Journal of Dermatology Research and Therapy
The Role of the Mast Cell in Skin Aging
Yang-lin Hua1, Wei Gao2, Hong-ying Li2 and Jian Tang1*
1Research & Development Center, Infinitus (China) Company Ltd, China
2Healthy Star Bio-Tech R&D Ltd, Shanghai, China
*Corresponding author:
Jian Tang, Research & Development Center, Infinitus (China) Company Ltd, 1st Floor in Building1, Hong Tai Wisdom Valley, 19 Sicheng Road, Tianhe District, Guangzhou, China, E-mail: Tom.Tang@infinitus-int.com
J Dermatol Res Ther, JDRT-2-035, (Volume 2, Issue 5), Mini Review; ISSN: 2469-5750
Received: August 29, 2016 | Accepted: October 11, 2016 | Published: October 14, 2016
Citation: Yang-lin H, Gao W, Hong-ying L, Tang J (2016) The Role of the Mast Cell in Skin Aging. J Dermatol Res Ther 2:035. 10.23937/2469-5750/1510035
Copyright: © 2016 Yang-lin H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Skin is the external organ of human body that provides protection against environmental stress. Direct and indirect damage causes skin aging. Scientists have been struggling to explore the mechanisms of skin aging and to think of ways to delay this course. The role of mast cell in regulating skin aging has attracted much attention recently. The granules of mast cell contain a great diversity of highly toxic compounds and active mediators. Degranulation of mast cell in papillary dermis may lead to extra cellular matrix reconstruction, inflammation and angiogenesis which result in accelerated skin aging. Essential factors implicated in aging and tissue damage in skin are possibly related to mast cells. Mast cell is becoming an important target for anti-aging therapy. Many natural products capable of inhibiting mast cell activation are considered functional ingredients for anti-skin aging.
Keywords
Mast cell, Skin aging, Skin tissue reconstruction, Inflammation, Angiogenesis, Mast cell stabilizer
Abbreviations
UV: Ultraviolet; TNF-α:Tumor Necrosis Factor-α; MMP: Matrix Metalloproteinase; ECM: Extracellular Matrix; SCF: Stem Cell Factor; PGD2: Prostaglandin 2; AP-1: Activating Protein-1; NF-κB: Nuclear Factor kappa B; FGF: Fibroblast Growth Factor; TGF: Transforming Growth Factor; VEGF: Vascular Endothelial Growth Factor; IL: Interleukin; ERK: Extra-signal Response Kinase; HMC-1: Human Mast Cell-1; JNK: Jun N-terminal Kinase; COX: Cyclooxygenase
Introduction
Everyone hopes to look younger. A lot of women spare no efforts and spend a lot of money to prevent skin aging. Skin aging gradually becomes a medical and social problem in modern world [1,2]. The pathological process of skin aging and the sustainable solutions of anti-skin aging are investigated by medical and biological scientists through ages. No solution has been explored to completely reverse or prevent aged skin appearance up to now. But the comforting thing is that some key mechanisms of skin aging are uncovered [3,4].
Skin aging is a complex physiological and pathological changing process, including a series of continuous changes, which finally leads to structural damage and dysfunction of skin tissue. Skin aging can be divided into intrinsic and extrinsic aging. Extrinsic aging is also called photoaging,because the major extrinsic factors is sun exposure, especially the ultraviolet (UV) radiation. Smoking is the second most common cause of extrinsic aging [5]. Chronic sun exposure profoundly impacts on the epidermis and dermis leading to signs of skin aging, including wrinkle, sagging, and laxity [6,7].
Recently, investigators have paid close attention to the role of mast cell in regulating skin aging. Mast cells mostly reside in tissues directly exposed to the environment, such as skin, airways and gastrointestinal tract [8]. In skin tissue, mast cells are prevalent in the papillary dermis around blood vessels, rarely observed in deep dermis and almost absent in epidermis. Once activated, mast cell will discharge particles i.e. degranulation of mast cell occurs. The granules of mast cell contain a great diversity of highly toxic compounds and active mediators, including chymase, tryptase, tumor necrosis factor-α (TNF-α), and histamine. These mediators are involved in inflammation from early phage of vessel reaction and extracellular matrix damage to later skin tissue reconstruction [9]. In vitro models demonstrated that cigarette smoke medium stimulated the production of chemokines [10] and induced phosphorylation of extra-signal response kinase (ERK) ½ in mast cells [11].
