International Journal of Ophthalmology and Clinical Research
Relationship between Full-Thickness Macular Hole and Retinal Break/Lattice Degeneration
Jinglin Zhang1, Yonghao Li2, Xiujuan Zhao2, Yu Cai2, Xiling Yu2 and Lin Lu2*
1Guangzhou Aier Eye Hospital, Aier Eye Hospital Group, China
2The State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-Sen Unversity, China
*Corresponding author: Lin Lu, MD, Ph.D, The State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-Sen University, Guangzhou 510060, China, E-mail: lulin888@126.com
Int J Ophthalmol Clin Res, IJOCR-2-036, (Volume 2, Issue 5), Research Article; ISSN: 2378-346X
Received: July 25, 2015 | Accepted: August 26, 2015 | Published: September 02, 2015
Citation: Zhang J, Li Y, Zhao X, Cai Y, Yu X, et al. (2015) Relationship between Full-Thickness Macular Hole and Retinal Break/Lattice Degeneration. Int J Ophthalmol Clin Res 2:036. 10.23937/2378-346X/1410036
Copyright: © 2015 Zhang J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: To investigate the relationship between full-thickness macular hole and retinal break (RB) and/or lattice degeneration.
Methods: Patients diagnosed as full-thickness macular hole and referred to Dr. Lin Lu from January 2009 to December 2013 were evaluated. All patients underwent general ophthalmologic examinations, fundus examination and optical coherence tomography (OCT). The RB and/or lattice degeneration were recorded.
Results: Totally 166 eyes of 151 patients were included. All the eyes were phakic. The sex ratio of men to women was 1:3.36. RB and/or lattice degeneration were found in 59 eyes (35.54%). The prevalence of RB and/or lattice degeneration was similar between men and women (p = 0.561). All of the RB and/or lattice degeneration were located near or anterior to the equator. The inferior quadrants and the vertical meridian were affected more often than the superior quadrants and the horizontal meridian.
Conclusion: We identified a high incidence of retinal breaks/lattice degeneration in cases of full-thickness macular hole. Carefully examination of the peripheral retina and prophylactic treatment of retinal breaks and/or lattice degeneration are critical.
Keywords
Macular hole, Retinal break, Lattice degeneration, Optical coherence tomography, Vitreous retinopathy
Introduction
The pathogenesis of full-thickness macular hole (MH) is not clearly understood but is believed to involve anteroposterior traction and/or tangential traction exerted by the posterior vitreous cortex at the fovea [1]. Retinal break (RB) and lattice degeneration are one of the most important abnormalities of vitreous and vitreoretinal interface. To figure out the relationship between the full-thickness macular hole and RB/lattice degeneration may contribute to the understanding of their pathogenesis.
We conducted a prospective observational case series to investigate the relationship between full-thickness macular hole and RB/lattice degeneration.
Methods
This is a prospective observational case series study conducted according to the tenets of Declaration of Helsinki. All patients gave informed consent to being imaged and for the collected data to be used for publication. The Zhongshan Ophthalmic Center Ethics Committee did not require for this study to undergo Internal Review Board (IRB) approval as all the tests carried out were part of the routine care of patients.
This study included patients who were diagnosed as full-thickness macular hole and referred to Dr. Lin Lu from January 2009 to December 2013 at the Zhongshan Ophthalmic Center. Patients suffering from MH secondary to uveitis, trauma, and high myopia or associated with a simultaneous retinal detachment (RD) were excluded. Pseudophakic eyes were excluded. All the patients received a general ophthalmologic examination. The status of macular was confirmed by optical coherence tomography (OCT). Macular holes were graded using the Gass classification [2]. The fundus was carefully inspected by a three-minor Goldmann lens with a dilated pupil. The RB and/or lattice degeneration were recorded.
Numerical computations were performed using a spreadsheet package (Excel 2010; Microsoft, Redmond, WA). Statistical comparison of categorical findings was performed using the chi-square test. Statistical significance was set as P < 0.05.
Results
In all, 166 eyes of 151 patients fulfilled the inclusion and exclusion criteria. A total of 113 patients (74.83%) were women. The sex ratio of men to women was 1:3.36. And the 15 bilateral macular hole cases were all women. The mean age of patients at presentation was 65.14 ± 7.17 (range, 54 to 79) years. The mean age of men and women was no difference (66.13 ± 6.90 vs. 65.86 ± 7.36, p = 0.099).The mean duration of patients' symptoms was 12.66 ± 6.67(range, 2 to 24) months.
Mean spherical equivalent refractive error was -1.34 ± 1.52 (range, -4.00 to +1.50) diopters. The mean intraocular pressure was 14.62 ± 3.01 (range, 10 to 24)mmHg. Macular holes were most commonly graded as stage 3, followed by stage 4 and stage 2 (Table 1).
![]()
Table 1: Macular hole staging and anatomic outcome
View Table 1
RB and/or lattice degeneration were detected in 59 eyes (35.54%). Three of them had the history of prophylactic laser photocoagulation. The lattice degeneration seems to be more common than RB (Table 1). Most of the retinal breaks were atrophic holes and only one of them was horseshoe-shaped tear. The prevalence of RB and/or lattice degeneration was similar (p = 0.561 > 0.05) between men (12/38, 31.58%) and women (47/128, 36.72%). All of the RB/lattice degeneration was located near or anterior to the equator. The inferior quadrants and the vertical meridian were affected more often than the superior quadrants and the horizontal meridian (Figure 1).
