International Journal of Neurology and Neurotherapy
Current Pharmacotherapy Strategies and Considerations for the Cognitive Dysfunction Associated with Schizophrenia: A Mini Review
Hikaru Hori*, Reiji Yoshimura, Asuka Katsuki, Kiyokazu Atake and Jun Nakamura
Department of Psychiatry, University of Occupational and Environmental Health, Japan
*Corresponding author:
Hikaru Hori, Department of Psychiatry, University of Occupational and Environmental Health, 1-1 Iseigaoka, Yahatanishi-ku, Kitakyushu, Fukuoka 8078555, Japan, Tel: +81936917253, Fax: +81936924894, E-mail: hori-h@med.uoeh-u.ac.jp
Int J Neurol Neurother, IJNN-2-024, (Volume 2, Issue 1), Mini Review; ISSN: 2378-3001
Received: February 27, 2015 | Accepted: March 17, 2015 | Published: March 19, 2015
Citation: Hori H, Yoshimura R, Katsuki A, Atake K, Nakamura J (2015) Current Pharmacotherapy Strategies and Considerations for the Cognitive Dysfunction Associated with Schizophrenia: A Mini Review. Int J Neurol Neurother 2:024. 10.23937/2378-3001/2/1/1024
Copyright: © 2015 Hori H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Cognitive dysfunction associated with schizophrenia is a core symptom that is strongly related to functional levels. In fact, cognitive dysfunction in patients with schizophrenia is due to a combination of the cognitive impairment induced by schizophrenia itself and that induced by the medications that psychiatrists prescribe. It is difficult to differentiate between the two sources, and at present, no medications have a large effect size in terms of improving the cognitive dysfunction induced by the disease itself. Therefore psychiatrists should strive to minimize drug-induced cognitive dysfunction when prescribing medications. In view of the cognitive dysfunction that patients with schizophrenia experience, it is important for psychiatrists who prescribe psychotropic agents to decrease chlorpromazine-equivalent doses and to dose each atypical antipsychotic as a monotherapy. The psychiatrist should avoid the chronic administration of the anticholinergic agents and benzodiazepines. In addition, adherence is important for preventing relapses, which can decrease cognitive function. In patients with schizophrenia, it is important to balance pharmacotherapy with the consideration of factors that contribute to cognitive dysfunction. The development of medications that can effectively treat the cognitive dysfunction caused by the disease itself is eagerly anticipated.
Keywords
Schizophrenia, Cognitive function, Pharamacotherapy, adherence, atypical antipsychotic
Introduction
The estimated prevalence of cognitive dysfunction in schizophrenia patients is 75% to 85%. Cognitive dysfunction is considered a core feature of the disease because it significantly affects patients' social and occupational functioning [1,2]. A meta-analysis of clinical trials investigating the effectiveness of antipsychotics on cognitive function in schizophrenia found that second-generation antipsychotics (SGAs) are slightly more effective than first-generation antipsychotics (FGAs), and each drug exerts a different effect on cognitive function [3]. However, recent studies have indicated that antipsychotics are limited in how much they can improve patients' cognitive function [4,5]. The cognitive dysfunction in schizophrenia consists of both disease-related impairment and antipsychotic drug-induced impairment, and it is difficult to distinguish between these two etiologies. Drug-induced cognitive impairment is caused by the psychoactive drugs that psychiatrists prescribe. Currently, the disease-related cognitive impairment is considered difficult to treat, whereas drug-induced cognitive impairment may be treatable or preventable.
This paper reviews pharmacological strategies that can help psychiatrists when treating schizophrenia patients with cognitive dysfunction.
Antipsychotic Polypharmacy and Cognitive Function
Antipsychotic polypharmacy is associated with reduced adherence, increased cost and a greater frequency of side effects [6-8]. Many patients with schizophrenia received antipsychotic polypharmacy. Polypharmacy has been found to adversely affect extrapyramidal symptoms, metabolic syndromes and oversedation in addition to cognitive functions [9,10]. We previously reported that even combined drug therapy that used atypical antipsychotics with reduced likelihoods of inducing adverse reactions had adverse effects on cognitive function [10]. A study investigating the effectiveness of switching from antipsychotic polypharmacy to monotherapy showed that the patients who switched to monotherapy showed greater improvement on measure of attention and processing speed compared with who continued with polypharmacy [11].
