Journal of Dermatology Research and Therapy
A Case of Generalized Lichenoid Reaction upon Red Permanent Lip-Liner Make-Up
Perruchoud DL1*, Kiermeir DM2, Adatto MA1,3, Lam MC1, Borradori L1 and Simon D1
1Department of Dermatology, Inselspital Bern University Hospital, University of Bern, Switzerland
2Department of Plastic Surgery, Inselspital Bern University Hospital, University of Bern, Switzerland
3Skinpulse Laser Center, Geneva, Switzerland
*Corresponding author: Perruchoud Delphine Lydie, Department of Dermatology, Inselspital Bern University Hospital, University of Bern, 3010 Bern, Switzerland, Tel: +41-0-79-600-37-52, Fax: +41-0-31-632-22-33, E-mail: delphine.perruchoud@h-fr.ch
J Dermatol Res Ther, JDRT-3-042, (Volume 3, Issue 1), Case Report; ISSN: 2469-5750
Received: October 07, 2016 | Accepted: February 15, 2017 | Published: February 18, 2017
Citation: Perruchoud DL, Kiermeir DM, Adatto MA, Lam MC, Borradori L, et al. (2016) A Case of Generalized Lichenoid Reaction upon Red Permanent Lip-Liner Make-Up. J Dermatol Res Ther 3:042. 10.23937/2469-5750/1510042
Copyright: © 2017 Perruchoud DL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background/Aims: Cosmetic permanent make-up is an increasingly popular form of tattooing. The latter is potentially associated with adverse skin reactions. Whereas localized lichenoid reactions at tattooed sites have been reported, generalized eruptions are rare.
Methods: We report a case of generalized lichenoid reaction upon red permanent lip-liner make-up.
Results: Based on both the clinical and histological features as well as the patch tests results, the underlying pathomechanisms and therapeutic approach are discussed.
Conclusion: Dissemination may be due to an allergic reaction or an isomorphic response.
Keywords
Lichenoid, Tattoo, Allergic reaction, Generalized, Isomorphic response
Introduction
The demand for cosmetic permanent make-up of lips, eyelids and eyebrows has significantly increased during recent years [1]. Most colorants used for cosmetic tattooing have not been licensed for medical application and therefore bear the risk for unpredictable adverse effects.
Tattoo reactions are most commonly associated with red inkdue to the presence of mercury and its sulphides. However, nowadays most allergic reactions to red tattoo are triggered by organic pigments such as Pigment Red 181 (CI 73360) and Pigment Red 170 rather than the traditional mercury sulphides. The use of red pigments containing mercury may result in lichenoid reactions and other localized side reactions [2]. Nevertheless, generalization of tattoo reactions with involvement of distant untattooed sites have been reported only anecdotally [3-5].
We here report the case of a generalized lichenoid reaction following red tattooing of the lips and discuss the potential underlying pathomechanisms and management.
Case Report
A 46-year-old female patient was referred because of swollen lips associated with a sensation of tightness, rapidly followed by the development of pruritic papules on her body. Her past history revealed hay fever and asthma. She has taken no medication. Furthermore, she had a red permanent lip-liner tattooing performed one year before the development of the cutaneous lesions, as well as older tattoos on her eyebrows.
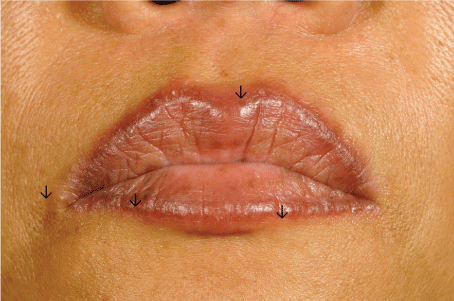
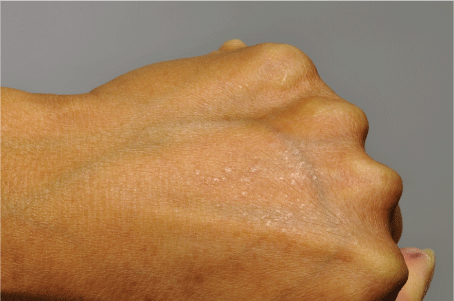
On examination the patient had papules and small nodules along the upper and lower vermilion borders (Figure 1). In addition, the patient had red and violaceous polygonal papules on the back of both hands (Figure 2), wrists and ankles. The oral and genital mucosae were unaffected. At the sites of tattooed eyebrows, no skin inflammation was noted.
Light microscopy studies of biopsy specimens obtained from the upper lip border and the right forearm (Figure 3) showed a lichenoid dermatitis with a lymphohistiocytic infiltrate along the basement membrane and few apoptotic keratinocytes. Eosinophils were present in the biopsy taken from the tattooed vermilion border (Figure 4). Immunohistochemistry studies revealed the presence of a CD3+ T-lymphocytic infiltrate, in which CD8+ lymphocytes slightly predominated over CD4+ cells. No increase of the CD1a+ Langerhans cells was observed.
