International Journal of Ophthalmology and Clinical Research
Retrospective Comparison of Scleral Flap and Scleral Burial Techniques to Fixate A Scleral Sutured Intraocular Lens Concurrently with Penetrating Keratoplasty
Bora Yuksel*, Alper Gulucu, Umut Duygu Uzunel and Tuncay Kusbeci
Department of Ophthalmology, Izmir Bozyaka Education and Research Hospital, Turkey
*Corresponding author: Dr. Bora Yuksel, Department of Ophthalmology, Izmir Bozyaka Education and Research Hospital, Karabaglar, Izmir- Turkey, Tel: 00.90.232.2505050, Fax: 00.90.232.2614444, E-mail: drborayuksel@gmail.com
Int J Ophthalmol Clin Res, IJOCR-2-034, (Volume 2, Issue 4), Research Article; ISSN: 2378-346X
Received: July 27, 2015 | Accepted: August 22, 2015 | Published: August 25, 2015
Citation: Yuksel B, Gulucu A, Uzunel UD, Kusbeci T (2015) Retrospective Comparison of Scleral Flap and Scleral Burial Techniques to Fixate A Scleral Sutured Intraocular Lens Concurrently with Penetrating Keratoplasty. Int J Ophthalmol Clin Res 2:034. 10.23937/2378-346X/1410034
Copyright: © 2015 Yuksel B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: To compare the outcomes of patients who underwent penetrating keratoplasty (PK) and transscleral sutured posterior chamber intraocular lens (TS PCIOL) implantation by using inside-out (open-sky) technique with scleral flap or scleral burial.
Methods: Data from all patients who had PK-TS PCIOL performed by the same surgeon (B.Y) between April 2004 and December 2013 were compiled. Fifty six eyes of 55 patients were analyzed. The patients were split into 2 groups: Group F (flap) consisted of 34 eyes of 33 patients who had PK-TS PCIOL with 10/0 prolene sutures. Scleral fixation knots were covered with a triangular scleral flap in those patients. Group B (burial) consisted of 22 eyes of 22 patients who had PK-TS PCIOL with 9/0 prolene sutures. In those patients, suture ends were buried into the sclera by using Baykara technique.
Results: Mean age was 58.0 ± 17.1 years, follow-up 19.9 ± 9.2 months in group F, 61.4 ± 15.2 and 18.1 ± 7.5 respectively in group B. Mean logMAR best spectacle-corrected visual acuity improved from 2.75 ± 0.51 to 1.59 ± 0.87 in group F (p<0.000), from 2.86 ± 0.47 to 1.35 ± 0.85 in group B postoperatively (p<0.000). Vitreous hemorrhage occurred in 7 eyes (20.6%) in group F, 2 eyes (9.1%) in group B. Seven suture erosion (20.6%) occurred in group F, none (0.0%) in group B. Postoperative IOP elevation in 10 eyes (29.4%) in group F, 11 eyes (50.0%) in group B. That elevation was statistically significant in group B (p=0.008). Graft survival rate at one year was 85.3% and 95.5% respectively (p=0.358). Cystoid macular edema was observed in 2 eyes of both groups. There were no dislocation, lens tilting, suture breakage or retinal detachment.
Conclusions: Scleral burial of prolene sutures during PK-TS PCIOL prevents exposure, shortens the surgical time and improves outcomes. However IOP should be monitored closely.
Keywords
Transscleral, Penetrating keratoplasty, Scleral flap, Scleral burial
Introduction
Definitive surgical treatment of aphakia in the presence of corneal opacity is secondary intraocular lens (IOL) implantation combined with penetrating keratoplasty (PK). The two main locations for IOL implantation are in the anterior chamber (ACIOL) and in the posterior chamber (PCIOL). Insertion of PCIOLs can be performed by capsular-supported, iris-supported, or transsclerally sutured PCIOL [1]. Each technique has strengths and weaknesses with respect to surgical difficulty, operative time, and complications [2]. For cases in which there is little or no capsular support, iris-sutured PCIOL and transscleral PCIOL (TS PCIOL) are preferred. Techniques for TS PCIOL vary and include the ab externo (outside-in) and the ab interno (inside-out or open-sky) approach [1].
