International Journal of Ophthalmology and Clinical Research
Systemic Lupus Erythematosus Presenting as Acute Posterior Multifocal Placoid Pigment Epitheliopathy - Case Report and Review of the Ocular Manifestations of Systemic Lupus Erythematosus
Stephanie Chan1* and Chloe C. Gottlieb2
1University of Ottawa Eye Institute, Ottawa, Ontario, Canada
2University of Ottawa Eye Institute and, Ottawa Hospital Research Institute, Ottawa, Ontario, Canada
*Corresponding author: Stephanie Chan, University of Ottawa - The Ottawa Hospital, 501 Smyth Rd, Ottawa, ON, K1H 8L6, Canada, E-mail: stchan@toh.on.ca
Int J Ophthalmol Clin Res, IJOCR-2-035, (Volume 2, Issue 5), Case Report; ISSN: 2378-346X
Received: June 25, 2015 | Accepted: September 08, 2015 | Published: September 11, 2015
Citation: Chan S, Gottlieb CC (2015) Systemic Lupus Erythematosus Presenting as Acute Posterior Multifocal Placoid Pigment Epitheliopathy - Case Report and Review of the Ocular Manifestations of Systemic Lupus Erythematosus. Int J Ophthalmol Clin Res 2:038. 10.23937/2378-346X/1410038
Copyright: © 2015 Chan S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The ocular manifestations of systemic lupus erythematosus (SLE) are numerous and may be due to complement-activating immune complex deposition causing inflammation or thrombosis, secondary effects of SLE such as hypertension, related diseases such as Sjogren's and Antiphospholipid antibody syndrome, or a combination of these.
Left untreated, these manifestations can result in serious morbidity and rarely, mortality. Here we present the first reported case of systemic lupus erythematosus masquerading as Acute Posterior Multifocal Placoid Pigment Epitheliopathy, a rare chorioretinal disorder. An overview of the numerous ocular manifestations of this disease are presented, as well as recent highlights into the pathophysiology of SLE.
Case Report
Acute posterior multifocal placoid pigment epitheliopathy (APMPPE) is a rare disease affecting males and females equally in their second to third decade of life. It is thought to be due to an immune driven vascular alteration of the choriocapillaris with a secondary pigment epithelial reaction. More than half are associated with a viral etiology, and up to one-third will have a viral prodrome. Systemic autoimmune diseases such as erythema nodosum, granulomatosis with polyangiitis (GPA), polyarteritis nodosa (PAN), as well as other inflammatory diseases such as cerebral vasculitis, microvascular nephropathy, scleritis and episcleritis are associated with APMPPE [1,2].
A 35 year-old Caucasian female with a known history of systemic lupus erythematosus presented with a two week history of decreased vision and headaches. She had been previously well with no symptoms of infection. Her visual acuity at presentation was 20/500 right eye and 20/30 left eye, with intraocular pressures of 12 mmHg in both eyes and no afferent pupillary defect. Diffuse anterior scleritis of the right eye was noted following instillation of phenylephrine 10%. Funduscopy revealed bilateral confluent, deep, cream-colored chorioretinal lesions of varying sizes with indistinct borders located mostly between the arcades (Figure 1). There were 0.5+ cells in the vitreous in both eyes and no haze. Fluorescein angiography showed early hypofluoresence (Figure 2) and late hyperfluorescence (Figure 3) of the lesions. Optic nerve edema was noted on the clinical examination and confirmed with fluorescein angiography, which showed early hyperfluorescence and late staining of the optic nerve (Figures 2 and Figure 3). In the late frames, there was significant background hyperfluorescence and vascular flushing with extravasation of dye (Figure 3). The clinical features and angiography appeared consistent with a diagnosis of APMPPE.
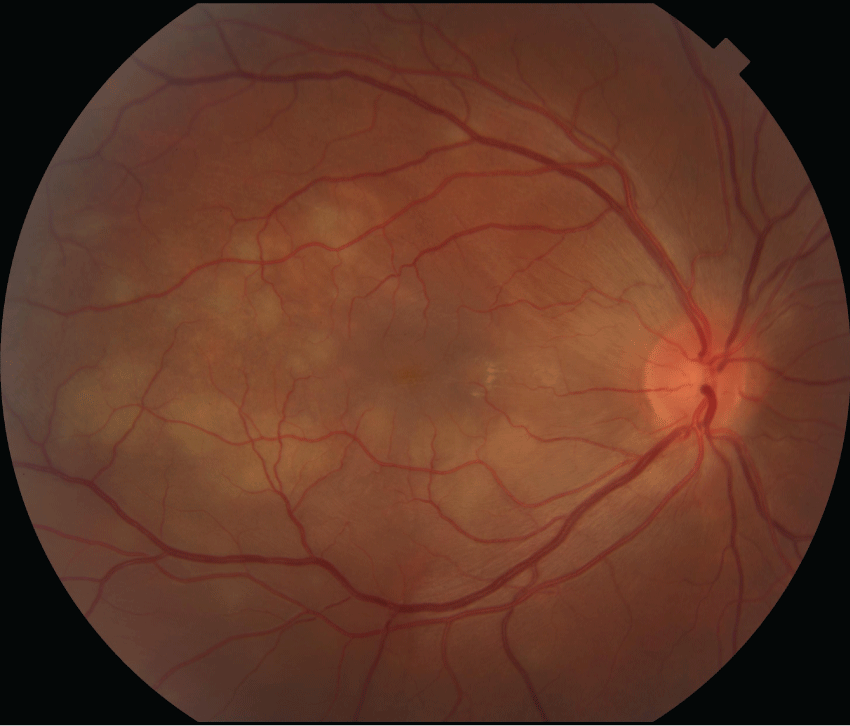
.
Figure 1: Color photograph of the right eye showing deep chorioretinal lesions of varying sizes becoming confluent, located mostly between the arcades, as well as disc edema.
View Figure 1
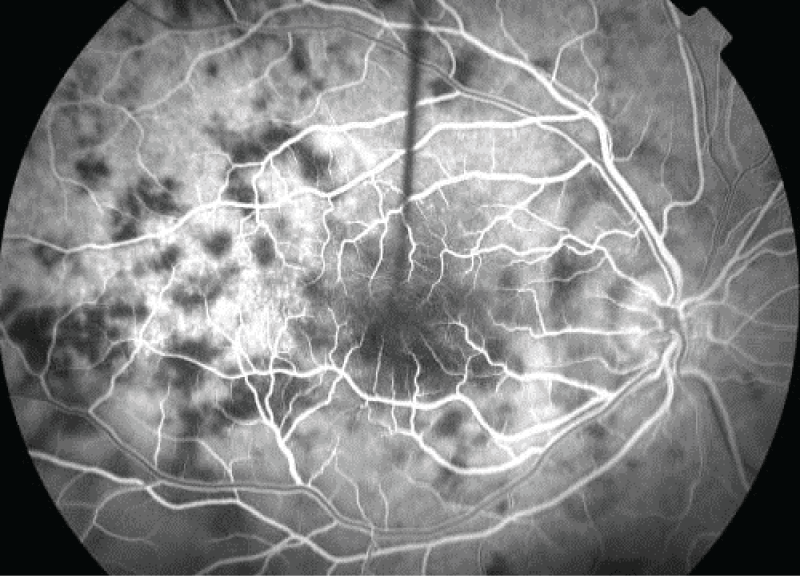
.
Figure 2: A fluorescein angiogram of the right eye showing early hypofluoresence of the lesions.
View Figure 2
However, there were atypical features including profuse vascular leakage and punctate hyperfluorescence in the temporal macula and around the optic nerve. As well, the fluorescein pooling was not typical of APMPPE. A macular OCT showed subretinal fluid (Figure 4). These characteristics, along with the anterior scleritis at presentation, pointed to a possible diagnosis of posterior scleritis.
