International Journal of Brain Disorders and Treatment
External Carotid Artery Steal Syndrome via Occipital-Vertebral Anastomosis
Menarvia Nixon*, Anil Nanda and Hugo Cuellar-Saenz
Department of Neurosurgery, LSUHSC in Shreveport, USA
*Corresponding author:
Menarvia Nixon, MD, Department of Neurosurgery, LSU HSC Shreveport, Shreveport, LA, 71130-3932, USA, Tel: 318-675-8865, Fax: 318-675-6787, E-mail: mnixon@lsuhsc.edu
Int J Brain Disord Treat, IJBDT-1-001, (Volume 1, Issue 1), Case Report; ISSN: 2469-5866
Received: July 29, 2015 | Accepted: August 24, 2015 | Published: August 26, 2015
Citation: Nixon M, Nanda A, Cuellar-Saenz H (2015) External Carotid Artery Steal Syndrome via Occipital-Vertebral Anastomosis. Int J Brain Disord Treat 1:001. 10.23937/2469-5866/1510001
Copyright: © 2015 Nixon M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We describe a case of ECA steal syndrome due to occipital- vertebral anastamosis in an 81 y/o female patient who presented with gait ataxia and dizziness. She was referred to Neuro-interventional Radiology after discovery of carotid bruits on her physical examination. A digital subtraction angiogram confirmed mild internal carotid artery stenosis, however, more concerning was the discovery of retrograde flow of the right vertebral artery with filling of the right external carotid artery via anastomosis with the occipital artery. This flow diversion from the vertebral artery as a result of external carotid artery occlusion was believed to be the cause of her symptoms. A recannulation of the right external carotid artery via angioplasty reversed the flow within the vertebral artery with a resolution of the patient's symptoms.
Keywords
ECA steal syndrome, Cerebral stenting, Occipital-vertebral anastomosis
Introduction
External carotid artery steal syndrome is a constellation of signs and symptoms that arise from retrograde flow of blood in the vertebral artery due to a proximal stenosis (narrowing) and/or occlusion of the external carotid artery [1]. Like subclavian steal syndrome, blood flows in a retrograde direction down the vertebral artery away from the vertebrobasilar circulation, at the expense of the brainstem. Due to this, ECA steal syndrome is characterized by brief ischemic attacks that are marked by dizziness and loss of balance caused by insufficient blood supply to the vertebral and basilar arteries [2].
Occipital-vertebral (O-V) anastomoses have been frequently observed on cadaveric examination of cerebral circulation. However, the O-V anastomoses are less commonly seen in angiographic studies [3]. Some cases of ECA steal have been described with management ranging from conservative to surgical [3-8]. To our knowledge only one other case is found in the literature managed by endovascular therapy [3,8,9]. This case differs from ours in management and etiology of the steal.
Case Illustration
An 81 y/o female patient with a past medical history of coronary artery disease, hypertension and dyslipidemia was referred to the Neurosurgery Department for evaluation and treatment of carotid stenosis. The patient was referred by her Cardiologist due to carotid bruits noted on physical examination. A Doppler ultrasound revealed stenosis of the left internal carotid artery. On presentation to the Neurosurgery Department she reported a 1 year history of dizziness and gait disturbances. Over the past month her symptoms have progressively worsened from dizziness whilst standing to occasional dizziness whilst sitting as well. The patient was scheduled for a cerebral angiogram with possible stenting.
On digital subtraction angiography, the left common carotid artery revealed atherosclerotic changes at the level of the bifurcation with less than 20 percent stenosis of the left carotid bulb. The right common carotid artery injection revealed atherosclerotic changes at the level of the bifurcation. The right internal carotid artery had less than 20 percent stenosis at the level of the carotid bulb. Intracranially, there was no evidence of aneurysm, stenosis or vascular malformation. The right external carotid artery had a 99 percent stenosis at the level of the origin secondary to calcified circumferential plaque. The branches of the external carotid artery were not opacified anterogradely (Figure 1). Selective examination of the right vertebral artery showed collateral flow through anastomosis with the occipital artery that completely opacified all the branches of the right external carotid artery with possible steal phenomenon (Figure 2).
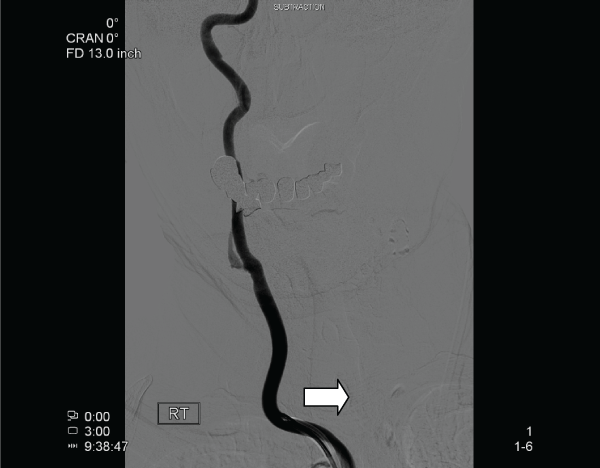
.
