International Journal of Pathology and Clinical Research
Glutamate Concentrations in Plasma and CSF in Patients with Glioma and Meningioma
George Dimogerontas1, Alexia Polissidis1, Petros Karkalousos2, Epameinondas Konstantinidis3, Zeta Papadopoulou-Daifoti1 and Charis Liapi1*
1Department of Pharmacology, Medical School, National & Kapodistrian University of Athens, Micras Asias 75, Goudi, Athens, Greece
2Department of Clinical Chemistry, Technological & Educational Institute of Athens, St. Spyridon, Aigaleo, Athens, Greece
3Neurosurgical Department of "Asclepeion” General Hospital of Voula, King Paul1, Voula, Athens, Greece
*Corresponding author:
Charis Liapi, MD, PhD, Endocrinologist, Associate Professor of Pharmacology, Medical School, National and Kapodistrian University of Athens, Greece, Tel: 00 30 210 7462504; Fax: 00302107462554; E-mail: cliapi@med.uoa.gr
Int J Pathol Clin Res, IJPCR-2-023, (Volume 2, Issue 1), Research Article; ISSN: 2469-5807
Received: December 02, 2015 | Accepted: February 04, 2016 | Published: February 07, 2016
Citation: Dimogerontas G, Polissidis A, Karkalousos P, Konstantinidis E, Papadopoulou-Daifoti Z, et al. (2016) Glutamate Concentrations in Plasma and CSF in Patients with Glioma and Meningioma. Int J Pathol Clin Res 2:023. 10.23937/2469-5807/1510023
Copyright: © 2016 Dimogerontas G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objectives: Glioma, a malignant intra-axial brain tumor, can release glutamate that facilitates tumor expansion, stimulates tumor-cell proliferation and motility and promotes epileptic activity. Glutamate acid is the major excitatory neurotransmitter in the mammalian Central Nervous System. We explore correlations of glutamate concentrations in blood and cerebrospinal fluid in patients with glioma in comparison to patients with meningioma which is the most common benign cerebral tumor.
Experimental design: Samples from 16 patients with glioma and 13 patients with meningioma were analyzed. Glutamate levels in blood and cerebrospinal fluid were measured by HPLC method.
Principal observations: Mean value ± SD of Glu concentration in CSF of patients with glioma was 64.2 ± 18.7 μΜ while the same value in serum was 103.0 ± 16.6 μΜ. In patients with meningioma, mean Glu concentration in CSF was 22.4 ± 7.12 μΜ while the same concentration in serum was 78.5 ± 11.4 μΜ. Biostatistical comparison of the two groups of patients revealed significant difference of Glu concentration in CSF compared to Glu concentration in serum but no significant difference was established between CSF concentrations of Glu in glioma and meningioma patients and between serum concentrations of Glu in the same group of patients as well.
Conclusion: Higher blood and CSF Glu concentrations are detected in glioma to meningioma patients. Statistical analysis showed significant difference between Glu concentrations in plasma and CSF in both glioma (p value = 0.01105) and meningioma patients (p value = 0.0012).
The invasive nature of gliomas, enhanced by Glu release, is one of the most important limitations to an effective treatment. CSF or plasma Glu concentrations might consist an easy and cheap biologic marker for tumor expansion, progression and response to therapeutic management.
Keyword
Brain neoplasms, Glioma, Glutamic acid, Meningioma, Glutamate
Introduction
Gliomas originate from glial cells or their progenitors and include astrocytomas, oligodendrogliomas and ependymomas; they comprise 32% of all primary brain tumors with two thirds of them being of high-grade. According to WHO low grade gliomas (grade I-II) are of benign histopathological characteristics while high grade gliomas (grade III-IV) are highly malignant tumors including anaplastic astrocytoma (grade III), glioblastoma multiform (GBM) (grade IV) and the diffuse-intrinsic pons glioma [1]. Glioblastoma the most common type of malignant glioma, accounts for about 17% of all primary cerebral tumors [1,2]. Gliomas are always growing intra-axially and are associated with high incidence of seizures [3].
On the other hand, meningioma is the most common primary, usually slow-growing, brain tumor in adults [4] (approximately 30%) [5] with a female predominance. The vast majority of meningiomas are benign (97.7%) and according to WHO, they are classified into three grades: grade I (typical or classic or benign meningiomas), grade II (atypical meningiomas) accounting for 5-15% and grade III (malignant or anaplastic or sarcomatous meningiomas) accounting for 1-3% of meningiomas [2,6]. Since these tumors are almost always growing extra-axially without invasion of brain parenchyma, they are not so frequently associated with automatic epileptic activity (21.6-39%) [7] as gliomas do [8].