In addition, the dopamine supersensitivity reaction in schizophrenia is somewhat similar to the dopamine supersensitivity that is induced by antipsychotic drugs. The probability that antipsychotic drugs induced dopamine supersensitivity can lead to cognitive difficulties is shown by the fact that D2 receptors, selectively genetically elevated in the striatum, reduced cognitive performance in animals [12]. Attention and memory problems in schizophrenia may directly result from dopamine overstimulation and are worsened by the lowered self-confidence that ensure from them.
These results indicate that monotherapy is less detrimental to cognitive function than antipsychotic polypharmacy.
Antipsychotic Dose and Cognitive Function
Several studies have reported that consuming large amounts of antipsychotics has harmful effects on cognitive function, suggesting that the amount of drugs consumed is positively correlated with the degree of possible harm to cognitive function. In fact, a study investigating the relationship between cognitive dysfunction and the occupancy rate of dopamine D2 receptors, estimated by the concentration of antipsychotics, showed that the a D2 receptor occupancy rate of 77% or higher may be related to cognitive impairment [13] . Recent studies have suggested that the effects of antipsychotics on cognitive function may vary depending on the dose of each drug [10,14,15]. We previously reported that risperidone and olanzapine doses were adversely correlated with cognitive function in patients with chronic schizophrenia, but the dose of aripiprazole monotherapy did not show the same relationship [16]. Takeuchi et al. reported that reduced doses of risperidone and olanzapine led to improvements in cognitive function. These results suggest that although the dose of antipsychotics relates to cognitive function, the pharmacological profile may be different for each antipsychotic in monotherapy [17].
Anticholinergic Drugs and Cognitive Function
Anticholinergic drugs are commonly used to treat extrapyramidal symptoms in patients with schizophrenia. However, the long-term use of anticholinergic drugs for schizophrenic patients leads to impairments in attention, memory, learning ability, and executive function. Mori et al. reported that reducing or discontinuing anticholinergic drugs led to improvements in immediate memory and verbal working memory in patients who were concurrently taking FGAs or risperidone [18]. Furthermore, Ogino et al. reported that the gradual discontinuation of biperiden in chronic schizophrenia patients who were concurrently treated with SGA monotherapy lead to improvements in motor function, attention, processing speed, and verbal fluency [19]. Therefore, treatment strategies should include selecting drugs that have a lower risk of inducing extrapyramidal symptoms, avoiding polypharmacy, and avoiding the use of anticholinergic drugs.
Benzodiazepines and Cognitive Function
In schizophrenia treatment, benzodiazepines(BZDs) are usually prescribed for agitation, anxiety, insomnia, catatonia, panic attacks, and extrapyramidal symptoms either as a monotherapy or as an adjunct to antipsychotic drugs [20-22]. However, BZDs can cause various adverse effects, such as sedation, ataxia, behavioral disinhibition, dependence, abuse, and withdrawal symptoms upon cessation [23]. In addition, the long-term use of BZDs has been shown to cause impairments in a variety of cognitive functions, including attention, verbal learning, memory, processing speed, and visuospatial ability [24-26]. A meta-analysis of the effects of benzodiazepines tapering on cognitive function in schizophrenia found that tapering led to improvement in verbal memory and working memory [27]. The results of a secondary analysis examining the differences between the complete discontinuation and incomplete discontinuation groups suggested that improvements in working memory could be achieved even with the incomplete discontinuation of daytime benzodiazepines.
Adherence and Cognitive Function
It has been repeatedly noted that schizophrenia patients have poor treatment adherence [28-30]. Poor treatment adherence is the most predictive factor for the relapse of schizophrenia. Disease relapse results in further deteriorations of cognitive function. Therefore, the prevention of relapse is an important pharmacological strategy.
