International Journal of Ophthalmology and Clinical Research
A Novel Osmoprotectant Tear Substitute for the Treatment of Dry Eye Disease
Giuseppe Giannaccare, Michela Fresina and Piera Versura*
Ophthalmology Unit, DIMES, Alma Mater Studiorum University of Bologna and S. Orsola-Malpighi Teaching Hospital, Bologna, Italy
*Corresponding author: Piera Versura, BSD, Ophthalmology Unit, DIMES University of Bologna S.Orsola-Malpighi Hospital, Pad. 1, Via Palagi, 9 40138 Bologna, Italy, Tel: +39 051 2142850, Fax: +39 051 6362846, E-mail: piera.versura@unibo.it
Int J Ophthalmol Clin Res, IJOCR-3-058, (Volume 3, Issue 3), Research Article; ISSN: 2378-346X
Received: April 21, 2016 | Accepted: June 03, 2016 | Published: July 05, 2016
Citation: Giannaccare G, Fresina M, Versura P(2016) A Novel Osmoprotectant Tear Substitute for the Treatment of Dry Eye Disease. Int J Ophthalmol Clin Res 3:058. 10.23937/2378-346X/1410058
Copyright: © 2016 Giannaccare G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: To investigate whether the application of a novel product containing a mix of osmoprotectant soluble molecules can modify tear osmolarity, clinical signs and subjective symptoms in dry eye patients.
Methods: Thirty patients (24 women, 6 men, median age 45.5 yrs) were enrolled. Inclusion criteria were: age ≥ 18 years, good general health, ocular discomfort symptoms for over three months, Ocular Surface Disease Index (OSDI) score ranging from 18 to 36, Schirmer test > 10 mm/5 min, Tear Film Break Up Time (TBUT) < 10 sec, corneal fluorescein staining ranging from 1 to 7 according to NEI level. Patients were administered three times daily for a two-month period with Isomar Eyes Plus, a hypotonic solution containing Hyaluronic Acid, Hypromellose and L-Carnitine, erythrol and betaine as osmoprotectant soluble molecules. Tear osmolarity (TearLab), Schirmer I Test, corneal and conjunctival vital stainings, conjunctival impression cytology with goblet cell (GCs) count, symptom intensity evaluation with VAS (Visual Analogue Scale) technique were performed and compared at endpoint versus baseline.
Results: At endpoint versus baseline, respectively, variables significantly improved (Wilcoxon test, p always < 0.01). Data are expressed as median (min-max values) [CI 95%]). Tear osmolarity (mOsm/L): 290 (279-301) [286-298] versus 307 (293-315) [300-312]; OSDI (score): 16 (16-26) [16-19.4] versus 28 (18-36) [24-30]; VAS (score): 2.8 (1.5-3.5) [2.1-2.9] versus 5.9 (5.2-7.1) [5.8-6.1]; TFBUT (sec): 9.5 (8-12) [8.5-10.7] versus 7.1 (5.4-9) [6.5-7.8]; vital staining showed complete epithelial healing at endpoint in 48 out of 60 eyes; imprint cytology score: 1 (1-2) [1-1.2] versus 1.5 (1-2.5) [1-1.5]. GC density improved at endpoint (media ± SD: 182.6 ± 28.6 cells/mm2) as compared to baseline (142.5 ± 25.6 cells/mm2, p < 0.01). Tolerability was high, with no adverse events noted.
Conclusions: A two-month treatment with Isomar eyes plus, containing L-Carnitine, Erythrol and Betaine as osmoprotectants, is able to reduce tear osmolarity, subjective symptoms of discomfort and ocular surface epithelial damage, associated to an increasing tear film stability.