Ketotifen, one kind of mast cell stabilizers, has been proved to significantly prevent UV-induced wrinkle formation, skin thickening, and an increasing amount of mast cell and degranulation ratio. The underlying mechanism may relate to the inhibition of matrix metalloproteinase (MMP) -13 and MMP-9 expression, as well as inflammatory cell infiltration by Ketotifen dose dependently [12].
Thus it can be seen that the essential factors implicated in aging and tissue damage in skin may possibly relate to mast cells. The anti-aging therapy should aim at mast cell as an important target. Divers natural products are available and able to stabilize mast cell membrane thereby inhibiting skin damage induced by mast cell activation.
Mast Cell and Extracellular Matrix (ECM) Reconstruction
Mast cells that exist in papillary dermis are concentrated around epithelia, nerves and blood vessels. Mast cells are derivatives of hematopoietic progenitor cells in the bone marrow. When progenitors move through the blood stream to peripheral tissues, they differentiate completely into mature mast cells with the action of micro environmental factors and stem cell factor (SCF) [13]. It is reported in a murine study that epidermal SCF production is upregulated by chronic UV irradiation. A considerable amount of SCF leads to mast cell increase in dermis after then [14].
Mast cells reside in dermis where UVB rays cannot reach that far. However, overwhelming evidences over the past decades revealed intensified dermal mast cell degranulation in response to sunlight [15]. Sensory nerve endings are rich in skin dermis. Neuropeptides from activated nerve endings often stimulate mast cell degranulation while releasing preformed mediators. Mediators released from UVB-irradiated keratinocytes have been identified to stimulate sensory nerves to release neuropeptides that could in turn trigger mast cell degranulation.
Investigators found an increase in elastin in papillary dermis of skin from the dorsum of the hand but not from the buttock. The deep cause of this observation was identified due to varying amounts of sun exposure to different areas of skin. They also noticed that extensive elastosis in sun-exposed hand skin was correlated with increased mast cell prevalence and with older age [16].
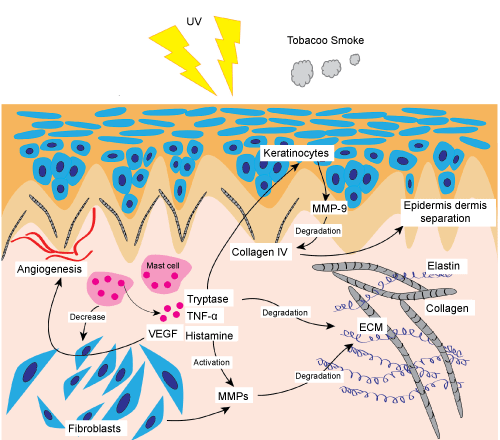
Typtase, the most abundant seine proteinase in granules of mast cells, differs from other trypsin like proteinases in its ability to evoke various processes leading to tissue remodeling [17]. Mast cell tryptase is a new potential enzyme discovered to contribute to trigger the matrix degradation process in dermis. Tryptase can activate MMPs which are recognized as the major enzymes in the ECM degradation process to cause direct damage on ECM proteins [9], especially on type I and type III collagen which are the vital components in dermal ECM (Figure 1).
It has been reported that tryptase is able to weaken the adhesive force of keratinocytes in epidermis and cleave fibronectinin the pericellular matrix of dermal fibroblasts. Fibronectin is an important adhesive protein in the dermal ECM. Therefore, tryptase is supposed to involve in dermal-epidermal separation which is another sign of skin aging [18,19]. However, literature also reported that UV-induced mast cell increasing and activation contribute to the tissue remodeling of photodamaged skin. Mast cells play an important role in maintaining the skin structural balance and help skin tissue restore itself from damage [20].
