Journal of Dermatology Research and Therapy
Split Face Comparative Study of using Fractional Erbium: Glass 1540 Nanometer and Nd: YAG Q-Switched 1064 Nanometer Laser Systems in the Treatment of Melasma
Azar Hadi Maluki1* and Haider Abdulrasool Al-Sabak2
1Laser Research Unit, College of Medicine, University of Kufa, Iraq
2Dermatology Department, College of Medicine, University of Kufa, Iraq
*Corresponding author:
Azar H. Maluki, Laser Research Unit, College of Medicine, University of Kufa, P.O. Box (450), AL-Najaf Post Office, Iraq, Tel: (+964)7802887712, E-mail: azarmaluki@gmail.com
J Dermatol Res Ther, JDRT-1-002, (Volume 1, Issue 1), Original Article; ISSN: 2469-5750
Received: March 24, 2015 | Accepted: May 12, 2015 | Published: May 14, 2015
Citation: Maluki AH, Al-Sabak HA (2015) Split Face Comparative Study of using Fractional Erbium: Glass 1540 Nanometer and Nd: YAG Q-Switched 1064 Nanometer Laser Systems in the Treatment of Melasma. J Dermatol Res Ther 1:002. 10.23937/2469-5750/1510002
Copyright: © 2015 Maluki AH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Melasma is a common skin problem and laser started to be an option of treatment.
Objective: To compare between the effectiveness of Erbium: Glass 1540 nm laser and Nd: YAG Q-Switched 1064nm laser in the treatment of melasma.
Methods: This comparative split face clinical study was carried out in Laser Research Unit, College of Medicine, University of Kufa, Iraq; for the period from October 2012 to December 2013. Each patient's face was divided into two halves, each half was treated with one of the two laser devices used in this study; Fractional Erbium: Glass 1540nm and Nd: YAG Q-Switched 1064nm lasers. The severity of melasma was assessed before, after treatment and 3 months later with the Modified Melasma Area and Severity Index (MASI) Score and by photographs.
Results: The mean Modified MASI scores were reduced in the facial halves treated by Erbium: Glass 1540nm laser (statistically highly significant P value of 0.001) more than those treated by Nd: YAG Q-Switched 1064nm laser (statistically significant P value of 0.022).
Conclusion: The treatment was well tolerated and patients demonstrated positive responses with promising results.
Keywords
Melasma, Erbium, Glass laser, Nd, YAG Q-Switched laser
Introduction
Melasma is a relatively common disorder of hyperpigmentation that affects sun exposed areas of skin, most commonly the face. It most often affects women, particularly with darker complexions, and who live in areas of intensive ultraviolet radiation exposure [1]. Melasma is characterized by brown sharply demarcated patches, typically on the malar prominences and forehead.
Melasma occurs frequently during pregnancy and there is a strong association with birth control pills uses [2]. In Iraq, melasma is considered as the most common pigmentary problem and is seen in 26.6% of Iraqi females with a mean age of onset of 26.6 years [3,4]. Successful treatment of melasma involves the triad of sun block, bleaching agents and time [3]. Different modalities of topical bleaching agents [5-7], antioxidants [8], and chemical peels [9] have been tried. Zinc sulphate and tranexamic acid [10,11] may also have a role.
Laser therapy has been used for the treatment of melasma in many countries with promising results. The Nd: YAG Q- Switched 1064nm laser has better results on dermal pigments than the 532nm wave length of same laser [12]; and epidermal melasma responds better than dermal or mixed types. The Erbium: Glass 1540 nm laser is fractional non-ablative type, with a mid-infrared range that has also been used for amelioration of fine facial rhytides and atrophic facial scars. Similar to other infrared laser systems, Erbium: Glass laser targets also intracellular water and penetrates tissue to a depth of 0.4-2mm [13]. Recently, it has been used as treatment for melasma with conflicting results. Indeed, the first clinical studies reported significant improvement in melasma with this type of laser, and were corroborated by the decrease in melanocytes compared to the pre-treatment histological specimens [14].
