introduction
Airway management of patients following facial trauma poses many challenges to the acute care team. We describe the use of the WuScope to secure the airway of a patient who suffered severe facial trauma after a pit bull attack.
Case Description
An 80 year old African American male (173 cm, 80 kg) presented to the emergency center after being attacked by 2 pit bulls while mowing his neighbor�s lawn. On presentation, he was awake with a GCS of 15. He had massive trauma to his face and scalp, including a missing left ear and left eye, and severe damage to his forehead, nose, right eye, and upper lip. He also had an avulsion of his scalp and multiple bite wounds on his back, bilateral wrists and legs (Figure 1).
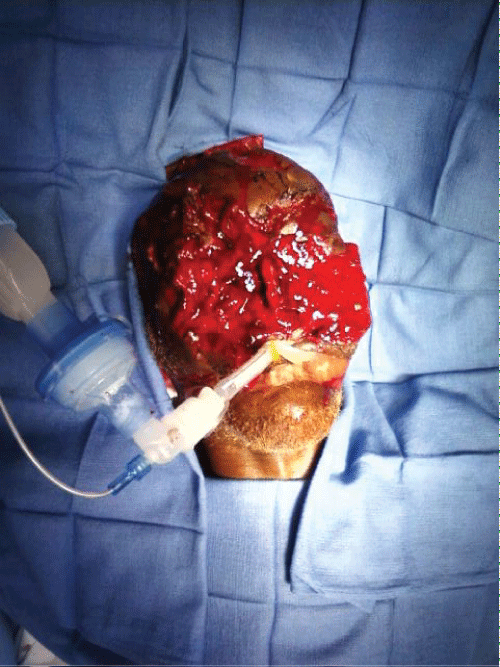
Figure 1: Case anatomy
View Figure 1
He was immediately transported to our trauma operating room for assessment and airway management. On physical exam, he was sitting upright, alert, and able to talk and open his mouth without difficulty. His face and mouth were covered in blood and noted to be actively oozing. His initial vital signs included blood pressure 85/50, heart rate 105, respiratory rate 24, and oxygen saturation 98% on 100% non-rebreather oxygen mask. A quick airway exam showed severe trauma to his nose and upper lip, a Mallampati Class II airway with an oral aperture greater than 3 cm, thyromental distance greater than 6.5 cm, and normal range of motion of the neck. There was no apparent trauma to his jaw or neck area.
After consultation with the trauma surgeons, the decision was made to secure the airway to allow for urgent exploration and repair of his numerous bleeding lacerations. Although performing an awake fiberoptic intubation was considered, we were deterred by the copious amount of blood in the airway which would have limited the view and made adequate airway topicalization difficult. In addition, there was concern about the potential to find loose teeth, other loose tissues, or swelling in the airway which could not be ruled out by the airway examination. Also, ventilation would have been difficult as the nasal injuries would have made it difficult to create an adequate seal with the mask. Because there was no obvious neck injury or deformity, and it appeared that the patient would have been an easy airway if not for the acute trauma, performing an awake tracheostomy did not seem necessary at this time.
The trauma surgeons prepared to perform an emergency tracheostomy if our attempt at intubation failed. The patient was kept in a sitting position and pre-oxygenated with 100% oxygen for 5 minutes. We then performed a rapid sequence induction with 18mg of etomidate and 80mg of succinylcholine while holding cricoid pressure. Rigid fiber optic laryngoscopy was performed with a WuScope. We were able to successfully visualize the vocal cords on our first attempt and passed an 8.0mm tracheal tube without difficulty. Auscultation of bilateral breath sounds and capnography confirmed successful position of the tracheal tube. The tracheal tube was secured to his mandible as allowed by his injuries. Vital signs remained stable throughout the induction and intubation with an oxygen saturation of 100%.
The surgical team proceeded to explore and repair his facial and scalp wounds, as well as the injuries sustained to his arms and legs. A tracheostomy was performed in order to achieve better surgical access for the multiple facial repairs. After a 2 week hospital stay, the patient was discharged to a rehabilitation facility.