Figure 1: Angiogram showing injection of the right common carotid artery with arrow indicating stenosis of the proximal right external carotid artery.
View Figure 1
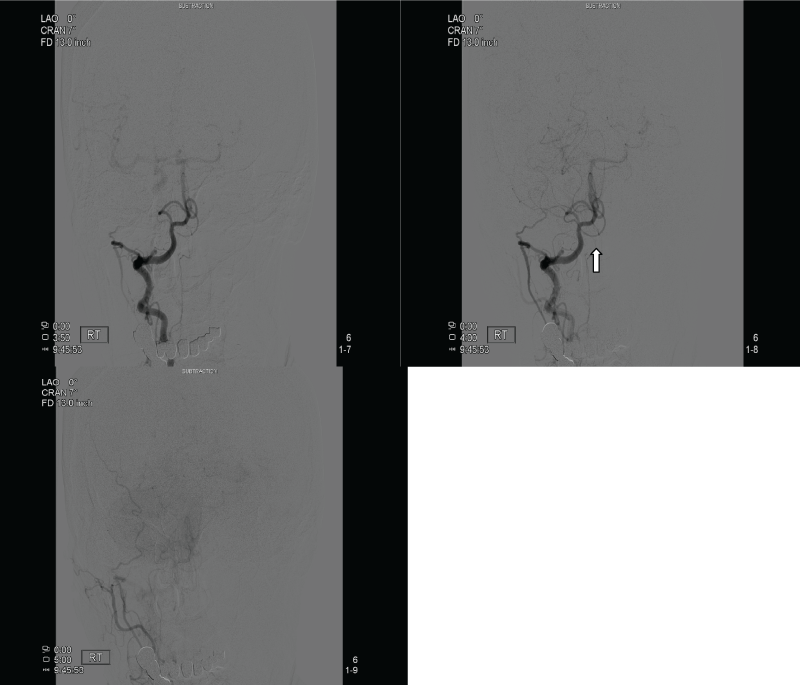
.
Figure 2: Selective examination of the right vertebral artery showing collateral flow through anastomosis with the occipital artery; sequential sequences revealing opacification of the branches of the right external carotid artery.
View Figure 2
Diagnostic angiography revealed a 99 percent stenosis of the origin of the right external carotid artery with retrograde flow from the right vertebral artery opacifying the external carotid artery branches were observed. Since the patient's chief complaint was dizziness and gait disturbances, the steal flow from the right vertebral artery was determined to be the cause of her symptoms. The decision is made to perform angioplasty at the origin of the right external carotid artery. Following angioplasty of the right external carotid artery, antegrade flow was observed (Figure 3a,3b.).Two weeks later, the patient reported resolution of dizziness and ataxia. She was again seen in clinic at 6 months and 1 year without recurrence of symptoms.
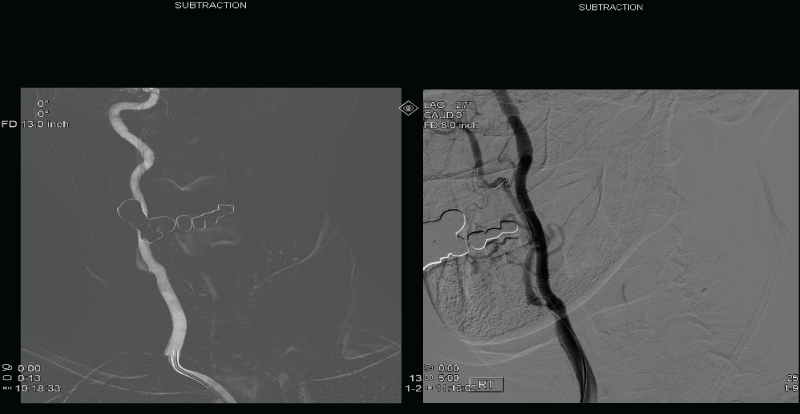
.
Figure 3: On the left, digital subtraction angiogram of balloon entering the right common carotid artery. On the right, antegrade flow of right external carotid artery following angioplasty.
View Figure 3
Discussion
The presence and significance of collateral circulation between the various branches of the intracranial circulation and branches of the extracranial circulation have been described in the literature. Most of these potential collateral channels become obvious when occlusive vascular disease interrupts the normal pathways, and the channels dilate to form alternate routes of blood flow. In general when there is carotid artery occlusion, cerebral blood flow can be achieved by diversion of flow across the vertebra-basilar junction. Retrograde blood flow into the vertebral artery can result in neurologic symptoms. Dizziness is by far the most common neurologic symptom of the steal syndromes, and usually has a spinning or vertiginous character. Dizziness can be accompanied by other signs of hindbrain ischemia including diplopia, oscillopsia, weakness of the lower extremities, staggering, hemiparesis, and numbness [3,4]. The patient described above had transient ischemic attacks representative of ischemic episodes involving the vertebra-basilar system.
