International Journal of Anesthetics and Anesthesiology
Anesthesiologists as Operating Room Directors: Results of a Survey
Steven Boggs1*, Elizabeth Frost1 and Jessica Feinleib2
1Department of Anesthesiology, Icahn Medical School at Mount Sinai, New York, USA
2Department of Anesthesiology, Yale Medical Center, New Haven, USA
*Corresponding author: Steven Boggs, Department of Anesthesiology, Icahn Medical School at Mount Sinai, New York, NY 10029, USA, E-mail: stevendaleboggs@gmail.com
Int J Anesthetic Anesthesiol, IJAA-3-041, (Volume 3, Issue 1), Research Article; ISSN: 2377-4630
Received: December 18, 2015 | Accepted: January 28, 2016 | Published: January 30, 2016
Citation: Boggs S, Frost E, Feinleib J (2016) Anesthesiologists as Operating Room Directors: Results of a Survey. Int J Anesthetic Anesthesiol 3:041. 10.23937/2377-4630/3/1/1041
Copyright: © 2016 Boggs S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Many ideas have gone into the development of the concept of the Perioperative Surgical Home (PSH) and Enhanced Recovery after Surgery (ERAS). Many anesthesiologists have advocated for an increased role in operating room (OR) management, advancing from OR managers to OR directors with greater decision making and improved means of communication. However, there is little uniformity at present in the running of ORs around the country.
Methods: In an attempt to better understand how ORs are run and to gauge the response and attitude of both academic and general practice anesthesiologists to playing an increased role, we performed an international literature review, followed by a survey both by internet and at a national meeting.
Results: Of 19 identified articles, 7 were from primarily non-English speaking countries. All articles noted that rational management of the OR requires appropriate data collection to make both strategic and tactical decisions. The E mail and meeting survey garnered 350 responses. Analysis indicated that the OR was managed by an anesthesiologist in 52% of cases, by a nurse in 46%, by a surgeon in 18% and by a team approach in 18%.Only 34% responded that the OR leaders had any training in management. An overwhelming 94% gave a positive response to the query about whether anesthesiologists possess the skills to be OR directors as either the team leader or as part of a team. While 71% were aware of PSH/ERAS, only 34% used these models.
Conclusions: Almost all the anesthesiologists polled believed that they were in the best position to direct the OR. Complex skills are required and currently are not adequately taught.
Introduction
Management of operating rooms (OR) has become increasingly complicated over time. Case scheduling and time management in the OR suite have always been critical skills, but knowledge of and compliance with hospital, state and national regulations and budgetary matters have grown in importance, complexity and significance to hospitals. The OR accounts for up to 60% of the revenue of a facility and up to 40% of its expenses [1]. Numerous factors in the perioperative period can and must be optimized to improve patient safety as well as both patient and surgeon satisfaction and increase profit margins. Improved scheduling to add greater efficiency, standardization of processes, especially as regards to drug management, better operational reporting, clearer throughput, on time first case start and transparency of OR utilization are just some of these factors [2-4].
To underscore the importance of surgery and procedures for facilities, a recent study demonstrated that cancelled surgeries have a highly significant financial impact on hospitals ($4,500/cancelled case) [5]. Managing an OR requires both medical and business acumen. For OR directorship, though, many other attributes are required including leadership over the entire perioperative process, a collaborative work ethic and the ability to understand and enforce policies and procedures, ensuring that Standards of Care are known and followed, as demonstrated in some recent job application sites [6,7].
Historically, either surgeons or anesthesiologists have acted as medical managers in ORs. These individuals have focused primarily on ensuring that facilities have met medical standards of care (a legal term). Operating room directors, in contrast, have typically come from nursing services and these individuals have usually been tasked with improving turnover and other metrics of performance in the operating suite. Unfortunately, the objectives that nurses who are OR directors pursue may not reflect those most significant to the facility, as they tend to focus rather on reduction of under-utilized OR time and nursing labor costs instead of total revenue and contribution margin to the facility as well as other more focused medical issues [8].
With the development of the Perioperative Surgical Home (PSA) and Enhanced Recovery after Surgery (ERAS), a compelling argument might be made that anesthesiologists should assume overall leadership in the OR. For example, as Dexter et al point out, anesthesiologists have several principle opportunities for net cost reduction by eliminating unnecessary interventions that do not have the potential to benefit patients (e.g. routine preoperative testing), decreasing fresh gas flows with inhalational agents and optimizing staff assignments [9]. The objectives of an anesthesia group are to maximize case production and efficiency and minimize OR downtime. These objectives mirror those of the facility. Anesthesiologists would seem to have ideal backgrounds to serve both as medical directors of the OR and as overall OR directors because their work place is primarily in the OR suite and they interact with all surgical and procedural services. Increasingly their work also involves provision of services at off-site, non-OR locations. In addition, anesthesiologists organize staff scheduling, often for very large departments, and manage large capital budgets. Most importantly, however, it is in the best interests of anesthesiologists and facilities to minimize underutilized OR time.