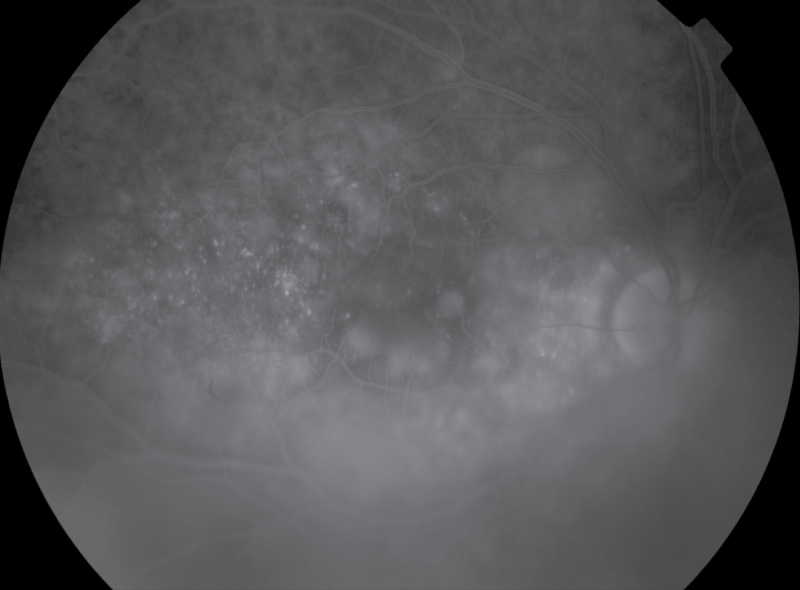
.
Figure 3: A fluorescein angiogram of the right eye showing late hyperfluorescence of the lesions, as well as was significant background hyperfluorescence with vascular flushing and optic nerve staining. Pinpoint areas of leakage in the temporal macula are consistent with posterior scleritis rather than APMPPE.
View Figure 3
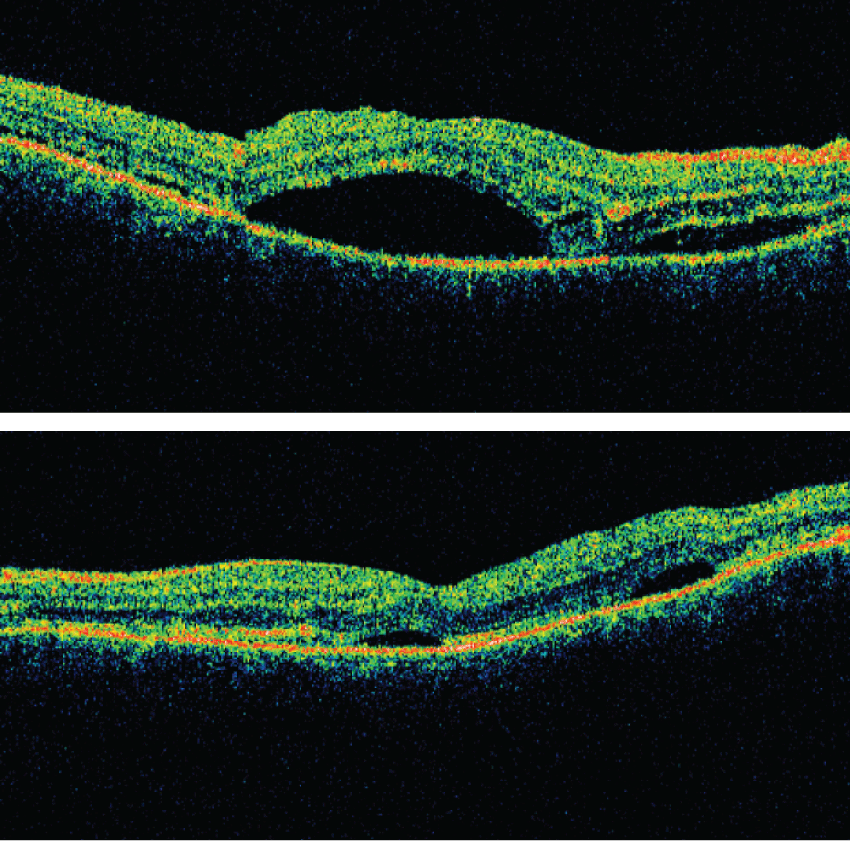
.
Figure 4: Macular OCT showing subretinal fluid in the right eye (Top) and left eye (bottom).
View Figure 4
A blood work panel was significant for an ANA of 2560, and further testing was negative for syphilis, Lyme disease and tuberculosis. An MRI/MRV/MRA of the brain did not reveal vasculitis or any other abnormality. Rapid resolution and visual improvement occurred with oral prednisone therapy
Literature Review
Systemic lupus erythematosus (SLE) is a chronic autoimmune disease that preferentially affects women in their childbearing years. African Americans, Hispanics and Asians are at greater risk of developing SLE [3].
While the diagnostic criteria for SLE by the American College of Rheumatology from 1997 are still being used, the Systemic Lupus International Collaborating Clinics (SLICC) group recently revised the criteria in 2012 to now include seventeen clinical or laboratory criteria. Diagnosis requires at least 4 criteria, including at least one clinical criterion and one immunologic criterion, or a positive biopsy-proven lupus nephritis in the presence of antinuclear antibodies or anti-double-stranded DNA antibodies [4]. Patients can also be classified as "probable SLE patients" if they do not fulfill the classification criteria, or for those with other SLE manifestations not included in the classification criteria. The revised criteria are as follows:
• Clinical criteria
1. Acute cutaneous lupus, including: lupus malar rash, bullous lupus, toxic epidermal necrolysis variant of SLE, maculopapular lupus rash, photosensitive lupus rash (in the absence of dermatomyositis), or subacute cutaneous lupus.
2. Chronic cutaneous lupus, including: classic discoid rash, hypertrophic (verrucous) lupus, lupus panniculitis (profundus), mucosal lupus, lupus erythematosus tumidus, chillblains lupus and discoid lupus/lichen planus overlap.
3. Oral ulcers or nasal ulcers in the absence of other causes such as vasculitis, Behcet's disease, infection (herpesvirus), inflammatory bowel disease, reactive arthritis, and acidic foods.
4. Nonscarring alopecia in the absence of other causes such as alopecia areata, drugs, iron deficiency, and androgenic alopecia.
5. Synovitis involving 2 or more joints, characterized by swelling or effusion or tenderness in 2 or more joints and at least 30 minutes of morning stiffness.
6. Serositis
7. Renal: Urine protein-to-creatinine ratio (or 24-hour urine protein) representing 500 mg protein/24 hours OR red blood cell casts
8. Neurologic: seizures, psychosis, mononeuritis multiplex (in the absence of other known causes such as primary vasculitis), myelitis, peripheral or cranial neuropathy (in the absence of other known causes such as primary vasculitis, infection, and diabetes mellitus), acute confusional state (in the absence of other causes including toxic/metabolic, uremia, drugs).
9. Hemolytic anemia
10. Leukopenia (< 4,000/mm3 at least once) (in the absence of other known causes such as Felty's syndrome, drugs, and portal hypertension), OR lymphopenia (< 1,000/mm3 at least once) (in the absence of other known causes such as corticosteroids, drugs, and infection).
11. Thrombocytopenia (100,000/mm3) at least once in the absence of other known causes such as drugs, portal hypertension, and thrombotic thrombocytopenic purpura
• Immunologic criteria
1. ANA level above laboratory reference range
2. Anti-dsDNA antibody level above laboratory reference range (or 2-fold the reference range if tested by ELISA)
3. Anti-Sm: presence of antibody to Sm nuclear antigen
4. Antiphospholipid antibody positivity as determined by any of the following: positive test result for lupus anticoagulant, false-positive test result for rapid plasma regain, medium- or high-titer anticardiolipin antibody level (IgA, IgG, or IgM), positive test result for anti-2-glycoprotein I (IgA, IgG, or IgM)
5. Low complement: Low C3, Low C4, Low CH50
6. Direct Coombs' test in the absence of hemolytic anemia
The ocular manifestations of SLE are numerous and diverse. The pathophysiology of ocular manifestations of SLE are also varied and somewhat controversial. They may be due to complement-activating immune complex deposition causing inflammation or thrombosis, secondary effects of SLE such as hypertension, related diseases such as Sjogren's and Antiphospholipid antibody syndrome, or a combination of these [5-9].
The ocular manifestations of SLE can be the initial presentation and if misdiagnosed or left untreated, can result in serious morbidity and even mortality. Therefore, prompt diagnosis and treatment is required.
Pathogenesis
Immune-complex deposits have been demonstrated in vessels in the conjunctiva, sclera, retina and choroid of patients with SLE [6,10-13]. One study found that patients with significant immune reactants, most commonly IgG, also had significant disease activity [6]. It is thought that these immune-complex deposits activate the complement pathway which produce C3 and C5, proteins also found in ocular tissue of patients with SLE [12]. These proteins then attract inflammatory cells, resulting in the release of pro-inflammatory cytokines and tissue-damaging enzymes [14]. Histopathological studies of choroidal vessels show necrosis and extravasation of fibrinoid material in the choroid, supporting the theory of a vasculitis secondary to immune-complex deposition [10,11].
