International Journal of Pathology and Clinical Research
Severe Complication of POPS: Mesh Malposition in the Bladder
Sabine Kersting1*, Dirk Kusche2, Klaus-PeterJung1 and Eugen Berg1
1Department of Coloproctology, Prosper-Hospital, Recklinghausen, Germany
2Department of Urology, Prosper-Hospital, Recklinghausen, Germany
*Corresponding author:
Sabine Kersting, Department of Coloproctology, Prosper-Hospital, Mühlenstr. 27, 45659 Recklinghausen, Germany, Tel: +492361542750, Fax: +492361542756, E-mail: sabine@drkersting.de
Int J Pathol Clin Res, IJPCR-2-035, (Volume 2, Issue 2), Case Report; ISSN: 2469-5807
Received: March 16, 2016 | Accepted: April 28, 2016 | Published: April 30, 2016
Citation: Kersting S, Kusche D, Klaus-Peter J, Berg E (2016) Severe Complication of POPS: Mesh Malposition in the Bladder. Int J Pathol Clin Res 2:035. 10.23937/2469-5807/1510035
Copyright: © 2016 Kersting S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The authors present a case of a 68-years-old woman suffering of persistent urinary tract infections accompanied by intermittent fever. She had a history of pelvic organ prolapse suspension (POPS) for descending perineal syndrome with rectal prolapse, carried out elsewhere 15 months ago. Cystoscopy revealed a part of the prolene mesh that was incrusted along the fundus of the bladder to be the source of symptoms. This is probably the first case that presents acomplication of POPS, which is a relative new surgical technique that gains more and more widespread use. At present no data exist about long-term results and complications. Although POPS is a minimally invasive procedure our case report shows that the risk of serious complications has to be taken in mind.
Keywords
Rectal prolapse, POPS, Mesh, Bladder injury
Introduction
Pelvic organ prolapse (POP) is a common and distressing condition. It is seen in 40% to 60% of parous women [1-3]. The etiology of POP is multifactorial and complex [3]. A descent of the pelvic organs (uterus, vagina, bladder or bowel) occurs when there is a weakness in the supporting structures of the pelvic floor. Vaginal childbirth and hysterectomy are the major accepted initializing factors [4]. A woman can present with prolapse of one or more of these organs. A variety of urinary, bowel and sexual symptoms may be associated. In cases of POP, different surgical approaches have been proposed and accepted. Traditionally, pelvic floor problems have been addressed through abdominal, vaginal or perineal approaches. Over the past decade, more and more minimally invasive procedures have been reported and refined. Pelvic organ prolapse suspension (POPS) is one of the newest surgical techniques that have been introduced for prolapse repair. This laparoscopic procedure is propagated by Antonio Longo (known for implementation of stapled haemorrhoidopexy in 1998 [5]) and increasingly applied in Europe during the past 3 years. As laxity of vaginal support results in protrusion of the pelvic organs, the goal of POPS is to re-suspend the vagina and associated pelvic organs through key-hole incisions. The vagina and pelvic organs are re-suspended internally with a supportive mesh. Pneumoperitoneum is established and a V-shaped mesh (25 cm length) is introduced into the abdominal cavity and fixed on the anterior vaginal vault or on the vaginal apex if the patient had hysterectomy. Nearby the right anterior superior iliac spine an incision is made. Here a clamp is inserted and under laparoscopic vision a subperitoneal tunnel to the anterior fornix of the vagina is generated. The right end of the V-shaped mesh is taken out through the subperitoneal tunnel. Starting from an incision in the vicinity of the left anterior superior iliac spine the same steps are performed to pull out the left end of the mesh. The mesh is fixed to both lateral fornices and pelvic organ suspension is achieved by making symmetrical tractions on both mesh strips. Then the mesh is fixed at the muscle's fascia close to the skin incisions nearby the right and left anterior superior iliac spines [6].
Due to the recent nature of laparoscopic POPS at the present time no much data is published about complications, outcome and long-term follow-up. We report herein a case of malposition of the mesh being detected in the bladder.