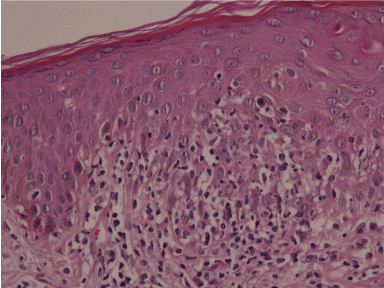
.
Figure 3: Hematoxylin-eosin stained skin biopsy of the right wrist, at 400 times magnification, revealing a lichenoid inflammation with few apoptotic keratinocytes.
View Figure 3
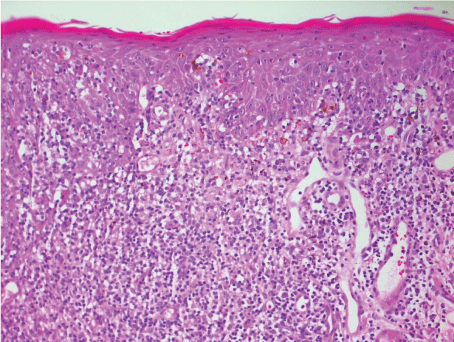
.
Figure 4: Histological image of the skin biopsy of the lip, at 400 times magnification, hematoxylin-eosin staining, showing a lichenoid inflammation with few eosinophilic granulocytes.
View Figure 4
We performed patch tests with standard, metal, preservative, dye and implant series on Finn chambers (Hermal, Almirall, Reinbeck, Germany) applied for two days on the back skin, which were evaluated at days 3 and 4. Positive reactions to nickel sulfate (++ at days 3 and 4) and to palladium chloride (+ at day 4) were noted, whereas no positive reaction to Pigment Red 181 (undiluted, 1% and 10% dilution) was found.
For treatment of the lips, mometasone cream for 7 days, followed by topical tacrolimus 0.1% once a day were applied, while all other lesions were treated with clobetasol cream. The skin lesions progressively improved and finally resolved within two months. One month later, the patient was still in remission. Unfortunately, she was lost for further follow-up.
Discussion
Clinical findings
We here present the striking case of a patient with a generalized lichenoid reaction which first started at a site of prior red tattooing on the lips.
Histopathological findings
Light microscopy studies revealed a lichenoid reaction in biopsies from both the tattooed lip and forearm. The presence of eosinophils in the biopsy of the lip pointed to the differential diagnosis of a delayed-type allergic response. On the other side, a Koebner's phenomenon by Lichen planus can be discussed based on the absence of eosinophils in the biopsy specimen obtained at a site distant from the tattoo and the predominance of a CD8+ T cell infiltrate.
Patch test results
Because the culprit original tattoo ink used for the tattooing of the lip was not available, we performed patch tests with frequently used Pigment Red 181 (CI 73360) and dye series. The failure to induce a positive reaction to red dye may be due to either the use of the inappropriate substances for patch testing and/or the fact that patches testing is inadequate for diagnosing the sensitization to the substances injected. Patch testing often fails to confirm hypersensitivity to tattoo dyes despite typical clinical and histological findings suggestive of allergic reactions and might be accomplished by testing with tape stripping, prick test, or photo patch test [2,6]. However, the strong positive patch test reactions to nickel sulfate found in our patient suggest that nickel contamination of the tattoo ink play a role as elicitor of skin reaction. Nickel contamination has been reported as etiology of allergic tattoo reactions in sensitized individuals. Even low amounts of 1.90 ± 0.34 ppm nickel were found sufficient to cause allergic reactions [7].
In contrast to frequently published adverse reactions confined to tattooed sites, generalized skin reactions seem to be rare and, to our knowledge, have not been reported after red permanent lip-liner make-up.
Pathophysiologically an allergic reaction or an isomorphic response may contribute to the development of generalized skin lesions. A disseminated delayed-type allergic response to either nickel or to an unidentified allergen consecutive to tattoo ingredient dissemination is possible. Alternatively, auto-sensitization has been described as secondary spreading of an initially localized dermatitis without detectable allergen at distant sites. Moreover, based on the absence of eosinophils in the biopsy specimen obtained at a site distant from the tattoo and the predominance of a CD8+ T cell infiltrate a Koebner's phenomenon by Lichen planus can be discussed, in analogy to the Koebner's reactions upon tattooing observed in patients with either psoriasis or discoid lupus erythematosus. Miscellaneous trauma like tuberculin skin test, scratch skin test and tattoo have been reported as causes of isomorphic responses. Delays of isomorphic responses up to one year as observed in our patient have been described, although they usually occur after 10 to 20 days [8,9].