These immune-complex deposits may alternatively cause a thrombotic reaction via interactions with platelet and endothelial cell surfaces [6,10,15].
However, the evidence for these two mechanisms is conflicting. One immunopathologic study of active inflamed conjunctiva of SLE patients showed several immune-complex deposits in conjunctival epithelium, stroma and vessel walls including IgA, IgD, IgG, IgM and C4. In this study, the finding of immune-complex deposits at the basement membrane zone was related to the clinical appearance of cicatrizing conjunctivitis. However, there was no evidence of vasculitis or thrombosis [13]. Another older study also failed to show evidence of necrosis and vasculitis in retinal vessels [16].
Interestingly, one study examining the presence of immune-complexes in various biopsy specimens of patients with SLE found that while the conjunctiva had a greater number of antibodies compared to the skin or other mucous membrane, this did not necessarily translate to active disease as many patients were asymptomatic [17].
Recent studies have also pointed to the role of abnormal differentiation of T-helper cells, specifically the role of the proinflammatory Th17 cell in the pathogenesis of SLE [18-20]. The combination of TGF-β and IL-6 leads to differentiation of Th17 cells, which in turn produce IL-17. IL-21 and IL-23 also contribute to the stabilization and proliferation of these cells [21].
The ocular surface provides all of these cytokines and when exposed to inflammatory stimuli or dessicating stress, these cytokines are further up regulated resulting in a vicious cycle [22].
Elevated tear IL-17 levels were found to have a direct correlation with clinical severity of ocular surface disease in patients with systemic inflammatory disease, including SLE. Interestingly, this correlation was not found in patients with ocular surface disease with no systemic inflammatory disease [23].
Related diseases such as antiphospholipid antibody syndrome can also cause thrombosis of ocular vessels, resulting in serious irreversible visual loss. Antiphospholipid antibody has been recognized as a risk factor for severe occlusive SLE retinopathy, and its presence signifies an overall poorer prognosis [7,24,25] .
Orbital Manifestations
SLE can involve the lids and periorbital area. It is more frequent in the discoid lupus erythematosus (DLE) variant and has been well-described in the literature. Presentations include eyelid edema, periorbital edema, plaque-like lesions, erythematous papules, ulcers, telangiectasias, cicatricial changes and madarosis [17,26-64].
The lower lid is most commonly involved and can clinically be mistaken for eczema, blepharitis, squamous cell carcinoma or basal cell carcinoma [26]. As well, squamous cell carcinoma and DLE share many histopathological features including cytologic atypia and infiltrative patterns of squamous proliferation [26,65]. The key features that distinguish DLE from squamous cell carcinoma are perifollicular or periacrosyringeal inflammation, vacuolar basal cell degeneration, and dermal mucin deposition [26,66].
Systemic antimalarial drugs were successfully used to treat these lesions [28,30]. For patients who failed antimalarial drugs, intralesional steroids or thalidomide were found to be beneficial [44,53,63].
Many of the cases described had a delay in diagnosis of up to 25 years, and surgical revision of cicatricial changes such as ectropion and trichiasis were required [61,63,67]. These cases highlight the importance of a biopsy in refractory or unusual periocular skin disease.
Another manifestation of SLE is panniculitis, usually presenting as firm, large subcutaneous nodules on the face and arm [68]. It can rarely affect the orbit, and include symptoms such as lid swelling, proptosis and limited extraocular movements [51,69-73]. Many of these patients improved with antimalarials, but one case resulted in severe orbital melting despite therapy [51,69].
Trochleitis, which presents with swelling and pain in the superonasal orbit that is worse with eye movements, has also been reported as an initial manifestation of SLE. In this particular case, the patient had poor response to conventional treatment consisting of corticosteroid injections, and only experienced relief of symptoms with systemic treatment [74].
Additional orbital manifestations of SLE include orbital myositis, dacryoadenitis and Tolosa-Hunt Syndrome, characterized by painful ophthalmoplegia due to inflammation of the cavernous sinus or superior orbital fissure. These patients improved on systemic corticosteroids [75-79].
Corneal Manifestations
Kerato conjunctivitis sicca (KCS) is the most common ocular manifestation of SLE. Symptoms include a foreign body sensation, pain, irritation and burning, and can affect up to 60% of patients with SLE [80,81].
Approximately 17.8% of patients with SLE also suffer from Sjogren's syndrome, a chronic autoimmune disorder of the exocrine glands characterized by lymphocytic infiltrates of the affected glands [8,82-84].
Patients with this combination are generally older with more mucosal or arthritic involvement, and less major internal organ involvement than patients with SLE alone. These patients also have a higher prevalence of anti-SSA, anti-SSB and anti-dsDNA antibodies, as well as an increased prevalence of DRB1*0301 [8,82]. These findings indicate that the combination of SLE and Sjogren's may be a separate systemic autoimmune entity with a more favorable prognosis [8,82,83].
Treatment for dry eye symptoms is often chronic and long-term, and can range from the use of artificial tears, oral fatty acids and punctal occlusion, to the use of topical cyclosporine A [85]. One study showed that in vivo blockade of IL-17 in a mouse model significantly reduced the number of Th17 cells, as well as the severity and progression of dry eye [86]. Drugs that target this pathway may play a role in future management of keratoconjunctivitis sicca.
Rare cases of peripheral ulcerative keratitis, corneal stromal keratitis and keratoendotheliitis have been reported. They were all generally responsive to corticosteroids and control of the systemic disease [13,87-92].
Refractive surgery is considered a relative contraindicated in patients with SLE or other autoimmune diseases due to reports of adverse complications such as corneal haze and stromal melting [93-95]. Two retrospective studies of refractive surgery performed on patients with well-controlled autoimmune systemic disease, including SLE, reported no adverse effects to the cornea [96,97]. In one study of 49 eyes of 26 patients, there were no reports of corneal haze, melting, flap, or interface complications at a mean follow-up time of 19 months [96]. A second study of 42 eyes of 22 patients also found the same result, with a minimum follow-up time of 6 months [96,97]. Despite this, long-term studies are lacking. As well, cases of patients with inactive autoimmune disease suffering from post-operative necrotizing keratitis after undergoing laser eye surgery have been reported in the literature [95].
Conjunctiva and Sclera
SLE can manifest as a chronic blepharoconjunctivitis, cicatrizing conjunctivitis, epibulbar mass, episcleritis and scleritis [13,17,30,44,98-101].
Reported cases of conjunctivitis often had a delay in diagnosis, and similarly to patients with lid manifestations, suffered serious sequelae including symblepharon [17]. These manifestations can also be isolated, as evidenced by a report describing a unilateral, chronic, isolated discoid lupus erythematosus of the conjunctiva [102]. Biopsies were essential in establishing the diagnosis, and in patients with refractory conjunctivitis, are strongly encouraged.
Episcleritis is a generally benign disease that presents with ocular redness without symptoms such as pain or irritation. In some patients with SLE-related episcleritis, the episcleritis can flare along with systemic flares. SLE-related episcleritis can be recurrent or chronic, but will resolve with systemic treatment [17].
Scleritis can be categorized into five categories: diffuse anterior scleritis, nodular anterior scleritis, necrotizing scleritis with inflammation, necrotizing scleritis without inflammation, and posterior scleritis. SLE has been associated with each of these [13,98,103,104]. Symptoms include blurred vision and eye pain. If there is involvement of the anterior sclera, the scleral vessels will be inflamed and patients will present with a red eye. A case of angle-closure glaucoma secondary to posterior scleritis has also been described [105].
Compared to other autoimmune diseases such as granulomatosis with polyangiitis, SLE-related scleritis was found to have a much lower incidence of necrotizing scleritis, and therefore a better prognosis [104]. SLE patients who do present with necrotizing scleritis were found to have significant renal and systemic manifestations [106].
Unlike episcleritis, the course of scleritis can be severe with significant visual loss if left untreated. While patients with idiopathic scleritis may respond well to oral non-steroidal anti-inflammatory drugs, patients with concurrent systemic disease often require systemic immunosuppression including systemic corticosteroids, methotrexate, TNF-inhibitors or cyclophosphamide. The prognosis is good with prompt therapy [98,103,104,106].