Activated mast cells are capable of evoking degranulation of adjacent mast cell through paracrine. Tryptase released from activated mast cells is proved to induce histamine release from non-activated mast cells [21]. Histamine is another predominant component in granules of mast cells and it is able to stimulate keratinocytes to produce MMP-9, to promote immune cell migration and to accelerate type IV collagen degradation [22].
Mast Cell and Inflammation
Fibroblast, the major type of cells in dermis, can synthesize almost all kinds of extracellular matrix as collagen fibers, elastin fibers, and proteoglycans [23,24]. It was reported that fibroblasts in dermis may decrease in number during age [25]. Hence, if the number of fibroblasts is lowered with age, renewal potency of aged skin is diminished. Interestingly, the number of mast cells observed in skin was increasing along with the decrease of fibroblasts.
Phenomenon that quantity of mast cell increases with ages is likely to be bound with inflammatory processes in dermis developed along the life. External and internal factors like UV irradiation, air humidity and temperature changes always induce repeatedly occurred dermal inflammation which finally leads to quantity increase of mast cells [26].
The appearance of photo aged skin is histologically identical to chronic inflammatory skin without any external inflammatory signs,which consists with the increase of mast cells after UV irradiation and suggests the important role of mast cell in skin inflammatory processes [27]. Inflammation is doubtlessly proved to be one of key factors resulting in skin aging.
Ultraviolet B contributes to ‘sun burn’ in human skin which is characterized by activated dermal blood vessel, altered traffic of Langerhans cell and acutely released TNF-α. The source of TNF-α is partly activated mast cells resided in skin [28]. The finding of decreased dermal mast cell prevalence in TNF-α- or TNF receptors-knockout mice [29] supported the hypothesis that TNF-α functions as a mast cell mitogenic factor. TNF-α is a cytokine triggering inflammatory responses that occur in the skin. TNF-α can induce the production of MMP-9, an enzyme responsible for skin aging, through regulating the expression of the MMP genes. MMP-9 is able to cause skin damage and inhibit the self-repair mechanism of skin tissue [30]. Increased number of mast cells is possibly resulting in earlier period of inflammations [31] and the release of inflammatory factors can upregulate MMP-9 [32]. The underlying mechanism is the upregulated MMP genes by transcription factors as activating protein-1 (AP-1) [33] and nuclear factor kappa B (NF-κB) of which the activity to bind to MMP-9 DNA sequence can be increased by TNF-α and then lead to over production of MMP-9 (Figure 1) [30].
Mast Cell and Angiogenesis
Mediators as fibroblast growth factor (FGF), transforming growth factor (TGF)-β, TNF-α, tryptase and heparin released from mast cells adjacent to blood vessels play a vital role in facilitating angiogenesis and neovascularization of remodeled skin.
Angiogenesis is the process that new blood vessels sprout from existing blood vessels of which the blood supply is poor. With the stimuli like UV radiation, infrared rays and heat, cutaneous new blood vessels increase. Newly formed vessels are leaky and immature. Inflammatory cells escaped from these vessels result in cutaneous inflammation and further degradation and reconstruction of dermal ECM. Large amount of high toxic compounds released from new blood vessels to skin tissue may also induce skin damage and aging [34,35]. Angiogenesis has been proved to be functionally associated with photoaging-related wrinkle formation [36].
UV radiation caused skin photoaging is partly resulted from the increased number of mast cells in human skin after UV irritation [37]. UV radiation can lead to the increased level of vascular endothelial growth factor (VEGF). VEGF is one of the chemotactic factors contained in mast cell andis also one of the molecular features of photo aged skin [38]. As an important regulator of angiogenesis, VEGF is able to induce mast cell migration at picomolar concentrations. Over expressed VEGF contributes to a 35% increase in mast cell prevalence in the papillary dermis and also increases the density of blood capillaries in dermis (Figure 1) [39]. Mediators released from activated mast cells can also stimulate keratinocytes to release excessive amount of VEGF which results in increased numbers of tortuous and hyperpermeable blood vessels due to enhanced skin vascularization [40].