Angle supported ACIOLs may be associated with various complications, such as endothelial cell loss, uveitis, cystoid macular edema (CME), angle damage, peripheral anterior synechiae, pupillary block, hyphema, iris pigment dispersion and secondary glaucoma [3-5]. Thus, TS PCIOL is preferred by many corneal surgeons in combination with PK [6-8]. However, TS PCIOLs are not free of complications. Suture breakage rate has been reported as 27.9% within 6 years [9]. Serious advers events have been encountered in 37% of the cases, including loss of light perception due to postoperative retinal detachment in 3 eyes [10] Suture exposure through the conjunctiva has ben reported in 11% of the patients within 12 months [11]. Whereas, Baykara reported no suture exposure with his scleral burial technique over 24 months [12].
The current study aims to compare the outcomes of patients who underwent PK- TS PCIOL with two different techniques including the covering the prolene suture knots under the scleral flap or burying them into the sclera. The results of 60 consecutive eyes are reviewed and advantages as well as complications of both methods are discussed.
Patients and Methods
Medical records of 56 eyes of 55 patients who had undergone TS PCIOL implantation in combination with PK between April 2004 and December 2013 at Izmir Bozyaka Education and Research Hospital were analyzed retrospectively. Patients with at least one year of follow-up were included into the study. 4 patients with shorter follow-up were excluded. The patients were split into 2 groups: Group F (flap) consisted of 34 eyes of 33 patients who had PK-TS PCIOL implantation between April 2004 and December 2011 with double thread10/0 polypropylene (prolene) sutures. Scleral fixation suture knots were tied, cut and free ends were covered with a triangular scleral flap in that group. Group B (burial) consisted of 22 eyes of 22 patients operated between January 2012 and December 2013 with 9/0 prolene sutures. In that group, suture ends were tied on each other. The long needle carrying that knot was passed once more through the sclera to bury them altogether underneath the sclera (Baykara's technique).
The medical records were reviewed for general demographics, preoperative and postoperative best spectacle-corrected visual acuity (BSCVA), date of and indication for surgery, surgical technique, intraoperative or postoperative complications, any subsequent surgical procedures required, and date of last follow-up. Intraocular pressure (IOP) was measured by Goldmann applanation tonometry. Values over 21.0mmHg at any point during follow-up were deemed IOP elevation requiring treatment. An allograft rejection was diagnosed if corneal clouding was noted in association with an epithelial or endothelial rejection line, keratic precipitates, and/or anterior chamber cells. Biometry was performed using contact A-scan ultrasound and keratometry. Corneal topography was performed with Keratograph III (Oculus, Wetzlar, Germany) after the removal of all running sutures. Optical coherence tomography (Cirrus 4000, Zeiss, Germany) was performed to confirm CME when suspected.
Surgical technique
All procedures were performed by a single surgeon (B.Y). Two-8 o'clock positions were marked. Three-9 axis was not preferred due to the location of the anterior ciliary arteries and long ciliary nerves. Prolene sutures were tied to the eyelets of a monobloc scleral-?xated IOL made of polymethyl methacrylate and 6.0×13.5mm in diameter. The conjunctiva was dissected at 2 and 8 o'clock quadrants. Two triangular scleral flaps were dissected at the limbus and a double-armed 10-0 prolene suture (Alcon PC-9, Texas, US) was used in group F. No flaps were dissected and a single thread 9-0 prolene suture (Mani 2452L, Tochigi, Japan) was used in group B. Donor corneas were cut from the endothelial side. Recipient corneas were trephined with a Hessburg-Barron vacuum trephine. The ACIOLs or dislocated PCIOLs were removed from the eye. Anterior vitrectomy was performed. Open-sky anterior segment reconstruction including goniosynechiolysis, membranectomy or iridoplasty was carried out. Long needles were passed through the corneal opening and brought out 1 mm behind the limbus. The IOL was centered behind the pupil. Corneal graft was sutured in place with a single 10-0 nylon running suture. Sutures were tightened. IOP was restored by injecting air or BSS. Prolene sutures were tightened and tied in aforementioned manner. The conjunctiva was closed and dexamethasone, gentamicin were injected subconjunctivally.
Statistics
The paired t-test, independent-samples t-test (Mann-Whitney U test and Kruskal-Wallis test) and Chi-square test (running in SPSS version 21.0) were used for statistical analysis; a p-value <0.05 was considered statistically significant.
