Journal of Dermatology Research and Therapy
Vancomycin Hypersensitivity Reaction Presenting with Extensive Oral Ulcerations
Justin G. Hastings1, Alok Vij2 and Anthony P. Fernandez2,3*
1Department of Medicine, Mercy St. Vincent Medical Center, USA
2Department of Dermatology, Cleveland Clinic, Cleveland, USA
3Department of Anatomic Pathology, Cleveland Clinic, USA
*Corresponding author:
Anthony P. Fernandez M.D, PhD, Director of Medical Dermatology, Departments of Dermatology and Anatomic Pathology, Cleveland Clinic, 9500 Euclid Avenue; A61, Cleveland, Ohio 44195, USA, Tel: (216) 445-8776, Fax: (216) 636-5150, E-mail: Fernana6@ccf.org
J Dermatol Res Ther, JDRT-1-004, (Volume 1, Issue 1), Case Report; ISSN: 2469-5750
Received: March 15, 2015 | Accepted: August 13, 2015 | Published: August 15, 2015
Citation: Hastings JG, Vij A, Fernandez AP (2015) Vancomycin Hypersensitivity Reaction Presenting with Extensive Oral Ulcerations. J Dermatol Res Ther 1:004. 10.23937/2469-5750/1510004
Copyright: © 2015 Hastings JG, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Vancomycin therapy can be associated with a hypersensitivity reaction characterized by fever, rash, neutropenia, and other variable manifestations. Here we report a 45-year old man who developed diffuse aphthous-like ulcers as the most prominent manifestation of vancomycin hypersensitivity reaction.
Keywords
Vancomycin, Hypersensitivity, Oral, Ulcers, Aphthous, Neutropenia
Introduction
Vancomycin therapy is associated with several hypersensitivity reactions, the most common being the non-immunologically mediated "red man syndrome." Fever, rash, neutropenia, and other manifestations have also been variably associated with a vancomycin hypersensitivity reaction that is likely immunologically mediated. Here we report a 45-year old man who developed diffuse oral aphthous-like ulcers as the most prominent manifestation of vancomycin hypersensitivity reaction. We identified only two previously reported cases of vancomycin hypersensitivity reaction involving oral lesions. Although the exact pathogenic mechanisms underlying aphthous ulcers and hypersensitivity reactions to vancomycin are not completely understood, both potentially involve Th-1 mediated cellular responses.
Case Synopsis
Our dermatology service was consulted to examine a 45 year-old Caucasian man hospitalized with a 2-week history of fever, 30lb weight loss, and progressively worsening oral ulcers. He had been diagnosed with amethicillin-resistant Staphylococcus aureus (MRSA) paraspinal abscess and was started on IV vancomycin following drainage 25 days prior to admission. After 2 weeks of vancomycin treatment, he acutely developed multiple oral ulcerations, tongue swelling, and odynophagia. He denied vesicles or prodromal burning or tingling. Review of systems was negative for arthralgias, shortness of breath, abdominal pain, and diarrhea. His PCP prescribed nystatin swish-and-swallow and oral fluconazole for presumed oral candidiasis but the progressively developed more oral ulcerations and worsening pain, limiting food intake. Eventual consultation with an Infectious Disease physician led to hospitalization for presumed orolabial herpes and intravenous acyclovir initiation. His past medical history (PMH) was significant for recurrent oral aphthous ulcerations every 4-6 months, but no episode was associated with more than three aphthae. He denied history of orolabial herpes, Crohn's disease or medications besides vancomycin.
On examination, he appeared uncomfortable and had difficulty speaking. Vital signs revealed 100.5℉ temperature and tachycardia. Involving his lips, tongue, buccal mucosa, and posterior pharynx were numerous well-circumscribed ulcerations with fibrinous bases and surrounding erythema (Figure 1A,1B). His tongue was edematous. Facial edema, rash, and ocular/genital abnormalities were absent and physical examination was otherwise normal. Complete blood count revealed anemia and leukopenia, with both neutropenia at 620/μL (normal, 1450-7500/μL) and lymphopenia at 390/μL (normal, 1000-4000/μL). C - reactive protein was 17.9mg/dl (normal, 0-1mg/dL). His eosinophil count was normal and there was no evidence of transaminitis or acute renal insufficiency.