Glutamate (Glu), a nonessential amino acid, is the most abundant free one in the mammalian brain where it is playing the role of the major excitatory neurotransmitter [9]. It is normally restricted to the synaptic and perisynaptic space of glutamatergic synapses where under normal conditions, is released by presynaptic neurons or even by glial cells [10] and mainly removed by astrocytes. In a healthy brain homeostasis keeps glutamate levels stable at harmless micromolar concentrations [11,12]. When brain homeostasis is disturbed the high Glu concentrations, cause excitotoxic death of the exposed neurons leading to irreversible neurological deficits. Furthermore, increased CSF glutamate levels have been linked to regulation of proliferation, differentiation and survival of several neuronal tumors, including medulloblastoma and high grade glioma [13,14].
Unfortunately the huge amount of evidences for the role of Glu in brain tumors mostly refer to animal studies or cultured cell lines [15-17] and despite the considerable body of in vitro experience clinical studies regarding Glu levels either in blood or cerebrospinal fluid (CSF) are very limited .
The aim of the present study was to determine Glu concentrations in blood and CSF in patients with glioma, a malignant and epileptogenic cerebral tumor and in patients with meningioma, a benign and less epileptogenic tumor and establish possible correlations.
Patients and methods
Patients
Twenty nine patients, 16 patients with glioma and 13 patients with meningioma, were included in the study. All patients (11 men and 18 women) were admitted at the Neurosurgery Department of a State Hospital, during four consecutive years and underwent craniotomy and brain tumor resection. The patients participated in the study after informed consent (Table 1).
![]()
Table 1: Demographic characteristics of study population.
View Table 1
Data about demographic (age, gender etc.) and clinical characteristics (seizures, time of operation from first symptom, survival etc.) of study participants were recorded (Table 1 and Table 2). Tumor volume was calculated from cerebral MRI. Grade and Ki67 labeling index were obtained from pathology reports.
![]()
Table 2: Statistical analysis of demographic characteristics of study population.
View Table 2
Twenty six out of twenty nine cases (3 patients were lost) were followed up for a period of at least one year as follows: ten out of eleven grade I meningiomas, both cases of atypical meningiomas and one case with grade II astrocytoma (grade 2), all three cases of anaplastic astrocytomas (grade 3) and ten out of twelve cases of grade 4 astrocytomas (GBM) (Table 3).
![]()
Table 3: Follow up ratios and mortality of tumour subgroups at the end of first post-operative year.
View Table 3
The study protocol was approved by the Research Ethics Committee of "Asclepeion" General Hospital, Voula, Athens, Greece.
Methods
Glu concentrations were measured in peripheral blood samples of 15 glioma and 13 meningioma patients as well as in CSF samples of 6 glioma and 7 meningioma patients by using High-Performance Liquid Chromatography (HPLC). All subjects abstained from tobacco, coffee and alcohol for at least 12 hours prior to blood sampling.
Sample preparation
Blood (2.5 cc) was obtained by venous puncture and collected in glass anticoagulated tubes with EDTA, immediately before the operation; it was centrifuged at 3000 g for 15 minutes and the supernatant was conserved at -80°C until it was processed.
CSF was obtained by direct aspiration from the operation field or through external lumbar drainage, which was preoperatively placed when a tight parenchyma was expected. CSF was centrifuged at 2000 g for 10 minutes and the supernatant was stored at -80°C until it was processed for the assessment of Glu levels [18].
Plasma and CSF samples were deproteinized with 3% sulfosalicylic acid (SSA = 1.5 g/50 ml dd H2O) by adding 50 μl of plasma to 450 μl SSA solution and leaved for 30 minutes at 4°C. Then they were centrifuged for 30 minutes at 9500 g and supernatants were stored at -80°C until the analysis.
High-performance liquid chromatography (HPLC) analysis
Following deproteinization of the samples, Glu concentrations were measured by HPLC, using specific software (Chromatography Station for Windows; Data Apex, Prague, Czech Republic), as described previously, [19,20] with minor modifications. The detection limit of HPLC was 0.05 μΜ. The mobile phase consisted of 5% acetonitrile (Merck, Darmstadt, Germany) - 0.1M phosphate buffer (Na2HPO4∙2H2O 8.8995 g/500 ml), pH 4.9-5.1, containing 50 μM EDTA (9.305 mg/500 ml). The sensitivity of the assay was tested for each series of samples, using external standards. Standard reactions were prepared as follows. Before analysis, samples were diluted with dd H2O 1:5 (40 μl plasma + 160 μl dd H2O) and 40 μl of sample (standard solution or sample) was added to 1-ml Eppendorf tubes along with 40 μl of 0.1M Borax buffer (Sigma-Aldrich, St. Louis, MO), pH 9.6, and 2 μl of the derivitizing reagent OPA (ortho-phthaldialdehyde; Sigma-Aldrich) and left at room temperature to react for 10 minutes. Final values were expressed in micromoles per liter (μmol/L or μΜ).
