International Journal of Ophthalmology and Clinical Research
Systemic Rituximab for Conjunctival Marginal Zone (Malt) Lymphoma is not Protective for Subsequent Disease Development in the Contralateral Eye
Konstantinos Kopsidas1*, Amit Arora1, Karim Hammamji1, Gordon Hay1, Victoria M.L. Cohen1, Mandeep S. Sagoo1,2, John L. Hungerford1 and P. Nicholas Plowman3
1Ocular Oncology Service, St. Bartholomew's Hospital and Moorfields Eye Hospital, London, UK
2UCL Institute of Ophthalmology, London, UK
3Department of Radiotherapy, St. Bartholomew�s Hospital, London, UK
*Corresponding author: Konstantinos Kopsidas, Moorfields Eye Hospital, 162 City Road, London EC1V 2PD, United Kingdom, E-mail: kkopsidas@hotmail.com
Int J Ophthalmol Clin Res, IJOCR-2-013, (Volume 2, Issue 1), Case Report; ISSN: 2378-346X
Received: October 07, 2014 | Accepted: February 20, 2015 | Published: February 23, 2015
Citation: Kopsidas K, Arora A, Hammamji K, Hay G, Cohen VML, et al. (2015) Systemic Rituximab for Conjunctival Marginal Zone (Malt) Lymphoma is not Protective for Subsequent Disease Development in the Contralateral Eye. Int J Ophthalmol Clin Res 2:013. 10.23937/2378-346X/1410013
Copyright: © 2015 Kopsidas K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: We report a case of a 35-year old male who presented with unilateral conjunctival extranodal marginal zone (MALT) lymphoma and underwent systemic Rituximab immunotherapy as primary treatment. After an excellent initial response and four years of complete remission he presents with MALT lymphoma to the contralateral conjunctiva.
Methods: MALT lymphoma is the most common lymphoid neoplasm of the conjunctiva, and has an indolent clinical course. Rare cases of spontaneous remission, bilateral involvement, systemic dissemination, and common local and contralateral relapses have been reported. Rituximab is a chimeric anti-CD20 antibody, currently used as first-line treatment of CD20 positive non-Hodgkin�s lymphoma. Several mechanisms can be responsible for rituximab resistance. Transformation of CD20 positive indolent to aggressive CD20 negative form is one of them.
Results: In this case, the patient did not demonstrate any systemic or orbital involvement. Both histological reports of the incisional biopsies revealed CD20 positive immunohistochemistry.
Conclusion: This is a highly unusual case of new primary conjunctival MALT lymphoma to the contralateral eye after systemic Rituximab treatment. This further supports the assumption that rituximab does not suppress MALT lymphoma formation in the long term in the other eye, suggesting that the predisposing immune factors are not annihilated by the course of rituximab. Long term review of these patients is therefore warranted.
Keywords
Conjunctiva, Orbit, MALT, Marginal zone, Lymphoma, Rituximab, CD20, B cell, Antibody
Introduction
Extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue (MALT lymphoma) is the most common lymphoid neoplasm of the conjunctiva. Orbital involvement and rarely a choroidal component [1] can occur, and this type of lymphoma is different to primary intraocular lymphoma of the vitreoretinal type [2,3]. It is characterized by painless, salmon-pink patches in the fornix or bulbar conjunctiva, and has an indolent clinical course (Figure 1). MALT lymphomas are diagnosed by their strong staining for CD20 and negative staining for CD10, CD23, and bcl6 (Figure 2). Both orbits are involved in 15% of the cases-some synchronous and some metachronous [4].