Uvea and Retina
The reported prevalence of SLE in patients with uveitis varies from 0.1% to 4.8% [107-111]. One retrospective study found that SLE accounted for 3.3% of anterior uveitis, 7.9% of posterior uveitis cases, and 9.1% of panuveitis cases [108]. In another prospective study examining patients with anterior uveitis, SLE was found to affect only 1.2% [109]. It is important to note that these numbers are inherently biased as the cohorts analyzed represented patients specifically referred to a tertiary care center for further management, and did not include patients seen by primary care eye providers.
Anterior uveitic manifestations of SLE present as pain, eye redness, photophobia and blurred vision. They can be bilateral and severe, and can at times include hypopyon [109,111,112].
SLE retinopathy was previously reported to affect up to 28% of patients [113], but more recent studies show a rate closer to 10-15% [114-116]. Findings are similar to vascular diseases such as diabetic retinopathy and hypertensive retinopathy, but with a better visual prognosis [114]. Signs include microaneurysms, hemorrhages, hard exudates, retinal edema, retinal ischemia and cotton-wool spots [15,117].
Immune-complexes have been well documented in retinal vessels, supporting the hypothesis that SLE retinopathy is primarily due to an inflammatory mechanism [13,16,118]. As well, SLE retinopathy appears to improve with systemic immunosuppression [5]. However, one study suggested that accelerated atherosclerosis due to the combination of hypertension, corticosteroid use and dyslipidemia in SLE may also play a role in SLE retinopathy [5].
Despite the excellent visual prognosis and generally asymptomatic nature, SLE retinopathy has been associated both with disease activity, and a decreased survival rate [114-116,119,120]. One study found that patients with SLE retinopathy had higher levels of serum creatinine, higher disease activity as measured by the SLE Disease Activity Index (SLEDAI), and a higher incidence of CNS lupus as compared to SLE patients without retinopathy [116].
SLE retinopathy can also present as a more rare, severe vaso-occlusive variant. Contrary to the more favorable prognosis of SLE retinopathy, this variant can result in severe and permanent visual loss from ischemia, neovascularization causing a vitreous hemorrhage or tractional retinal detachment [7]. Presentations include a Purtscher-like retinopathy, central retinal artery occlusions, cilioretinal artery occlusions, retinal vein occlusions, or combinations of these [7,121-130]. One study found that SLE was considered an independent risk factor for the development of vein occlusions, with a reported 3.46 times higher incidence than in controls [131]. The prognosis for these patients depends on the amount of retinal ischemia, but is generally poor [121-126,130].
CNS lupus appears to have a strong association with severe occlusive retinopathy, with one study finding the incidence to be more than 50% [7].
Additional retinal presentations, in addition to our patient with pseudo-APMPPE, include an exudative macular edema with frosted branch periphelbitis similar to CMV retinitis [132], and pseudoretinitis pigmentosa-like picture with bilateral retinal pigment epithelium changes [133]. These patients resolved markedly on corticosteroids.
Treatment is focused mainly on treatment of the systemic disease and includes systemic corticosteroids and immune-modulating therapy [134]. Patients who present with vein occlusions or severe vaso-occlusive disease should undergo screening for antiphospholipid antibody syndrome [24,135,136]. In patients with antiphospholipid antibody syndrome and concurrent SLE, there is often a role for systemic anticoagulation both in preventing further thrombotic events, which can happen in as little as one week, and in possibly treating the retinal occlusions and improving vision [92,121,123,135].
For cases of retinal neovascularization due to ischemia, treatments such as laser and surgery may be warranted, though they are not always successful in regaining or maintaining vision [7].
Lupus choroidopathy is a rare entity characterized by macular serous detachment, RPE detachments and RPE changes, and exudative retinal detachments which can be large and bullous [137,138].
One report detailing the indocyanine green angiography findings of lupus choroidopathy found that there were four main findings: focal, transient hypofluorescent areas in the very early phase indicating a choroidal filling delay, fuzziness of large choroidal vessels with late diffuse zonal choroidal hyperfluorescence indicationg choroidal vascular leakage; poorly-defined areas of choroidal hypofluorescence visible up to the late phase indicating vascular obstruction; and focal cluster of pinpoint spots of choroidal hyperfluorescence visible from the intermediate to late phase. The first three are nonspecific and can be found in many other choroidal diseases, but the finding of focal pinpoint spots of hyperfluorescence in the intermediate to late phase may represent immune deposits specific to lupus choroidopathy [139].
Lupus choroidopathy has a strong association with disease activity, with one study finding that 100% of cases of reported lupus choroidopathy had evidence of active systemic vascular disease, 64% had nephropathy and 36% had CNS lupus vasculitis [137].
Left untreated, permanent retinal pigment epithelial damage can result in permanent severe visual loss. For this reason, aggressive control of SLE with immunosuppressive therapy is the initial treatment [11]. While most patients will have good resolution of their symptoms, many patients will suffer from persistent areas of choroidal leakage despite adequate immunosuppression and inactive systemic disease. In these cases, plasmapharesis, focal laser and PDT and surgery have all been used successfully [11,137,140-142].
A rare case of punctate inner choroidopathy (PIC) was recently reported in a patient with SLE. On subsequent general exam, this patient was found to have renal impairment [143].
Neuro-ophthalmic Manifestations
Neuro-ophthalmic manifestations of SLE are uncommon, and a recent review estimated the prevalence to be 1.6% in children and 3.6% in adults [144].
Optic neuropathy caused by SLE is well-recognized in the literature and represents approximately 1% of SLE patients [145-150]. It can present as an optic neuritis with symptoms of decreased vision, dyschromatopsia, pain with extraocular movements or orbital pain, and scotoma [145]. It can further present as neuromyelitis optica, with optic neuritis that is often bilateral, and transverse myelitis [9,144]. Optic chiasmitis causing a junctional scotoma and ischemic optic neuropathy due to SLE have also been reported in the literature [144,151,152].
Optic neuropathy is generally associated with active disease and responds dramatically to corticosteroids, indicating an ischemic pathogenesis that in turn, causes demyelination [144]. Since recurrences can occur with corticosteroid taper, some authors advocate the use of concurrent immunosuppressives such as cyclophosphamide [146,153].
Eye movement restrictions causing diplopia have also been reported. Causes include cranial nerve palsies, internuclear ophthalmoplegia causing an ipsilateral adduction deficit, and Brown's syndrome where the superior oblique tendon becomes inflamed and restricted. Similarly to optic neuropathy, there is often dramatic improvement with systemic corticosteroids [154-164].
SLE-associated intracranial hypertension is characterized by headaches, blurry vision, and papilledema [165-168]. One study found abnormalities of the choroid plexus on MRI, which may indicate micro-occlusion of arachnoid villi [169,170]. In addition, many patients were found to have concurrent antiphospholipid antibody syndrome, and some suffered subsequent cerebral venous sinus thrombosis [171]. Almost all patients were found to have systemic active disease, and treatment mainly involved the use systemic corticosteroids with a slow taper due to the high rate of recurrence, plasmapharesis and immunomodulating therapy [168,170]. As well, treatment for the high intracranial pressure was also required and involved the use of acetazolamide, mannitol and in cases of sinus thrombosis, anticoagulation or surgical intervention [168,170].
Conclusion
The ocular manifesations of SLE are varied and numerous. This is the first reported case of SLE presenting as APMPPE. As with other ocular manifestations of SLE, the disease resolved markedly with corticosteroids. It is important to note that while the ocular manifestations of SLE are rare, they are often misdiagnosed. In addition, they can present as the initial manifestation, with systemic disease expressing itself years later. This highlights the importance of maintaining clinical suspicion and initiating appropriate investigations, including biopsies and serological analysis, in cases of ocular disease refractory to conventional treatment.
Treatment for these manifestations mainly consists of systemic immunosuppressive therapy. However, as the mechanism and pathophysiology of SLE continues to be elucidated, targeted therapy may play a greater role in its management.
References
-
Crawford CM, Igboeli O (2013) A review of the inflammatory chorioretinopathies: the white dot syndromes. ISRN Inflamm 2013: 783190.
-
Jones NP (1995) Acute posterior multifocal placoid pigment epitheliopathy. Br J Ophthalmol 79: 384-389.
-
Lisnevskaia L, Murphy G, Isenberg D (2014) Systemic lupus erythematosus. Lancet 384: 1878-1888.
-
Petri M, Orbai AM, Alarcón GS, Gordon C, Merrill JT, et al. (2012) Derivation and validation of the systemic lupus international collaborating clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum 64: 2677-2686.
-
Giorgi D, Pace F, Giorgi A, Bonomo L, Gabrieli CB (1999) Retinopathy in systemic lupus erythematosus: pathogenesis and approach to therapy. Hum Immunol 60: 688-696.