Keywords
Dry eye, Tear instability, Ocular discomfort, Visual related function, OSDI score, VAS score, Osmoprotectants
Introduction
Increasing evidence suggests that osmotic stress, caused by altered extracellular osmolality, is a highly relevant challenge to normal cell function in a variety of tissues, including human bronchial epithelial cells [1,2], peripheral blood mononuclear cells [3], kidney [4], and the corneal epithelium [5]. Dry eye disease (DED) is "a multifactorial disease of the tears and ocular surface that results in symptoms of discomfort, visual disturbance, and tear film instability with potential damage to the ocular surface. It is accompanied by increased osmolarity of the tear film and inflammation of the ocular surface" [6]. The pathophysiology of DED is referred as a vicious circle where tear hyperosmolarity plays a key role [7]. Tear hyperosmolarity stimulates death of the epithelial surface cells and a cascade of inflammatory events, which lead to loss of mucin-producing goblet cells. This exacerbates the tear film instability and contributes to the circle of events that perpetuate DED [8]. Both in vitro and in vivo experiments have linked hyperosmolarity to inflammatory changes in DED [9,10].
Various therapies are addressed to reduce hyperosmolarity in DED. Traditional approaches include the use of hypotonic tear substitutes, which shows a limited stay for a few minutes after instillation [11]. Treatments may also benefit from inclusion of osmoprotectants in the tear substitute formulation; these are naturally occurring compatible solutes that are internalized by cells, restoring cell volume and stabilizing proteins. Recent formulations of artificial tears including one or more osmoprotectants have been developed. The osmoprotective effects of L-Carnitine, betaine, and glycerol have been previously shown in osmotically stressed bacteria and yeast [12-15]. In particular, betaine is one of the essential osmolytes accumulated in most tissues to assist cell volume regulation [16-20]. It has been reported that addition of betaine to cultured human corneal epithelial cells subjected to hyperosmolar media inhibited the hyperosmotic-induced phosphorylation ratios of Jun-N-terminal and p38 kinases to below the ratios found for physiologic osmolarity, indicating an osmo protective role for betaine in these cells [21]. Garrett and collaborators demonstrated the ability of exogenous betaine to stabilize human corneal limbal epithelial (HCLE) cell volume under hyperosmotic stress and to limit hyperosmotic stress-induced HCLE apoptosis, thus aiding the survival of HCLE cells under hyperosmotic stress [22].
The purpose of this study is to preliminarily investigate whether the application of a novel product containing L-Carnitine, erythrol and betaine as osmoprotectant soluble molecules designed to reduce the tear hyperosmolarity can modify signs, symptoms and tear osmolarity in dry eye patients.
Methods
This was a prospective, open-label, single-centre study performed at one research site in Bologna, Italy (Ophthalmic Unit, University of Bologna, S. Orsola-Malpighi Hospital).
Thirty patients (sixty eyes) affected by mild-moderate hyper evaporative DED with subjective ocular discomfort symptoms for over three months were enrolled (24 women, 6 men, median age 45.5 years, min-max value 24-53 yrs, 95% CI 42.3-51 yrs). The study was approved by the local Independent Ethics Committee and was conducted in accordance with the ethical principles of the Declaration of Helsinki and in agreement with the current legislation on clinical research in Italy. All subjects signed an informed consent form before starting the study.
Inclusion criteria were: age ≥ 18 years, good general health, ocular discomfort symptoms for over three months, Ocular Surface Disease Index (OSDI) [23] score ranging from 18 to 36, Schirmer test > 10 mm/5 min, TBUT < 10 sec, corneal fluorescein staining ranging from 1 to 17 according to NEI level [24].
Exclusion criteria were: previous ocular surgery performed in the year leading up to the visit; wearing contact lenses; punctual plug placement or cauterization, ocular allergy, concomitant topic medications. Subjects who met the inclusion criteria of the study were dispensed sodium chloride-based eye drops, to be used in both eyes for two days (wash-out period). This served to normalize the study population to an identical regimen of eye drops use, and allowed for washout and minimization of any effect from previous lubricant eye drops/medications use.