Patients and Methods
This therapeutic comparative split face study was carried out in the Laser Research Unit, College of Medicine, University of Kufa, Iraq; for the period from October 2012 to December 2013.
Thirty eight patients with melasma were enrolled in this study. The inclusion criteria included patients with melasma of different facial types who attended for laser treatment. All patients should not receive any treatment for melasma for the last two months except for sun block.
The exclusion criteria included patients with skin types V and VI, past or recent history of skin tumors, personal or family history of hypertrophic scar and keloid formation, the presence of chronic systemic disease, immune suppressed patients, pregnant and lactating women, females on contraceptive pills and those on concurrent treatment with other depigmenting agents.
A detailed history was taken from each patient including the name, sex, age, occupation, disease onset, history of pregnancy, contraceptive pills, and details of sun exposure. Drug history and any other exacerbating factors were also recorded.
A careful physical examination for all patients was done including site, pattern, color, homogeneity of melasma and the surface area involved. Wood's light (Waldmann Medizintechnik Co., Germany) examination was performed for all patients to assess the depth of pigmentation and type of melasma.
This study was approved ethically by the Scientific Committee of Dermatology and Venereology, Iraqi Board for Medical Specializations; and all patients signed a written formal consent.
Treatment Protocol
Thirty eight patients (32 females and 6 males) were included in the study. Each patient's face was divided into two halves, right and left, each half was treated with one of the two laser devices used in this study:
Erbium : Glass laser 1540nm
(Quanta system - DNA laser technology - MATISSE),
Non-ablative, fractional, flat tip, pulse duration 7ms, frequency 1Hz, and energy 6.3mj; with expected skin depth of 150um.
Nd : YAG Q-Switched 1064nm
(Quanta system - DNA laser technology - ULTRALIGHT),
Low fluence of 10J/cm2, tip 2mm, and frequency 5Hz.
Total number of sessions for each patient was eight, at a two-week interval. During laser therapy, the patients were instructed to lie in supine position on the couch and to wear the special goggles for eye protection with no local anesthesia was used. All facial sites affected by melasma were treated including: the forehead, malar areas and chin. The probe of each laser device was held perpendicular on the patients faces. Treatment with Erbium glass laser was performed by the continuous sliding technique; the laser beam was preceded by the cooling piece. The selected skin depth was estimated to be 100um in the first four sessions increasing to 150um in the last four sessions; so approaching the limits of upper dermis. This depth was the maximum tolerable setting used with the lowest side effects. While the probe of Nd: YAG laser was held separated from the patient faces at a fixed distance through a metallic guide connected to the machine handle. All patients were asked about any pain or discomfort during laser treatment. At the end of each session, the treated sites were observed, and the early skin reactions to laser treatment were recorded.
Post-Treatment Instructions
All patients were instructed to avoid sun exposure and a sun screen of sun protection factor (SPF) of 30 or more was prescribed, during the treatment and follow up periods. Also the patients were asked not to try any other topical facial therapy during the study period. Patients who complained of discomfort and erythema were given topical skin emollient.
Follow Up
The patients were seen regularly every two weeks during the treatment period and at each visit the side effects were recorded. The patients were followed up monthly for three months after the last treatment session to look for any complication or any sign of relapse.
Evaluation
All the treated patients were evaluated objectively and subjectively regarding their response to treatment with both laser types, by the following methods:
Objective methods
A. Modified MASI score: Melasma severity was scored with the Modified Melasma Area and Severity Index "Modified MASI". In this system the face is divided into two halves, right and left. Each half is further subdivided into three parts, forehead, malar area and chin. Then melasma in each of these parts is graded depending on three variables:
Percentage of the total area involved on a scale: this was measured by using transparent square paper. By this method the melasma and the total face surface areas were measured accurately by square centimeters, then the percentage of the total melasma area relative to the total area of the face was measured and scoring was done as follow:
| 0 | No involvement |
| 1 | < 10% |
| 2 | 10-29% |
| 3 | 30-49% |
| 4 | 50-69% |
| 5 | 70-89% |
| 6 | >90-100% |
Darkness
scoring from 0-4 was assessed according to 4 special color charts:

Scale 0= no melasma
Scale 1= light brown
Scale 2= brown
Scale 3= dark brown
Scale 4= black
Homogeneity
on scale 0(minimal) to 4(maximal).