However, many anesthesiologists feel they are already overburdened, especially balancing work and family. For this reason we sought to devise a pilot study to assess attitudes of anesthesiologists to the concept of assuming the greater responsibilities of OR directorships.
Methods
Our study involved two parts. The first was a literature review; the second a survey. For the literature review, we worked with the reference librarian at the Levy Library at the Icahn School of Medicine. A search was conducted in the English, French, German and Spanish literature with the following keywords:
• Anesthesiologist(s) as operating room director
• Anesthesiologist(s) + operating room director
• Anesthesiologists + running the operating room
• Nurses as operating room director
• Nurse + operating room director
• Nurse + running the operating room
• Operating room (OR) Director
• Anesthesiologist + operating room (OR) director
• Medical Director + operating room (OR) (surgeon, anesthesiologist)
In addition, general search engines were used to identify available residency and post-residency training programs in OR management in all specialties.
For the survey, in November 2014 an e-mail questionnaire was sent to all anesthesiologist registrants at the Post Graduate Assembly (PGA) meeting of the New York State Society of Anesthesiologists (NYSSA) in New York. Information sought consisted of basic demographic data, OR management at individual facilities, views on the role of the anesthesiologist in that position and use and familiarity with PSH/ERAS. Additional data were collected by direct yes or no voting at a scientific booth at the meeting, with the same questionnaire. Participants were asked not to fill out the electronic survey at the booth if they had previously completed it online.
Results
Our literature search found nineteen (19) articles that met our search criteria since 1998. Of these, seven (7) were from non-primarily English-speaking countries. The work of Dexter and colleagues constituted two (2) of the articles from the English literature [8,10]. The US literature had a slight tilt toward data-driven management of the OR while the European literature tended to focus more on the questions of "who" should manage the OR [11-16]. All articles cited an underlying theme that rational management of the operating room requires appropriate data collection to make both strategic and tactical decisions [17]. The OR manager cannot make optimal decisions without basic data. Yet, learning how to obtain these data and then act on them is not intuitive to any manager - surgeon, nurse or anesthesiologist [18,19]. For example, Wang et al performed a behavioral study of daily mean turnover times and first case start times [20]. They found that overall, the staff worked just as quickly on days with few or many hours of cases with no slow down apparent. Other data have focused on managerial decisions by anesthesiologists that resulted in increased clinical work with over-utilized OR times, higher staffing costs and unpredictable work hours that could mandate overtime [21,22]. The authors suggest that enterprise-wide scheduling cab coordinate anesthetics with other appointments on the same date and improve consistency and accuracy of patient instructions [23].
To address these and other deficiencies an intensive 4-day course in OR Operations Research is conducted at the University of Iowa [24] This course is an intensive 4-day course in which participants receive refresher training in statistics and then learn to both gather data and make decisions based on the data so obtained. Examples of the case studies from the course include:
• Anesthesia preoperative evaluation clinics
• Decision-making on the day of surgery
• Service-specific operating room staffing
• Operating room financial assessment for tactical decision-making
• Economics of reducing turnover times
• Economics of anesthetic agents
• Strategic planning: financial impact of different types of surgery
• Anesthesiologist and nurse anesthetist staffing
• Physician agreements - Anesthesia support & surgeon blocks
• Showing differences among hospitals and their surgical practices
A recent survey of anesthesiology training programs revealed that while residents and program directors felt that they received adequate instruction in quality management and OR scheduling, they did not receive enough training in actual practice management - particularly as it pertains to cost containment [25]. Only a few established programs in the Management of Perioperative Services exist (Stanford, MGH, Irvine, and Columbia). Most residents finish their training, believing that they know how to "run the board", which involves triaging cases and assigning anesthesia staff. However, without testing this assumption cannot be made [21,22]. Moreover, most residents do not graduate with significant understanding of OR management, which includes leadership skills, logistics, communication systems and understanding of the financial and accounting skills for efficiently managing an OR suite. Such a skill-set differs radically from the didactic programs that are the norm.
