Journal of Dermatology Research and Therapy
Facial Follicular Mucinosis in Adolescence
Gokce Isil Kurmus1*, Filiz Canpolat2, Müzeyyen Gonul2 and Murat Alper3
1Igdır State Hospital, Department of Dermatology, Igdır, Turkey
2Ankara Diskapi Yildirim Beyazit Education and Research Hospital, Department of Dermatology, Ankara, Turkey
3Ankara Diskapi Yildirim Beyazit Education and Research Hospital, Department of Pathology, Turkey
*Corresponding author:
Gokce Isil Kurmus, Igdir State Hospital, Department of Dermatology, Igdir, 76000, Turkey, E-mail: isilkurmus@gmail.com
J Dermatol Res Ther, JDRT-2-021, (Volume 2, Issue 2), Case Report; ISSN: 2469-5750
Received: February 16, 2016 | Accepted: April 09, 2016 | Published: April 12, 2016
Citation: Kurmus GI, Canpolat F, Gonul M, Alper M (2016) Facial Follicular Mucinosis in Adolescence. J Dermatol Res Ther 2:021. 10.23937/2469-5750/1510021
Copyright: © 2016 Kurmus GI, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Follicular mucinosis (FM), also known as alopecia mucinosa, is a rare inflammatory disorder that characteristically presents as follicular papules or infiltrated plaques with prominent follicular openings associated with alopecia. Histologically, the disorder is characterized by mucin deposition in the follicular epithelium and sebaceous glands.
FM was classified in two distinct entities: a primary or idiopathic form, usually presents in children and young adults with a benign course, and a secondary form in elderly associated other benign and malignant diseases. Among the malignant diseases, the main association is with mycosis fungoides. Herein we describe the case of an adolescent primary follicular mucinosis with facial lesion and discuss the clinical variants, histopathological pattern, and treatment options.
Keywords
Follicular mucinosis, Alopecia mucinosa, Adolescence
Introduction
FM is an uncommon idiopathic skin disease that usually presents as fleshcolored follicular papules, hypopigmented or erythematous, slightly scaling patches, infiltrated plaques and nodules [1-3]. Unusual presentations include alopecia areata-like, scarring alopecia, folliculitis, acneiform eruptions, linear lesions following Blaschko lines and urticaria-like follicular mucinosis [3]. Face, head and neck are the most frequent sides of involvement in primary FM whereas the secondary form shows widespread lesions on the trunk and extremities [4]. However, clinical parameters are not specific enough to distinguish benign primary form from secondary form associated with mycosis fungoides. Therefore follow-up is essential.
Case Report
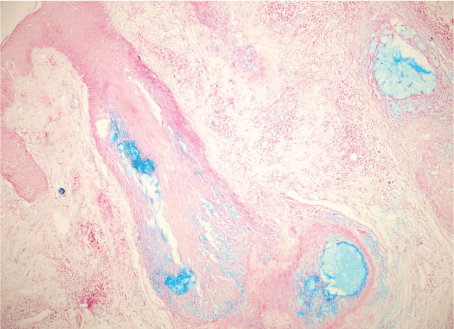
A 16-year-old girl presented with a two year history of a slowly growing, erythematous, slightly itchy patch on the right side of forehead. The patient’s past medical history and family history were normal. Dermatological examination revealed a well defined, alopecic and erythematous 1 × 2 cm patch that has prominent follicular plugs in the center (Figure 1). A narrow ring of slightly hypopigmented skin around the lesion was observed. General physical examination was normal. All laboratory tests, including complete blood count, erythrocyte sedimentation rate, liver and kidney function tests, and urinalysis were within the normal range. Chest x-ray, abdominal ultrasound revealed no lymph node enlargement, organomegaly or other pathological findings. A skin punch biopsy was performed. Hematoxylin and eosin (H&E) staining of a section of the sample revealed a mixed inflammatory infiltrate, composed mostly of lymphocytes that surround, and involve follicular epithelium associated with mild focal follicular spongiosis (Figure 2). Alcian blue staining demonstrated the mucinous nature of the infiltration in the follicular epithelium (Figure 3). The histopathological examination was characteristic for FM. On the basis of clinical, and histopathological examination, a diagnosis of follicular mucinosis was made.
.
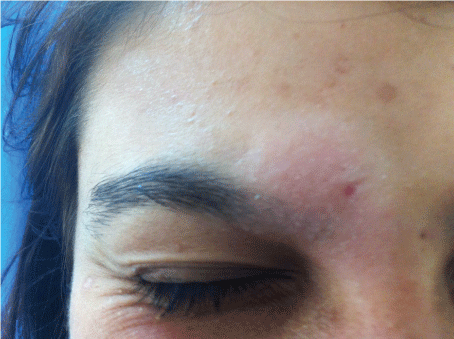
Figure 1: Erythematous 1 × 2 cm plaque with hypopigmented halo which has prominent follicular plugs in the center.