Summary
This review summarizes the current state of research on the effects of pharmacotherapy on cognitive function in patients with schizophrenia (Figure 1). Although atypical antipsychotics were expected to be effective for improving cognitive function, the effect size was moderate, and atypical antipsychotics can even be harmful depending on their dose and prescription pattern. Based on the current evidence, psychiatrists should minimize the occurrence of drug-induced cognitive dysfunction. To achieve this goal, antipsychotic monotherapy with careful dosing consideration is important. Regarding concurrently prescribed drugs, anticholinergics and benzodiazepines should be administered with care. In addition, relapse prevention is important because cognitive function deteriorates after each relapse. Finally, the most important factor predicting relapse is treatment adherence. Pharmacotherapy should consider these points. In the future, it is expected that a new drug that specifically targets cognitive impairment will be developed and will contribute to the functional outcomes of patients with schizophrenia.
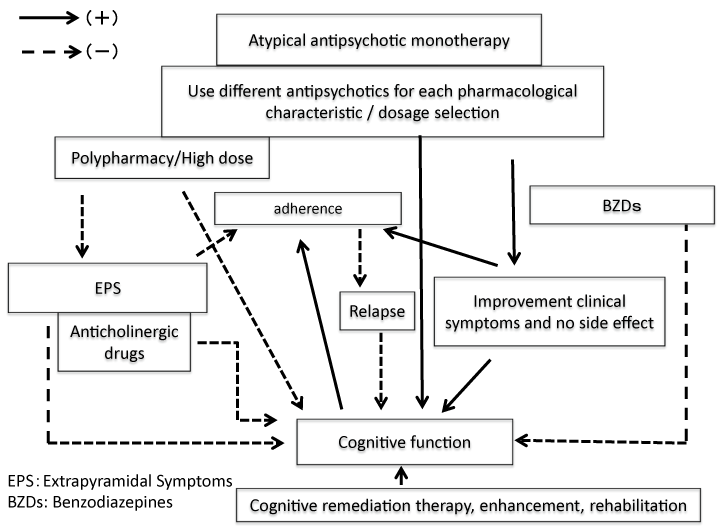
Figure 1: Pharmacotherapy on cognitive function in patients with schizophrenia
View Figure 1
References
-
Green MF (1996) What are the functional consequences of neurocognitive deficits in schizophrenia? Am J Psychiatry 153: 321-330.
-
Green MF, Kern RS, Braff DL, Mintz J (2000) Neurocognitive deficits and functional outcome in schizophrenia: are we measuring the "right stuff"? Schizophr Bull 26: 119-136.
-
Keefe RS, Silva SG, Perkins DO, Lieberman JA (1999) The effects of atypical antipsychotic drugs on neurocognitive impairment in schizophrenia: a review and meta-analysis. Schizophr Bull 25: 201-222.
-
Keefe RS, Bilder RM, Davis SM, Harvey PD, Palmer BW, et al. (2007) Neurocognitive effects of antipsychotic medications in patients with chronic schizophrenia in the CATIE Trial. Arch Gen Psychiatry 64: 633-647.
-
Goldberg TE, Keefe RS, Goldman RS, Robinson DG, Harvey PD (2010) Circumstances under which practice does not make perfect: a review of the practice effect literature in schizophrenia and its relevance to clinical treatment studies. Neuropsychopharmacology 35: 1053-1062.
-
Miller AL, Craig CS (2002) Combination antipsychotics: pros, cons, and questions. Schizophr Bull 28: 105-109.
-
Stahl SM (2002) Antipsychotic polypharmacy: squandering precious resources? J Clin Psychiatry 63: 93-94.
-
Suzuki T, Uchida H, Takeuchi H, Nomura K, Tanabe A, et al. (2005) Simplifying psychotropic medication regimen into a single night dosage and reducing the dose for patients with chronic schizophrenia. Psychopharmacology (Berl) 181: 566-575.
-
Essock SM, Schooler NR, Stroup TS, McEvoy JP, Rojas I, et al. (2011) Effectiveness of switching from antipsychotic polypharmacy to monotherapy. Am J Psychiatry 168: 702-708.
-
Hori H, Yoshimura R, Katsuki A, Hayashi K, Ikenouchi-Sugita A, et al. (2012) Several prescription patterns of antipsychotic drugs influence cognitive functions in Japanese chronic schizophrenia patients. Int J Psychiatry Clin Pract 16: 138-142.