So the Modified MASI score in each half of the face was calculated by the following equation:
Forehead (A+D+H) + Malar (A+D+H) + Chin (A+D+H)
Whereas A is area, D is darkness and H is homogeneity.
So Modified MASI score was measured for each half of the patient's faces at baseline, after two weeks from the last laser session and at three months later.
B. Photographic assessment: Color photographs for each patient were taken at base line, and after completing all the eight sessions of laser therapy; using Sony-digital, high sensitivity, 9.1 mega pixel, DSC-HX1 still camera; in the same place with fixed illumination and distance.
Subjective method: Patient's satisfaction to response to therapy was evaluated on a score of 3 points as follows:
(1) Full satisfaction.
(2) Partial satisfaction.
(3) No satisfaction.
Results
Twenty nine out of thirty eight patients completed all eight sessions of treatment, and the other nine patients were defaulted from the study due to different causes including pregnancy, poor compliance for treatment, and for unknown causes.
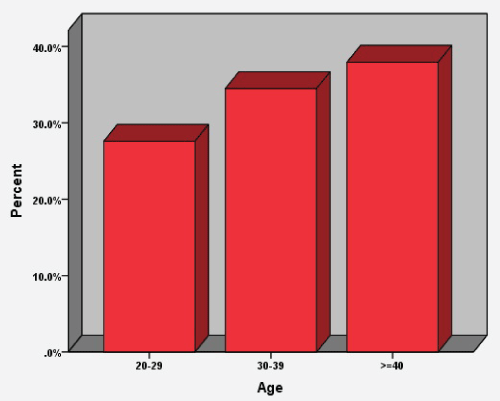
There were 25 (86.21%) females and 4 (13.79%) males as in (Figure 1). Their ages ranged from 23-48 years with mean of 35.2 ± 7.2SD years as in (Figure 2).
Regarding skin types, all patients were Fitzpatrick's skin types III and IV, with different melasma patterns and all of them showed negative Wood's light examination indicating dermal and mixed types of melasma (Figure 3).
Total number of sessions for each patient was eight, at a two-week interval. In each session both laser systems were used for each patient; Erbium: Glass 1540nm on one half of the face and Nd: YAG QSW 1064 nm on the other half, and continuing the same protocol for all sessions of each patient.
Evaluation
Each patient was assessed objectively at baseline, after treatment and three months later by two methods: Modified MASI score (Table 1), and photographs (Figure 4,5).
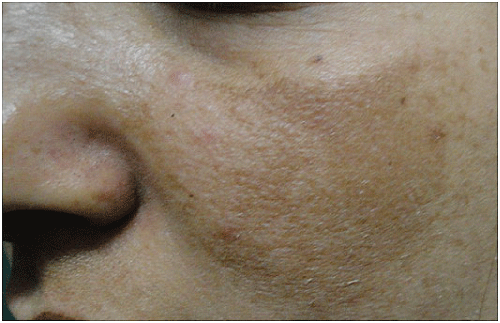
.
Figure 4A: Left malar melasma. Forty two years old lady before treatment by Erbium: Glass 1540nm laser
View Figure 4A
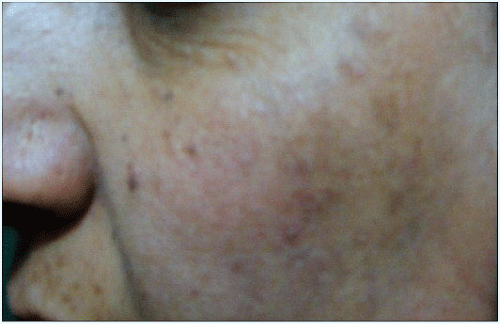
.