Natural Mast Cell Stabilizers
Quercetin
Quercetin is one kind of polyphenolic compounds naturally existed in fruits, vegetables, nuts, seeds and herbs [41,42] with various pharmacological effects as anti-oxidant, anti-inflammatory and mast cell stabilizing abilities [43]. Quercetin was reported effectively equivalent with cromolyn, one kind of mast cell stabilizers, in inhibiting histamine and prostaglandin 2 (PGD2) release but much more effective in reducing inflammatory cytokines release from human mast cells [44], of which the underlying mechanism may be the attenuation of NF-κ and p38MAPK signaling pathways in mast cell [45]. NF-κB and p38MAPK are well known involved in skin photoaging [46]. Quercetin is capable of regulatinginterleukin (IL)-6, IL-8, TNF-α, histamine and tryptase release from mast cells [44] and accordingly attenuates atopic dermatitis symptoms [47]. A murine study demonstrated that water in oilmicroemulsion containing quercetin reduced the incidence of histological skin alterations, mainly the connective-tissue damage, induced by UVB irradiation [48].
Resveratrol
Resveratrol, a stilbenoid is a polyphenolic compound found predominantly in various plants, including grapes, berries and peanuts. Resveratrol has been well-studied to possess anti-inflammatory and anti-oxidant properties against aging. Resveratrol was confirmed to protect skin against photo damage through enhancing skin moisture and elasticity, reducing depth and length of wrinkles and decreasing intensity of spots [49-51]. In vitro test revealed that resveratrol directly inhibited degranulation of RBL-2H3 mast cells and human skin mast cells [52,53]. Resveratrol was reported to decrease the phosphorylation of ERK 1/2 in activated human mast cell-1(HMC-1) cells and inhibit NF-κB activation, which in turn lead to suppressed expression of TNF-α, IL-6, IL-8 and cyclooxygenase (COX)-2 [54]. And thus resveratrol plays a role in regulating mast cell mediated inflammatory processes that result in tissue damage including skin.
Angelica sinensis
The root of angelica sinensis is one of the most commonly used traditional Chinese medicine that processes multiple medical actions, for instance, antitumor, antiaging, antioxidant, immunoregulation etc. Angelica sinensis is also used for treating skin disorders.Topical application of angelica sinensis on skin of mice with atopic dermatitis was proved to regulate the level of substance P and distribution of mast cells in the skin. Angelica sinensis also inhibits the activation of NF-κB, IκBα and MAPKs (ERK1/2, p38, and JNK) which are known to be associated with inflammatory cytokines secretion [55]. Angelicapolysaccharide, one of the important and active constituents of angelica sinensis, has recently come of note as its wide range of pharmacological activities. Investigation demonstrated that angelica polysaccharide could inhibit the releases of proinflammatory cytokines from mast cells including histamine which is the notable markers indicating the degranulation of mast cells [56].
Conclusion
With development of technology and progress in civilization, human activities are increasingly changing the natural environment. As the external organ of human body, skin bears the brunt of environmental changes and shows the aging appearance. People struggle to explore the causes and mechanisms underlying skin aging and fight for a youthful skin appearance. In recent years, mast cells resided in dermis has attracted attention by many investigators. Reports showed that mast cells were rarely observed in dermis of fetus and young people but more often observed in dermis of aged people [27], which indicates the potential role of mast cell in regulating skin aging. Mast cells have been demonstrated to play a role in ECM remodeling, inflammation and angiogenesis in skin which are closely associated with skin aging processes. Thus, the essential factor implicated in aging and tissue damage in skin may possibly relate to mast cells. There are many natural products play stabilizing roles to inhibit mast cell from degranulation and block the downstream reactions induced by cytokine release.The exploration of natural mast cell stabilizers may do great to prevent or slow the skin aging process.
Acknowledgements
We thank Ya Cai and Xiao-li Weifor their strongly support and assistance.
References
-
Gupta MA, Gilchrest BA (2005) Psychosocial aspects of aging skin. Dermatol Clin 23: 643-648.
-
Zouboulis CC, Makrantonaki E (2011) Clinical aspects and molecular diagnostics of skin aging. Clin Dermatol 29: 3-14.
-
Zouboulis CC, Adjaye J, Akamatsu H, Moe-Behrens G, Niemann C (2008) Human skin stem cells and the ageing process. Exp Gerontol 43: 986-997.