Treatment
ISOMAR Eyes Plus is an ophthalmic solution hypotonic as compared to natural tears (290 mOsm/L). The product contains 0.25% Hyaluronic Acid (HA), at a molecular weight 1.5-1.8 kD and Hypromellose 0.25%, both substances that give rise to mucus mimetic solutions and muco adhesive, with excellent lubricating properties [25]. The viscosity of such solutions is close to the non-Newtonian fluid behavior of natural tears and is such as to allow an effective moisturizing effect and a stabilization of the tear film. The Polyethylene glycol 0.25% enhances the rheological behavior of HA and its better distribution on the corneal surface. A group of osmoprotectant substances (L-Carnitine, Erythritol) are combined with Betaine, and in this respect the formulation is unique. These substances tested in vitro individually and in combination have proved to exert a protective effect against the hyperosmotic stress [26]. To complete soothing action, extracts of medicinal plants (Cineraria Marittima, Calendula, Euphrasia, Strawflower, Cornflower), known for the refreshing effect on the mucous membranes and epithelia, have been added.
Visits
The study included four visits during two months, i.e., visit 0 (V0, recruitment), after 1-3 days of wash out with sodium chloride eye drops (baseline, V1, beginning of treatment), after 1 month (V2) and after 2 months of therapy (endpoint, V3). Patients were instructed to administer one Isomar Plus® drop/eye/3 times/day and to record any specific sensation at instillation.
Tests
The following tests were performed at all four visits. Subjective symptoms of dry eye were graded on the basis of the OSDI (Ocular Surface Disease Index) dry eye discomfort symptoms questionnaire. Factor analysis disclosed that there were 3 subscales, interpreted as subscale A. ocular symptoms (5 questions); subscale B. Vision-related function (4 questions); and subscale C. environmental triggers (3 questions). Each of the three subscale score was calculated and included in the statistic.
A 100 mm horizontal VAS (Visual Analogue Scale) technique was used to measure symptom intensity. Patients were asked to mark the level of their discomfort on a 100 mm, non-hatched VAS scale marked at one end as "no pain" and at the other as "pain as bad as it could be". Using a ruler, the score was determined by measuring the distance between the "no pain" end and the patient's mark, providing a range of scores from 0-100 with a higher score indicating a greater pain intensity [27].
Tear Film Break Up Time (TBUT) was measured and recorded (average of three measurements) using 2 μL sodium fluorescein (Fluoralfa 0.25%, Alfa Intes, Italy). Schirmer test I was performed by using validated sterile test strips (ContaCare Ophthalmics and Diagnostics, Gujarat, India), as recommended in DEWS [28]. To quantify corneal and conjunctival surface damage, 1% fluorescein sodium vital staining (2 μl volume) was graded according to the NEI (0-15) [24] with the aid of a 7503 Boston yellow filter kit (equivalent to Kodak Wratten 12) to enhance staining details. Conjunctiva Van Bjisterveldt score 0-18 was graded according to Lemp [24].
The following tests were performed at visits V1 and V3. Tear osmolarity was measured with the TearLab Osmolarity System (TearLab Corp, San Diego, CA, USA) at the lower external fornix, as described elsewhere, with the 305 mOsm/L value taken as cut-off for DED diagnosis [29]. Only the higher value among the two eyes was included in the statistical analysis.
Impression cytology was used to evaluate conjunctival epithelial metaplasia and goblet cells (GCs) density. Conjunctival epithelial metaplasia scoring was performed accordingly to DEWS recommendations and scored grading 0-5, as described by Tseng [30], with values > 1 being considered pathological. PAS-positive goblet cells density was expressed as the number of cells/mm2 (mean of four adjacent visual fields at × 100 magnification) [31].
Patient's satisfaction was evaluated by a VAS-based satisfaction questionnaire composed by 4 questions (Table 1). For statistical analysis, score at baseline (V1) concerning their feeling about the last therapy administered prior to the study was compared to endpoint (V3).
![]()
Table 1: Summary of the results from the four-question VAS satisfaction questionnaire. The V1 results refer to answers given by patients concerning their feeling about the last therapy administered prior to the study. A statistically significant (always p < 0.01).
View Table 1
Tolerability was assessed by a VAS scoring of specific symptoms (blurring, redness, itching, stinging) recorded upon instillation.
Statistical analysis
Data were collected in both eyes, with the worse of the two being the more relevant number included in the statistic Data were statistically analysed using the MedCalc 5.0 and SPSS 14 software and applying the Wilcoxon's test for paired to evaluate the changes between baseline and endpoint (p < 0.05 was considered to be statistically significant). Descriptive statistics for tests and variables analysed in subjects were reported as the mean ± SD. Pearson's (r) or Spearman's (ρ) correlation coefficients were applied when appropriate; correlations were considered statistically significant at p < 0.05 (small correlation strength 0.10 to 0.29; medium 0.30 to 0.49; large 0.50 to 1.00).
