International Journal of Neurology and Neurotherapy
Permanent Memory Deficits with Normal MRI Following Heat Stroke after Physical Activity and Sauna
Massimiliano Ruggeri1,2* and Priscilla Rosini2
1Department of Neuroscience, San Camillo-Forlanini Hospital, Rome, Italy
2Rehabilitation Center C.A.R., Rome, Italy
*Corresponding author:
Massimiliano Ruggeri, Department of Neuroscience, San Camillo-Forlanini Hospital, Circonvallazione Gianicolense 87, 00152 Rome, Italy, E-mail: massimiliano.ruggeri@uniroma1.it
Int J Neurol Neurother, IJNN-3-050, (Volume 3, Issue 3), Case Report; ISSN: 2378-3001
Received: January 10, 2016 | Accepted: June 22, 2016 | Published: June 24, 2016
Citation: Ruggeri M, Rosini P (2016) Permanent Memory Deficits with Normal MRI Following Heat Stroke after Physical Activity and Sauna. Int J Neurol Neurother 3:050. 10.23937/2378-3001/3/3/1050
Copyright: © 2016 Ruggeri M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Heat stroke is the result of high heat stress and determines multi-organ dysfunction with predominant encephalopathy. Heat stroke only rarely leads to permanent neurologic deficits with a propensity to cerebellar dysfunction while memory disorders are very unusual. We report a unique case of a patient who suffered from a heat stroke after strenuous physical activity and sauna, resulting in persistent memory deficit with normal acute and follow-up normal MRI. Neuropsychological assessment suggested an involvement of the hippocampal-depending memory process. This is the only case in literature with long-lasting memory deficit with no MRI abnormalities, following heat stroke after excessive exercise and sauna.
Keywords
Heat stroke, Memory disorder, MRI, Sauna, Physical activity
Introduction
Heat stroke (HS) is a life threatening illness that occurs after exposure to high environmental temperature (classic or non-exertional) or strenuous physical activity (exertional). HS is defined as a form of hyperthermia associated with a complex response of heat cytotoxic effects and patient's inflammatory and coagulation response, leading to a syndrome of multiorgan dysfunction with predominant encephalopathy [1].
HS is clinically defined by high body temperature rising above 40°, together with history of exposure to heat stress, and mental abnormalities, such as confusion, seizures and deep coma. Central nervous system injuries may be explained by numerous pathological mechanisms: vasogenic edema and microvascular thrombosis with subsequent small vessels ischemic damage, and cytotoxic effect of the heat on most vulnerable cells [2]. Brain damage after HS usually involves cerebellum, being the Purkinje cells more vulnerable to heat stress [3], but differs in supratentorial findings, involving also basal ganglia, thalamus, and cerebral cortex, and rarely in the medial temporal lobes [4-8]. Given the neurological presentation of HS, brain computed tomography (CT) and magnetic resonance imaging (MRI) scans are normal in many cases, providing rare findings of cerebral edema, atrophy, or ischemic-hypoxic damage [9].
Recovery from HS is usually complete. In rare cases permanent neurological deficitsentail mainly cerebellar dysfunctions while cognitive deficits are very unusual [10]. Only in two patients persistent memory disorders in association with MRI findings of bilateral thalamic or hippocampal damage have been reported [5,8], and to the best of our knowledge there is no case study reporting patients with persistent memory deficit with normal MRI findings.
Case Report
The patient was a 60-year-old male, preparing for a triathlon marathon, with negative neurologic and psychiatric history and without medication. He had experienced diarrhea and mild nausea during the days before heat stroke (later recognized as a prodromal symptom). The patient lost consciousness in a sauna following three hours of strenuous physical activity in a gym center. On admission to hospital, he was unconscious (Glasgow Coma Scale 7) and his body temperature was 39°C. No specific cooling procedures were administered either on field or in the hospital. He showed miotic pupils, no motor responses to noxious stimuli, and athetotic movements. The EEG was normal, while a brain CT showed bilateral temporal lobe edema. He was intubated and ventilated, and remained in deep coma for 24 hours. The brain MRI performed 24 hours after onset was normal. There were no signs of liver or renal failure, but later he developed coagulopathy, thrombocytopenia and leukocytosis. On awakening, he was stuporous, confused and amnesic. During the following week, he recovered from his clinical status, improving memory functions and showing no motor impairments. He was discharged from the hospital 11 days after HS in general discrete clinical conditions.