Discussion
An estimated 1 million people in the United States are bitten by dogs each year [1], accounting for approximately 1% of all emergency room visits to hospitals [2]. Dog bites sustained to the head, face, and neck are found much more frequently in young children, accounting for approximately 65% of these injuries [1]. Airway management in these patients, as in any facial trauma patient, is a primary concern. Not only does damage sustained to the airway itself present immediate challenges, but associated conditions such as cervical fracture, full stomach, and alcohol/drug intoxication can complicate the clinical picture [3]. Frequently, further compromise of the airway due to bleeding, loose teeth, and displaced fracture fragments are also encountered. However, it has been noted, that dog bites rarely result in facial fractures. The index of suspicion should be raised when the injury occurs in a child and involves the orbit, nose, or cheek [4]. The most common injuries resulting from dog bites include lacerations, nerve damage, and major blood loss [5].
In this case, we encountered a patient with severe facial trauma, a potentially difficult airway, and a full stomach. Although imaging studies had not yet been obtained, the etiology of the injuries combined with a brief physical exam suggested the damage was limited to the soft tissues. To secure the airway we opted for rigid fiber optic laryngoscopy with a WuScope.
The WuScope apparatus (Achi Corp., Fremont, CA, and Asahi Optical Co., Pentax, Tokyo, Japan) consists of a tubular, curved, bi-valved, rigid blade portion and a flexible fiberscope [6]. This device facilitates tracheal intubation without neck extension, tongue lifting, or forceful jaw opening, secondary to a 1100 handle-to-blade angle permitting easy visualization of the glottis unobtainable with conventional laryngoscopy. Because it combines the best characteristics of both rigid and flexible laryngoscopy, it can be useful in a variety of complex clinical situations. In addition, the tubular blade protects the fiberscope lens from secretions, blood, or redundant tissues better than during flexible fiber optic intubation. This feature is the reason why we felt the WuScope gave us the best and safest approach to securing this patient�s airway. In addition, its use allowed the entire trauma team to visualize the airway in real time during our intubation.
The efficacy of the WuScope device in the management of anticipated difficult airways, as a rescue device for unexpected difficult airways, and for emergency awake intubations has been well documented [6,7]. Specifically, its successful use has been described in cases of cervical hematoma following carotid endarterectomy, glottic tumor [7], and unstable cervical spines requiring immobilization [8]. We are not aware of a case report describing its use in this type of facial trauma.
Alternative management options for this trauma patient with a potential difficult airway included rapid sequence induction with conventional direct laryngoscopy, use of other fiber optic laryngoscopy devices such as the GlideScope, Bullard scope, intubating Laryngeal Mask Airway™ (LMA), awake or asleep fiber optic intubation, awake blind nasal intubation, tracheostomy under local anesthesia, and cricothyrotomy. Given the profound bleeding and soft tissue injuries around the oral area, we opted against conventional laryngoscopy. Although our patient was cooperative and not hypoxic, significant facial, nasal, and oral trauma with active bleeding diminished the likelihood of a successful awake or asleep fiber optic intubation. In addition, intubation through the nares was ruled out based on significant injury to this area. After making sure that the surgical team was ready to perform a tracheostomy if we were unable to successfully intubate or ventilate the patient, we proceeded with a rapid sequence induction and successful intubation using the WuScope.
In conclusion, the present case confirmed that the WuScope is a useful tool for airway management in a case of severe facial trauma.
References
-
Abuabara A (2006) A review of facial injuries due to dog bites. Med Oral Patol Oral Cir Bucal 11: E348-350.
-
Weiss HB, Friedman DI, Coben JH (1998) Incidence of dog bite injuries treated in emergency departments. JAMA 279: 51-53.
-
King HK (1996) Airway managements of patients with maxillofacial trauma. Acta Anaesthesiol Sin 34: 213-220.
-
Tu AH, Girotto JA, Singh N, Dufresne CR, Robertson BC, et al. (2002) Facial fractures from dog bite injuries. Plast Reconstr Surg 109: 1259-1265.
-
Bergmann J, Lee K, Klein R, Slonim CB (2009) Upper face and orbit "degloving" dog bite injury. Ophthal Plast Reconstr Surg 25: 44-46.
-
Wu TL, Chou HC (1994) A new laryngoscope: the combination intubating device. Anesthesiology 81: 1085-1087.
-
Sprung J, Weingarten T, Dilger J (2003) The use of WuScope fiberoptic laryngoscopy for tracheal intubation in complex clinical situations. Anesthesiology 98: 263-265.
-
Smith CE, Pinchak AB, Sidhu TS, Radesic BP, Pinchak AC, et al. (1999) Evaluation of tracheal intubation difficulty in patients with cervical spine immobilzation: fiber optic (WuScope) versus conventional layrngoscopy. Anesthesiology 91: 1253-1259.