Regarding our NY State Society of Anesthesiologist Survey at the PGA, of the 3069 anesthesiologist registrants 280 responded. An additional 70 voted directly. Results are as follows:
• 52% stated that an anesthesiologist managed their OR
• 46% stated that a nurse managed their OR
• 16% stated that a surgeon was currently managing their OR.
• 18% noted team management.
• 71% were familiar with PSH/ERAS, but only
• 34% used these models
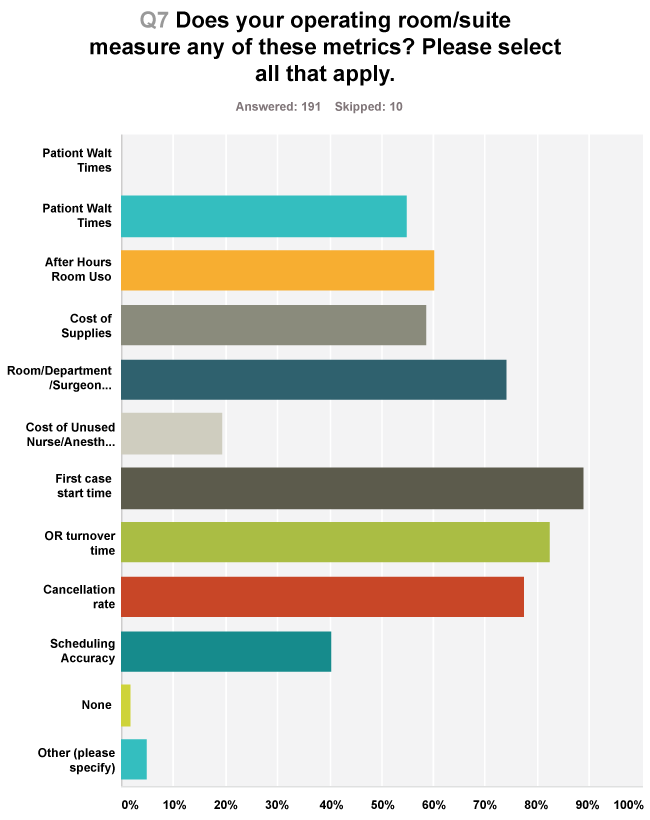
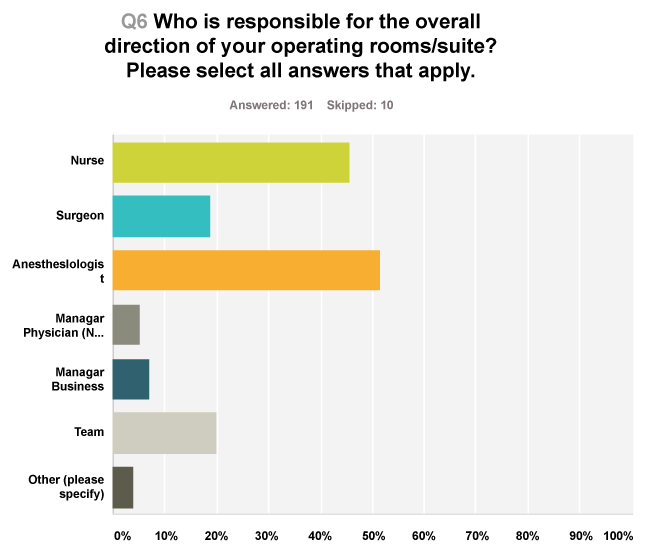
Multiple metrics were measured at most facilities (Figure 1). These factors included documentation of first-time start performance, turnover time and room utilization. In 2% of facilities, no metrics were measured. Sixty-40% of respondents thought that OR directors should use management techniques and fiscal decision making skills. However, only 34% of respondents stated that their OR managers had any management training and of that number only 8% had 1-2 years of training either in attending courses or completing advanced programs and/or degrees in business or hospital management. Manual voting plus the survey results pointed to a 94% positive response to the query about whether anesthesiologists possess the skills to be OR directors as either the team leader or as part of a team. The voting also indicated that in this study population, responsibility for the overall direction of the operating room was considered the responsibility of anesthesiologists, nurses and then surgeons 52%, 45% and 18% of the time, respectively (Figure 2).
.
Figure 2: The majority of anesthesiologists believe that they are suited to be OR directors.
View Figure 2
Discussion
Managing operating suites requires multiple high-level skills. Leadership attributes are essential to harness the efforts of a well and diversely trained workforce. Yet, because ORs function as significant revenue sources, an OR director must also be able to both gather the requisite data needed for efficiency while appreciating the interventions needed to accomplish those goals. Residency programs train clinicians to function as excellent clinical anesthesiologists, but most graduates do not feel that they complete residency programs with the skill-set to competently manage complex ORs efficiently.