Figure 4B: Same patient as in Figure 4A. Improvement of melasma after eight treatment sessions by Erbium: Glass 1540nm laser
View Figure 4B
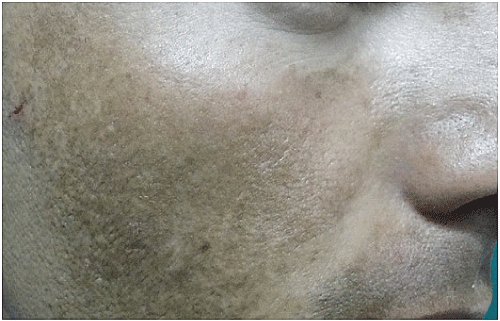
.
Figure 5A: Right malar melasma. Twenty three years old male before treatment by Nd: YAG Q-Switched 1064nm laser
View Figure 5A
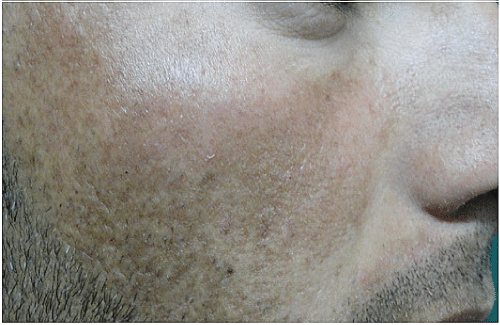
.
Figure 5B: Same patient as in Figure 5A. Mild improvement of melasma after eight treatment sessions using Nd: YAG Q-Switched 1064nm laser
View Figure 5B
![]()
Table 1: Modified MASI Score and other clinical characteristics of the studied patients
View Table 1
Subjective assessment was done by asking each patient about his or her satisfaction degree to the improvement of melasma in each half of the face separately Tables 2-4.
![]()
Table 2: Mean Modified MASI score before and after laser treatment
View Table 2
![]()
Table 3: Mean difference of Modified MASI score between both laser systems
View Table 3
![]()
Table 4: Percentage of patients' satisfaction
View Table 4
Statistical analysis
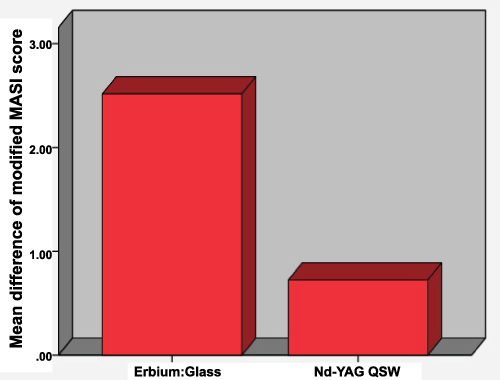
Statistical analysis was done by using SPSS version 20 in which paired sample and independent sample T-test were used to compute P value; and P value of less than 0.05 was regarded as statistically significant. The Modified MASI score was reduced in the facial halves treated by Erbium: Glass laser from mean of (14.89 ± 6.11SD) before treatment to mean of (12.37 ± 6.03SD) after treatment, with statistically highly significant P value (P=0.001). While in facial halves treated by Nd: YAG laser the Modified MASI score was also reduced from mean of (15.34 ± 6.06SD) before treatment to mean of (14.62 ± 5.6SD) after treatment, but with statistically significant P value (P=0.022), as in (Table 2). There was a high difference in the degree of reduction of Modified MASI score between both laser systems; in a way that the reduction in mean Modified MASI of Erbium: Glass laser was (2.51 ± 1.49SD), while that of Nd: YAG laser was (0.72 ± 1.60SD). This difference was statistically significant (P value=0.015), as in (Table 3) and (Figure 3).
Side effects
All treated patients developed transient erythema and burning sensation lasting not more than 2 days after each session in both sides of face, while only three patients (10.3%) developed mottled post inflammatory hyper pigmentation in the facial halves that were treated by Nd: YAG laser only then improved spontaneously at the end of follow up period.
Follow up
Three months after the last treatment session, the Modified MASI score was elevated in most of the patients in both facial halves and reached to the pre-treatment score. This elevation in the score was statistically not significant in both Erbium: Glass laser (P value=0.477), and in Nd: YAG laser (P value=0.155), as in (Table 5).