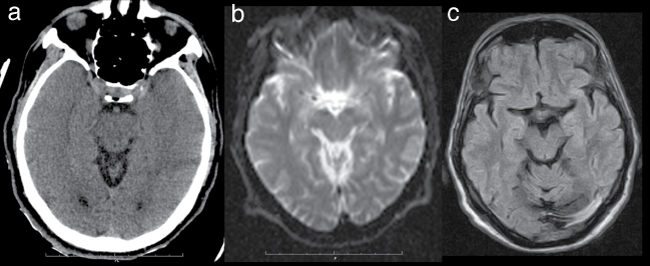
Initial brain CT scans immediately after the stroke showed swelling in the bilateral temporal lobe and hippocampus with reduced visualization of the cortical circonvolutions and loss of gray-white matter differentiation, as a consequence of vasogenic edema (Figure 1a). Brain MRI study, acquired on a 1.5 Tesla scanner 24 hours after onset, showed no signal abnormalities in the diffusion weighted images (DWI) (Figure 1b) and apparent diffusion coefficient (ADC), indicating no cytotoxic edema. Also fluid attenuated inversion recovery (FLAIR), T1- and T2-weighted images were normal. In a follow-up clinical evaluation six months after the onset, the MRI study was unchanged in the FLAIR (Figure 1c), T1- and T2-weighted images, showing no long-term hypoxic-ischemic damages to cortical, subcortical, or cerebellar sites.
.
Figure 1:(a) Initial brain CT scans show swelling of the bilateral temporal lobes as from vasogenic edema;
(b) DWI 24 hours after onsetreveals no signal abnormalities indicating resolution of edema;
(c) FLAIR images 6 months after the onset show no hypoxic-ischemic injuries of the brain.
View Figure 1
Six months after the onset the patient was attentive and well oriented in time and place. He could recall remote events immediately before the HS as well as most of his recent personal events and social facts. He returned to his previous job as a business consultant, but complained of memory problems in everyday life. Language and emotional-behavioral functions were adequate.
Neuropsychological assessment showed normal performances in attentional, executive and language tests. Attentional processes were measured by four subtests of the Test of Attentional Performance: alertness, go/no-go, divided attention and working memory [11]. Verbal and visual-spatial short-term memory were excellent. However, he showed impaired performances in both verbal and visual-spatial long-term memory tests. Immediate recall on the Rey Auditory Verbal Learning Test was in the normal range, with a mildrecency effect, while delayed recall and recognition were impaired, with no intrusions or false positives. Story recall was normal and not confabulating. In the Corsisupra-spantest, he was unable to learn the eight-block sequence despite 18 trials, with recall not exceeding his short-term span. In addition, delayed recall of the Rey Complex Figure was very poor. Performances on the Rivermead Behavioural Memory Test were below normal limits, with more prominent difficulties on the prospective memory and remembering names tasks. Retrograde memory was normal (Table 1).
![]()
Table 1: Neuropsychological assessment 6 months after the heat stroke.
View Table 1
Discussion
In this report we describe a patient with permanent memory disorders after HS. Our patient is unique because this is the only case described in the literature with permanent memory impairment and normal MRI following HS after intense physical activity and sauna.
Most of the previously reported cases of HS showed cerebellar dysfunctions and motor impairments but this was not the case with our patient, whose motor performances were normal [3,4]. Only a few cases of memory impairments after HS have been reported, but none showed isolated memory deficit [5,6,8]. The three amnesic patients of Romero et al. (2000) also presented with dementia, behavioral disorders and disexecutive impairments, respectively. Case 3 resembled our patient, being moderately impaired in memory with normal MRI findings and mild disexecutive deficit [5]. The patient of Seong-Yi et al. [8], on the other hand, was severely amnesic, in association with hippocampal-retrosplenial damage in the MRI findings, but he also showed a mild deficit of executive functions [8,12]. In our opinion, in the above-mentioned studies the neuropsychological assessments lacked adequate measurements of attention and executive functions, and at the same time, structure-function relationships were not adequately outlined.