Results
All subjects enrolled for treatment completed the study. They declared to have administered the eye drops three times/day as requested in the protocol. No significant changes in any of the tests performed were observed between enrolment (V0) and baseline visits (V1), data from visit V0 were however included in graphs.
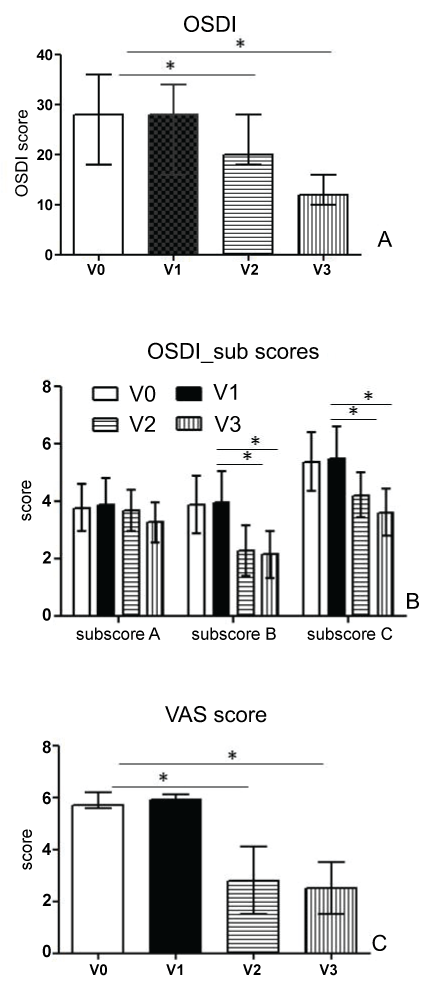
Subjects underwent to a progressive and statistically significant reduction of discomfort symptoms, as evaluated by OSDI score (Figure 1A); in particular, the OSDI score at endpoint was shown to be half that detected at baseline. OSDI was further analysed in the following three subscales: ocular symptoms, vision-related functions, and environmental triggers (Figure 1B). Scores on the ocular symptoms subscale improved significantly more in vision-related functions (sub-scale B) and environmental triggers (sub-scale C).
.
Figure 1: Results from Ocular Surface Disease Index (A) and VAS score (C) for subjective symptoms, recorded at enrollment (V0), baseline (V1) and after one (V2) and two (endpoint, V3) months of treatment with Isomar Eyes Plus. OSDI sub scores graphed in B refer to ocular symptoms questions (sub scale A), vision-related function questions (sub scale B) and environmental trigger questions (subscale C). *Indicate statistically significant results p < 0.05.
View Figure 1
The Visual Analogue Scale of symptoms was also shown to be significantly reduced already at V2, with a value at endpoint found to be half that detected at baseline (Figure 1C).