Ki67 (MIB-1) labeling index
The Ki67 labeling index was calculated as a percentage of labeled nuclei per 1000 cells. One thousand tumor cells were counted in several areas of tissue where positively stained nuclei were evenly distributed. In cases with uneven distribution of positive nuclei, the tumor cells were counted in the areas with highest density of positive nuclei by visual analysis [21].
Statistical analysis
Since the values of each variable were not many, non-parametrical statistical methods were used. Specifically, for each comparison of two different groups, the Mann-Whitney test was used and for each comparison of more than two different groups the Kruskal-Wallis test. For the statistical analysis and the majority of the diagrams the statistical packages S.P.S.S. and Minitab were used (academic licenses). For some diagrams we used MS Excel. Values are presented as the mean ± SD or mean ± SE; P values less than 0.05 were considered significant.
Results
Mean age of the 16 patients with glioma was 65.06 ± 9.38 years; (age range 39 to 74 years) and of the 13 patients with meningioma was 65.69 ± 8.29 years (age range 49 to 79 years). Eleven cases (38%) were in males, while eighteen (62%) were in females (Table 2).
Glioblastoma multiform (WHO Grade IV) was the most common histologic type (12 cases; 75%) of glial neoplasms followed by anaplastic glioma (3 cases; 18.75%) (WHO Grade III). Meningotheliomatous meningioma (WHO Grade I) was the most common histologic type (8 cases; 61.53%) of meningeal neoplasms.
At the end of the first post-operative year only sixteen of the twenty six patients (61.53%) were alive as follows (respective mortality as percentage): eight out of ten patients with grade I meningioma (20%), one out of two patients with atypical meningioma (50%), the single patient with grade II astrocytoma (0%), two out of three cases with anaplastic astrocytoma (33.3%) and four out of ten cases with GBM (60%) (Figure 1). Mortality rate at the end of first post-operative year is shown at Table 3. Of the fourteen glioma suffering patients in whom follow up was available, ten suffered from GBM (71.4 %) and of the twelve meningioma suffering patients in whom follow up was available, 10 had a benign meningioma (WHO Grade I) (83.3%).
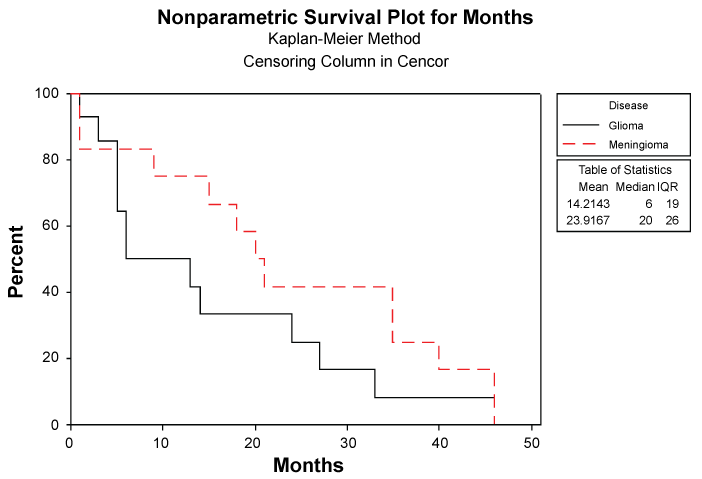
.
Figure 1: Nonparametric Survival Plot for patients suffering from Glioma and Meningioma showing that only 50% and 75% of them, respectively, survived at the end of first postoperative year.
View Figure 1
Mean value ± SE of Glu concentrations in CSF of patients with glioma was 64.2 ± 18.7 μΜ while in plasma it was 103.0 ± 16.6 μΜ. In patients with meningioma, mean ± SE Glu concentrations in CSF was 22.4 ± 7.12 μΜ while in plasma was 78.5 ± 11.4 μΜ (Table 4). Comparison between Glu concentrations in plasma and CSF either in patients with glioma or in patients with meningioma, using Mann-Whitney t-test, revealed a statistical significant difference between them (p value a/b = 0.01105, and p value c/d= 0.0012 for gliomas and meningiomas respectively) (Table 4 and Figure 2).