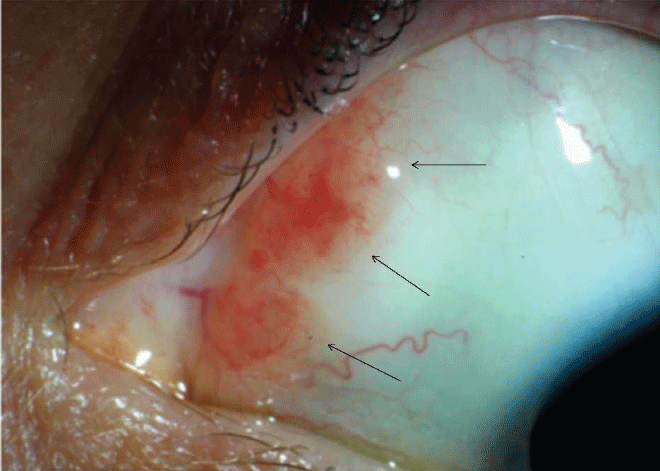
Figure 1: The slit-lamp examination of the left eye revealed a salmon-pink gelatinous lesion in the superonasal bulbar conjunctiva, confirmed immunohistochemically as mucosa-associated lymphoid tissue (MALT) lymphoma (arrows), 4 years after systemic rituximab for the treatment of conjunctival MALT lymphoma to the right eye.
View Figure 1
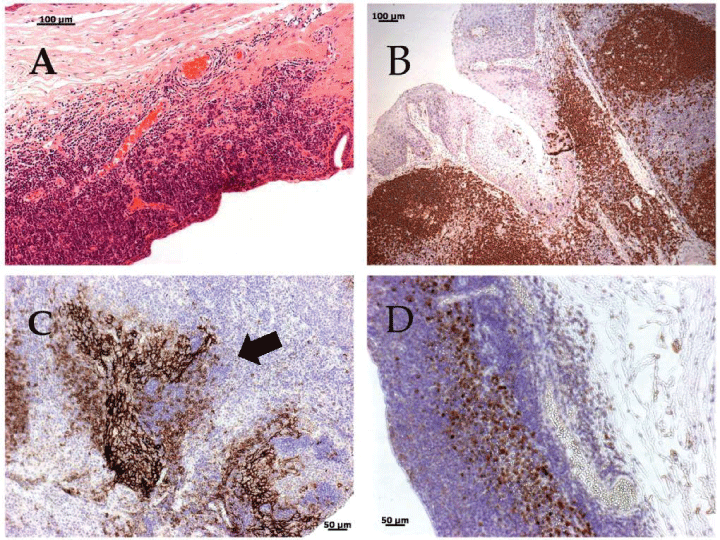
Figure 2: Immunohistochemistry of the lymphomatous tissue of the left eye. (A) H&E staining showing diffuse infiltrate of monomorphic small round blue cells. (B) CD20 positive staining of the majority of lymphoma cells (brown). (C) CD23 staining reveals expanded and disrupted germinal centers. The remnants of germinal centers are intensely stained, while the neoplastic cells are negative (Arrow), classically seen in MALT lymphoma.(D) BCL-6 negative staining for the majority of lymphomatous population, excluding follicular lymphoma.
View Figure 2
It has been reported that all orbital lymphomas have a 5-year relapse-free survival of 65%, although this increases to 85-90% for purely conjunctival lymphomas treated by conventional radiotherapy. Such cases usually involve the contralateral orbit and distant extranodal organs. Systemic dissemination occurs in 5-10% of cases, being rare in patients with conjunctival lymphoma [5]. In 10% of orbital lymphomas there is bilateral disease, despite the absence of direct lymphatic connections between the orbits- a fact that supports the theory of systemic predisposition rendering both orbits at risk of the disease. Only immunosuppression, for example related to organ transplantation [6], thyroid eye disease [7], or chronic chlamydial infection [5] are known predisposing factors.
Case Report
A 35-year-old white male presented with a salmon pink conjunctival mass in the right eye. Visual acuity was 6/6 in both eyes. There was no prior history of Chlamydial infection or thyroid eye disease. A diagnostic biopsy confirmed CD20 positive MALT lymphoma. The patient had no systemic symptoms. MRI scans of the head and orbits excluded intracranial or retrobulbar involvement.