Results
Demographic features as well as indications for PK, host trephine size and donor-host trephine disparities are shown in table 1. There was no statistically significant difference between two groups in terms of mean age, sex and PK indications. The only statistically significant difference was found in donor-host trephine disparity between two groups. A larger donor size had been chosen in group B compare to group F (p<0.000). 0.75mm larger donor had been used in 8 eyes of group B, whereas none in group F.
![]()
Table 1: Demographic features, PK indications, recipient trephine size and donor-host trephine disparities of the study eyes.
View Table 1
Preoperative fundus examination could be performed in only 3 eyes in each group because of the corneal opacity. The fundus was normal in 2 eyes in each group. 1 eye had CME in group F and 1 eye had macular pucker in group B. The retina was attached in the remaining eyes on ocular ultrasonography. Preexisting glaucoma was treated either medically or surgically prior to PK in all cases. For this purpose, trabeculectomy was performed in 3 eyes in both groups. Ahmed Valve (New World Medical Inc., CA) was implanted in 1 eye in each group.
Since penetrating trauma or complicated cataract surgery caused severe damage, most of the study eyes had disorganized anterior segments. Open-sky anterior segment reconstruction was performed in these eyes. There was no statistically significant difference between two groups in terms of concurrent procedures performed during PK (all p values>0.300, Chi-square test). Graft survival rate at the end of the 1st year, mean preoperative and postoperative BSCVA, IOP and follow-up of both groups may be seen in table 2.
![]()
Table 2: Comparison of group F and B in terms of graft survival at one year, mean preoperative and postoperative BSCVA, IOP and follow-up.
View Table 2
Although graft survival at one year was higher in group B, this difference was not statistically significant (p=0.358). There was no statistically significant difference in baseline BSCVA between the two groups (p=0.282). When visual acuities at the end of the first year were compared with baseline, a statistically significant improvement in BSCVA was found in both groups (p values were <0.001 in both groups, paired t-test). Mean logMAR BSCVA improved from 2.75 ± 0.51 to 1.59 ± 0.87 in group F and from 2.86 ± 0.47 to 1.35 ± 0.85 in group B.
When postoperative first year IOP values were compared with baseline values, no statistically significant IOP elevation was found in group F (p=0.052, paired t-test). Whereas, a statistically significant IOP elevation was observed in group B (p=0.008, paired t-test). Postoperative IOP elevation occurred in 10 (29.4%) of 34 eyes in group F, 11 (50.0%) of 22 eyes in group B during follow-up. It was controlled medically in most of the cases. Surgical intervention either trabeculectomy or Ahmed valve was required in 3 cases from each group. AC IOL appeared to be a risk factor for postoperative IOP elevation. The percentage of the patients with AC IOL was 14.7% in group F and 22.7% in group B. Overall, 10 (17.9%) of 56 eyes had IOP higher than 30mmHg and half of them had AC IOL. A subgroup analysis revealed that the eyes with AC IOL from both groups showed a statistically significant IOP elevation at 1 year compare to baseline (p?0.000, paired t-test). Mean IOP elevation was approximately 3mmHg.
Topographic analysis was achieved in 24 eyes with clear grafts in group F and 19 eyes in group B. Mean topographic astigmatism was 6.1 ± 3.2D in group F and 5.4 ± 3.8D in group B. The difference was not statistically significant (p=0.488, independent t-test). Intraoperative complications were vitreous hemorrhage in 7 eyes (20.6%) in group F, 2 eyes (9.1%) in group B, anterior chamber hemorrhage in 3 eyes (8.8%) in group F, 1 eye in group B (5.0%). Scleral flap hemorrhage occurred in 3 eyes of group F (8.8%). Reasons for poor vision despite a successful surgery were as follows: irregular astigmatism, corneal haze, maculopathy, CME, diabetic retinopathy, primary/glaucomatous optic atrophy and amblyopia. Late postoperative conditions are summarized in table 3.
![]()
Table 3: Late postoperative conditions.