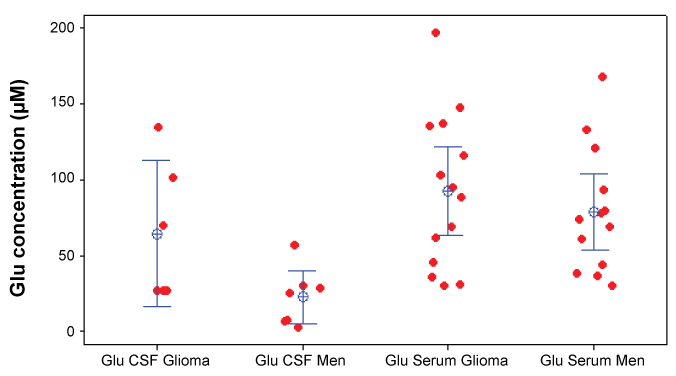
.
Figure 2: Dot plot of Glutamate concentrations in blood and CSF for patients with Glioma and Meningioma.
View Figure 2
![]()
Table 4: Mean values ± SE of Glu concentration in blood and CSF in patients suffer from cerebral glioma (A) or meningioma (B). Values are expressed in μΜ. Comparison made using Mann-Whitney t-test. Statistical significance between the groups is as follows: A: Serum Glu and CSF Glu (p value a/b = 0.01105, B: Serum Glu and CSF Glu( p value: c/d = 0.0012).
View Table 4
Mean Glu CSF or blood concentrations in patients with glioma compared to patients with meningioma, using the non-parametric Mann-Whitney t-test, revealed no significant difference in none of the compared groups (p value = 0.9431 and p value = 0.3334 for CSF and blood respectively) (Table 5 and Table 6).
![]()
Table 5: Mean values ± SE of Glu concentration in blood and CSF in patients suffer from cerebral glioma (A) or meningioma (B). Values are expressed in μΜ. Comparison made using Mann-Whitney t-test. Statistical significance between the groups is as follows: A: Serum Glu and CSF Glu (p value a/b = 0.01105, B: Serum Glu and CSF Glu( p value: c/d = 0.0012).
View Table 5
![]()
Table 6: Subgroups of patients with brain tumours and the corresponding Glu concentrations in peripheral blood. Values are expressed in μΜ.
View Table 6
We also seek if there was any correlation between Glu levels either in blood or CSF in the various subgroups, using Mann-Whitney t-test or 1-Single Wilcoxon test, but no statistical significant relationships was found except for the subgroups of patients with meningioma with and without epileptic spasms, in which paradoxically mean Glu concentrations in plasma were significantly higher in those without spasms (p value = 0.025 < 0.05) (Table 6) and in the subgroup of glioma patients with mass effect, that had Glu blood levels significantly higher than in the subgroup with no mass effect (p value = 0.0253 < 0.05) (Table 6).
Detailed survival analysis between GBM patients revealed that patients with Glu blood concentration below 40 μΜ survived over the first post-operative year in a statistical significant manner (p = 0.0188) in contrast to those with Glu blood concentration over 40 μΜ, although two patients with very high Glu blood concentration (mean ± SD= 149.7 ± 65.87 mM accomplished to survive over twelve months) but in a non-significant manner (p = 0.4492) when compared with those patients who didn’t accomplish it (mean ± SD = 91.83 ± 35.95 μΜ). In patients with grade I meningioma with Glu blood concentration between 70 μΜ and 130 μΜ (mean ± SD = 87.65 ± 21.79) survived less than two years in a statistical significant manner (p = 0.0197) in contrast to those with Glu blood concentration below 70 μΜ (mean ± SD = 44.96 ± 16.63) or over 130 μΜ (150 ± 25.01) who survived over two years.
No correlation between Glu CSF concentration and survival either in glioma neither in meningioma patients was established.
Discussion
In the present study Glu levels in blood and CSF were studied by HPLC in patients with a common brain tumor (glioma or meningioma). We demonstrated higher blood and CSF Glu concentrations in glioma than in meningioma patients. A plethora of evidences in the literature indicate the tight correlations between gliomas and Glu [22-24] while such a relation of Glu with benign cerebral tumors in humans has not been confirmed. Glutamate, under physiological conditions at micromolar concentration, is of great importance for the homeostasis in the brain extracellular fluids and crucial for the proper physiological functioning of the brain, a fact accomplished through the protective mechanisms of Na+-dependent, excitatory amino acid transporters [(EAATs): EAAT1= glial glutamate/aspartate amino acid transporter or GLAST, EAAT2 = glutamate transporter-1 or GLT-1 and EAAT 3] [11].