![]()
Table 5: Mean Modified MASI score after three months follow up
View Table 5
Discussion
Since laser therapy started nowadays to achieve a revolutionary role in the treatment of pigmentary skin diseases, many therapeutic laser trials have been explored with variable results on melasma worldwide [14,15].
Tourlaki et al. used a combination of fractional Erbium: Glass laser and topical therapy in melasma patients who are resistant to triple combination cream and concluded that this regimen was logical and effective therapy, but its long term efficacy was limited [14]. Manela-Azulay M and Borges J used fractional Erbium: Glass 1540nm laser alone and showed 50-100% improvement in their patients [15].
Manaloto and Alster used Erbium: YAG resurfacing which effectively improved melasma, but with marked post inflammatory hyper pigmentation (PIH), so they concluded that this type of laser could be only used for refractory melasma [16].
Suh et al. used Q-switched Nd: YAG 1064nm and found that it was safe and effective modality for treating melasma in Asian peoples [17]. Bevec et al. treated successfully melasma with low fluence Q-switched Nd: YAG laser but with high recurrence rate [18]. Kar et al. concluded that low fluence mode of Q-switched Nd: YAG laser was more effective than the high fluence mode in the treatment of melasma with the least side effects [19].
The choice of laser systems in the present study depended on previous studies and on the fact that both Erbium: Glass and Nd: YAG QSW lasers are nonsurgical modes with minimum downtime.
The mechanism of action of these laser types is different and this explains the differences in improvement of melasma between them. Erbium: Glass laser acts on rejuvenation of skin through its photo thermal activity, so improving collagen and elastic fibers integrity which will have positive influence on skin texture and pigment reduction; along with the creation of thermal micro columns in the skin that eliminate excess pigmentation and preserve healthy skin [15].
On the other hand the photomechanical effect of Nd: YAG Q-Switched laser leads to fragmentation of melanosomes and dispersion of the pigment in the cutaneous tissue because of thermal gradient between melanosome and the surrounding tissue, through both photo thermal and photomechanical effects [20,21].
This might explain the mottled hyper pigmentation that developed on one side of the faces of three patients treated by Nd: YAG Q-Switched laser while the other side of those faces treated by Erbium: Glass laser did not show such hyper pigmentation; otherwise all patients developed transient erythema and mild burning sensation lasting for a couple of days following each session on both sides of the faces.
Using low fluence Nd: YAG Q-Switched 1064 nm laser in this study was aimed to overcome the possible post inflammatory hyper pigmentation that is closely associated with the use of this type of laser on the skin.
Wood's light examination was negative in all studied patients, so reflecting that their melasma was either dermal or mixed type. Accordingly after three months follow up period the recurrence rate of melasma was high in the most of the patients especially on the sides treated with Nd: YAG Q-Switched laser. The P value of follow up results was statistically not significant in both types of laser.
Modified MASI score used in this study facilitated an accurate objective method for evaluating the results of laser treatment, through dividing the faces into two halves and doing split face comparative treatment using two modes of laser systems in the same patient.
Recurrence of melasma in the follow up period in this study may be attributed to the following causes: absence of combination therapy of laser with other topical preparations like hydroquinone and steroids unlike most previous studies; the nature of melasma and its close relationship to UV light exposure; and the impact of genetic background on melasma patients.
Conclusion
In general this laser therapy was well tolerated and the patients demonstrated positive responses with promising results. Erbium: Glass 1540nm laser was more effective than Nd: YAG Q-Switched 1064nm laser in the treatment of melasma despite of the high recurrence rate of disease reported after both laser types.
References
-
Kauh YC, Zachian TF (1999) Melasma. Adv Exp Med Biol 455: 491-499.
-
Odom RB, James WD, Berger TG (2000) Disturbances of pigmentation. In: Odom RB, James WD, Berger TG. Andrews Diseases of the Skin, clinical Dermatology. (9th edn) W.B. Saunders Company, Philadelphia: 1058-1059.
