International Journal of Anesthetics and Anesthesiology
Trachway Intubating Stylet Facilitates the Double-Lumen Endobronchial Tube Placement in Patients with Limited Mouth Opening
Wen-Ming Chuang1, Hung-Te Hsu1,2, Shah-Hwa Chou3, Chia-Chen Wu1, Kuang-Yi Tseng1, Kuang-I Cheng1,4 and Miao-Pei Su1*
1Department of Anesthesia, Kaohsiung Medical University Hospital, Kaohsiung, Taiwan
2Graduate Institute of Medicine, College of Medicine, Kaohsiung Medical University, Kaohsiung, Taiwan
3Department of Chest Surgery, Kaohsiung Medical University Hospital and School of Medicine, Kaohsiung Medical University, Kaohsiung, Taiwan
4Faculty of Anesthesiology, College of Medicine, Kaohsiung Medical University, Kaohsiung, Taiwan
*Corresponding author:
Miao-Pei Su, Department of Anesthesia, Kaohsiung Medical University Hospital, No.100, Ziyou 1st Rd., Sanmin Dist., Kaohsiung City 807, Taiwan, Tel: +886-7-3121101-7033, Fax: +886-7-3127874, E-mail: cavia0803@hotmail.com
Int J Anesthetic Anesthesiol, IJAA-4-057, (Volume 4, Issue 1), Case Report; ISSN: 2377-4630
Received: January 25, 2017 | Accepted: March 10, 2017 | Published: March 13, 2017
Citation: Wen-Ming C, Hung-Te H, Shah-Hwa C, Chia-Chen W, Kuang-Yi T, et al. (2017) Trachway Intubating Stylet Facilitates the Double-Lumen Endobronchial Tube Placement in Patients with
Limited Mouth Opening. Int J Anesthetic Anesthesiol 4:057. 10.23937/2377-4630/1410057
Copyright: © 2017 Wen-Ming C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Intubation for one lung ventilation in patients with difficult airways can be a challenge. Severely limited mouth opening restricts the use of direct laryngoscopy or video-assisted laryngoscopy. We present two patients with limited mouth opening undergoing video-assisted thoracoscopic decortication, who were successfully intubated with left-sided double-lumen endobronchial tube (DLT) using the Trachway® intubating stylet. This technique provides a safe and reliable method for DLT intubation in patients with limited mouth opening.
Keywords
Difficul airway, Double-lumen tubes, One-lung ventilation
Introduction
Thoracic surgeries in patients with difficult airways always make the anesthesiologist face the challenges of lung isolation. One lung ventilation (OLV) usually can be achieved with double lumen endobronchial tube (DLT) or bronchial blocker. In patients with difficult airways, the first step is endotracheal intubation with a single-lumen endotracheal tube (ETT), which for further an independent bronchial blocker advanced in or being replaced by a DLT over an exchange catheter [1-3]. However, the quality and time-consuming of lung deflation when using bronchial blocker in video-assisted thoracoscopic surgery (VATS) remains a debate [4,5]. The tube exchange technique via an airway exchange catheter would be difficult if the bronchial lumen of DLT impacted at the arytenoid cartilages [6].
Limited mouth opening, one of major cause of difficult intubation, restricts the use of direct laryngoscopy or video-assisted laryngoscopy. Several video-assisted airway devices such as GlideScope® and Airtraq® have been developed for the management of difficult intubation. Awake fiberoptic intubation for these patients was a good solution but some patients might not tolerate and cooperate during the procedure only under topical anesthesia. Trachway® (Biotronic Instrument Enterprise Ltd., Taichung, Taiwan) intubating styleth as demonstrate to be successful in tracheal intubation in some difficult airway scenarios such as limited neck motion, and also has been applied in DLT intubation in normal airway [7,8]. However, its efficacy in DLT intubation in patients with difficult airways has not yet been reported.
We are presenting two patients with limited mouth opening who were successfully intubated orotracheally with left-sided DLT using Trachway® intubating stylet. Written informed consents were obtaine from both patients to publish this case report.
Case Report
Case 1
A 61-year-old, weight 68 kg, male patient was scheduled to undergo video-assisted thoracic surgery (VATS) decortications for left empyema. General anesthesia and one-lung ventilation with a double-lumen endobronchial tube (DLT) were required. His past medical history was significant for nasopharyngeal cancer (NPC) with radiation therapy, left facial palsy caused by cerebral infarction six months ago, and hearing impairment. Pre-operative examination revealed limited mouth opening (1.6 cm) and a moderate amount of encapsulated left pleural effusion.