In gliomas, Glu can be produced and released from their cells facilitating their expansion by destroying the surrounding brain tissue [16], by stimulating tumor-cell proliferation and motility in an autocrine or paracrine manner and by promoting epileptic activity from surrounding neuronal cells [25]. Over 50% of Glu produced by glioma cell lines has been found to be released as an obligatory byproduct of the xc-specific transporter [16,26], a transporter that mediates the exchange of intracellular Glu for extracellular cystine which is required by glioma cells for glutathione-based protection against reactive oxygen radicals [27]. Such a transporter has not been identified in meningiomas. Although the role of Glu as signal mediator in neuronal tumors, such as glioma [22-24], is well known, in the last decade evidence has emerged about the involvement of Glu in non-neuronal tumors [27] such as colorectal cancer [28], gastric cancer [29], oral squamous cell carcinoma [30], prostate cancer [31], melanoma [32], osteosarcoma [33] suggesting a more complex role of glutamate than simply the death of the exposed neurons and the entailing irreversible neurological deficits.
Blood Glu concentrations (μΜ) both in patients with glioma or meningioma, were significantly higher compared to CSF concentrations (3.5 times higher in meningioma patients and 1.6 times higher in glioma patients). Several studies have tried to establish the physiological glutamate levels either in plasma or in CSF [34-37] but the considerable variability noted was probably due, among others, to the methodology used. The two compartments, blood/plasma and CSF, are in equilibrium with the blood-brain barrier at the interface, regulating exchanges of several constituents but correlations of Glu concentrations in blood and CSF in cerebral tumor patients lack. Since in neurological disorders the blood-brain barrier can be damaged, implying alterations of the physiologic crosstalk between central and peripheral tissues [38,39]; the increased CSF glutamate levels are probably due to glial and neuronal cell necrosis. Although it is difficult to determine the exact source of plasma glutamate, based on the ratio between Glu plasma and CSF levels, it can be postulated that plasma levels derive, at least partially, from the brain through the damaged blood-brain barrier. The relationship between glutamate release from glioma tissue and its clearance dynamics into and from the CSF is not fully elucidated according to our knowledge.
Although theoretically, malignant tumors ought to produce Glu in massive amounts in contrast to benign tumors, brain Glu concentrations in glioma patients remain controversial; some of the studies report elevated Glu in peritumoral brain [40] others report unchanged or even lower in the tumor [41]. Two studies in which microdialysis probes were placed into the brain of ambulatory patients allowing a continuous sampling of extracellular Glu showed elevated Glu concentrations [42,43]. In another study Glu concentrations were in excess of 100 μM at the tumor margin in all nine patients examined; yet, neither non-malignant brain tumor nor acute brain trauma have shown sustained elevation in Glu [43]. In our study, CSF Glu levels were approximately 3 times higher in glioma patients compared to meningioma ones while plasma Glu concentrations showed a smaller difference. However, the interpretation of our results must be carefully evaluated since we could not study the profile of CSF glutamate levels at repeated intervals (due to ethical reasons).
Stratification of both groups of patients according to age, sex, grade of tumor, tumor volume, mean time of operation from first symptom appearance and postoperative survival did not reveal any significant correlation between these subgroups, in accordance to other studies. Although Glu is an epileptogenic neurotransmitter, unexpectedly, mean concentrations of Glu in the plasma of non epileptic patients with meningioma were significantly higher than the corresponding concentrations in epileptic patients, but the underlying pathophysiologic mechanisms of tumor related seizures is more complex, involving: different structural changes (such as neuronal loss in the CA1 and CA3a/b regions of hippocampus as in mesial temporal sclerosis) [44], biochemical (like pH) changes in peritumoral brain tissue [45], decreased extracellular [Mg2+] [46], and increased peritumoral extracellular [Fe3+] [47] and histologic alterations (such as increased expression of connexin (CX) 43 protein in surrounding of brain tumor tissue etc.) [48,49]. This phenomenon must be studied in depth.
Ki67, a non-histone protein, expressed in the proliferative phase of the cell cycle, is the most widely used immunohistochemical marker to measure cell proliferation (the net growth rate of a tumor is a balance between cell proliferation and apoptosis); Ki67 labeling index (LI) correlates well with increasing histological grade of meningiomas [50,51] and gliomas [52,53], poor prognosis of higher grades, reduced interval of recurrence [54,55] and decreased survival [56]. A cut off value of 4.2 for Ki67 has been suggested as indicative of high tumor proliferation activity and as a predictor of meningiomas recurrence [57]. Glu concentrations in plasma and CSF didn’t differ significantly between glioma patients with Ki67 over or less than 15%.
In accordance with the literature, Ki67 LI was statistically different between groups of grade I and grade II meningiomas, but Glu concentrations in plasma and CSF didn’t differ significantly in any subgroup of these patients either with Ki67 < 5% or Ki67 > 5%.