-
Karpik AG, Schwartz MM, Dickey LE, Streeten BW, Roberts JL (1985) Ocular immune reactants in patients dying with systemic lupus erythematosus. Clin Immunol Immunopathol 35: 295-312.
-
Au A, O'Day J (2004) Review of severe vaso-occlusive retinopathy in systemic lupus erythematosus and the antiphospholipid syndrome: Associations, visual outcomes, complications and treatment. Clin Experiment Ophthalmol 32: 87-100.
-
Yao Q, Altman RD, Wang X (2012) Systemic lupus erythematosus with Sjögren syndrome compared to systemic lupus erythematosus alone: a meta-analysis. J Clin Rheumatol 18: 28-32.
-
Giorgi D, Balacco Gabrieli C (1999) Optic neuropathy in systemic lupus erythematosus and antiphospholipid syndrome (APS): Clinical features, pathogenesis, review of the literature and proposed ophthalmological criteria for APS diagnosis. Clin Rheumatol 18: 124-131.
-
Schwartz MM, Roberts JL (1983) Membranous and vascular choroidopathy: two patterns of immune deposits in systemic lupus erythematosus. Clin Immunol Immunopathol 29: 369-380.
-
Hannouche D, Korobelnik JF, Cochereau I, Hayem G, Beaudreuil J, et al. (1995) Systemic lupus erythematosus with choroidopathy and serous retinal detachment. Int Ophthalmol 19: 125-127.
-
Aronson AJ, Ordoñez NG, Diddie KR, Ernest JT (1979) Immune-complex deposition in the eye in systemic lupus erythematosus. Arch Intern Med 139: 1312-1313.
-
Heiligenhaus A, Dutt JE, Foster CS (1996) Histology and immunopathology of systemic lupus erythematosus affecting the conjunctiva. Eye (Lond) 10 : 425-432.
-
Read RW (2004) Clinical mini-review: systemic lupus erythematosus and the eye. Ocul Immunol Inflamm 12: 87-99.
-
Nag TC, Wadhwa S (2006) Vascular changes of the retina and choroid in systemic lupus erythematosus: pathology and pathogenesis. Curr Neurovasc Res 3: 159-168.
-
Graham EM, Spalton DJ, Barnard RO, Garner A, Russell RW (1985) Cerebral and retinal vascular changes in systemic lupus erythematosus. Ophthalmology 92: 444-448.
-
Frith P, Burge SM, Millard PR, Wojnarowska F (1990) External ocular findings in lupus erythematosus: a clinical and immunopathological study. Br J Ophthalmol 74: 163-167.
-
Amarilyo G, Lourenço EV, Shi FD, La Cava A (2014) IL-17 promotes murine lupus. J Immunol 193: 540-543.
-
Wang HX, Chu S, Li J, Lai WN, Wang HX, et al. (2014) Increased IL-17 and IL-21 producing TCRαβ+CD4-CD8- T cells in Chinese systemic lupus erythematosus patients. Lupus 23: 643-654.
-
Crispín JC, Oukka M, Bayliss G, Cohen RA, Van Beek CA, et al. (2008) Expanded double negative T cells in patients with systemic lupus erythematosus produce IL-17 and infiltrate the kidneys. J Immunol 181: 8761-8766.
-
Wahren-Herlenius M, Dörner T (2013) Immunopathogenic mechanisms of systemic autoimmune disease. Lancet 382: 819-831.
-
De Paiva CS, Chotikavanich S, Pangelinan SB, Pitcher JD 3rd, Fang B, et al. (2009) IL-17 disrupts corneal barrier following desiccating stress. Mucosal Immunol 2: 243-253.
-
Kang MH, Kim MK, Lee HJ, Lee HI, Wee WR, et al. (2011) Interleukin-17 in various ocular surface inflammatory diseases. J Korean Med Sci 26: 938-944.
-
Asherson RA, Merry P, Acheson JF, Harris EN, Hughes GR (1989) Antiphospholipid antibodies: a risk factor for occlusive ocular vascular disease in systemic lupus erythematosus and the 'primary' antiphospholipid syndrome. Ann Rheum Dis 48: 358-361.
-
Montehermoso A, Cervera R, Font J, Ramos-Casals M, García-carrasco M, et al. (1999) Association of antiphospholipid antibodies with retinal vascular disease in systemic lupus erythematosus. Semin Arthritis Rheum 28: 326-332.
-
Papalas JA, Hitchcock MG, Gandhi P, Proia AD (2011) Cutaneous lupus erythematosus of the eyelid as a mimic of squamous epithelial malignancies: A clinicopathologic study of 9 cases. Ophthal Plast Reconstr Surg 27:168-172.
-
Trindade MA, Alchorne AO, da Costa EB, Enokihara MM (2004) Eyelid discoid lupus erythematosus and contact dermatitis: a case report. J Eur Acad Dermatol Venereol 18: 577-579.
-
Tosti A, Tosti G, Giovannini A (1987) Discoid lupus erythematosus solely involving the eyelids: report of three cases. J Am Acad Dermatol 16: 1259-1260.
-
Pandhi D, Singal A, Rohtagi J (2006) Eyelid involvement in disseminated chronic cutaneous lupus erythematosus. Indian J Dermatol Venereol Leprol 72: 370-372.
-
Acharya N, Pineda R,2nd, Uy HS, Foster CS (2005) Discoid lupus erythematosus masquerading as chronic blepharoconjunctivitis. Ophthalmology 112: 19-23.
-
Anderson HF, Musgrave DP (1949) Lupus erythematosus of the conjunctiva and lid margin; report of a case. Arch Derm Syphilol 59: 247.
-
Bettis VM, Vaughn RY, Guill MA (1993) Erythematous plaques on the eyelids. Discoid lupus erythematosus (DLE). Arch Dermatol 129: 497, 500.
-
Braun RP, French LE, Massouyé I, Saurat JH (2002) Periorbital oedema and erythema as a manifestation of discoid lupus erythematosus. Dermatology 205: 194-197.
-
Cyran S, Douglass MC, Silverstein JL (1992) Chronic cutaneous lupus erythematosus presenting as periorbital edema and erythema. J Am Acad Dermatol 26: 334-338.
-
Dai YS, Chiu HC (2000) Periorbital heliotrope oedema as the only initial clinical manifestation of systemic lupus erythematosus in a primigravida. Br J Dermatol 143: 679-680.
-
Dimoski N, Dimoski A (1985) Chronic discoid lupus erythematosus of the eyelids. Med Pregl 38: 551-552.
-
Donzis PB, Insler MS, Buntin DM, Gately LE (1984) Discoid lupus erythematosus involving the eyelids. Am J Ophthalmol 98: 32-36.
-
Ena P, Pinna A, Carta F (2006) Discoid lupus erythematosus of the eyelids associated with staphylococcal blepharitis and Meibomian gland dysfunction. Clin Exp Dermatol 31: 77-79.
-
Feiler-Ofry V, Isler Z, Hanau D, Godel V (1979) Eyelid involvement as the presenting manifestation of discoid lupus erythematosus. J Pediatr Ophthalmol Strabismus 16: 395-397.
-
Galeone M, Arunachalam M, Scarfì F, Palleschi GM, Massi D, et al. (2014) Unilateral eyelid involvement in discoid lupus erythematosus. Int J Dermatol 53: 894-896.
-
Giménez-García R, Sánchez-Ramón S, De Andrés A (2005) Discoid lupus erythematosus involving the eyelids. J Eur Acad Dermatol Venereol 19: 138-139.
-
Gloor P, Kim M, McNiff JM, Wolfley D (1997) Discoid lupus erythematosus presenting as asymmetric posterior blepharitis. Am J Ophthalmol 124: 707-709.
-
Gunasekera V, Jayaram H, Kashani S, Toma NM, Olver JM (2008) Refractory discoid lupus erythematosis of the eyelid successfully treated with intra-lesional triamcinolone. Eye (Lond) 22: 1205-1206.
-
Gupta T, Beaconsfield M, Rose GE, Verity DH (2012) Discoid lupus erythematosus of the periorbita: clinical dilemmas, diagnostic delays. Eye (Lond) 26: 609-612.
-
Koga M, Kubota Y, Kiryu H, Nakayama J (2006) A case of discoid lupus erythematosus of the eyelid. J Dermatol 33: 368-371.
-
Kormann RB, Cunha E, Silva AT, Beckhauser AP, Werner B (2009) [Discoid lupus on the eyelids: case report]. Arq Bras Oftalmol 72: 549-551.