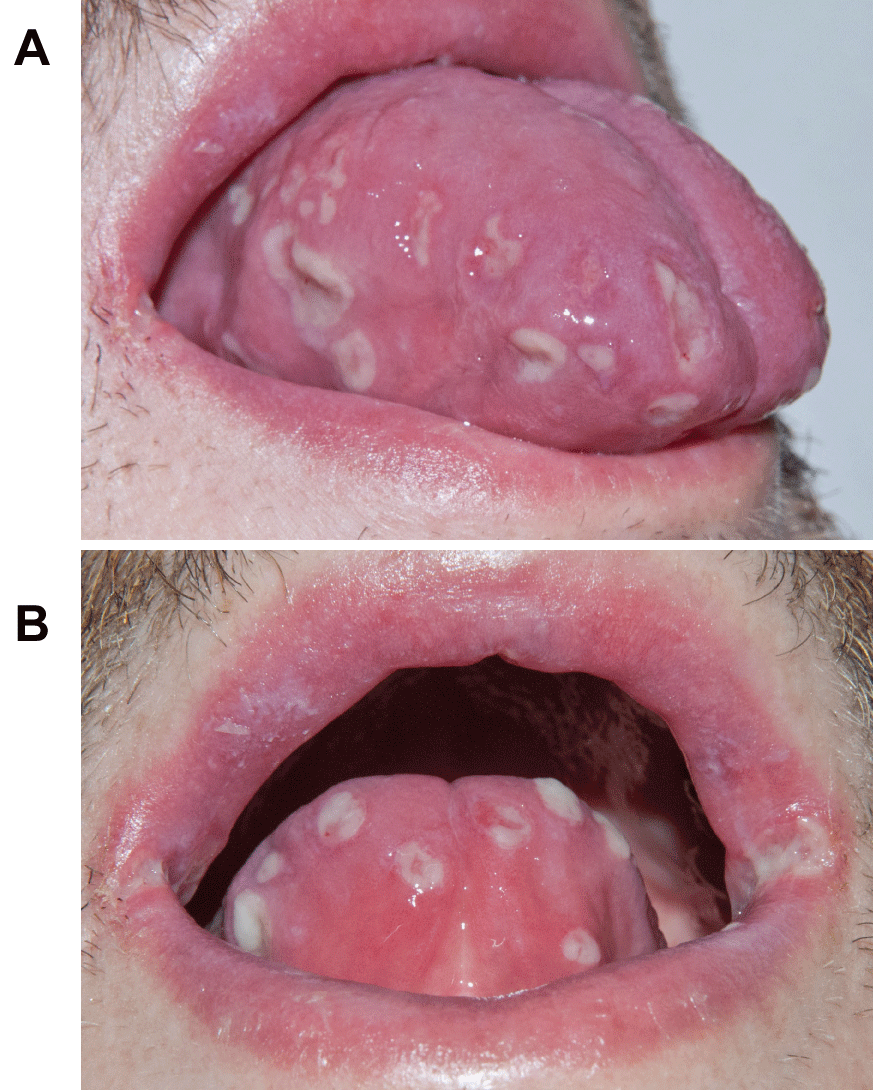
.
Figure 1A and 1B: Anterior and lateral views demonstrating numerous, variably-sized ulcerations with fibrinous bases and surrounding erythema involving the dorsal, ventral, and lateral aspects of the tongue, as well as the lips and oral commissures.
View Figure 1A and 1B
The combination of fever, neutropenia, and lymphopeniain association with recent vancomycin initiation made us suspicious his diffuse oral ulcerations were a manifestation of a vancomycin hypersensitivity reaction. Several oral ulceration swabs were submitted for Herpes simplex virus/Varicella Zoster virus direct fluorescent antibody screen and culture, all of which were negative. Biopsy was deferred by the patient due to severe oral discomfort. Acyclovir and vancomycin were stopped. He was switched to daptomycin and initiated on IV methylprednisolone 60mg daily. Within 36 hours, fever and cytopenias resolved, and the oral ulcerations were almost completely healed. No recurrence of fever, leukopenia, or aphthous ulcerations occurred followingmethylprednisolone discontinuation. Follow-up with the patient more than 24 months following this outbreak reveals no recurrence of diffuse oral ulcerations, although he does continue to develop occasional aphthous ulcerations as in the past.
Discussion
We herein describe a patient that developed diffuse aphthous-like oral ulcerations as the most prominent manifestation of a vancomycin hypersensitivity reaction. Hypersensitivity reactions to vancomycin are rare and generally of two types. The most common and well-known is "red man syndrome," characterized by flushing, erythema, and pruritus attributed to non-immune-mediated histamine liberation from mast cells [1]. The other reported hypersensitivity reaction manifests mainly as neutropenia, but is occasionally associated with fever and/or additional clinical manifestations such as rash and/or eosinophilia [2]. However, variable clinical manifestations make it difficult to recognize.