View Table 3
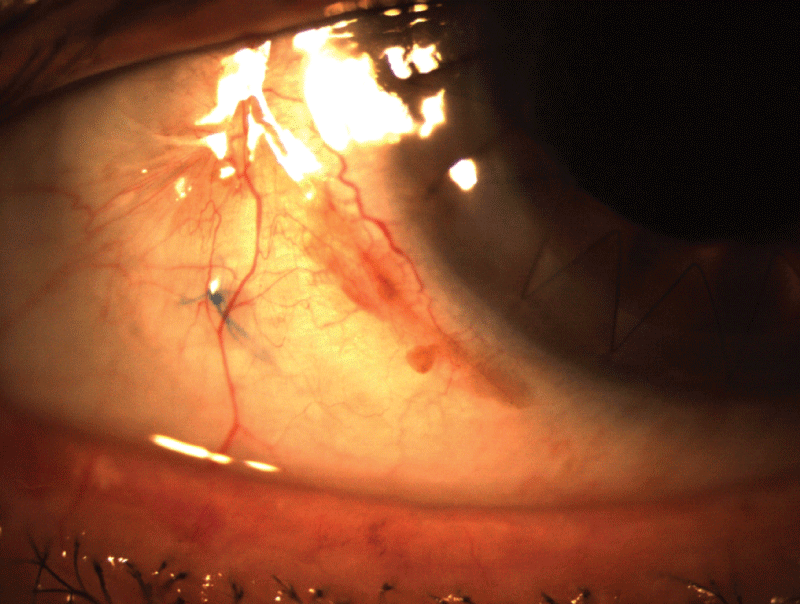
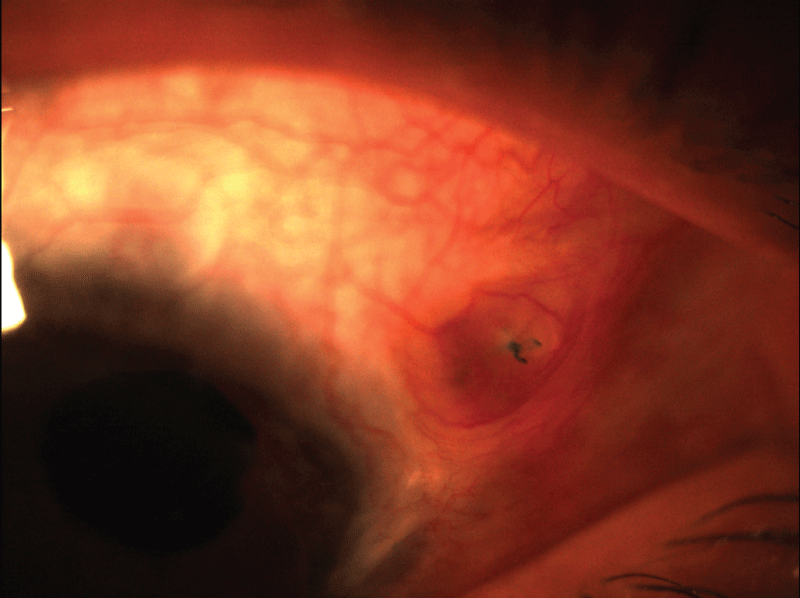
In group F; the cut ends of prolene sutures became exposed through the sclera and the conjunctiva in 7 eyes (20.6%) (Figure 1), whereas no exposure occurred in group B (Figure 2). The difference between two groups was statistically significant (p=0.023). Suture exposure occurred in 4 eyes within one year postoperatively and in 3 eyes beyond 2 years. Argon laser suturolysis was performed on these eyes to cease discomfort and prevent infection. There wasn't any statistically significant difference between two groups in terms of other complications.
.
Figure 1: Prolene suture exposure through the sclera and conjunctiva in an eye from group F
View Figure 1
Discussion
In our study, preoperative visual acuity was hand motions in 50.0% of the eyes in group F and 59.0% in group B. A statistically significant improvement was achieved in mean BSCVA after PK-TS PCIOL in both groups (p<0.001). Visual acuity improved in 82.4% of the eyes in group F and 95.5% in group B. This rate has been reported as 86.2% with PK-TS PCIOL [8]. Malta et al reported an improvement in 59.0% of the patients with 42.9% of the eyes 20/100 or better [6]. Postoperative BSCVA was higher than 20/400 in 44.2% of group F and 81.7% of group B eyes. Despite visual results of group F are lower than previous reports, the results of group B are comparable. Although graft survival at 1 year was higher in group B (86.5%) than group F (70.6%), this difference was not statistically significant. That rate was reported as 89.7% by Koçak-Altintas and 97.0% by Malta [6,8].