-
Lee CW, Sung YK, Bae SC (2005) An unusual form of cutaneous lupus erythematosus over the eyelid in systemic lupus erythematosus. Lupus 14: 564-565.
-
Maeguchi M, Nogita T, Ishiguro N, Nihei H, Kawashima M (1996) Periorbital oedema and erythema in systemic lupus erythematosus. Br J Dermatol 134: 601-602.
-
Meiusi RS, Cameron JD, Holland EJ, Summers CG (1991) Discoid lupus erythematosus of the eyelid complicated by wound dehiscence. Am J Ophthalmol 111: 108-109.
-
Mseddi M, Marrekchi S, Meziou TJ, Sellami D, Kammoun B, et al. (2007) Discoid lupus erythematosus with eyelid involvement. A series of nine patients. J Fr Ophtalmol 30: 247-249.
-
Nowinski T, Bernardino V, Naidoff M, Parrish R (1982) Ocular involvement in lupus erythematosus profundus (panniculitis). Ophthalmology 89: 1149-1154.
-
Palic-Szantoo (1955) Primary isolated lupus erythematosus of the eyelid. Ophthalmologica 130: 186-191.
-
Panse I, Cordoliani F, Rybojad M, Rivet J, Lebbé C, et al. (2004) Discoid lupus erythematosus involving the eyelids: 4 cases. Ann Dermatol Venereol 131: 58-60.
-
Pianigiani E, Andreassi A, De Aloe G, Rubegni P, Rufa A, et al. (2002) Chronic erythematous desquamative plaques of the eyelids: discoid lupus erythematosis (DLE). Arch Dermatol 138: 527-532.
-
Paroli MP, Riso D, Pinca M, Pivetti-Pezzi P (2001) Chorioretinopathy and discoid plaque-like lesions of the eyelids as useful indicators of systemic lupus erythematosus (SLE) progression. Lupus 10: 571-575.
-
Ricotti C, Tozman E, Fernandez A, Nousari CH (2008) Unilateral eyelid discoid lupus erythematosus. Am J Dermatopathol 30: 512-513.
-
Selva D, Chen CS, James CL, Huilgol SC (2003) Discoid lupus erythematosus presenting as madarosis. Am J Ophthalmol 136: 545-546.
-
Sheehan-Dare RA, Cunliffe WJ (1988) Severe periorbital oedema in association with lupus erythematosus profundus. Clin Exp Dermatol 13: 406-407.
-
Tóth A, Nagy E, Varga M, Schneider I (1990) Discoid lupus erythematosus beginning on the eyelids. Z Hautkr 65: 589-591.
-
Vassallo C, Colombo G, Canevari R, Brazzelli V, Ardigò M, et al. (2005) Monolateral severe eyelid erythema and edema as unique manifestation of lupus tumidus. Int J Dermatol 44: 858-860.
-
Yaghoobi R, Feily A, Behrooz B, Yaghoobi E, Mokhtarzadeh S (2010) Palpebral involvement as a presenting and sole manifestation of discoid lupus erythematosus. ScientificWorldJournal 10: 2130-2131.
-
Vukicevic JS, Milobratovic DJ (2010) Discoid lupus erythematosus of the eyelid. Indian J Dermatol Venereol Leprol 76: 418-420.
-
Ziv R, Schewach-Millet M, Trau H (1986) Discoid lupus erythematosus of the eyelids. J Am Acad Dermatol 15: 112-113.
-
Ghauri AJ, Valenzuela AA, O'Donnell B, Selva D, Madge SN (2012) Periorbital discoid lupus erythematosus. Ophthalmology 119: 2193-2194.
-
Deprez M, Uffer S (2009) Clinicopathological features of eyelid skin tumors. A retrospective study of 5504 cases and review of literature. Am J Dermatopathol 31: 256-262.
-
Zedek DC, Smith ET Jr, Hitchcock MG, Feldman SR, Shelton BJ, et al. (2007) Cutaneous lupus erythematosus simulating squamous neoplasia: The clinicopathologic conundrum and histopathologic pitfalls. J Am Acad Dermatol 56: 1013-1020.
-
Kopsachilis N, Tsaousis KT, Tourtas T, Tsinopoulos IT (2013) Severe chronic blepharitis and scarring ectropion associated with discoid lupus erythematosus. Clin Exp Optom 96: 124-125.
-
Fraga J, García-Díez A (2008) Lupus erythematosus panniculitis. Dermatol Clin 26: 453-463.
-
Arthurs BP, Khalil MK, Chagnon F, Lindley SK, Anderson DP, et al. (1999) Orbital infarction and melting in a patient with systemic lupus erythematosus. Ophthalmology 106: 2387-2390.
-
Inuzuka M, Tomita K, Tokura Y, Takigawa M (2001) Lupus erythematosus profundus with unusual skin manifestation: subcutaneous nodules coexisting with eyelid plaques. J Dermatol 28: 437-441.
-
Jordan DR, McDonald H, Olberg B, McKim D, McKendry R (1993) Orbital panniculitis as the initial manifestation of systemic lupus erythematosus. Ophthal Plast Reconstr Surg 9: 71-75.
-
Magee KL, Hymes SR, Rapini RP, Yeakley JW, Jordon RE (1991) Lupus erythematosus profundus with periorbital swelling and proptosis. J Am Acad Dermatol 24: 288-290.
-
Ohsie LH, Murchison AP, Wojno TH (2012) Lupus erythematosus profundus masquerading as idiopathic orbital inflammatory syndrome. Orbit 31: 181-183.
-
Fonseca P, Manno RL, Miller NR (2013) Bilateral sequential trochleitis as the presenting feature of systemic lupus erythematosus. J Neuroophthalmol 33: 74-76.
-
Feinfield RE, Hesse RJ, Rosenberg SA (1991) Orbital inflammatory disease associated with systemic lupus erythematosus. South Med J 84: 98-99.
-
Grimson BS, Simons KB (1983) Orbital inflammation, myositis, and systemic lupus erythematosus. Arch Ophthalmol 101: 736-738.
-
Sanchez IJ, Finger DR, Bradshaw DJ (1995) Orbital inflammatory syndrome and systemic lupus erythematosus. J Clin Rheumatol 1: 295-298.
-
Serop S, Vianna RN, Claeys M, De Laey JJ (1994) Orbital myositis secondary to systemic lupus erythematosus. Acta Ophthalmol (Copenh) 72: 520-523.
-
Calistri V, Mostardini C, Pantano P, Pierallini A, Colonnese C, et al. (2002) Tolosa-Hunt syndrome in a patient with systemic lupus erythematosus. Eur Radiol 12: 341-344.
-
Gilboe IM, Kvien TK, Uhlig T, Husby G (2001) Sicca symptoms and secondary Sjögren's syndrome in systemic lupus erythematosus: comparison with rheumatoid arthritis and correlation with disease variables. Ann Rheum Dis 60: 1103-1109.
-
Jensen JL, Bergem HO, Gilboe IM, Husby G, Axéll T (1999) Oral and ocular sicca symptoms and findings are prevalent in systemic lupus erythematosus. J Oral Pathol Med 28: 317-322.
-
Manoussakis MN, Georgopoulou C, Zintzaras E, Spyropoulou M, Stavropoulou A, et al. (2004) Sjögren's syndrome associated with systemic lupus erythematosus: clinical and laboratory profiles and comparison with primary Sjögren's syndrome. Arthritis Rheum 50: 882-891.
-
Nossent JC, Swaak AJ (1998) Systemic lupus erythematosus VII: frequency and impact of secondary Sjøgren's syndrome. Lupus 7: 231-234.
-
Fox RI (2005) Sjögren's syndrome. Lancet 366: 321-331.
-
Alves M, Fonseca EC, Alves MF, Malki LT, Arruda GV, et al. (2013) Dry eye disease treatment: a systematic review of published trials and a critical appraisal of therapeutic strategies. Ocul Surf 11: 181-192.
-
Chauhan SK, El Annan J, Ecoiffier T, Goyal S, Zhang Q, et al. (2009) Autoimmunity in dry eye is due to resistance of Th17 to Treg suppression. J Immunol 182: 1247-1252.
-
Reeves JA (1965) Keratopathy associated with systemic lupus erythematosus. Arch Ophthalmol 74: 159-160.
-
Adan CB, Trevisani VF, Vasconcellos M, de Freitas D, de Souza LB, et al. (2004) Bilateral deep keratitis caused by systemic lupus erythematosus. Cornea 23: 207-209.