Our findings strongly suggest that Glu release has to be considered a common attribute of malignant gliomas and important in considering the various ways in which Glu affects the tumor biology. The determination of Glu signaling is feasible by functional imaging techniques or by microdialysis, but these techniques are invasive and expensive, limitating the large scale applicability of these methods [58]. Thus we strongly believe that CSF, or even better, plasma concentrations of Glu might consist an easy and cheap biologic marker indicating the role of excitotoxicity in CNS tumor expansion and their progression or their response to therapeutic management; several studies have shown that Glu receptor antagonists [15,59,60] and silencing of selected receptor subunits [61] inhibit proliferation of cancer cells [62,63] while potent blockers of the xc- system such as sulfasalazine and (S)-4-carboxyphenylglycine [64] can inhibit the autocrine/paracrine signal which promotes glioma cell invasion [65,66]. In our study the individual variability in glutamate values does not permit to clearly identify a cut-off value of diagnostic or prognostic usefulness thus larger studies are needed.
Disclosure
No conflict of interest
Acknowledgement
This study was supported by a scholarship of "Stella Tsaga - Letta Despotidou" Foundation.
References
-
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, et al. (2007) The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 114: 97-109.
-
Central Brain Tumor Registry of the United States (2010) CBTRUS Statistical Report: Primary Brain and Central Nervous System Tumors Diagnosed in the United States in 2004-2006. Central Brain Tumor Registry of the United States.
-
Drappatz J, Norden AD, Wen PY (2009) Therapeutic strategies for inhibiting invasion in glioblastoma. Expert Rev Neurother 9: 519-534.
-
Ryken TC, Chamberlain M (2012) Update on Meningioma: Neurosurgeon and Medical Neuro-oncologist Perspective.
-
Claus EB, Bondy ML, Schildkraut JM, Wiemels JL, Wrensch M, et al. (2005) Epidemiology of intracranial meningioma. Neurosurgery 57: 1088-1095.
-
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, et al. (2007) The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 114: 97-109.
-
Groff RA (1935) The Meningioma as a Cause of Epilepsy. Ann Surg 101: 167-175.
-
Cushing H (1932) Intracranial Tumors, Baltimore, USA, C. C. Thomas Publisher.
-
Brocke KS, Staufner C, Luksch H, Geiger KD, Stepulak A, et al. (2010) Glutamate receptors in pediatric tumors of the central nervous system. Cancer Biol Ther 9: 455-468.
-
Kimura T, Ohkubo M, Igarashi H et al. (2007) Increase in glutamate as a sensitive indicator of extracellular matrix integrity in peritumoral edema: a 3.0-tesla proton magnetic resonance spectroscopy study. J Neurosurg 106: 609-613.
-
Beart PM, O'Shea RD (2007) Transporters for L-glutamate: an update on their molecular pharmacology and pathological involvement. Br J Pharmacol 150: 5-17.
-
Danbolt NC (2001) Glutamate uptake. Prog Neurobiol 65: 1-105.
-
Olney JW, Ho OL, Rhee V (1971) Cytotoxic effects of acidic and sulphur containing amino acids on the infant mouse central nervous system. Exp Brain Res 14: 61-76.
-
Tan S, Schubert D, Maher P (2001) Oxytosis: A novel form of programmed cell death. Curr Top Med Chem 1: 497-506.
-
Ishiuchi S, Tsuzuki K, Yoshida Y, Yamada N, Hagimura N, et al. (2002) Blockage of Ca(2+)-permeable AMPA receptors suppresses migration and induces apoptosis in human glioblastoma cells. Nat Med 8: 971-978.
-
Takano T, Lin JH, Arcuino G, Gao Q, Yang J, et al. (2001) Glutamate release promotes growth of malignant gliomas. Nat Med 7: 1010-1015.
-
Stepulak A, Luksch H, Gebhardt C, Uckermann O, Marzahn J, et al. (2009) Expression of glutamate receptor subunits in human cancers. Histochem Cell Biol 132: 435-445.
-
Zhang H, Zhai SD, Li YM, et al. (2003) Effect of different sample pretreatment methods on the concentrations of excitatory amino acids in cerebrospinal fluid determined by high-performance liquid chromatography. J Chromatogr B Analyt Technol Biomed Life Sci 784: 131-135.
-
Bongiovanni R, Yamamoto BK, Jaskiw GE (2001) Improved method for the measurement of large neutral amino acids in biological matrices. J Chromatogr B Biomed Sci Appl 754: 369-376.
-
Le Boucher J, Charret C, Coudray-Lucas C, Giboudeau J, Cynober L (1997) Amino acid determination in biological fluids by automated ion-exchange chromatography: performance of Hitachi L-8500A. Clin Chem 43: 1421-1428.
-
Ralte AM, Sharma MC, Karak AK, Mehta VS, Sarkar C (2001) Clinicopathological features, MIB-1 labeling index and apoptotic index in recurrent astrocytic tumors. Pathol Oncol Res 7: 267-278.