Out patient's memory disorders were characterized by deficit of recall and recognition, abnormal rate of forgetting, and normal memory for related material (Story recall). These findings suggested an impairment of the hippocampal-dependent encoding/storage processes, which is in line with the few previous findings of hippocampal involvement after HS [4,8], showing the hippocampus, as well as the cerebellum, thalamus, and basal ganglia, a selective vulnerability to HS and hypoxic damage [3,4]. Unlike previous case reports of HS, we accurately assessed the attentional functions of the patient by administering the Test of Attentional Performance [11] to rule out the possibility that attentional impairments could be a contributing factor in the memory deficit of our patient.
The striking contrast between our patient's persistent memory deficits and normal neuroradiological findings has never been reported in previous case studies, and represents an enigma. We hypothesize that the his permanent memory disorders were the expression of the initial transient edema of the temporal lobes, as the result of vasogenic edema from blood-brain barrier breakdown without definitive cell death, which might have resulted in subtle neuropathologic abnormalities of the medial temporal lobes, not identifiable at MRI scans.
This unique case suggests that, despite the widespread notion of complete recovery following HS, the long-lasting outcome can lead to permanent cognitive sequelae, despite resolution of the edema and normal MRI findings, challenging the view of a close correlation between imaging findings, clinical outcome and prognosis in HS. This points to a role for accurate neuropsychological examination and functional neuroimaging as good practice in the management of HS.
References
-
Bouchama A, Knochel JP (2002) Heat stroke. N Engl J Med 346: 1978-1988.
-
Leon LR, Helwig BG (2010) Heat stroke: role of the systemic inflammatory response. J Appl Physiol (1985) 109: 1980-1988.
-
Bazille C, Megarbane B, Bensimhon D, Lavergne-Slove A, Baglin AC, et al. (2005) Brain damage after heat stroke. J Neuropathol Exp Neurol 64: 970-975.
-
Mahajan S, Schucany WG (2008) Symmetric bilateral caudate, hippocampal, cerebellar, and subcortical white matter MRI abnormalities in an adult patient with heat stroke. Proc (Bayl Univ Med Cent) 21: 433-436.
-
Romero JJ, Clement PF, Belden C (2000) Neuropsychological sequelae of heat stroke: report of three cases and discussion. Mil Med 165: 500-503.
-
Rav-Acha M, Shuvy M, Hagag S, Gomori M, Biran I (2007) Unique persistent neurological sequelae of heat stroke. Mil Med 172: 603-606.
-
De Cori S, Biancofiore G, Bindi L, Cosottini M, Pesaresi I, et al. (2010) Clinical Recovery despite Cortical Cerebral and Cerebellar Damage in Heat Stroke. Neuroradiol J 23: 35-37.
-
Cha SY, Kang TH, Kim SJ, Lee HY, Kim HJ, et al. (2013) Selective anterograde amnesia associated with hippocampal and splenial damage after heat stroke. Clin Neurol Neurosurg 115: 1867-1870.
-
Dematte JE, O'Mara K, Buescher J, Whitney CG, Forsythe S, et al. (1998) Near-fatal heat stroke during the 1995 heat wave in Chicago. Ann Intern Med 129: 173-181.
-
Royburt M, Epstein Y, Solomon Z, Shemer J (1993) Long-term psychological and physiological effects of heat stroke. Physiol Behav 54: 265-267.
-
Zimmermann P, Fimm B (1995) Test for Attentional Performance (TAP). Psytest.
-
Pergola G, Suchan B (2013) Associative learning beyond the medial temporal lobe: many actors on the memory stage. Front Behav Neurosci 7: 162.