Anesthesiologists generally finish training and enter practice with the basic skills required to be OR medical directors. These essential skills include:
1. Daily management of the operating room schedule
2. Planning for patients in the pre-, intra-, and postoperative stages of surgery
2. Work ethics to assure effective and appropriate use of OR resources
3. Establishment of protocols for the management of patients in all stages of surgery to promote quality, safety and cost-effective delivery of care
4. Ensuring adequate anesthesia personnel are available to cover the daily surgical schedule
7. Enforcing standards of care within guidelines of regulatory agencies
8. Safeguarding the fiscal integrity of the program
The duties of an OR director are different and require additional training. The duties of an OR director include [26]:
1. Overseeing the management of perioperative services
2. Coordinating, facilitating and managing changes within the perioperative services
3. Collecting and analyzing data related to quality, performance or cost improvement projects as they apply to perioperative services
4. Use of conflict resolution techniques as a leader of a multidisciplinary team
5. Evaluation of performance of perioperative personnel
6. Interview techniques for personnel selection
7. Ensuring that personnel, equipment and supplies are available for all perioperative services
8. Coordination of advanced project management with principals.
9. Conveying the mission of the organization
When asked, the majority of anesthesiologists believe that they are suited to be OR directors. However, as the above list illustrates, managerial techniques, personnel management, quantitative analysis and behavioral managerial tools are skills required to successfully function as an OR director. Most anesthesiologists are capable of mastering this body of knowledge but additional education is required to become fully competent in these areas.
There are inherent difficulties in searching out information on OR management as many people making management decisions do not read published literature, rather relying on colleague advice [27]. On-line help files may be complicated to navigate with specialized vocabularies, unique to the application. In addition, to date, there are very few articles that address specific subject areas such as anesthesia group management.
It is not surprising that up to now the selection of both medical directors and OR directors for operating suites has been a local decision. Previously, no specific training background has been identified for these positions. However, to improve both financial and operational metrics for facilities, the ability to both measure appropriate indicators and to make decisions on that data will become increasingly important. The costs of hiring an ill suited person or losing valuable staff members due to poor management will continue to grow. Ensuring continuous supply of material to the OR will be more challenging with just-in-time delivery and more complicated informational technology ordering systems.
Our study is admittedly skewed in that we surveyed only anesthesiologists, not nurses and surgeons. Our initial aim was to gauge the interest of anesthesiologists in expanding their role in the OR, especially in the light of the PSH/ERAS initiative. Admittedly the response rate was low but that is not uncommon in electronic surveys today. As a pilot study the positive information obtained will be used to design studies of other groups that also have significant involvement and interest in the management of operating suites, including surgeons and nurses. Going forward we will partner with colleagues in these specialties to explore the level of training and interest among surgeons and nurses for operating room management.
We believe that the time has come to raise awareness of the capability of anesthesiologists to assume broader leadership in the operating suite. Anesthesiologists already understand the flow from pre-operative assessment through the operating suite and other non-operating room locations all the way through the post-operative recovery phase. They spend their entire workday in this environment and are already familiar with many of the roadblocks to process improvement. And, they are familiar with the necessary standards of perioperative care.
However, anesthesiologists or anyone who assumes management of an operating room suite must add to their medical knowledge with education in operations, finance, accounting and personnel management to serve as effective leaders in the role of operating room directors. The clinical significance of this is that when functioning in this capacity, the individual is not ensuring the welfare of only an individual patient but rather that of an entire group of patients. If the OR suite is not managed efficiently, it can limit the care a hospital can provide [28].
While no particular background in and of itself can prepare someone for these positions, with the correct training anesthesiologists may be ideal candidates. Moreover, as major proponents of the Perioperative Surgical Home (PSH), such leadership allows anesthesiologists to further contribute to patient welfare, efficiencies for hospitals, cost-minimization and increased throughput. Conducting a similar survey at a national surgical or nursing meeting should offer increased insight.
In sum, this study points out that OR managers require advanced training in business. It needs to be investigated if any one primary specialization is optimal preparation for managing an OR. Further research across disciplines (nursing, surgery and anesthesiology) is required to answer this question. However, in a period of significant cost pressures and declining reimbursement, the need for optimal operating suite function is more important than ever to ensure safe and appropriate provision of service to patients.
References
-
Randa K, Heiser R, Gill R (2009) Strategic investments in the operating room: information technology to generate rapid ROI and long-term competitive advantage.