Standard monitors including ECG, invasive blood pressure measurement (arterial line in right radial artery) and pulse oximetry were placed in the operating room. The Trachway® intubating stylet (Extra-length size) was preloaded with a 37F left-sided DLT through the bronchial lumen (Figure 1). A suction unit was available to clear upper airway secretions if necessary. After pre-oxygenation for 3 minutes, general anesthesia was induced using fentanyl 2 μg/kg, lidocaine 1.0 mg/kg, thiamylal 5 mg/kg rocuronium 0.8 mg/kg. Incremental dose of propofol 1.0 mg/kg were given to decrease hemodynamic response to intubation. The combination of Trachway® and DLT was introduced smoothly via midline approach into trachea, the bronchial cuff is passedthrough the vocal cords while patient in a sniffing position (Figure 2), and the whole device is rotated 90 degrees counter clock wise. The Trachway® intubating stylet is retrieved from DLT whichis advanced more deeply until resistance was felt. Success of intubation was confirmed by end-tidal carbon dioxide and bilateral breath sounds. The duration of intubation was about one minute, without desaturation. The position of DLT was further confirmed by fiberoptic bronchoscopy.

.
Figure 1: The assembly of Trachway® intubating stylet and left-sided double-lumen endobronchial tube.
View Figure 1
.
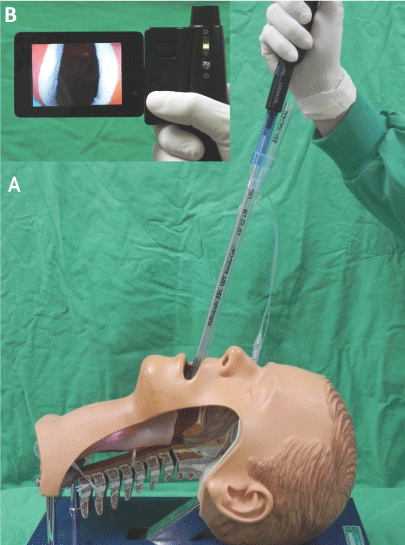
Figure 2: The Simulation of DLT intubation with Trachway® intubating stylet. A) Insert the Trachway-DLT assembly into the mouth in a sniffing position; B) vocal cord images displayed on the monitor of Trachway.
View Figure 2
At the end of surgery, the DLT was replaced with an 8 Fr. sized single lumen endotracheal tube by using a 14F airway exchange catheter (AEC, Cook Critical Care, Bloomington, IN). The patient was transferred from ICU to ward on the next day, and discharged 10 days later without any sequelae.
Case 2
This case is a 22-year-old, 42 kg, ASA class II, autistic female patient with less than 2 cm mouth opening was undergoing VATS decortications for right lobulated pleural effusion with mediastinal shifting. Endotracheal intubation general anesthesia and lung isolation were requested. The patient's general condition was well except mild pericardial effusion. The oxygen saturation under room air was 97%.
Trachway® intubating stylet preloaded with a well lubricated 32F left-sided DLT was planned via midline approach. After adequate pre-oxygenation, fentanyl 2 μg/kg, thiamylal 5 mg/kg, and rocuronium 0.8 mg/kg were administered to facilitate DLT intubation and incremental dose of propofol 1 mg/kg was used to blunt the hemodynamic responses during intubation. Trachway®-guided intubation was successful under the facilitation of video-assisted system. Trachway®-DLT intubation procedures in the second patient are same as that of the first. The intubating time was about one minute, without de saturation. The position of DLT was further confirmed by fiberoptic bronchoscopy.
At the end of surgery, the DLT was replaced with a 7 Fr. sized single lumen endotracheal tube using a 14F AEC. She was discharged from hospital 17 days later without any sequelae.
Discussion
One lung ventilation is achieved with DLT in most thoracic surgery, for the advantages of more rapid lung deflation, less intraoperative tube displacement, and allowing suctioning and re-expanding the operative lung during surgery [4]. However, in patients with limited mouth opening, DLT insertion may be very difficult.
There are several techniques for DLT intubation in patients with difficult airways. The first technique is awake fiberoptic endobronchial intubation [9]. The fiberoptic bronchoscope is placed through the bronchial lumen of DLT, which can be advanced into main bronchus under fiberoscopic guidance. This technique requires high anesthesiologist skill, as well as patient cooperation. The second technique is using video laryngoscope to assist DLT intubation [10-12]. These devices include Airtraq® (Prodol Meditec S.A., Vizcaya, Spain), GlideScope® (Saturn Biomedical Systems, Burnaby, BC, Canada), McGrath® (Covidien, Mansfield, MA), and Pentax-Airway Scope® (Pentax-AWS, Hoya Corp., Tokyo, Japan). The important role of video laryngoscope in difficult airway intubation was already established in SLT intubation. However, the extremely limited mouth opening, as shown in our cases, restricts the manipulation of above devices due to the thickness of the blades. The third technique is video-stylets. With a build-in camera, Trachway® provides direct visualization of the epiglottis, vocal cords, and tracheal rings, and the DLT can be pushed into the trachea immediately after the tip of Trachway® just at the vocal cords level [8]. In our experience, the width of mouth opening required in this method is almost the outside diameter of DLT, which makes the Trachway® suitable for more difficult airway intubation scenario. Bonfils is another intubating rigid fiberscope similar to Trachway with a curved tip for tracheal intubation in both normal and difficult airway scenarios. The major difference was that the image of Bonfils was observed by eyepiece. Subramani, et al. and Bein, et al. demonstrated case reports in successful double lumen tube placement by using Bonfils scope [13,14]. However, all of the video-assisted airway devices are limited by saliva, blood and secretions obscuring the vision of the airway. Therefore, clearing of upper airway secretions is a key point of successful intubation with these devices.