-
Hori H, Yoshimura R, Katsuki A, Sugita AI, Atake K, et al. (2013) Switching to antipsychotic monotherapy can improve attention and processing speed, and social activity in chronic schizophrenia patients. J Psychiatr Res 47: 1843-1848.
-
Kellendonk C, Simpson EH, Polan HJ, Malleret G, Vronskaya S, et al. (2006) Transient and selective overexpression of dopamine D2 receptors in the striatum causes persistent abnormalities in prefrontal cortex functioning. Neuron 49: 603-615.
-
Sakurai H, Bies RR, Stroup ST, Keefe RS, Rajji TK, et al. (2013) Dopamine D2 receptor occupancy and cognition in schizophrenia: analysis of the CATIE data. Schizophr Bull 39: 564-574.
-
Hori H, Noguchi H, Hashimoto R, Nakabayashi T, Omori M, et al. (2006) Antipsychotic medication and cognitive function in schizophrenia. Schizophr Res 86: 138-146.
-
Elie D, Poirier M, Chianetta J, Durand M, Grégoire C, et al. (2010) Cognitive effects of antipsychotic dosage and polypharmacy: a study with the BACS in patients with schizophrenia and schizoaffective disorder. J Psychopharmacol 24: 1037-1044.
-
Hori H, Yoshimura R, Katsuki A, Hayashi K, Ikenouchi-Sugita A, et al. (2012) The cognitive profile of aripiprazole differs from that of other atypical antipsychotics in schizophrenia patients. J Psychiatr Res 46: 757-761.
-
Takeuchi H, Suzuki T, Remington G, Bies RR, Abe T, et al. (2013) Effects of risperidone and olanzapine dose reduction on cognitive function in stable patients with schizophrenia: an open-label, randomized, controlled, pilot study. Schizophr Bull 39: 993-998.
-
Mori K, Yamashita H, Nagao M, Horiguchi J, Yamawaki S (2002) Effects of anticholinergic drug withdrawal on memory, regional cerebral blood flow and extrapyramidal side effects in schizophrenic patients. Pharmacopsychiatry 35: 6-11.
-
Ogino S, Miyamoto S, Tenjin T, Kitajima R, Ojima K, et al. (2011) Effects of discontinuation of long-term biperiden use on cognitive function and quality of life in schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry 35: 78-83.
-
Fleischhacker WW (2003) New developments in the pharmacotherapy of schizophrenia. J Neural Transm Suppl : 105-117.
-
Higuchi H, Kamata M, Yoshimoto M, Shimisu T, Hishikawa Y (1999) Panic attacks in patients with chronic schizophrenia: a complication of long-term neuroleptic treatment. Psychiatry Clin Neurosci 53: 91-94.
-
Kane JM (1996) Schizophrenia. N Engl J Med 334: 34-41.
-
Rickels K, DeMartinis N, Rynn M, Mandos L (1999) Pharmacologic strategies for discontinuing benzodiazepine treatment. J Clin Psychopharmacol 19: 12S-16S.
-
Ashton H (2005) The diagnosis and management of benzodiazepine dependence. Curr Opin Psychiatry 18: 249-255.
-
Barker MJ, Greenwood KM, Jackson M, Crowe SF (2004) Persistence of cognitive effects after withdrawal from long-term benzodiazepine use: a meta-analysis. Arch Clin Neuropsychol 19: 437-454.
-
Stewart SA (2005) The effects of benzodiazepines on cognition. J Clin Psychiatry 66 Suppl 2: 9-13.
-
Barker MJ, Greenwood KM, Jackson M, Crowe SF (2004) Cognitive effects of long-term benzodiazepine use: a meta-analysis. CNS Drugs 18: 37-48.
-
Cramer JA, Rosenheck R (1998) Compliance with medication regimens for mental and physical disorders. Psychiatr Serv 49: 196-201.
-
Gilmer TP, Dolder CR, Lacro JP, Folsom DP, Lindamer L, et al. (2004) Adherence to treatment with antipsychotic medication and health care costs among Medicaid beneficiaries with schizophrenia. Am J Psychiatry 161: 692-699.
-
Kane JM, Kishimoto T, Correll CU (2013) Non-adherence to medication in patients with psychotic disorders: epidemiology, contributing factors and management strategies. World Psychiatry 12: 216-226.