Isolated neutropenia occurs in 2-12% of patients receiving vancomycin therapy [2,3]. Rarely, vancomycin-induced neutropenia is additionally associated with fever and/or other clinical manifestations. Vancomycin-induced neutropenia, both with/without fever or other clinical symptoms, typically occurs only after prolonged vancomycin administration (>2 weeks) and resolves within 2-5 days after vancomycin cessation [2]. Whether involving fever and other clinical manifestations or not, this vancomycin hypersensitivity reaction type is thought to be immunologically-mediated [2,3]. One hypothesis argues this hypersensitivity reaction type is caused by immune-mediated peripheral neutrophil destruction and aberrant cytokine release [2,4,5]. Another hypothesis argues that, under certain circumstances, vancomycin is oxidized to a reactive metabolite that binds tissue macromolecules to form haptens, which stimulate T-cells to destroy neutrophils and promote other manifestations [2,6]. The true pathogenesis is poorly understood.
We identified two other potential vancomycin hypersensitivity reactions that included oral manifestations. One patient developed necrotic oral mucosal lesions, fever, neutropenia, rash, and eosinophilia on vancomycin treatment day 15 [4]. The other patient had systemic lupus erythematosus (SLE) patient and developed fever, tachycardia, oral ulcers, and rapidly spreading rash after 3 weeks of vancomycin therapy [5]. The latter patient's clinical findings were attributed to an SLE flare because a skin biopsy showed direct immunofluorescence (DIF) findings suggestive of a lupus band. However, a vancomycin hypersensitivity reaction is also possible given symptoms resolved with prednisone and vancomycin discontinuation, and since DIF findings could have been unrelated to the acute rash, but rather the known underlying SLE. Neither report included photographs of patients' oral manifestations or mentioned whether patients had a history of aphthae.
Numerous diseases are associated with acute onset of multiple oral aphthous-like ulcerations and it was important to consider these in our patient. Absence of prodromal symptoms, no antecedent history of orolabial herpes, and negative HSV/VZV DFA and culture, in association with acute hematologic abnormalities, strongly argue against the possibility of acute orolabial herpes. The diffuse ulcerations, in concert with the absence of co-existing fever, neutropenia, or recurrent infections with past episodes of aphthae argue against either a coincidental routine outbreak or aphthae associated with undiagnosed cyclic neutropenia. Absence of associated genital ulcers, uveitis, or rash argues against Behcet's disease. Absence of abdominal pain and gastrointestinal symptoms argue against pyostmatitis vegetans. Finally, absence of rash, peripheral eosinophilia, transaminitis or acute renal insufficiency as well as lack of recurrence after only several days of methylprednisolone, argue against DRESS (drug rash with eosinophilia and systemic symptoms) syndrome.
We also considered the possibility of vancomycin-induced linear IgA bullous dermatosis (LABD). Although histology would have helped definitively rule this out, numerous clinical findings strongly argue against this possibility in our opinion. For one, the oral ulcerations clinically were not consistent with an autoimmune bullous disorder, which typically display thin, bloody superficial ulcerations as opposed to deeper ulcers with fibrinous bases and non-inflammatory borders. Also, mucosal involvement does not generally appear to be a prominent feature of vancomycin-induced LABD. Only about 36% of all patients reported have had mucosal involvement [7]. Even of cases that mimicked toxic epidermal necrolysis, a disease that classically involves the oral mucosa, only 8/13 cases (61.5%) that mentioned oral mucosal examination noted involvement [8]. Additionally, median time to healing for patients with vancomycin-induced LABD has been reported to be 20 days, whereas our patient healed in about 36 hours [9]. Most importantly, though, our patient lacked a cutaneous rash. To our knowledge a case of vancomycin-induced LABD without a cutaneous rash has never been reported [7-10] and it is extremely rare for patients with vancomycin-induced LABD to lack visible cutaneous bullae in addition to other morphologic cutaneous abnormalities [10].
Our patient's clinical and serologic findings, along with a prompt response to methylprednisolone and discontinuation of vancomycin are most consistent with a diagnosis of vancomycin hypersensitivity reaction-associated diffuse oral ulcerations. Finally, lack of recurrence after methylprednisolone discontinuation argues against another disorder transiently masked by this medication. Given the above, the Naranjo probability scale indicates a probable relationship (score=6) between development of the oral aphthous-like ulcerations and vancomycin use in our patient [11].