Due to the young age of the patient, rituximab immunotherapy was commenced as primary treatment in order to avoid the side-effects of radiotherapy. A total of 6 courses of weekly rituximab at a dose of 375mg/m2 were delivered intravenously with excellent response. There was complete remission clinically without any evidence of lesion recurrence in a 4-year follow-up period.
After 4 years a similar conjunctival lesion appeared in the superior bulbar conjunctival surface of the contralateral eye (Figure 1). Diagnostic biopsy showed the same type of CD20 positive MALT lymphoma (Figure 2), and treatment with further intravenous rituximab has been successful.
Discussion
Rituximab is a chimeric antiCD20 monoclonal antibody that induces a rapid depletion of benign and malignant CD20 positive cells. Its cytotoxicity is based on the lysis of B cells by a complement and antibody dependent mechanism that induces apoptosis of malignant cells. Complete B cell depletion occurs in a matter of days, with B cells reaching normal levels usually after a period of 9�12 months [8,10].
Rituximab has shown efficacy in the treatment of conjunctival MALT lymphoma, with response rates between 50-87%. However, response duration is usually less than a year with a high relapse rate [4]. The response rate at relapse after use in prior responders is lower than 50% and probably less durable. This secondary resistance can be attributed to loss of CD20 expression after rituximab therapy or to conformation of the CD20 receptor that can be produced by the effect of medication such as statins [9,2].
This case is highly unusual in that there was contralateral involvement 4 years after successful treatment with systemic rituximab. This supports the notion that rituximab does not suppress MALT lymphoma formation in the long term in the other eye � perhaps demonstrating that the predisposing immune factors are not eradicated by the course of rituximab, and advocating for the long term follow-up of these patients.
References
-
Moslehi R, Devesa SS, Schairer C, Fraumeni JF Jr (2006) Rapidly increasing incidence of ocular non-hodgkin lymphoma. J Natl Cancer Inst 98: 936-939.
-
Sagoo MS, Mehta H, Swampillai AJ, Cohen VM, Amin SZ, et al. (2014) Primary Intraocular Lymphoma. Surv Ophthalmol 59: 503-516.
-
Coupland SE, Damato B (2008) Understanding intraocular lymphomas. Clin Experiment Ophthalmol 36: 564-578.
-
Coupland SE, Hummel M, Stein H (2002) Ocular adnexal lymphomas: five case presentations and a review of the literature. Surv Ophthalmol 47: 470-490.
-
Ferreri AJ, Dolcetti R, Du MQ, Doglioni C, Resti AG, et al. (2008) Ocular adnexal MALT lymphoma: an intriguing model for antigen-driven lymphomagenesis and microbial-targeted therapy. Ann Oncol 19: 835-846
-
Woolf DK, Ahmed M, Plowman PN (2012) Primary lymphoma of the ocular adnexa (orbital lymphoma) and primary intraocular lymphoma. Clin Oncol (R CollRadiol) 24: 339-344.
-
Nutting CM, Shah-Desai S, Rose GE, Norton AP, Plowman PN (2006) Thyroid orbitopathy possibly predisposes to late-onset of periocular lymphoma. Eye (Lond) 20: 645-648.
-
Dunleavy K, Hakim F, Kim HK, Janik JE, Grant N, et al. (2005) B-cell recovery following rituximab-based therapy is associated with perturbations in stromal derived factor-1 and granulocyte homeostasis. Blood 106:795-802.
-
Duman BB, Sahin B, Ergin M, Guvenc B (2012) Loss of CD20 antigen expression after rituximab therapy of CD20 positive B cell lymphoma (diffuse large B cell extranodal marginal zone lymphoma combination): a case report and review of the literature. Med Oncol 29:1223-1226.
-
Smith MR (2003) Rituximab (monoclonal anti-CD20 antibody): mechanisms of action and resistance. Oncogene 22:7359-7368.





