Journal of Dermatology Research and Therapy
Pseudolymphoma Concomitant with Parvovirus B19 Infection
Loan Towersey1*, Maria VictóriaQuaresma2, Fred Bernardes Filho3, Porphirio José Soares Filho4, Inês K. Praxedes Baeta Neves5, Andréa Rodriguez Cordovil Pires4, Omar Lupi6 and Roderick Hay7
1AIDS Division, HMCT, Ministry of Health, Brazil
2Department of Dermatopathology, Medical School of the University of São Paulo (FMUSP), Brazil
3Department of Dermatology, Professor Rubem David Azulay Institute of Dermatology, Brazil
4Department of Pathology, HUAP, Universidade Federal Fluminense, Brazil
5Laboratório Praxedes, Brazil
6Dermatology Service of the General Polyclinic of Rio de Janeiro (RJ), Brazil
7ILDS/ King's College Hospital, UK
*Corresponding author:
Loan Towersey, AIDS Division, HMCT, Ministry of Health, Rua Cel, Moreira César 229/1112 Icaraí, Niterói -Rio de Janeiro, Brazil, Tel: 24230-052, E-mail: loantowersey@gmail.com
J Dermatol Res Ther, JDRT-1-007, (Volume 1, Issue 1), Correspondence; ISSN: 2469-5750
Received: May 28, 2015 | Accepted: September 03, 2015 | Published: September 05, 2015
Citation: Towersey L, Quaresma MV, Filho FB, Filho PJS, Neves IKPB, et al. (2015) Pseudolymphoma Concomitant with Parvovirus B19 Infection. J Dermatol Res Ther 1:007. 10.23937/2469-5750/1510007
Copyright: © 2015 Towersey L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Jessner's lymphocytic infiltration, JLIS, Dermoscopy
Jessner's lymphocytic infiltration of the skin (JLIS) is a skin condition of unknown an etiology characterized by erythematouspapules, plaques, and/or nodules located on the head, neck and upper back. Lesions usually are asymptomatic and resolve without scarring. JLIS can be similar in appearance to other benign lymphocytic infiltrates which include for instance a variant of lupus erythematosus (LE), in particular, tumid LE. A few cases of JLIS-like lymphocytic infiltrates are related to Borrelia burgdorferi; infection or drugs and contact allergy have also been reported. Some investigators favor polymorphic light eruption (PLE) or pseudolymphoma (PL) as possible causes [1-3]. We here in report a case of pseudolymphoma coexisting with parvovirus infection and describe the dermatoscopic features of this disease.
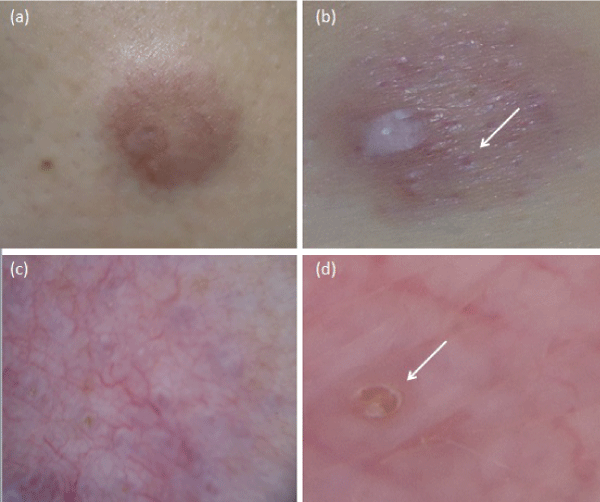
A 52-year-old woman presented with a 3-month history of a popular lesion that progressed to an erythematous nodule with cutaneous peau d'orange aspecton the left mammary region (Figure 1a,1b). The lesion had appeared 24 hours after a surgical procedure (hysterectomy and oophorectomy). It was sporadically pruritic. Dermoscopy with a handheld dermoscope (DermLite II Pro 3Gen [3Gen; SanJuan Capistrano, CA]) revealed arborizing blood vessels of different caliber with an erythematous background (Figure 1c) and yellow dots were observed. At higher magnification with the use of a handheld digital microscope (Proscope HR® [Bodelin Technologies, Lake Oswego, OR]) some yellow dots surrounded by a ridge like border were seen (Figure 1d). Skin biopsy demonstrated a normal epidermis with a perivascular and periadnexal infiltrate of lymphocytes in the dermis, particularly prominent and dense in the reticular dermis. Differential diagnosis included lymphoma. Immunohistochemistry showed a predominance of T cells, mostly CD3+, CD8+, CD4+, and CD20+B cells (multifocal), and sparse CD30+cells, indicating this was a reactive inflammatory process (Figure 2). Laboratory investigation revealed parvovirus B19 infection as a coexisting condition with reactive IgG 9.44 against Parvovirus B19 (reference value above 1.1) and not reactive IgM 0.21 (reference value lower than 0.9). Hypovitaminosis D was also detected. Within one year IgG level against Parvovirus B19 dropped to non reactive.