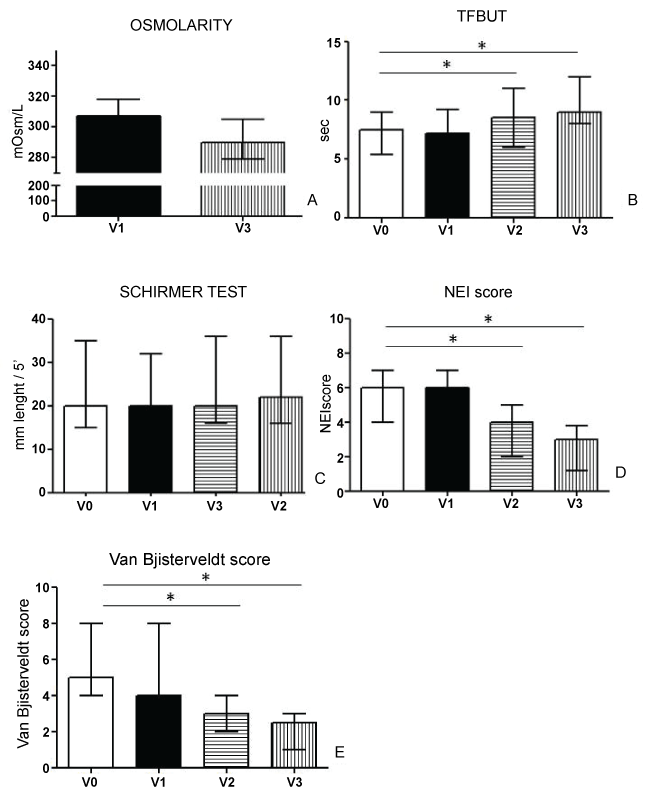
In figure 2 results from clinical tests were summarized. Statistically significant decrease in tear osmolality was found at endpoint versus baseline (Figure 2A). Statistically significant improvement of TFBUT from baseline were observed at each follow-up visit and endpoint (Figure 2B) whereas Schirmer I test did not show significant changes in tear production from baseline at each follow-up visit and endpoint (Figure 2C). Corneal staining scores (Figure 2D) and conjunctival staining scores (Figure 2E) were significantly decreased from baseline at each follow-up visit and endpoint.
.
Figure 2: Summary of results from Tear Osmolarity (A), Tear Film Break Up Time (B), Schirmer I test (C), corneal vital staining scored with the NEI (National Eye Institute) score (D) and conjunctival vital staining scored with the van Bjisterveldt score (E) recorded at enrollment (V0), baseline (V1) and after one (V2) and two (endpoint, V3) months of treatment with Isomar Eyes Plus. *Indicate statistically significant results p < 0.05.
View Figure 2
A strong direct correlation between tear osmolarity and VAS score of subjective symptom of discomfort was shown either at baseline and endpoint (respectively Spearman's ρ = 0.610 and 0.629, p < 0.01).
Conjunctival epithelial metaplasia score significantly decreased to 0.8 ± 0.3 at endpoint (V3) with respect to baseline (V1, 1.4 ± 0.5). Conjunctival impression cytology showed a statistically significant increase in GC density at endpoint (V3, media ± SD: 182.6 ± 28.6 cells/mm2) as compared to baseline (V1, 142.5 ± 25.6 cells/mm2, p < 0.01).
Scores for the VAS satisfaction questionnaire are summarized in table 1. Symptom relief after one month treatment and further at endpoint (V3) with respect to baseline (V1) was found. The V1 point showed the answers given by patients at baseline, which refer to their feeling about the last topical therapy administered before the present study.
The overall incidence of treatment-related Adverse Events (AEs) was very low and feelings were disappearing within 3 minutes from instillation. Mild eye irritation with conjunctival hyperemia was reported in 1 subjects, blurred vision was reported in another subject. The rate of discontinuations due to AEs was 0%.
Discussion
The present study demonstrated that treatment with a novel multiple action solution containing three osmo protectant molecules including betaine is able to reduce tear osmolarity value in mild to moderate DED patients. This was shown to be associated to an increase in tear stability, a reduction of subjective discomfort symptoms and ocular surface epithelial damage.
DED is characterized by the presence of typical symptoms of irritation, burning, itching, and sensation of a foreign body eye that significantly affect the quality of life the patients. Even in its early stages, DED subjective symptoms are accompanied by increased osmolarity of tears and reduction of mucus cells, which progresses to an advanced stage epithelial metaplasia and conjunctival pseudo-keratinization of mucosa [32]. The main mechanisms of DED are part of a vicious cycle that is self-perpetuating in the absence of adequate therapy, and can be traced back to four cornerstones referred as tear hyper osmolarity, tear instability, cell apoptosis and inflammation with release of various cytokines and MMPs.