-
Raizman MB, Baum J (1989) Discoid lupus keratitis. Arch Ophthalmol 107: 545-547.
-
Halmay O, Ludwig K (1964) Bilateral band-shaped deep keratitis and iridocyclitis in systemic lupus erythematosus. Br J Ophthalmol 48: 558-562.
-
Varga JH, Wolf TC (1993) Bilateral transient keratoendotheliitis associated with systemic lupus erythematosus. Ann Ophthalmol 25: 222-223.
-
Messmer EM, Foster CS (1999) Vasculitic peripheral ulcerative keratitis. Surv Ophthalmol 43: 379-396.
-
Cua IY, Pepose JS (2002) Late corneal scarring after photorefractive keratectomy concurrent with development of systemic lupus erythematosus. J Refract Surg 18: 750-752.
-
Carp GI, Verhamme T, Gobbe M, Ayliffe WH, Reinstein DZ (2010) Surgically induced corneal necrotizing keratitis following LASIK in a patient with inflammatory bowel disease. J Cataract Refract Surg 36: 1786-1789.
-
Aman-Ullah M, Gimbel HV, Purba MK, van Westenbrugge JA (2012) Necrotizing keratitis after laser refractive surgery in patients with inactive inflammatory bowel disease. Case Rep Ophthalmol 3: 54-60.
-
Smith RJ, Maloney RK (2006) Laser in situ keratomileusis in patients with autoimmune diseases. J Cataract Refract Surg 32: 1292-1295.
-
Alió JL, Artola A, Belda JI, Perez-Santonja JJ, Muñoz G, et al. (2005) LASIK in patients with rheumatic diseases: a pilot study. Ophthalmology 112: 1948-1954.
-
Jabs DA, Mudun A, Dunn JP, Marsh MJ (2000) Episcleritis and scleritis: clinical features and treatment results. Am J Ophthalmol 130: 469-476.
-
Thorne JE, Jabs DA, Nikolskaia O, Anhalt G, Nousari HC (2002) Discoid lupus erythematosus and cicatrizing conjunctivitis: Clinicopathologic study of two cases. Ocul Immunol Inflamm 10: 287-292.
-
Uy HS, Pineda R 2nd, Shore JW, Polcharoen W, Jakobiec FA, et al. (1999) Hypertrophic discoid lupus erythematosus of the conjunctiva. Am J Ophthalmol 127: 604-605.
-
Dubois EL, Tuffanelli DL (1964) Clinical manifestations of systemic lupus erythematosus. Computer Analysis of 520 cases. JAMA 190: 104-111.
-
Foster RE, Lowder CY, Meisler DM, Valenzuela R, McMahon JT, et al. (1994) An unusual ocular manifestation of discoid lupus erythematosus. Cleve Clin J Med 61: 232-237.
-
Wong RW, Chan A, Johnson RN, McDonald HR, Kumar A, et al. (2010) Posterior scleritis in patients with systemic lupus erythematosus. Retin Cases Brief Rep 4: 326-331.
-
Sainz de la Maza M, Foster CS, Jabbur NS (1995) Scleritis associated with systemic vasculitic diseases. Ophthalmology 102: 687-692.
-
Wagemans MA, Bos PJ (1989) Angle-closure glaucoma in a patient with systemic lupus erythematosus. Doc Ophthalmol 72: 201-207.
-
Pavesio CE, Meier FM (2001) Systemic disorders associated with episcleritis and scleritis. Curr Opin Ophthalmol 12: 471-478.
-
Rosenbaum JT, Wernick R (1990) The utility of routine screening of patients with uveitis for systemic lupus erythematosus or tuberculosis. A Bayesian analysis. Arch Ophthalmol 108: 1291-1293.
-
Rodriguez A, Calonge M, Pedroza-Seres M, Akova YA, Messmer EM, et al. (1996) Referral patterns of uveitis in a tertiary eye care center. Arch Ophthalmol 114: 593-599.
-
Jiménez-Alonso J, Martín-Armada M, Toribio M, Herranz-Marín MT, Rivera-Cívico F, et al. (2002) Incidence of systemic lupus erythematosus among 255 patients with uveitis of unknown origin. Ann Rheum Dis 61: 471.
-
Bañares A, Jover JA, Fernández-Gutiérrez B, Benítez del Castillo JM, García J, et al. (1997) Patterns of uveitis as a guide in making rheumatologic and immunologic diagnoses. Arthritis Rheum 40: 358-370.
-
Drosos AA, Petris CA, Petroutsos GM, Moutsopoulos HM (1989) Unusual eye manifestations in systemic lupus erythematosus patients. Clin Rheumatol 8: 49-53.
-
Zink JM, Singh-Parikshak R, Johnson CS, Zacks DN (2005) Hypopyon uveitis associated with systemic lupus erythematosus and antiphospholipid antibody syndrome. Graefes Arch Clin Exp Ophthalmol 243: 386-388.
-
Gold DH, Morris DA, Henkind P (1972) Ocular findings in systemic lupus erythematosus. Br J Ophthalmol 56: 800-804.
-
Stafford-Brady FJ, Urowitz MB, Gladman DD, Easterbrook M (1988) Lupus retinopathy. Patterns, associations, and prognosis. Arthritis Rheum 31: 1105-1110.
-
Klinkhoff AV, Beattie CW, Chalmers A (1986) Retinopathy in systemic lupus erythematosus: relationship to disease activity. Arthritis Rheum 29: 1152-1156.
-
Ushiyama O, Ushiyama K, Koarada S, Tada Y, Suzuki N, et al. (2000) Retinal disease in patients with systemic lupus erythematosus. Ann Rheum Dis 59: 705-708.
-
Ho TY, Chung YM, Lee AF, Tsai CY (2008) Severe vaso-occlusive retinopathy as the primary manifestation in a patient with systemic lupus erythematosus. J Chin Med Assoc 71: 377-380.
-
Nag TC, Wadhwa S (2005) Histopathological changes in the eyes in systemic lupus erythematosus: An electron microscope and immunohistochemical study. Histol Histopathol 20: 373-382.
-
Giocanti-Auregan A, Grenet T, Rohart C, Badelon I, Chaine G (2013) Inaugural severe vaso-occlusive retinopathy in systemic lupus erythematosus. Int Ophthalmol 33: 323-326.
-
Md Noh UK, Zahidin AZ, Yong TK (2012) Retinal vasculitis in systemic lupus erythematosus: an indication of active disease. Clin Pract 2: e54.
-
Chang PC, Chen WS, Lin HY, Lee HM, Chen SJ (2010) Combined central retinal artery and vein occlusion in a patient with systemic lupus erythematosus and anti-phospholipid syndrome. Lupus 19: 206-209.
-
Song YH, Kim CG, Kim SD, Kim YY, Choe JY (2001) Systemic lupus erythematosus presenting earlier as retinal vaso-occlusion. Korean J Intern Med 16: 210-213.
-
Nishiguchi KM, Ito Y, Terasaki H (2013) Bilateral central retinal artery occlusion and vein occlusion complicated by severe choroidopathy in systemic lupus erythematosus. Lupus 22: 733-735.
-
Mendrinos E, Mavrakanas N, Kiel R, Pournaras CJ (2009) Bilateral combined central retinal artery and vein occlusion in systemic lupus erythematosus resulting in complete blindness. Eye (Lond) 23: 1231-1232.
-
Hwang HS, Kang S (2012) Combined central retinal vein and artery occlusion in systemic lupus erythematosus patient. Retin Cases Brief Rep 6: 187-188.
-
Read RW, Chong LP, Rao NA (2000) Occlusive retinal vasculitis associated with systemic lupus erythematosus. Arch Ophthalmol 118: 588-589.
-
Cooper BA, Shah GK, Grand MG (2004) Purtscher's-like retinopathy in a patient with systemic lupus erythematosus. Ophthalmic Surg Lasers Imaging 35: 438-439.
-
Wu C, Dai R, Dong F, Wang Q (2014) Purtscher-like retinopathy in systemic lupus erythematosus. Am J Ophthalmol 158: 1335-1341.
-
Kunavisarut P, Pathanapitoon K, Rothova A (2015) Purtscher-like Retinopathy Associated with Systemic Lupus Erythematosus. Ocul Immunol Inflamm.
-
Noma H, Shimizu H, Mimura T (2013) Unilateral macular edema with central retinal vein occlusion in systemic lupus erythematosus: a case report. Clin Ophthalmol 7: 865-867.