.
Figure 1: (a) Erythematous nodule on the chest, (b) Peau d'orange phenomenon (arrow), (c) Dermoscopy: arborizing blood vessels and yellow dots, (d) Dermoscopy: ridge like border (arrow).
View Figure 1
.
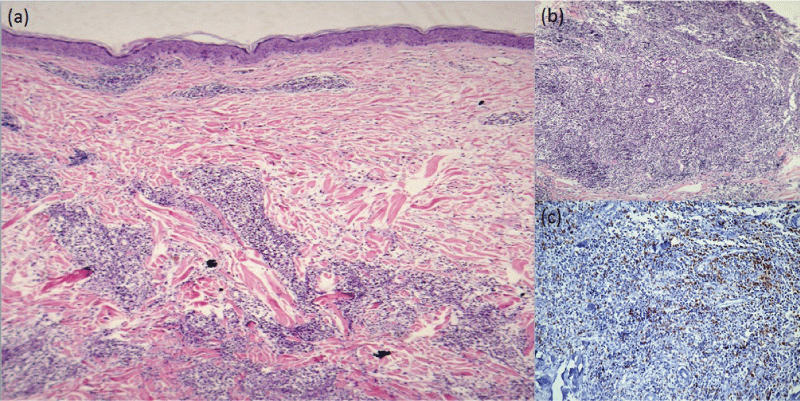
Figure 2: Histopathological findings: (a) perivascular and periadnexal lymphocytic infiltrate, (b) Deep massive lymphocytic infiltration in the dermis, (c) Immunostaining with positive CD8 lymphocytes in the infiltrate(hematoxylin and eosin stain; a,50x, b,100x, Immunostain; c, 200x)
View Figure 2
The use of the Proscope HR® allowed for a more refined observation, highlighting the usefulness of this imaging device. We emphasize the dermatoscopic findings of arborizing vessels, yellow dots, some presenting a thread-like border. The later dermatoscopic pattern may be correlated topeau d'orange phenomenon. The arborizing vessels may correspond to the perivascular sleeve-like lymphocytic infiltrate, and may also be found in other cutaneous pseudolymphomas. The yellow dots and the ridgelike border may correlate to periadnexal lymphocytic infiltrate with perifollicular accentuation, and intact adnexal structures. The predominance of a small mature polyclonal lymphocytic infiltrate without epidermal involvement confirmed the inflammatory nature of the nodule. Cutaneous manifestations associated with parvovirus B19 infection include vasculitis, erythema nodosum, the lupus erythematosus-like syndrome, some vesiculo-pustular eruptions, pityriasis lichenoides, scleroderma and Kikuchi-Fujimoto disease [4,5]. The concomitance with pseudolymphoma has not been previously reported to the best of our knowledge.
References
-
Zieme M, Elsendle K, Muller H, Zeiger B (2009) Lymphocytic infiltration of the skin (Jessner-Kanof) but not reticular erythematous mucinosis occasionally represents clinical manifestations of Borrelia- associated pseudolymphoma. Br J Dermatol 163: 583-590.
-
Laurinaviciene R, Clemmensen O, Bygum A (2009) Successful treatment of Jessner's lymphocytic infiltration of the skin with methotrexate. Acta Derm Venereol 89: 542-543.
-
Lima AAB (1974) Infiltratio Lymphocytaria Cutis. Tese para concurso de Livre Docência de Clínica de Dermatologia da Escola de Medicina e Cirurgia do Rio de Janeiro. Rio de Janeiro.
-
Blaise G, Nikkels AF, Piérard GE (2007) Cutaneous manifestations of parvovirus B19 infection. Rev Med Liege 62: 492-495.
-
Pai SA, Naresh KN, Soman CS, Borges AM (1998) Pseudolymphomatous phase of Kikuchi-Fujimoto disease. Indian J Cancer 35: 119-128.