Treatment
Spontaneous resolution may occur, thus an expectative strategy should be followed first. Application of topical corticosteroids and tacrolimus resulted in complete resolution of the skin lesions in our patient. In addition to topical immunosuppressives, intralesional corticosteroids are useful in the management of lichenoid tattoo reaction [10,11]. In case of skin lesions refractory to conservative treatment, tattoo removal using laser technologies that allow selective photothermolysis of the usually monochromatic permanent make-up tattoos, have been employed. Laser systems using very short pulse durations in nano (Q-switched) or picosecond are the gold standard for tattoo removal, as they deliver high amount of energy with very short pulse durations, leading to fragmentation of colorant particles, which subsequently can be phagocyzed by macrophages. Q-switched frequency doubled Nd:YAG or picosecond lasers at 532 nm can successfully remove red pigment tattoo. However, cosmetic tattoos may contain ferric oxide (Fe2O3), which after chemical reduction to ferrous oxide (FeO) upon laser treatment might turn black (darkening) [12]. To avoid this side effect, it might be better to use an ablative laser, pulsed CO2 or Er:YAG, mainly in fractional mode, which can also efficiently remove red tattoo colorants [13]. Local reactions can be successful treated by tattoo removal [14-16]. Nevertheless, laser tattoo removal was also shown to evoke immediate cutaneous reactions at the tattoo site as well as generalized allergic skin eruptions [17]. In presence of a of local or generalized lichenoid skin reaction related to either a delayed type hypersensitivity and/or isomorph response, we recommend as initial therapy topical anti-inflammatory substances, such as corticosteroids. Laser tattoo removal should be restricted to cases refractory to anti-inflammatory therapy.
Conclusion
The booming popularity of cosmetic permanent make-up has led to an increasing incidence of adverse tattoo reactions. While localized reactions are common and wellknown, spreading to distant un-tattooed sites should be considered in generalized dermatosis. In addition to dermatologists, the general public should be aware of potential severe complications of an otherwise harmless, optional esthetic intervention such as permanent make-up.
Key Message
This is the report of a generalized lichenoid reaction upon red permanent lip-liner make-up.
Conflict of Interest
None.
References
-
Laumann AE, Derick AJ (2006) Tattoos and body piercings in the United States: A national data set. J Am Acad Dermatol 55: 413-421.
-
Wenzel SM, Welzel J, Hafner C, Landthaler M, Bäumler W (2010) Permanent make-up colorants may cause severe skin reactions. Contact Dermatitis 63: 223-227.
-
Litak J, Ke MS, Gutierrez MA, Soriano T, Lask GP (2007) Generalized lichenoid reaction from tattoo. Dermatol Surg 33: 736-740.
-
Fang HY, Wu PY, Hsieh HJ (2013) Generalized lichenoid tattoo reaction with spontaneous resolution after skin biopsy. Dermatol Sinica 31: 38-40.
-
Greve B, Chytry R, Raulin C (2003) Contact dermatitis from red tattoo pigment (quinacridone) with secondary spread. Contact Dermatitis 49: 265-266.
-
Serup J, Hutton Carlsen K (2014) Patch test study of 90 patients with tattoo reactions: negative outcome of allergy patch test to baseline batteries and culprit inks suggests allergen(s) are generated in the skin through haptenization. Contact Dermatitis 71: 255-263.
-
Corazza M, Zampino MR, Montanari A, Pagnoni A, Virgili A (2002) Lichenoid reaction from a permanent red tattoo: has nickel a possible aetiologic role? Contact Dermatitis 46: 114-115.
-
Weiss G, Shemer A, Trau H (2002) The Koebner phenomenon: review of the literature. J Eur Acad Dermatol Venereol 16: 241-248.
-
Shelley WB, Arthur RP (1958) Biochemical and physiological clues to the nature of psoriasis. AMA Arch Derm 78: 14-29.
-
Quint KD, Genders RE, Vermeer MH (2012) A delayed granulomatous reaction to a cosmetic tattoo of the eyebrows: a report of total regression after intralesional corticosteroid injections. Dermatol Surg 38: 951-953.
-
Wylie G, Gupta G (2008) Lip-enhancing tattoo reaction resolving with topical tacrolimus. Clin Exp Dermatol 33: 505-506.
-
Anderson RR, Geronemus R, Kilmer SL, Farinelli W, Fitzpatrick RE (1993) Cosmetic tattoo ink darkening. A complication of Q-switched and pulsed-laser treatment. Arch Dermatol 129: 1010-1014.
-
Wang CC, Huang CL, Sue YM, Lee SC, Leu FJ (2013) Treatment of cosmetic tattoos using carbon dioxide ablative fractional resurfacing in an animal model: a novel method confirmed histopathologically. Dermatol Surg 39: 571-577.
-
Ibrahimi OA, Syed Z, Sakamoto FH, Avram MM, Anderson RR (2011) Treatment of tattoo allergy with ablative fractional resurfacing: a novel paradigm for tattoo removal. J Am Acad Dermatol 64: 1111-1114.
-
Antony FC, Harland CC (2003) Red ink tattoo reactions: successful treatment with the Q-switched 532 nm Nd:YAG laser. Br J Dermatol 149: 94-98.
-
De Argila D, Chaves A, Moreno JC (2004) Erbium: Yag laser therapy of lichenoid red tattoo reaction. J Eur Acad Dermatol Venereol 18: 332-333.
-
England RW, Vogel P, Hagan L (2002) Immediate cutaneous hypersensitivity after treatment of tattoo with Nd: YAG laser: a case report and review of the literature. Ann Allergy Asthma Immunol 89: 215-217.