Chen, et al. reported the use of a video fiberoptic bronchoscope to assist DLT intubation in a patient with limited mouth opening due to oral cancer [15]. Unlike traditional awake fiberscope intubation, DLT was shaped like a "hockey-stick" and 5.5-mm video FOB was used to pass through the nostril to the pharynx as the monitor screen for DLT intubation guiding. However, this method is a two-men-procedure and is more complex. In our opinion, compared with Chen's method, using Trachway® intubating stylet for DLT intubation is a simple, single person technique. Previous reports of Trachway® were via midline approach. However, retromolar approach was valuable and feasible in specific conditions such extremely limited mouth opening or very loose teeth.
In patients with potential difficult airway, securing the airway is the first priority. Adequate assessment before intubation and selection of the appropriate tools to achieve OLV are the key elements of success. Using Trachway® to intubate the DLT in patients with limited mouth opening is safe and reliable. But the single-lumen ETT with bronchial blocker and fiberoptic bronchoscope should be prepared as alternative in case of failed DLT intubation.
References
-
Brodsky JB (2009) Lung separation and the difficult airway. Br J Anaesth 103: 66-75.
-
Campos JH (2010) Lung isolation techniques for patients with difficult airway. Curr Opin Anaesthesiol 23: 12-17.
-
Globokar MD, Novak-Jankovic V (2012) Difficult airway and one lung ventilation. Acta Clin Croat 51: 477-482.
-
Brodsky JB (2015) Con: a bronchial blocker is not a substitute for a double-lumen endobronchial tube. J Cardiothorac Vasc Anesth 29: 237-239.
-
Steven M Neustein (2015) Pro: bronchial blockers should be used routinely for providing one-lung ventilation. J Cardiothorac Vasc Anesth 29: 234-236.
-
Gamez R, Slinger PA (2014) simulator study of tube exchange with three different designs of double-lumen tubes. Anesth Analg 119: 449-453.
-
Kim JK, Kim JA, Kim CS, Ahn HJ, Yang MK, et al. (2011) Comparison of tracheal intubation with the Airway Scope or Clarus Video System in patients with cervical collars. Anaesthesia 66: 694-698.
-
Hsu HT, Chou SH, Chen CL, Tseng KY, Kuo YW, et al. (2013) Left endobronchial intubation with a double-lumen tube using direct laryngoscopy or the Trachway (R) video stylet. Anaesthesia 68: 851-855.
-
Patane PS, Sell BA, Mahla ME (1990) Awake fiberoptic endobronchial intubation. J Cardiothorac Anesth 4: 229-231.
-
Chastel B, Perrier V, Germain A, Seramondi R, Roze H, et al. (2015) Usefulness of the Airtraq DL videolaryngoscope for placing a double-lumen tube. Anaesth Crit Care Pain Med 34: 89-93.
-
Suzuki A, Kunisawa T, Iwasaki H (2007) Double lumen tube placement with the Pentax-Airway Scope. Can J Anaesth 54: 853-854.
-
El-Tahan MR (2016) Videolaryngoscopes for placement of double lumen tubes: Is it time to say goodbye to direct view? Saudi J Anaesth 10: 218-227.
-
Subramani S, Poopalalingam R (2014) Bonfils assisted double lumen endobronchial tube placement in an anticipated difficult airway. J Anaesthesiol Clin Pharmacol 30: 568-570
-
Bein B, Caliebe D, Römer T, Scholz J, Dörges V, et al. (2005) Using the Bonfils intubation fiberscope with a double-lumen tracheal tube. Anesthesiology 102: 1290-1291.
-
Chen KY, Lin SK, Hsiao CL, Hsu WT, Tsao SL, et al. (2011) Use of a video fiberoptic bronchoscope assist double-lumen endobronchial tube intubation in a patient with a difficult airway. Acta Anaesthesiol Taiwan 49: 26-28.





