International Journal of Ophthalmology and Clinical Research
Pseudo-Duane Retraction Syndrome Secondary to Orbital Trauma: Case Report
Aysel Pelit*
Department of Ophthalmology, Baskent University, Turkey
*Corresponding author: Prof. Aysel Pelit, Faculty of Medicine, Department of Ophthalmology, Baskent University, Yuregir, Adana/Turkey, Tel: +90322-327-2727, E-mail: aypelitq@yahoo.com
Int J Ophthalmol Clin Res, IJOCR-3-064, (Volume 3, Issue 4), Case Report; ISSN: 2378-346X
Received: September 28, 2016 | Accepted: November 05, 2016 | Published: November 08, 2016
Citation: Pelit A (2016) Pseudo-Duane Retraction Syndrome Secondary to Orbital Trauma: Case Report. Int J Ophthalmol Clin Res 3:064. 10.23937/2378-346X/1410064
Copyright: © 2016 Pelit A. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The report presents a case of type 3 pseudo-Duane retraction syndrome secondary to orbital trauma. There was widening of the palpebral fissure in abduction and globe retraction accompanied by narrowing of the palpebral fissure and up-shoot during attempted adduction. Orbital computed tomography scan was normal.
Introduction
Duane retraction syndrome is an eye movement disorder characterized by deficient abduction of the affected eye, retraction of the globe with adduction, and narrowing of palpebral fissure on attempted adduction [1]. Thomas Duane reported a similar, but different set of symptoms and sign as 'pseudo-Duane retraction syndrome' in 1976 [2]. This condition is called by others as inverse-Duane syndrome [3] because abduction of the affected eye is possible to some extent and the globe retraction occurs on abduction accompanied by narrowing of the palpebral fissure presenting the opposite features as those of classic Duane syndrome. Inverse-Duane retraction syndrome has been reported as being caused by acquired or congenital factors that affect the medial rectus [3,4].
In this article, we present a case of pseudo-Duane retraction syndrome secondary to orbital trauma without entrapment of the medial rectus, which ocular motility is characteristic to classic-Duane rather than inverse-Duane.
Case Report
A 30-year-old man came to our clinic complaining motility limitation in the left eye. He had left direct orbital trauma due to car accident 8 years ago. The motility disorder was onset 6 months later after the accident. Before the trauma, the patient had normal ocular motility. The patient had scar tissue on the left upper eyelid and temporal side.
His visual acuity was 20/20 in each eye. He had compensatory face turn to the right to eliminate diplopia (Figure 1). The patient had diplopia on left and right gaze.
Ophthalmologic examination showed marked limited adduction and abduction in his left eye. There was widening of the palpebral fissure in abduction (Figure 1). On attempted adduction of the left eye, globe retraction accompanied by narrowing of the palpebral fissure and up-shoot were observed (Figure 1). Globe retraction may be related to disruption of the connective tissue, pulleys, extraocular muscles and orbital hematoma. He showed left exotropia (XT) of 15 prism diopters (PD) in primary position. Enophthalmos was not noted in his left eye. Forced duction tests under topical anesthesia were negative. Orbital computed tomography and magnetic resonance imaging scan were normal. With these findings our case more looks like type 3 Duane retraction syndrome. The patient was undecided about strabismus surgery.
.
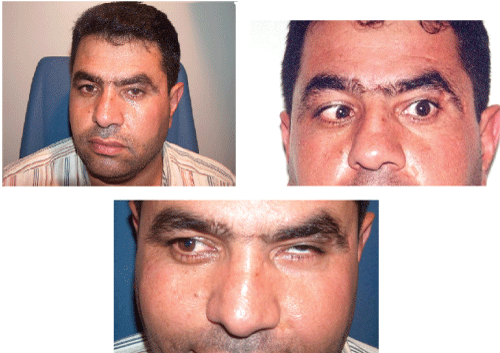
Figure 1: Compensatory face turn to the right. Left gaze shows the inability of the left eye to completely abduct. Right gaze shows globe retraction, upshot, and narrowing of the palpebral fissure in the left eye.
View Figure 1
Discussion
Duane retraction syndrome is a well-known congenital ocular motility disorder caused by anomalous innervation and mechanics of the lateral rectus muscle. Duane retraction syndrome, is thought to be due to a fibrosis of the lateral rectus with or without similar changes in the medial rectus leading to a cocontracture of the recti muscles. The co-contraction is innervational. Inverse-Duane retraction syndrome is most often due to trauma of the medial wall ethmoidal sinuses with entrapment of the medial rectus extending through the fractured lamina papyracea [5]. Classic Duane retraction syndrome usually presents from birth with an abnormal eye movement, inverse-Duane syndrome usually occurs after a trauma with diplopia.
All horizontal gaze movements may be limited in both types. In inverse-Duane syndrome, the globe retraction occurs on abduction accompanied by narrowing of the palpebral fissure. But, in our patient, the globe retraction occurred on adduction accompanied by narrowing of the palpebral fissure as those of classic Duane retraction syndrome.
Roentgenograms show abnormalities in the size and position of the extraocular muscles in classic Duane retraction syndrome, but medial wall fracture and air in orbita can be seen in inverse-Duane syndrome. In our case, all radiologic imaging were normal. The patient's ocular motor impairment was concluded to have arose from posttraumatic orbital changes and was diagnosed as pseudo-Duane retraction syndrome. Our case is the first of which we are aware to document posttraumatic pseudo-Duane retraction syndrome apparently due to abnormal innervation.
In conclusion, pseudo-Duane retraction syndrome may occur secondary to trauma without entrapment of the medial rectus muscle.
References
-
DeRespinis PA, Caputo AR, Wagner RS, Guo S (1993) Duane's retraction syndrome. Surv Ophthalmol 38: 257-288.
-
Duane TD, Schatz NJ, Caputo AR (1976) Pseudo-Duane's retraction syndrome. Trans Am Ophthalmol Soc 74: 122-132.
-
Lee SH, Lee JH, Lee SY, Kim SY (2009) A case of pseudo-Duane's retraction syndrome with old medial orbital wall fracture. Korean J Ophthalmol 23: 329-331.
-
Khan AO (2007) Bilateral inverse globe retraction (Duane's) syndrome. Indian J Ophthalmol 15: 205-208.
-
Gittinger JW Jr, Hughes JP, Suran EL (1986) Medial orbital wall blow-out fracture producing an acquired retraction syndrome. J Clin Neuroophthalmol 6: 153-156.