The most prominent difference between two groups was observed in prolene suture erosion (p=0.023). The cut ends of scleral fixation suture became exposed in 7 eyes (20.6%) in scleral flap group. Suture exposure occurred within 1 year in 4 eyes (11.7%) which is comparable to previous reports of 11%-17.0% in a year [11,13]. To prevent exposure, sutures are suggested to be cut long to lie parallel to the sclera [14]. Suture exposure may cause irritation, granuloma, giant papillary conjunctivitis, suture abscess and endophthalmitis [2,6,8,15]. No exposure was observed in group B eyes with Baykara's scleral burial technique [12]. Spontaneous dislocation of TS PCIOL is reported between 1.9 [6] to 27.9% [9,15] No dislocation occurred in our patients, like Kjeka's result [16]. Either double armed 10-0 prolene in group F or a single armed but thick 9-0 prolene in group B have provided strong fixation. However, crowded ends of double thread 10-0 suture under the scleral flap caused erosion. Although thicker, 9-0 prolene did not cause erosion, because it was buried parallel to the surface.
Although ACIOLs and iris-sutured PCIOLs are reported to be comparably safe for secondary implantation [17,18], the TS PCIOL is more appropriate in young patients [19] and in eyes with compromised cornea, anterior synechiae, shallow anterior chamber and glaucoma [1]. It is a preferred technique especially in combination with PK because of its anatomical location [4,5,7,8,16]. PK-TS PCIOL gives the surgeon access to the anterior segment via the open-sky approach and facilitates IOL explantation, anterior vitrectomy, synechiolysis, pupilloplasty and IOL implantation [20]. However, it carries expulsive hemorrhage risk and requires minimal maniplation. Thus, we have tried to work under a closed chamber as long as possible [7].
There are reports of TS PCIOL with favourable results, however, serious complications have also been reported [2,16,18]. Ciliary bleeding has been reported in 4.4% [16] and 52% [15,21]. It occurred 20.6% in group F and 9.1% in group B. Lower rate in group B may be a result of improving surgeon's skills over time. IOP elevation has been reported between 21.4 - 24.1% after PK-TS PCIOL [6,8]. It was observed 29.4% in group F and 50.0% in group B. Higher rate in group B may be a result of higher percentage of the eyes with an AC IOL. Another explanation is the more complicated anterior segment due to the selection of more difficult cases for surgery as a result of improved experience of the surgeon. IOP elevation was reported in 2.2% after TS PCIOL alone [16]. Higher rates in PK-TS PCIOL may be due to longer topical steroid use. CME was reported 17% in PK-TS PCIOL [6]. It occurred 5.9% in group F and 9.1% in group B. Retinal detachment may arise in 4.4% to 8.0% after TS PCIOL [16,22]. Retinal tears are usually related to vitreous incarceration [23]. It did not occur in our patients. This may be related to meticulous removal of the vitreous before IOL implantation.
In conclusion, despite its limitations of its single-center and retrospective nature, our study showed that the PK-TS PCIOL procedure, as done by the open-sky method, provides visual improvement with an acceptable rate of complications. Scleral flap cover of the prolene sutures is associated with a high rate of suture exposure. Scleral burial of the sutures prevents exposure and shortens the surgical time. However, close monitoring of IOP after surgery is mandatory. Further prospective randomized studies may shed light on the efficacy and safety of these two techniques.
Acknowledgements
This study has no financial support or conflict of interest. The study was approved by our institution's ethical committee and followed the tenets of Helsinki Declaration.
References
-
Nottage JM, Bhasin V, Nirankari VS (2009) Long-term safety and visual outcomes of transscleral sutured posterior chamber IOLs and penetrating keratoplasty combined with transscleral sutured posterior chamber IOLs. S Trans Am Ophthalmol Soc 107: 242-250.
-
Holt DG, Young J, Stagg B, Ambati BK (2012) Anterior chamber intraocular lens, sutured posterior chamber intraocular lens, or glued intraocular lens: where do we stand? S Curr Opin Ophthalmol 23: 62-67.
-
Hannush SB (2000) Sutured posterior chamber intraocular lenses: indications and procedure. S Curr Opin Ophthalmol 11: 233-240.