Tear substitutes represent the first-level treatment for DED and their formulations have undergone numerous improvements to enhance their efficacy and safety to the ocular surface [33]. In vitro studies showed that some substances with osmo protectant action such as L-Carnitine, betaine, glycerol, and the polyol erythritol significantly lowered levels of activated MAP kinases in human corneal cells subjected to hyperosmolar stress condition that simulate the DED [21]. Interestingly, these osmo protectants not only suppressed production but also inhibited activation of MMP-9 and MMP-2, and L-Carnitine showed the strongest suppressive effect on these MMPs [34]. L-Carnitine was also shown to regulate cell volume under hyperosmotic stress in vitro models and ameliorate hyperosmotic stress-induced apoptosis evaluated with TNF-alpha release and caspase enzymes activity [35]. Betaine was shown to exert similar protective effects against apoptosis [22]. Further, osmoprotectant L-Carnitine, erythritol and betaine were shown to suppress inflammatory responses in HCECs exposed to hyperosmotic stress, with particular reference to pro-inflammatory cytokines, TNF-α, IL-1β and IL-6, and chemokines, IL-8, CCL2 and CCL20, thus providing evidence on potential efficacy in reducing innate inflammation in DED [36]. Efficacy of osmo protectants betaine, L-Carnitine and erythrol was also confirmed in environmentally induced DED animal models. Treatment of mouse dry eye with osmo protectants resulted in a significant reduction in corneal staining, number of apoptotic epithelial cells, and expression of TNF-α, IL-17, IL-6, or IL-1β, as well as significantly increase of conjunctival goblet cells density [26]. L-Carnitine and erythrol enter in formulations of commercially available tear substitutes and the efficacy of these products has been evaluated in the course of clinical trials.
Kaercher and coll performed observational studies in large populations of DED patients and found a reduction in subjective symptoms of discomfort and improvement of tear stability after 4 weeks treatment with products containing osmo protectants L/Carnitine and erythrol [37,38].
Subjective symptom reduction and improvement of tear stability were confirmed in another multi centre study after three months of therapy with the same commercially available products containing osmo protectant L-Carnitine and erythrol [39]. On the contrary, Lanzini and coll found no significant difference in Schirmer I Test, TFBUT and vital staining but significant reduction of the expression of MMP-9 and IL6 associated to a better in vivo confocal microscopy ocular surface morphology in an osmo protectant containing product treated group compared to a non-osmo protectant product treated control group of DED patients [40].
All patients enrolled in the present study exhibited good compliance to the treatment: data showed good tolerability, lacking of adverse effects upon instillation and high satisfaction score. All patients reported a statistically significant reduction in subjective symptoms of discomfort, conjunctival epithelium metaplasia (associated to increase of GC density) and tear osmolarity values, both after one month treatment and at endpoint by comparison with baseline. A strong direct correlation was found between DED symptoms scored with VAS scale and tear osmolarity values, in agreement with previous works [41,42], and further confirming the role of tear hyper osmolarity in epithelial damage [9,43].
Our results showed statistically significant increasing in TFBUT in all patients, improving over time, although only 21 out of 30 patients was able to reach normal values over the period of observation in this study. Both corneal and conjunctival epithelial damage were significantly reduced after one month of treatment and vital staining showed complete epithelial healing at endpoint in 48 out of 60 eyes.
In summary, our study demonstrated that a two-month treatment in mild to moderate dry eye patients with Isomar eyes plus, containing L-Carnitine, Erythrol and Betaine as osmoprotectants, is able to reduce tear osmolarity, subjective symptoms and ocular surface epithelial damage, associated to an increasing tear film stability.
Conflict of Interest
The authors have no financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in this manuscript.
Authorship Credit
All authors contributed to conception, design and acquisition of data, GG and PV analyzed and interpreted data.
References
-
Hashimoto S, Matsumoto K, Gon Y, Nakayama T, Takeshita I, et al. (1999) Hyperosmolarity-induced interleukin-8 expression in human bronchial epithelial cells through p38 mitogen-activated protein kinase. Am J Respir Crit Care Med 159: 634-640.
-
Loitsch SM, von Mallinckrodt C, Kippenberger S, Steinhilber D, Wagner TO, et al. (2000) Reactive oxygen intermediates are involved in IL-8 production induced by hyperosmotic stress in human bronchial epithelial cells. Biochem Biophys Res Commun 276: 571-578.
-
Shapiro L, Dinarello CA (1997) Hyperosmotic stress as a stimulant for proinflammatory cytokine production. Exp Cell Res 231: 354-362.