-
Gilchrest BA, Campisi J, Chang H, Fisher G, Kulesz-Martin M (2015) Skin Aging: Molecular Mechanisms and Tissue Consequences. J Invest Dermatol 135: 950.
-
Kammeyer A, Luiten RM (2015) Oxidation events and skin aging. Ageing Res Rev 21: 16-29.
-
Poon F, Kang S, Chien AL (2015) Mechanisms and treatments of photoaging. Photodermatol Photoimmunol Photomed 31: 65-74.
-
Bosch R, Philips N, Suárez-Pérez JA, Juarranz A, Devmurari A, et al. (2015) Mechanisms of photoaging and cutaneous photocarcinogenesis and photoprotective strategies with phytochemicals. Antioxidants 4: 248-268.
-
Metcalfe DD, Baram D, Mekori YA (1997) Mast cells. Physiol Rev 77: 1033-1079.
-
Iddamalgoda A, Le QT, Ito K, Tanaka K, Kojima H, et al. (2008) Mast cell tryptase and photoaging: possible involvement in the degradation of extra cellular matrix and basement membrane proteins. Archives of dermatological research 300: 69-76.
-
Mortaz E, Redegeld FA, Sarir H, Karimi K, Raats D, et al. (2008) Cigarette smoke stimulates the production of chemokines in mast cells. J Leukoc Biol 83: 575-580.
-
Mortaz E, Folkerts G, Engels F, Nijkamp FP, Redegeld FA (2009) Cigarette smoke suppresses in vitro allergic activation of mouse mast cells. Clin Exp Allergy 39: 679-687.
-
Kim MS, Lee DH, Lee CW, Kim YK, Lee MJ, et al. (2013) Mast cell stabilizer ketotifen prevents UV-induced wrinkle formation. J Invest Dermatol 133: 1104-1107.
-
Bischoff SC, Sellge G (2002) Mast cell hyperplasia: role of cytokines. Int Arch Allergy Immunol 127: 118-122.
-
Kligman LH, Murphy GF (1996) Ultraviolet B Radiation Increases Hairless Mouse Mast Cells in A Dose-Dependent Manner and Alters Distribution of UV-lnduced Mast Cell Growth Factor. Photochem Photobiol 63:123-127.
-
Gilchrest BA, Soter NA, Stoff JS, Mihm MC (1981) The human sunburn reaction: histologic and biochemical studies. J Am Acad Dermatol 5: 411-422.
-
Grimbaldeston MA, Finlay-Jones JJ, Hart PH (2006) Mast cells in photodamaged skin: what is their role in skin cancer? Photochem Photobiol Sci 5: 177-183.
-
Vitte J (2015) Human mast cell tryptase in biology and medicine. Mol Immunol 63: 18-24.
-
Kaminska R, Helisalmi P, Harvima RJ, Horsmanheimo M, Harvima IT, et al. (1999) Focal dermal-epidermal separation and fibronectin cleavage in basement membrane by human mast cell tryptase. J Invest Dermatol 113: 567-573.
-
Lohi J, Kesksi-Oja J, Harvima I (1992) Pericellulars substrates of human mast cell tryptase: 72000 Dalton gelatinase and fibronectin. J Cell Biochem 50: 337-349.
-
Calderhead RG, Kubota J, Trelles MA, Ohshiro T (2008) One mechanism behind LED phototherapy for wound healing and skin rejuvenation: key role of the mast cell. Laser Therapy 17: 141-148.
-
He S, Gaça MD, Walls AF (1998) A role for tryptase in the activation of human mast cells: modulation of histamine release by tryptase and inhibitors of tryptase. J Pharmacol Exp Ther 286: 289-297.
-
Gschwandtner M, Purwar R, Wittmann M, Bäumer W, Kietzmann M, et al. (2008) Histamine upregulates keratinocyte MMP-9 production via the histamine H1 receptor. Journal of Investigative Dermatology 128: 2783-2791.
-
Makrantonaki E, Zouboulis CC (2007) Molecular mechanisms of skin aging: state of the art. Ann N Y Acad Sci 1119: 40-50.