-
Herman B (2012) Seven Strategies To Help Hospitals Break Even on Medicare. Becker's Hospital Review.
-
Fixler T, Wright J (2013) Identification and Use of Operating Room Efficiency Indicators: The Problem of Definition. Can J Chir 56: 224-226.
-
Tsai MH, Hudson ME, Emerick TD, McFadden DW (2015) The true relevance of first-case start delays. Am J Surg 209: 427-429.
-
Bent S, Mora S, Russo N (2012) The Financial Burden of Cancelled Surgeries: Implications for Performance Improvement. Practice Management, Research in Perioperative Management. Practice Management 23.
-
http://harrisonmedical.org/home/news-media/
-
https://www.higheredjobs.com/
-
Masursky D, Dexter F, Nussmeier NA (2008) Operating room nursing directors' influence on anesthesia group operating room productivity. Anesth Analg 107: 1989-1996.
-
Dexter F, Wachtel RE (2014) Strategies for net cost reductions with the expanded role and expertise of anesthesiologists in the perioperative surgical home. Anesth Analg 118: 1062-1071.
-
Dexter F, Masursky D, Wachtel RE, Nussmeier NA (2010) Application of an Online reference for Reviewing Basic Statistical Principles of Operating Room Management. J Statistics Education 18.
-
Bender HJ, Denz C, Schleppers A (2007) The optimization of a medicinal process and the organization of work in an operating-room. Anesteziol Reanimatol : 6-9.
-
Butler V, Clinton C, Sagi HK, Kenney R, Barsoum WK (2012) Applying science and strategy to operating room workforce management. Nurs Econ 30: 275-281.
-
Tsai MH (2008) Ten tips in providing value in operating room management. Anesthesiol Clin 26: 765-783, viii.
-
Gebhard E, Hartwig E, Isenmann R, Triebsch K, Gerstner H, et al. (2003) OR-manager: surgeon or anesthesiologist? An interdisciplinary study. Anaesthesist 52: 1062-1067.
-
Marjamaa R, Vakkuri A, Kirvela O (2008) Operating room management: why, how and by whom? Acta Anaesthesiol Scand 52: 596-600.
-
Marty J, Plaud B (2009) Anesthetic process, organization, management and economic issues: the French perspective. Curr Opin Anaesthesiol 22: 249-254.
-
Baumgart A, Schupfer G, Welker A, Bender HJ, Schleppers A (2010) Status quo and current trends of operating room management in Germany. Curr Opin Anaesthesiol 23: 193-200.
-
Wang J, Yang K (2014) Using type IV Pearson distribution to calculate the probabilities of underrun and overrun of lists of multiple cases. Eur J Anaesthesiol 31: 363-370.
-
Sanford JA, Macario A (2014) Data, data, on the server: challenges in applying data analysis to operating room management. Anesthesiology 121: 6-8.
-
Wang J, Dexter F, Yang K (2013) A behavioral study of daily mean turnover times and first case of the day start tardiness. Anesth Analg 116: 1333-1341.
-
Dexter F, Lee JD, Dow AJ, Lubarsky DA (2007) A psychological basis for anesthesiologists' operating room managerial decision-making on the day of surgery. Anesth Analg 105: 430-434.
-
Dexter F, Willemsen-Dunlap A, Lee JD (2007) Operating room managerial decision-making on the day of surgery with and without computer recommendations and status displays. Anesth Analg 105: 419-429.
-
Dexter F, Xiao Y, Dow AJ, Strader MM, Ho D, et al. (2007) Coordination of appointments for anesthesia care outside of operating rooms using an enterprise-wide scheduling system. Anesth Analg 105: 1701-1710, table of contents.
-
Wachtel RE, Dexter F (2010) Curriculum providing cognitive knowledge and problem-solving skills for anesthesia systems-based practice. J Grad Med Educ 2: 624-632.
-
Kalarickal PL, Stain E, Rieff B, Fox CJ, Rosinia FA (2012) Practice Management Education in Anesthesiology Training programs is not Adequate: The Results of a Survey of the ASA Membership. Abstracts. ASA Practice Management (PM) PM19.
-
Director of operating room, job description. Roosevelt General hospital.
-
Wachtel RE, Dexter F (2013) Difficulties and challenges associated with literature searches in operating room management, complete with recommendations. Anesth Analg 117: 1460-1479.
-
Mango PD, Schapiro LA (2001) Hospitals get serious about operations. The McKinsey Quarterly 2: 74-85.