-
Seeburg PH (1993) The TINS/TiPS Lecture. The molecular biology of mammalian glutamate receptor channels. Trends Neurosci 16: 359-365.
-
Hollmann M, Heinemann S (1994) Cloned glutamate receptors. Annu Rev Neurosci 17: 31-108.
-
Ozawa S, Kamiya H, Tsuzuki K (1998) Glutamate receptors in the mammalian central nervous system. Prog Neurobiol 54: 581-618.
-
Aronica E, Yankava B, Jansen GH, et al. (2001) Ionotropic and metabotropic glutamate receptor protein expression in glioneuronal tumours from patients with intractable epilepsy. Neuropathol Appl Neurobiol 27: 223-237.
-
Ye ZC, Sontheimer H (1999) Glioma cells release excitotoxic concentrations of glutamate. Cancer Res 59: 4383-4391.
-
Chung WJ, Lyons SA, Nelson GM, Hamza H, Gladson CL, et al. (2005) Inhibition of cystine uptake disrupts the growth of primary brain tumors. J Neurosci 25: 7101-7110.
-
Chang HJ, Yoo BC, Lim SB, Jeong SY, Kim WH, et al. (2005) Metabotropic glutamate receptor 4 expression in colorectal carcinoma and its prognostic significance. Clin Cancer Res 11: 3288-3295.
-
Liu JW, Kim MS, Nagpal J, Yamashita K, Poeta L, et al. (2007) Quantitative hypermethylation of NMDAR2B in human gastric cancer. Int J Cancer 121: 1994-2000.
-
Park SY, Lee SA, Han IH, Yoo BC, Lee SH, et al. (2007) Clinical significance of metabotropic glutamate receptor 5 expression in oral squamous cell carcinoma. Oncol Rep 17: 81-87.
-
Abdul M, Hoosein N (2005) N-methyl-D-aspartate receptor in human prostate cancer. J Membr Biol 205: 125-128.
-
Marín YE, Chen S (2004) Involvement of metabotropic glutamate receptor , a G protein coupled receptor, in melanoma development. J Mol Med (Berl) 82: 735-749.
-
Kalariti N, Pissimissis N, Koutsilieris M (2005) The glutamatergic system outside the CNS and in cancer biology. Expert Opin Investig Drugs 14: 1487-1496.
-
Ferraro TN, Hare TA (1985) Free and conjugated amino acids in human CSF: influence of age and sex. Brain Res 338: 53-60.
-
Yuan HB, Cheng LY, Yin F, Zhang GX, Peng J, et al. (2008) [Levels of amino acids in cerebral spinal fluid in children with cerebral palsy]. Zhongguo Dang Dai Er Ke Za Zhi 10: 475-477.
-
Mutani R Monaco F, Durelli L et al. (1975) Levels of free amino acids in serum and cerebrospinal fluid after administration of taurine to epileptic and normal subjects. Epilepsia 16: 765-769.
-
Ferrarese C, Aliprandi A, Tremolizzo L, Stanzani L, De Micheli A, et al. (2001) Increased glutamate in CSF and plasma of patients with HIV dementia. Neurology 57: 671-675.
-
Broman T (1964) Blood-brain barrier damage in multiple sclerosis supravital test-observations. Acta Neurol Scand Suppl 40: SUPPL 10:21-24.
-
Ginsbourg M, Foncin JF, Le Beau J (1970) [Studies on the blood-brain barrier with a fluorescent tracer in human brain edema]. C R Seances Soc Biol Fil 164: 2443-2446.
-
Fan G, Sun B, Wu Z, Guo Q, Guo Y (2004) In vivo single-voxel proton MR spectroscopy in the differentiation of high-grade gliomas and solitary metastases. Clin Radiol 59: 77-85.
-
Harris LM, Davies NP, Macpherson L, Lateef S, Natarajan K, et al. (2008) Magnetic resonance spectroscopy in the assessment of pilocytic astrocytomas. Eur J Cancer 44: 2640-2647.
-
Roslin M, Henriksson R, Bergström P, Ungerstedt U, Bergenheim AT (2003) Baseline levels of glucose metabolites, glutamate and glycerol in malignant glioma assessed by stereotactic microdialysis. J Neurooncol 61: 151-160.
-
Marcus HJ, Carpenter KL, Price SJ, et al. (2010) In vivo assessment of high-grade glioma biochemistry using microdialysis: a study of energy-related molecules, growth factors and cytokines. J Neurooncol 97: 11-23.
-
Kim JH, Guimaraes PO, Shen MY, Masukawa LM, Spencer DD (1990) Hippocampal neuronal density in temporal lobe epilepsy with and without gliomas. Acta Neuropathol 80: 41-45.