-
Ishida Y, Kimura A, Takayasu T, Eisenmenger W, Kondo T, (2009) Detection of fibrocytes in human skin wounds and its application for wound age determination. Int J Legal Med 123: 299-304.
-
Oh JH, Kim YK, Jung JY, Shin JE, Kim KH, et al. (2011) Intrinsic aging-and photoaging-dependent level changes of glycosaminoglycans and their correlation with water content in human skin. J Dermatol Sci 62: 192-201.
-
Petrov VV, Vasilyeva OV, Kornilova NK, Gunin AG (2013) Age-related changes in mast cells and eosinophils of human dermis. Ontogenez 44: 179-185.
-
Bosset S, Bonnet-Duquennoy M, Barre P, Chalon A, Kurfurst R, et al. (2003) Photoageing shows histological features of chronic skin inflammation without clinical and molecular abnormalities. Br J Dermatol 149: 826-835.
-
Walsh LJ (1995) Ultraviolet B irradiation of skin induces mast cell degranulation and release of tumour necrosis factor-a. Immunol Cell Biol 73.
-
Hart PH, Grimbaldeston MA, Swift GJ, Sedgwick JD, Körner H, et al. (1998) TNF modulates susceptibility to UVB-induced systemic immunomodulation in mice by effects on dermal mast cell prevalence. European journal of immunology 28: 2893-2901.
-
Youn UJ, Nam KW, Kim HS, Choi G, Jeong WS, et al. (2011) 3-Deoxysappanchalcone Inhibits Tumor Necrosis Factor-. ALPHA.-Induced Matrix Metalloproteinase-9 Expression in Human Keratinocytes through Activated Protein-1 Inhibition and Nuclear Factor-Kappa B DNA Binding Activity. Biol Pharm Bull 34: 890-893.
-
Gunin AG, Kornilova NK, Vasilieva OV, Petrov VV (2010) Age-related changes in proliferation the numbers of mast cells eosinophils and cd45-positive cells in human dermis. J Gerontol A Biol Sci Med Sci 66: 385-392.
-
Saja K, Babu MS, Karunagaran D, Sudhakaran PR (2007) Anti-inflammatory effect of curcumin involves downregulation of MMP-9 in blood mononuclear cells. Int Immunopharmacol 7: 1659-1667.
-
Crawford HC, Matrisian LM (1995) Mechanisms controlling the transcription of matrix metalloproteinase genes in normal and neoplastic cells. Enzyme protein 49: 20-37.
-
Chung JH, Eun HC (2007) Angiogenesis in skin aging and photoaging. J Dermatol 34: 593-600.
-
Gunin AG, Petrov VV, Vasilieva OV, Golubtsova NN (2015) Age-related changes of blood vessels in the human dermis. Advances in Gerontology 5: 65-71.
-
Yano K, Oura H, Detmar M (2002) Targeted over expression of the angiogenesis inhibitor thrombospondin-1 in the epidermis of transgenic mice prevents ultraviolet-B-induced angiogenesis and cutaneous photo-damage. J Invest Dermatol 118: 800-805.
-
Kim MS, Kim YK, Lee DH, Seo JE, Cho KH, et al. (2009) Acute exposure of human skin to ultraviolet or infrared radiation or heat stimuli increases mast cell numbers and tryptase expression in human skin in vivo. Br J Dermatol 160: 393-402.
-
Grether-Beck S, Marini A, Jaenicke T, Krutmann J (2014) Photoprotection of human skin beyond ultraviolet radiation. Photodermatol Photoimmunol Photomed 30: 167-174.
-
Detmar M, Brown LF, Schön MP, Elicker BM, Velasco P, et al. (1998) Increased microvascular density and enhanced leukocyte rolling and adhesion in the skin of VEGF transgenic mice. J Invest Dermatol 111: 1-6.
-
Gunin AG, Petrov VV, Golubtzova NN, Vasilieva OV, Kornilova NK (2014) Age-related changes in angiogenesis in human dermis. Exp Gerontol 55: 143-151.