The pathogenesis of oral ulcerations in our patient is unknown. Although pathogenesis of aphthous ulcerations, in general, is not completely understood, Th1-mediated inflammatory cytokines such as IFN-γ, TNF-α, and IL-6 are increased in aphthous ulcer lesional mucosa [12]. Interestingly, drug hypersensitivity reactions have also repeatedly been shown to be mediated by Th1-cytokine production [13,14]. Therefore, a Th1-mediated vancomycin hypersensitivity reaction, in association with underlying susceptibility for developing aphthous ulcerations, may have precipitated our patient's diffuse oral lesions.
It is also important to note that oral ulcers in patients with vancomycin hypersensitivity reactions have been reported in the setting of co-existent neutropenia. As aphthous ulcers and fever are associated with other diseases manifesting neutropenia, including cyclic neutropenia, our patient's oral ulcers may be more directly related to neutropenia than to a Th1 cytokine profile, or to a combination of these. In the future, cytokine profiles and testing for anti-neutrophil antibodies may be useful to clarify the pathogenesis of vancomycin hypersensitivity reaction with neutropenia and oral ulcerations.
In summary, we describe a 45 year-old man who developed fever, neutropenia, lymphopenia and diffuse oral ulcerations several weeks after initiating IV vancomycin therapy. This constellation of clinical findings, in association with negative HSV/VZV DFA and cultures and rapid improvement after vancomycin discontinuation and methylprednisolone administration, provides strong evidence his oral ulcerations were precipitated by avancomycin hypersensitivity reaction. As identification of vancomycin hypersensitivity reactions is difficult, awareness of aphthous-like ulcerations as a potential manifestation is important. Given our patient's misdiagnosis as oral candidiasis and orolabial herpes led to hospitalization, recognition ofthis mucosal reaction can allow for prompt vancomycin discontinuation and avoidance of unnecessary and costly diagnostic and therapeutic measures.
References
-
Sivagnanam S, Deleu D (2003) Red man syndrome. Crit Care 7: 119-120.
-
Smith PF, Taylor CT (1999) Vancomycin-induced neutropenia associated with fever: similarities between two immune-mediated drug reactions. Pharmacotherapy 19: 240-244.
-
Black E, Lau TT, Ensom MH (2011) Vancomycin-induced neutropenia: is it dose- or duration-related? Ann Pharmacother 45: 629-638.
-
Rocha JL, Kondo W, Baptista MI, Da Cunha CA, Martins LT (2002) Uncommon vancomycin-induced side effects. Braz J Infect Dis 6: 196-200.
-
Manocha D, TenorioCdel C, Rose F (2009) Vancomycin leading to lupus flare in an elderly lady: a case report. Cases J 23: 6293.
-
Tesfa D, Keisu M, Palmblad J (2009) Idiosyncratic drug-induced agranulocytosis: possible mechanisms and management. Am J Hematol 84: 428-434.
-
Fortuna G, Salas-Alanis JC, Guidetti E, Marinkovich MP (2012) A critical reappraisal of the current data on drug-induced linear immunoglobulin A bullous dermatosis: a real and separate nosological entity? J Am Acad Dermatol 66: 988-994.
-
Kakar R, Paugh H, Jaworsky C (2013) Linear IgA bullous disease presenting as toxic epidermal necrolysis: a case report and review of the literature. Dermatology 227: 209-213.
-
Chanal J, Ingen-Housz-Oro S, Ortonne N, Duong TA, Thomas M, et al. (2013) Linear IgA bullous dermatosis: comparison between the drug-induced and spontaneous forms. Br J Dermatol 169: 1041-1048.
-
Billet SE, Kortuem KR, Gibson LE, El-Azhary R (2008) A morbilliform variant of vancomycin-induced linear IgA bullous dermatosis. Arch Dermatol 144: 774-778.
-
Naranjo CA, Busto U, Sellers EM, Sandor P, Ruiz I, et al. (1981) A method for estimating the probability of adverse drug reactions. Clin Pharmacol Ther 30: 239-245.
-
Femiano F, Lanza A, Buonaiuto C, Gombos F, Nunziata M, et al. (2007) Guidelines for diagnosis and management of aphthous stomatitis. Pediatr Infect Dis J 26: 728-732.
-
Almeida CA, Martin AM, Nolan D, Lucas A, Cameron PU, et al. (2008) Cytokine profiling in abacavir hypersensitivity patients. Antivir Ther 13: 281-288.
-
Neuman MG, Shear NH, Malkiewicz IM, Taeri M, Shapiro LE, et al. (2007) Immunopathogenesis of hypersensitivity syndrome reactions to sulfonamides. Transl Res 149: 243-253.