-
Ma LW, Xuan D, Li XY, Zhang JS (2011) Corneal astigmatism correction with scleral flaps in trans-scleral suture-fixed posterior chamber lens implantation: a preliminary clinical observation. S Int J Ophthalmol 4: 502-507.
-
Evereklioglu C, Er H, Bekir NA, Borazan M, Zorlu F (2003) Comparison of secondary implantation of flexible open-loop anterior chamber and scleral-fixated posterior chamber intraocular lenses. S J Cataract Refract Surg 29: 301-308.
-
Malta JB, Banitt M, Musch DC, Sugar A, Mian SI, et al. (2009) Long-term outcome of combined penetrating keratoplasty with scleral-sutured posterior chamber intraocular lens implantation. Cornea 28: 741-746.
-
Al-Qahtani FA (2010) Scleral fixation of intraocular lenses combined with penetrating keratoplasty. S J Cataract Refract Surg 36: 373-376.
-
Koçak-Altintas AG, Koçak-Midillioglu I, Dengisik F, Duman S (2000) Implantation of scleral-sutured posterior chamber intraocular lenses during penetrating keratoplasty. J Refract Surg 16: 456-458.
-
Vote BJ, Tranos P, Bunce C, Charteris DG, Da Cruz L (2006) Long-term outcome of combined pars plana vitrectomy and scleral fixated sutured posterior chamber intraocular lens implantation. S Am J Ophthalmol 141: 308-312.
-
Yang YF, Bunce C, Dart JK, Johnston RL, Charteris DG (2006) Scleral-fixated posterior chamber intraocular lenses in non-vitrectomized eyes. S Eye (Lond) 20: 64-70.
-
Djalilian AR, Anderson SO, Fang-Yen M, Lane SS, Holland EJ (1998) Long-term results of transsclerally sutured posterior chamber lenses in penetrating keratoplasty. S Cornea 17: 359-364.
-
Baykara M, Timucin OB (2008) Long-term results of a suture burial technique. S Eur J Ophthalmol 18: 368-370.
-
Solomon K, Gussler JR, Gussler C, Van Meter WS (1993) Incidence and management of complications of transsclerally sutured posterior chamber lenses. S J Cataract Refract Surg 19: 488-493.
-
Yalniz-Akkaya Z, Burcu A, Uney GO, Abay I, Eksioglu U, et al. (2014) Primary and secondary implantation of scleral-fixated posterior chamber intraocular lenses in adult patients. S Middle East Afr J Ophthalmol 21: 44-49.
-
Asadi R, Kheirkhah A (2008) Long-term results of scleral fixation of posterior chamber intraocular lenses in children. S Ophthalmology 115: 67-72.
-
Kjeka O, Bohnstedt J, Meberg K, Seland JH (2008) Implantation of scleral-fixated posterior chamber intraocular lenses in adults. S Acta Ophthalmol 86: 537-542.
-
Kwong YY, Yuen HK, Lam RF, Lee VY, Rao SK, et al. (2007) Comparison of outcomes of primary scleral-fixated versus primary anterior chamber intraocular lens implantation in complicated cataract surgeries. S Ophthalmology 114: 80-85.
-
Wagoner MD, Cox TA, Ariyasu RG, Jacobs DS, Karp CL; American Academy of Ophthalmology (2003) Intraocular lens implantation in the absence of capsular support: a report by the American Academy of Ophthalmology. S Ophthalmology 110: 840-859.
-
Dick HB, Augustin AJ (2001) Lens implant selection with absence of capsular support. S Curr Opin Ophthalmol 12: 47-57.
-
Hara T, Hara T (2004) Ten-year results of anterior chamber fixation of the posterior chamber intraocular lens. S Arch Ophthalmol 122: 1112-1116.
-
Almashad GY, Abdelrahman AM, Khattab HA, Samir A (2010) Four-point scleral fixation of posterior chamber intraocular lenses without scleral flaps. S Br J Ophthalmol 94: 693-695.
-
Hyun DW, Lee TG, Cho SW (2009) Unilateral scleral fixation of posterior chamber intraocular lenses in pediatric complicated traumatic cataracts. S Korean J Ophthalmol 23: 148-152.
-
Bourke RD, Gray PJ, Rosen PH, Cooling RJ (1996) Retinal detachment complicating scleral-sutured posterior chamber intraocular lens surgery. S Eye (Lond) 10: 501-508.