-
Huxley RR, Lean M, Crozier A, John JH, Neil HAW (2004) Effect of dietary advice to increase fruit and vegetable consumption on plasma flavonol concentrations: results from a randomised controlled intervention trial. Journal of epidemiology and community health 58: 288-289.
-
Lako J, Trenerry C, Wahlqvist ML, Wattanapenpaiboon N, Sotheeswaran S, et al. (2004) Total antioxidant capacity and selected flavonols and carotenoids of some Australian and Fijian fruits and vegetables. Asia Pacific Journal of Clinical Nutrition 13.
-
Park HH, Lee S, Son HY, Park SB, Kim MS, et al. (2008) Flavonoids inhibit histamine release and expression of proinflammatory cytokines in mast cells. Arch Pharm Res 31: 1303-1311.
-
Weng Z, Zhang B, Asadi S, Sismanopoulos N, Butcher A, et al. (2012) Quercetin is more effective than cromolyn in blocking human mast cell cytokine release and inhibits contact dermatitis and photosensitivity in humans. PLoS One 7: e33805.
-
Min YD, Choi CH, Bark H, Son HY, Park HH, et al. (2007) Quercetin inhibits expression of inflammatory cytokines through attenuation of NF-κB and p38 MAPK in HMC-1 human mast cell line. Inflamm Res 56: 210-215.
-
Ren X, Shi Y, Zhao D, Xu M, Li X, et al. (2016) Naringin protects ultraviolet B-induced skin damage by regulating p38 MAPK signal pathway. J Dermatol Sci 82:106-114.
-
Karuppagounder V, Arumugam S, Thandavarayan RA, Pitchaimani V, Sreedhar R, et al. (2015) Modulation of HMGB1 translocation and RAGE/NFκB cascade by quercetin treatment mitigates atopic dermatitis in NC/Nga transgenic mice. Exp Dermatol 24: 418-423.
-
Vicentini FT, Fonseca YM, Pitol DL, Iyomasa MM, Bentley MVL, et al. (2010) Evaluation of protective effect of a water-in-oil microemulsion incorporating quercetin against UVB-induced damage in hairless mice skin. J Pharm Pharm Sci 13: 274-285.
-
Polonini HC, Lima LL, Gonçalves KM, do Carmo AM R, da Silva AD, et al. (2013) Photoprotective activity of resveratrol analogues. Bioorg Med Chem 21: 964-968.
-
Wu Y, Jia LL, Zheng YN, Xu XG, Luo YJ, et al. (2013) Resveratrate protects human skin from damage due to repetitive ultraviolet irradiation. J Eur Acad Dermatol Venereol 27: 345-350.
-
Buonocore D, Lazzeretti A, Tocabens P, Nobile V, Cestone E, et al. (2012) Resveratrol-procyanidin blend: nutraceutical and antiaging efficacy evaluated in a placebocontrolled double-blind study. Clin Cosmet Investig Dermatol 5: 159.
-
Han SY, Bae JY, Park SH, Kim YH, Park JHY, et al. (2013) Resveratrol inhibits IgE-mediated basophilic mast cell degranulation and passive cutaneous anaphylaxis in mice. J Nutr 143: 632-639.
-
Shirley D, McHale C, Gomez G (2016) Resveratrol preferentially inhibits IgE-dependent PGD 2 biosynthesis but enhances TNF production from human skin mast cells. Biochim Biophys Acta 1860: 678-685.
-
Kang OH, Jang HJ, Chae HS, Oh YC, Choi JG, et al. (2009) Anti-inflammatory mechanisms of resveratrol in activated HMC-1 cells: pivotal roles of NF-kappaB and MAPK. Pharmacol Res 59: 330-337.
-
Lee J, Choi YY, Kim MH, Han JM, Lee JE, et al. (2016) Topical application of Angelica sinensis improves pruritus and skin inflammation in mice with atopic dermatitis-like symptoms. J Med Food 19: 98-105.
-
Mao WA, Sun YY, Mao JY, Wang L, Zhang J, et al. (2016) Inhibitory Effects of Angelica Polysaccharide on Activation of Mast Cells. Evid Based Complement Alternat Med 2016.