-
Brocker C, Thompson DC, Vasiliou V (2012) The role of hyperosmotic stress in inflammation and disease. Biomol Concepts 3: 345-364.
-
Katsuyama I, Arakawa T (2003) A convenient rabbit model of ocular epithelium damage induced by osmotic dehydration. J Ocul Pharmacol Ther 19: 281-289.
-
(2007) The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 5: 75-92.
-
Baudouin C, Aragona P, Messmer EM, Tomlinson A, Calonge M, et al. (2013) Role of hyperosmolarity in the pathogenesis and management of dry eye disease: proceedings of the OCEAN group meeting. Ocul Surf 11: 246-258.
-
Baudouin C (2007) A new approach for better comprehension of diseases of the ocular surface. J Fr Ophtalmol 30: 239-246.
-
Versura P, Profazio V, Schiavi C, Campos EC (2011) Hyperosmolar stress upregulates HLA-DR ecpression in human conjunctival epithelium in dry eye patients and in vitro models. Invest Ophthalmol Vis Sci 52: 5488-5496.
-
Li DQ, Chen Z, Song XJ, Luo L, Pfludfelder SC (2004) Stimulation of matrix met alloproteinases by hyperosmolarity via a JNK pathway in human corneal epithelial cells. Invest Ophthalmol Vis Sci 45: 4302-4311.
-
Holly FJ, Lamberts DW (1981) Effect of nonisotonic solutions on tear film osmolality. Invest Ophthalmol Vis Sci 20: 236-245.
-
Peluso G, Barbarisi A, Savica V, Reda E, Nicolai R, et al. (2000) Carnitine: an osmolyte that plays a metabolic role. J Cell Biochem 80: 1-10.
-
Wood JM, Bremer E, Csonka LN, Kraemer R, Poolman B, et al. (2001) Osmosensing and osmoregulatory compatible solute accumulation by bacteria. Comp Biochem Physiol A Mol Integr Physiol 130: 437-460.
-
Mager WH, Siderius M (2002) Novel insights into the osmotic stress response of yeast. FEMS Yeast Res 2: 251-257.
-
Cánovas M, Bernal V, Sevilla A, Torroglosa T, Iborra JL (2007) Salt stress effects on the central and carnitine metabolisms of Escherichia coli. Biotechnol Bioeng 96: 722-737.
-
Lang F (2007) Mechanisms and significance of cell volume regulation. J Am Coll Nutr 26: 613S-623S.
-
Schliess F, Häussinger D (2002) The cellular hydration state: a critical determinant for cell death and survival. Biol Chem 383: 577-583.
-
Verbalis JG (2010) Brain volume regulation in response to changes in osmolality. Neuroscience 168: 862-870.
-
Wehner F, Olsen H, Tinel H, Kinne-Saffran E, Kinne RKH (2003) Cell volume regulation: osmolytes, osmolyte transport, and signal transduction. Rev Physiol Biochem Pharmacol 148: 1-80.
-
Zhou Y, Holmseth S, Hua R, Lehre AC, Olofsson AM, et al. (2012) The betaine-GABA transporter (BGT1, slc6a12) is predominantly expressed in the liver and at lower levels in the kidneys and at the brain surface. Am J Physiol Renal Physiol 302: F316-F328.
-
Corrales RM, Luo L, Chang EY, Pflugfelder SC (2008) Effects of osmoprotectants on hyperosmolar stress in cultured human corneal epithelial cells. Cornea 27: 574-579.
-
Garrett Q, Khandekar N, Shih S, Flanagana JL, Simmonsc P, et al. (2013) Betaine stabilizes cell volume and protects against apoptosis in human corneal epithelial cells under hyperosmotic stress. Exp Eye Res 108: 33-41.
-
Schiffman RM, Christianson MD, Jacobsen G, Hirsch JD, Reis BL (2000) Reliability and validity of the Ocular Surface Disease Index. Arch Ophthalmol 118: 615-621.
-
Lemp MA (1995) Report of the National Eye Institute/Industry workshop on Clinical Trials in Dry Eyes. CLAO J 21: 221-232.