-
Ransom BR (2000) Glial modulation of neural excitability mediated by extracellular pH: a hypothesis revisited. Prog Brain Res 125: 217-228.
-
Avoli M, Drapeau C, Louvel J, Pumain R, Olivier A, et al. (1991) Epileptiform activity induced by low extracellular magnesium in the human cortex maintained in vitro. Ann Neurol 30: 589-596.
-
Singh R, Pathak DN (1990) Lipid peroxidation and glutathione peroxidase, glutathione reductase, superoxide dismutase, catalase, and glucose-6-phosphate dehydrogenase activities in FeCl3-induced epileptogenic foci in the rat brain. Epilepsia 31: 15-26.
-
Aronica E, Gorter JA, Jansen GH, Leenstra S, Yankaya B, et al. (2001) Expression of connexin 43 and connexin 32 gap-junction proteins in epilepsy-associated brain tumors and in the perilesional epileptic cortex. Acta Neuropathol 101: 449-459.
-
Schaller B, Ruegg SJ (2003) Brain Tumor and Seizures: Pathophysiology and Its Implications for Treatment Revisited. Epilepsia 44: 1223-1232.
-
Carvalho LH, Smirnov I, Baia GS, Modrusan Z, Smith JS, et al. (2007) Molecular signatures define two main classes of meningiomas. Mol Cancer 6: 64.
-
Ragel B, Jensen RL (2003) New approaches for the treatment of refractory meningiomas. Cancer Control 10: 148-158.
-
Johannessen AL, Torp SH (2006) The clinical value of Ki-67/MIB-1 labeling index in human astrocytomas. Pathol Oncol Res 12: 143-147.
-
Arshad H, Ahmad Z, Hasan SH (2010) Gliomas: correlation of histologic grade, Ki67 and p53 expression with patient survival. Asian Pac J Cancer Prev 11: 1637-1640.
-
Brat DJ, Parisi JE, Kleinschmidt-DeMasters BK, Yachnis AT, Montine TJ, et al. (2008) Surgical neuropathology update: a review of changes introduced by the WHO classification of tumours of the central nervous system, 4th edition. Arch Pathol Lab Med 132: 993-1007.
-
Kleinhues P, Cavence WK (2000) World health organization classification of tumors. Pathology & genetics. Tumors of the nervous system. IARC Press Lyon.
-
Jaros E, Perry RH, Adam L, Kelly PJ, Crawford PJ, et al. (1992) Prognostic implications of p53 protein, epidermal growth factor receptor, and Ki-67 labelling in brain tumours. Br J Cancer 66: 373-385.
-
Ho DM, Hsu CY, Ting LT, Chiang H (2002) Histopathology and MIB-1 labeling index predicted recurrence of meningiomas: a proposal of diagnostic criteria for patients with atypical meningioma. Cancer 94: 1538-1547.
-
Tremolizzo L, Beretta S, Ferrarese C (2004) Peripheral markers of glutamatergic dysfunction in neurological diseases: focus on ex vivo tools. Crit Rev Neurobiol 16: 141-146.
-
Nicoletti F, Arcella A, Iacovelli L, Battaglia G, Giangaspero F, et al. (2007) Metabotropic glutamate receptors: new targets for the control of tumor growth? Trends Pharmacol Sci 28: 206-213.
-
Rzeski W, Turski L, Ikonomidou C (2001) Glutamate antagonists limit tumor growth. Proc Natl Acad Sci U S A 98: 6372-6377.
-
de Groot JF, Piao Y, Lu L, Fuller GN, Yung WK (2008) Knockdown of GluR1 expression by RNA interference inhibits glioma proliferation. J Neurooncol 88: 121-133.
-
Arcella A, Carpinelli G, Battaglia G, D'Onofrio M, Santoro F, et al. (2005) Pharmacological blockade of group II metabotropic glutamate receptors reduces the growth of glioma cells in vivo. Neuro Oncol 7: 236-245.
-
Stepulak A, Luksch H, Gebhardt C, Uckermann O, Marzahn J, et al. (2009) Expression of glutamate receptor subunits in human cancers. Histochem Cell Biol 132: 435-445.
-
Lyons SA, Chung WJ, Weaver AK, Ogunrinu T, Sontheimer H (2007) Autocrine glutamate signaling promotes glioma cell invasion. Cancer Res 67: 9463-9471.
-
Lo M, Wang YZ, Gout PW (2008) The x(c)- cystine/glutamate antiporter: a potential target for therapy of cancer and other diseases. J Cell Physiol 215: 593-602.
-
Sontheimer H (2008) A role for glutamate in growth and invasion of primary brain tumors. J Neurochem 105: 287-295.