.
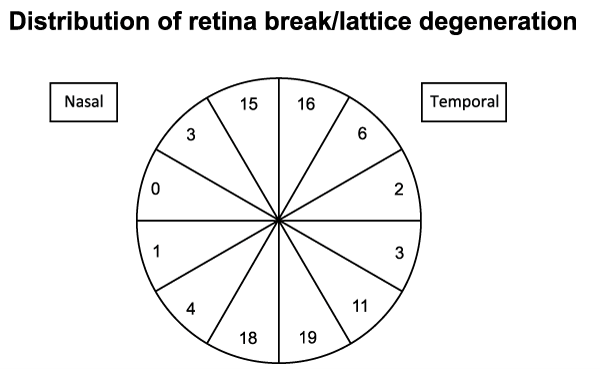
Figure 1: Relative distribution of retina break/lattice degeneration.
This figure showed the relative distribution of retinal break/lattice degeneration. The lesions were somewhat more prevalent in the inferior hemisphere (56/98, 57.14%). The vertical meridian was affected more often than the horizontal meridian (68 vs. 6).
View Figure 1
Discussion
No previous study on the relationship between retinal breaks/lattice degeneration and macular hole has been reported. Few studies mentioned it indirectly and had a few limitations. Guillaubey et al. [3] retrospectively analyzed 272 idiopathic macular hole surgery cases. Only the cases of retinal breaks were recorded and the lattice degenerations were not included. No RD occurred in patients presenting with an intraoperative (14 eyes) or preoperative (21 eyes) successfully treated RB. They didn't mention the RB found during the procedure was iatrogenic or not. If the retinal breaks found during the procedure were already exist, the RB rate (12.87%) in their cases is similar with ours cases (21/166 = 12.65%). In another study by Hwang et al. [4], 235 macular hole surgery cases were reviewed. Only 8 eyes (3.40%) preexisted retinal break and/or lattice degeneration before the surgery received intraoperative endolaser photocoagulation. They only concerned about the cases which had been treated during the operation and didn't present the status before the surgery. That's why the RB and/or lattice degeneration rate seems so low in their series.
The prevalence of lattice degeneration of the retina ranges from 6% to 10.7% in the general populations. [5-7]. In the fellow eye of patients with retinal detachment the prevalence is estimated to be 35% [8]. This study identified that retinal breaks and/or lattice degeneration were involved in almost one third of the full-thickness macular hole cases. It revealed macular hole and RB/lattice degeneration might have some pathogenic relationship.
Generally the attachment of the vitreous to the retina is greatest at those sites where the ILM of the retina is the thinnest. These sites include the vitreous base, the major retinal vessels, the optic nerve head, the 1500μm-diameter rim surrounding the fovea, and the 500μm-diameter foveolar. Forces generated by movement of the vitreous and the premacular bursa as the eye moves may also play a role in the pathogenesis of posterior vitreous detachment, macular hole and retinal breaks [9]. This theory might explain why the retinal break and/or lattice degenerations found in our cases were located near or anterior to the equator. The RB/lattice degeneration was involved in the inferior temporal quadrant most often in our cases. 69.39% of the lesions were found between the clock hours of 11 to 1 above, or between 5 and 7 below. These findings are similar to previously reported outcomes [5-7]. The movement of the eyeball contributes to distribution of the lesions.
In conclusion, the prevalence of RB/lattice degeneration is high in full-thickness macular hole. Preoperative and intraoperative detection and treatment of RB/lattice degeneration are critical.
References
-
Bainbridge J, Herbert E, Gregor Z (2008) Macular holes: vitreoretinal relationships and surgical approaches. Eye (Lond) 22: 1301-1309.
-
Gass JD (1995) Reappraisal of biomicroscopic classification of stages of development of a macular hole. Am J Ophthalmol 119: 752-759.
-
Guillaubey A, Malvitte L, Lafontaine PO, Hubert I, Bron A, et al. (2007) Incidence of retinal detachment after macular surgery: a retrospective study of 634 cases. Br J Ophthalmol 91: 1327-1330.
-
Hwang J, Escariao P, Iranmanesh R, Tosi GM, Chang S (2007) Outcomes of macular hole surgery in patients treated intraoperatively for retinal breaks and/or lattice degeneration. Retina 27: 1243-1248.
-
Straatsma BR, Zeegen PD, Foos RY, Feman SS, Shabo AL (1974) XXX Edward Jackson Memorial Lecture. Lattice degeneration of the retina. Trans Am Acad Ophthalmol Otolaryngol 78: OP87-113.
-
Byer NE (1965) Clinical study of lattice degeneration of the retina. Trans Am Acad Ophthalmol Otolaryngol 69: 1065-1081.
-
Byer NE (1979) Lattice degeneration of the retina. Surv Ophthalmol 23: 213-248.
-
Madjarov B, Hilton GF, Brinton DA, Lee SS (1995) A new classification of the retinoschises. Retina 15: 282-285.
-
Agarwal A (2012) Gass' Atlas of Macular Diseases. (5th edn). Collingwood: Saunders.