View Figure 1
.
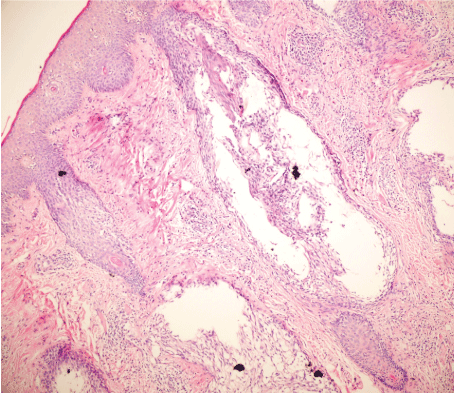
Figure 2: H&E, X20, superficial and deep perivascular and interstitial mixed-cell infiltrate within follicular epithelium.
View Figure 2
Discussion
FM was first described as alopecia mucinosa by Pinkus in 1957. It is a rare idiopathic disorder with unknown etiology characterized by mucin deposition within the hair follicles and sebaceous glands of the pilosebaceous unit besides a superficial and deep perivascular and interstitial mixed‑cell infiltrate. The follicular keratinocytes have been considered to be source of mucin [3,4].
Clinically, FM usually presents with follicular papules or erythematous, infiltrated plaques with prominent follicular openings associated with alopecia on the head and neck [1,4]. However, clinical manifestation may not be typical and there are reports of hypopigmented plaques and nodulary forms and presentations that simulate folliculitis, alopecia areata, scarring alopecia, chronic eczema, acne, urticaria and erythrodermic forms [3].
The dermatosis can be differentiated into two clinical types. The most common is idiopathic (primary or benign) FM, that is usually presented in children and young adults. Primary FM, demonstrates spontaneous resolution, is also considered to be a transient form of disease which tend to resolve within a few years. Secondary FM, presents as widespread lesions, usually occurs in older patients and is associated with underlying inflammatory and malignant processes, mycosis fungoides (MF) being the most common malignancy [1-4]. Although MF is the most commonly associated lymphoma, other lymphomas such as Hodgkin disease have been reported in children/young adults with longer periods of follow-up [5].
Clinical and histopathological criteria are fundamental for the distinction between primary and secondary variants; however, they are not specific enough for such definition, thus making the followup of patients necessary. It has also been reported that a clonal T-cell receptor gene rearrangement could help to differentiate malignancy associated FM [2]. It has also been reported that no clear-cut criteria allow the differantion of idiopathic from lymphoma-associated FM, and idiopathic FM may belong to the variant forms of MF that show prolonged, nonagressive clinical course [5]. Patients with so-called idiopathic FM should be observed carefully for long periods of time.
There is no standard treatment for primary FM, so a wide variety of treatments based on anecdotal evidence, such as corticosteroids (topical, intralesional, systemic), topical and systemic retinoids, dapsone, methotrexate, cyclophosphamide, minocycline, hydroxychloroquine, interferons, indomethacin, topical pimecrolimus, ultraviolet A, superficial radiation and photodynamic therapy have been tried. Our patient remains under clinical follow-up with improvement of the aspect of the lesion with the topical corticosteroid treatment [3-6].
References
-
Alikhan A, Griffin J, Nguyen N, Davis DM, Gibson LE (2013) Pediatric follicular mucinosis: presentation, histopathology, molecular genetics, treatment,and outcomes over an 11-year period at the Mayo Clinic. Pediatr Dermatol 30: 192-198.
-
Rupnik H, Podrumac B, Zgavec B, Lunder T (2005) Follicular mucinosis in a teenage girl. Acta Dermatovenerol Alp Panonica Adriat 14: 111-114.
-
Passos PC, Zuchi MF, Fabre AB, Martins LE (2014) Follicular mucinosis- case report. An Bras Dermatol 89: 337-339.
-
Lewars M, Levin Ji Purcell S (2013) Follicular mucinosis. Indian Dermatol Online J 4: 333-335.
-
Cerroni L, Fink-Puches R, Bäck B, Kerl H (2002) Follicular mucinosis: a critical reappraisal of clinicopathologic features and association with mycosis fungoides and Sézary syndrome. Arch Dermatol 138: 182-189.
-
Schneider SW, Metze D, Bonsmann G (2010) Treatment of so-called idiopathic follicular mucinosis with hydroxychloroquine. Br J Dermatol 163: 420-423.