-
Yen YC, Weng SF, Chen HA, Lin YS (2013) Risk of retinal vein occlusion in patients with systemic lupus erythematosus: a population-based cohort study. Br J Ophthalmol 97: 1192-1196.
-
Quillen DA, Stathopoulos NA, Blankenship GW, Ferriss JA (1997) Lupus associated frosted branch periphlebitis and exudative maculopathy. Retina 17: 449-451.
-
Sekimoto M, Hayasaka S, Noda S, Setogawa T (1993) Pseudoretinitis pigmentosa in patients with systemic lupus erythematosus. Ann Ophthalmol 25: 264-266.
-
Neumann R, Foster CS (1995) Corticosteroid-sparing strategies in the treatment of retinal vasculitis in systemic lupus erythematosus. Retina 15: 201-212.
-
Hong-Kee N, Mei-Fong C, Azhany Y, Zunaina E (2014) Antiphospholipid syndrome in lupus retinopathy. Clin Ophthalmol 8: 2359-2363.
-
Snyers B, Lambert M, Hardy JP (1990) Retinal and choroidal vaso-occlusive disease in systemic lupus erythematosus associated with antiphospholipid antibodies. Retina 10: 255-260.
-
Nguyen QD, Uy HS, Akpek EK, Harper SL, Zacks DN, et al. (2000) Choroidopathy of systemic lupus erythematosus. Lupus 9: 288-298.
-
Jabs DA, Hanneken AM, Schachat AP, Fine SL (1988) Choroidopathy in systemic lupus erythematosus. Arch Ophthalmol 106: 230-234.
-
Gharbiya M, Bozzoni-Pantaleoni F, Augello F, Balacco-Gabrieli C (2002) Indocyanine green angiographic findings in systemic lupus erythematosus choroidopathy. Am J Ophthalmol 134: 286-290.
-
Cho HY, Nasir HH, Sobrin L (2014) Focal laser photocoagulation and photodynamic therapy for lupus choroidopathy. Lupus 23: 412-416.
-
Shimura M, Tatehana Y, Yasuda K, Saito Si, Sasaki T, et al. (2003) Choroiditis in systemic lupus erythematosus: systemic steroid therapy and focal laser treatment. Jpn J Ophthalmol 47: 312-315.
-
Nicholson L, Sobrin L (2013) The use of pars plana vitrectomy in the treatment of a serous retinal detachment secondary to lupus choroidopathy. Ophthalmic Surg Lasers Imaging Retina 44: 502-504.
-
Hafidi Z, Handor H, Berradi S, Regragui A, El Atiqi A, et al. (2015) Punctate inner choroidopathy in systemic lupus. J Fr Ophtalmol 38: e49-50.
-
Man BL, Mok CC, Fu YP (2014) Neuro-ophthalmologic manifestations of systemic lupus erythematosus: a systematic review. Int J Rheum Dis 17: 494-501.
-
Jabs DA, Miller NR, Newman SA, Johnson MA, Stevens MB (1986) Optic neuropathy in systemic lupus erythematosus. Arch Ophthalmol 104: 564-568.
-
Siatkowski RM, Scott IU, Verm AM, Warn AA, Farris BK, et al. (2001) Optic neuropathy and chiasmopathy in the diagnosis of systemic lupus erythematosus. J Neuroophthalmol 21: 193-198.
-
Ahmadieh H, Roodpeyma S, Azarmina M, Soheilian M, Sajjadi SH (1994) Bilateral simultaneous optic neuritis in childhood systemic lupus erythematosus. A case report. J Neuroophthalmol 14: 84-86.
-
Hackett ER, Martinez RD, Larson PF, Paddison RM (1974) Optic neuritis in systemic lupus erythematosus. Arch Neurol 31: 9-11.
-
Im CY, Kim SS, Kim HK (2002) Bilateral optic neuritis as first manifestation of systemic lupus erythematosus. Korean J Ophthalmol 16: 52-58.
-
Lin YC, Wang AG, Yen MY (2009) Systemic lupus erythematosus-associated optic neuritis: clinical experience and literature review. Acta Ophthalmol 87: 204-210.
-
Frohman LP, Frieman BJ, Wolansky L (2001) Reversible blindness resulting from optic chiasmitis secondary to systemic lupus erythematosus. J Neuroophthalmol 21: 18-21.
-
Frigui M, Frikha F, Sellemi D, Chouayakh F, Feki J, et al. (2011) Optic neuropathy as a presenting feature of systemic lupus erythematosus: two case reports and literature review. Lupus 20: 1214-1218.
-
Rosenbaum JT, Simpson J, Neuwelt CM (1997) Successful treatment of optic neuropathy in association with systemic lupus erythematosus using intravenous cyclophosphamide. Br J Ophthalmol 81: 130-132.
-
Galindo M, Pablos JL, Gómez-Reino JJ (1998) Internuclear ophthalmoplegia in systemic lupus erythematosus. Semin Arthritis Rheum 28: 179-186.
-
Alonso-Valdivielso JL, Alvarez Lario B, Alegre López J, Sedano Tous MJ, Buitrago Gómez A (1993) Acquired Brown's syndrome in a patient with systemic lupus erythematosus. Ann Rheum Dis 52: 63-64.
-
McGalliard J, Bell AL (1990) Acquired Brown's syndrome in systemic lupus erythematosus: another ocular manifestation. Clin Rheumatol 9: 399-400.
-
Whitefield L, Isenberg DA, Brazier DJ, Forbes J (1995) Acquired Brown's syndrome in systemic lupus erythematosus. Br J Rheumatol 34: 1092-1094.
-
Saleh Z, Menassa J, Abbas O, Atweh S, Arayssi T (2010) Cranial nerve VI palsy as a rare initial presentation of systemic lupus erythematosus: case report and review of the literature. Lupus 19: 201-205.
-
Abel MP1, Murphy FT, Enzenauer RJ, Enzenauer RW (2003) Internuclear ophthalmoplegia (INO): an unusual presentation of neuropsychiatric lupus erythematosus. Binocul Vis Strabismus Q 18: 29-30.
-
Cakir A, Duzgun E, Demir S, Aydin A (2014) Jerky seesaw nystagmus with internuclear ophthalmoplegia as the presenting finding in systemic lupus erythematosus. J Fr Ophtalmol 37: e157-159.
-
Cogen MS, Kline LB, Duvall ER (1987) Bilateral internuclear ophthalmoplegia in systemic lupus erythematosus. J Clin Neuroophthalmol 7: 69-73.
-
Jackson G, Miller M, Littlejohn G, Helme R, King R (1986) Bilateral internuclear ophthalmoplegia in systemic lupus erythematosus. J Rheumatol 13: 1161-1162.
-
Meyer MW, Wild JH (1975) Letter: Unilateral internuclear ophthalmoplegia in systemic lupus erythematosus. Arch Neurol 32: 486.
-
Rheu CW, Lee SI, Yoo WH (2005) A catastrophic-onset longitudinal myelitis accompanied by bilateral internuclear ophthalmoplegia in a patient with systemic lupus erythematosus. J Korean Med Sci 20: 1085-1088.
-
Carlow TJ, Glaser JS (1974) Pseudotumor cerebri syndrome in systemic lupus erythematosus. JAMA 228: 197-200.
-
Rajasekharan C, Renjith SW, Marzook A, Parvathy R (2013) Idiopathic intracranial hypertension as the initial presentation of systemic lupus erythematosus. BMJ Case Rep 2013.
-
Shin SY, Lee JM (2006) A case of multiple cranial nerve palsies as the initial ophthalmic presentation of antiphospholipid syndrome. Korean J Ophthalmol 20: 76-78.
-
Dave S, Longmuir R, Shah VA, Wall M, Lee AG (2008) Intracranial hypertension in systemic lupus erythematosus. Semin Ophthalmol 23: 127-133.
-
Duprez T, Nzeusseu A, Peeters A, Houssiau FA (2001) Selective involvement of the choroid plexus on cerebral magnetic resonance images: a new radiological sign in patients with systemic lupus erythematosus with neurological symptoms. J Rheumatol 28: 387-391.
-
Nampoory MR, Johny KV, Gupta RK, Constandi JN, Nair MP, et al. (1997) Treatable intracranial hypertension in patients with lupus nephritis. Lupus 6: 597-602.
-
Green L, Vinker S, Amital H, Amir T, Bar-Dayan Y, et al. (1995) Pseudotumor cerebri in systemic lupus erythematosus. Semin Arthritis Rheum 25: 103-108.