Review of the literature reveals a relatively low angiographic incidence of O-V anastomosis. Gito et al. reported 8 cases out of 100 carotid arteriograms [7]. Takahashi reported 4 cases out of 2108 carotid and 315 vertebral arteriograms [8]. Conversely, spontaneous anatomoses have been reported without concomitant obliterative lesions. The first reported case of symptomatic O-V anastomosis was published by Kondo et al in 1980, where they described a patient who presented with recurrent vertebra-basilar insufficiency [9]. After 12 years of recurrent symptoms of right sided hemiparesis and paresthesias, an angiogram revealed a large single anastomotic channel between the left occipital and left vertebral artery at the level of C1. There were no atherosclerotic changes or obliterative lesions in this patient, however, after surgical obliteration of this channel via clipping there was rapid postoperative improvement of his clinical symptoms [9]. Twenty years later, Harada et al published a case of ECA steal syndrome due to occipital-vertebral anastomosis in a patient who presented with syncope and recurrent episodes of dizziness. In this case the anastomotic channel was endovascularly obliterated with platinum coils [5].
In reference to the treatment options for symptomatic O-V anastamoses, medical management, and to a lesser degree, surgical obliteration was considered the mainstay of treatment. Surgical intervention consisted of either placing a clip on the anastomotic channel or bypass of the channel with a vein graft to induce occlusion. With regards to external carotid artery stenosis/occlusion, the mainstay of treatment involved ECA endarterectomy or angioplasty/stenting. Indications for ECA endarterectomy include ipsilateral transient ischemic attacks (hemispheric or ocular) in patients with occlusion of the ipsilateral internal carotid artery and severe external carotid artery stenosis; occlusion of the ipsilateral internal carotid artery and moderate stenosis of the external carotid artery with ulceration; or ipsilateral transient ischemic attacks with a nonstenotic ipsilateral external carotid artery and thrombus within the cul-de-sac of the occluded ipsilateral internal carotid artery [9]. The most clear-cut indication for external carotid artery endarterectomy is monocular amaurosis fugax in patients with ipsilateral internal carotid artery occlusion and a microembolic source in the origin of the external carotid artery or the occluded carotid sinus. However, with the lack of these criteria it was decided that the patient avoids undergoing a major surgical procedure. Due to its relatively recent development in the treatment of cerebrovascular disease, the durability of external carotid artery angioplasty has yet to be determined. Moreover, with current interest and emphasis on endovascular treatment of cerebrovascular disease and with improvements in endovascular procedures, a clearer demonstration of these collateral channels is now more frequently recognized and treated [9]. Endovascular obliteration for the treatment of ECA steal syndrome can range from coil-assisted occlusion as mentioned above or simply treatment of the occlusive disease as in this case illustration.
Conclusion
We conclude that anastomotic channels with or without concomitant occlusive disease can result in intracranial steal phenomenon. Depending on the direction and rate of flow within these channels, a number of neurologic sequelae can occur. Endovascular treatment of symptomatic anastomoses is a safe and effective method of therapy, as witnessed by the disappearance of this patient's symptoms after treatment.
Contributorship Statement
Menarvia Nixon provided the abstract, case illustration, discussion, figures and editing. Anil Nanda assisted with final editing. Hugo Cuellar-Saenz provided the introduction and assisted with final editing.
References
-
Reivich M, Holling E, Roberts B, Toole JF (1961) Reversal of blood flow through the vertebral artery and its effect on cerebral circulation. N Engl J Med 265: 878-885.
-
Sharma VK, Chuah B, Teoh HL, Chan BP, Sinha AK, et al. (2010) chronic brainstem ischemia in subclavian steal syndrome. J Clin Neurosci 17: 1339-1341.
-
Schechter MM (1964) The Occipital-Vertebral Anastomosis. J Neurosurg 21: 758-762.
-
Oguzkurt L, Kizilkilic O, Tercan F, Turkoz R (2005) Yildirim T Vertebrocarotid collateral in extracranial carotid artery occlusions: digital subtraction angiography findings. Eur J Radiol 53: 168-174.
-
Harada J, Kuwayama N, Nishijima M, Okamoto S, Kubo M, et al. (2000) Symptomatic occipital-vertebral anastomosis - a case report. Interv Neuroradiol 6: 317-320.
-
Kostanian VJ, Mathews MS, Westhout FD, Yu W (2007) Facial steal syndrome: identification and endovascular management. Neuroradiol J 20: 85-88.
-
Gito Y, Miyasaka K (1975) Occipito-vertebral anastomosis. Jpn J Clin Radiol 20: 17-22.
-
Takahashi H, Yamaguchi K, Uemura K, Kowada M, Matsuoka S (1971) Four cases of occipital-vertebral anastomosis. No to Shinkei 23: 1315-1319.
-
Kondo A, Koyama T, Ishikawa J, Yamasaki T (1980) Occipito-vertebral anastomosis; its clinical significance. Neurol Med Chir 20: 61-66