-
Mosher DB, Fitzpatrick TB, Ortonne JP, Hori Y (2008) Hypomelanosis and hypermelanosis. In: Freeberg UM, Eisen AZ, Wolff K, Austen KF, Goldsmith LA, et al. (7th edn) Fitzpatrick's Dermatology in General Medicine, McGraw-hill, New York: 996-997.
-
Sharquie KE, Dhahir SA (2000) Melasma in Iraqi women, a Clinical, Histopathological and Histochemical Study. J Pan-Arab League Dermatologists 3: 111-117.
-
Palumbo A, d'Ischia M, Misuraca G, Prota G (1991) Mechanism of inhibition of melanogenesis by hydroquinone. Biochim Biophys Acta 1073: 85-90.
-
Fitton A, Goa KL (1991) Azelaic acid. A review of its pharmacological properties and therapeutic efficacy in acne and hyperpigmentary skin disorders. Drugs 41: 780-798.
-
Nakagawa M, Kawai K, Kawai K (1995) Contact allergy to kojic acid in skin care products. Contact Dermatitis 32: 9-13.
-
Huh CH, Seo KI, Park JY, Lim JG, Eun HC, et al. (2003) A randomized, double-blind, placebo-controlled trial of vitamin C iontophoresis in melasma. Dermatology 206: 316-320.
-
Sharquie KE, Al-Tikreety MM, Al-Mashhadani SA (2005) Lactic acid as a new therapeutic peeling agent in melasma. Dermatol Surg 31: 149-154.
-
Wu S, Shi H, Wu H, Yan S, Guo J, et al. (2012) Treatment of melasma with oral administration of tranexamic acid. Aesthetic Plast Surg 36: 964-970.
-
Na JI, Choi SY, Yang SH, Choi HR, Kang HY, et al. (2013) Effect of tranexamic acid on melasma: a clinical trial with histological evaluation. J Eur Acad Dermatol Venereol 27: 1035-1039.
-
Grevelink JM, Duke D, van Leeuwen RL, Gonzalez E, DeCoste SD, et al. (1996) Laser treatment of tattoos in darkly pigmented patients: efficacy and side effects. J Am Acad Dermatol 34: 653-656.
-
Alster TS, Lupton JR (2002) Are all infrared lasers equally effective in skin rejuvenation. Semin Cutan Med Surg 21: 274-279.
-
Tourlaki A, Galimberti MG, Pellacani G, Bencini PL (2012) Combination of fractional erbium-glass laser and topical therapy in melasma resistant to triple-combination cream. J Dermatolog Treat 25: 218-222.
-
Manela-Azulay M, Borges J (2011) Treating Melasma with 1540nm fractional non-ablative erbium laser: a pilot study. Surg Cosmet Dermatol 3: 313-318.
-
Manaloto RM, Alster T (1999) Erbium:YAG laser resurfacing for refractory melasma. Dermatol Surg 25: 121-123.
-
Suh KS, Sung JY, Roh HJ, Jeon YS, Kim YC, et al. (2011) Efficacy of the 1064-nm Q-switched Nd:YAG laser in melasma. J Dermatolog Treat 22: 233-238.
-
Bevec T (2011) Treating melasma with sub-thermolytic Q-Switched Nd:YAG. Journal of Laser and Health Academy: 53-55.
-
Kar HK, Gupta L, Chauhan A (2012) A comparative study on efficacy of high and low fluence Q-switched Nd:YAG laser and glycolic acid peel in melasma. Indian J Dermatol Venereol Leprol 78: 165-171.
-
Cencic B, Lukac M, Marincek M, Vizintin Z (2010) High fluence, high beam quality Q-switched Nd:YAG laser with optoflex delivery system for treating benign pigmented lesions and tattoos. J LAHA 2010: 9-18.
-
Kim YJ, Whang KU, Choi WB, Kim HJ, Hwang JY, et al. (2012) Efficacy and safety of 1,064nm Q-switched Nd:YAG laser treatment for removing melanocytic nevi. Ann Dermatol 24: 162-167.