-
Lee JH, Ahn HS, Kim EK, Kim TI (2011) Efficacy of sodium hyaluronate and carboxymethylcellulose in treating mild to moderate dry eye disease. Cornea 30: 175-179.
-
Chen W, Zhang X, Li J, Wang Y, Chen Q, et al. (2013) Efficacy of osmoprotectants on prevention and treatment of murine dry eye. Invest Ophthalmol Vis Sci 54: 6287-6297.
-
Jensen MP, Karoly P, Braver S (1986) The measurement of clinical pain intensity: a comparison of six methods. Pain 27: 117-126.
-
(2007) Methodologies to diagnose and monitor dry eye disease: report of the Diagnostic Methodology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 5: 108-152.
-
Versura P, Campos EC (2013) TearLab® Osmolarity System for diagnosing dry eye. Expert Rev Mol Diagn 13: 119-129.
-
Tseng SC (1985) Staging of conjunctival squamous metaplasia by impression cytology. Ophthalmology 92: 728-733.
-
Lopin E, Deveney T, Asbell PA (2009) Impression cytology: recent advances and applications in dry eye disease. Ocul Surf 7: 93-110.
-
De Paiva CS, Villarreal AL, Corrales RM, Rahman HT, Chang VY, et al. (2007) Dry eye-induced conjunctival epithelial squamous metaplasia is modulated by interferon-gamma. Invest Ophthalmol Vis Sci 48: 2553-2560.
-
Moshirfar M, Pierson K, Hanamaikai K, Santiago-Caban L, Muthappan V, et al. (2014) Artificial tears potpourri: a literature review. Clin Ophthalmol 8: 1419-1433.
-
Deng R, Su Z, Hua X, Zhang Z, Li DQ, et al. (2014) Osmoprotectants suppress the production and activity of matrix met alloproteinases induced by hyperosmolarity in primary human corneal epithelial cells. Mol Vis 20: 1243-1252.
-
Khandekar N, Willcox MD, Shih S, Simmons P, Vehige J, et al. (2013) Decrease in hyperosmotic stress-induced corneal epithelial cell apoptosis by L-carnitine. Mol Vis 19: 1945-1956.
-
Hua X, Su Z, Deng R, Lin J, Li DQ, et al. (2015) Effects of L-carnitine, erythritol and betaine on pro-inflammatory markers in primary human corneal epithelial cells exposed to hyperosmotic stress. Curr Eye Res 40: 657-667.
-
Kaercher T, Buchholz P, Kimmich F (2009) Treatment of patients with keratoconjunctivitis sicca with Optive: results of a multicenter, open-label observational study in Germany. Clin Ophthalmol 3: 33-39.
-
Kaercher T, Thelen U, Brief G, Morgan-Warren RJ, Leaback R (2014) A prospective, multicenter, noninterventional study of Optive Plus(®) in the treatment of patients with dry eye: the prolipid study. Clin Ophthalmol 8: 1147-1155.
-
Simmons PA, Liu H, Carlisle-Wilcox C, Vehige JG (2015) Efficacy and safety of two new formulations of artificial tears in subjects with dry eye disease: a 3-month, multicenter, active-controlled, randomized trial. Clin Ophthalmol 9: 665-675.
-
Lanzini M, Curcio C, Colabelli-Gisoldi RA, Mastropasqua A, Calienno R, et al. (2015) In Vivo and Impression Cytology Study on the Effect of Compatible Solutes Eye Drops on the Ocular Surface Epithelial Cell Quality in Dry Eye Patients. Mediators Inflamm 2015: 351424.
-
Liu H, Begley C, Chen M, Bradley A, Bonanno J, et al. (2009) A link between tear instability and hyperosmolarity in dry eye. Invest Ophthalmol Vis Sci 50: 3671-3679.
-
Foulks GN (2007) The correlation between the tear film lipid layer and dry eye disease. Surv Ophthalmol 52: 369-374.
-
Pflugfelder SC (2011) Tear dysfunction and the cornea: LXVIII Edward Jackson Memorial Lecture. Am J Ophthalmol 152: 900-909.