Case Report
A 68-years-old woman presented with persistent urinary tract infections accompanied by intermittent fever. She had a history of POPS for descending perineal syndrome with rectal prolapse, carried out elsewhere 15 months ago. The postoperative course after POPS was complicated. A bladder leakage was diagnosed and urine secretion was noticed on the second postoperative day via an intra-operatively placed intra-abdominal drainage. A retrograde cystrogram was performed and confirmed the bladder leakage. After a conservative treatment with transurethral catheterisation for 4 weeks the leakage had stopped and the catheter was removed. Due to persistent urinary tract infections many investigations were performed. However, ultrasound, magnetic resonance imaging, rectoscopy, cystourethrography, retrograde pyelography and colposcopy did not show any pathological evidence for the reason of the complaints. For further clinical examination the woman was admitted to our hospital. Cystoscopy was carried out and revealed a part of the prolene mesh that was incrusted along the fundus of the bladder to be the source of symptoms (Figure 1). The woman underwent surgery for removal of the mesh. Diagnostic laparotomy was performed and the bladder was incised at the dome. Over a distance of 3 cm the mesh was in grown into the mucosa of the posterior surface of the urinary bladder. After cutting out the mesh the defect was closed by double row suture technique. The postoperative course was without any complication. On the 7th postoperative day a cystourethrography was performed. An extravasation was excluded thus the intraoperatively inserted foley catheter was removed. The woman was released from hospital 8 days after the operation. At the follow-up clinical examination 4 weeks later she remained completely free of complaints and without any symptoms of urinary tract infection and without any recurrence of pelvic organ prolapse.
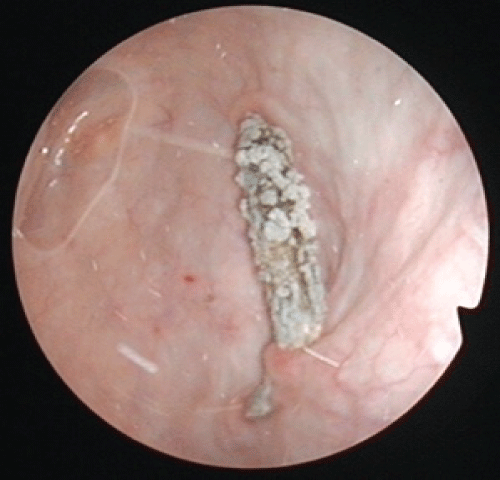
.
Figure 1: Cystoscopy revealed a part of the prolene mesh that was incrusted along the fundus of the bladder.
View Figure 1
Discussion
A review of the literature has shown, that POPS is a further development of the method of ventral vaginopexy first described by Williams and Richardson in 1952. Instead of mesh implantation, Williams and Richardson fixed the vagina with two extraperitoneally transmitted strips of the right and left oblique aponeurosis [7,8]. In 1967 Kapandji [9] proposed the suspension of the vagina by tense subperitoneal skin-strips from the anterior superior iliac spines to the vagina. The truly innovative aspect of POPS is the laparoscopic approach and the suspension of the vagina using a mesh that has the ability to provide adequate anatomical support.
Although POPS is increasingly applied, publications on POPS are scarce. To our knowledge there exist only two publications in peer reviewed journals. Both originate from the study group of Ceci et al. (University of Rome and A. Fiorini Hospital of Terracina [6,10]). They describe preliminary results of POPS in 54 respectively 73 patients. All patients underwent at the same time stapled transanal rectal resection (STARR) to correct the residual prolapse. Patients were evaluated after one year follow-up. The majority of patients presented with an important reduction of the pre-operative symptomatology. One year following POPS, in 76% of patients rectal prolapse and in 83% of patients rectocele was no longer detectable and no patient was incontinent for stool. The most frequent surgical complication was defecation urgency (18%) [6]. Further case studies and follow-up studies are not yet available.
This is probably the first case that presents a complication following POPS. 15 months after POPS the inserted mesh had been found incrusted in the bladder. Mesh erosion following female pelvic floor reconstructions has been extensively studied [11]. That is one of the reasons the Food and Drug Administration (FDA) refused the approval for meshes for transvaginal repair [12]. The danger for mesh erosion does not just only exist in ventral suspension but also in mesh implantation for obstructed defecation. A current example is ventral mesh rectopexy, another modern operating method for rectal prolapse and POP first described by D'Hoore et al. in 2004 [13]. This laparoscopic procedure has achieved widespread use and popularity over the past decade. However, mesh associated complications are frequently discussed, as there is a lack of strong evidence to support the routine use of mesh in pelvic floor reconstructive surgery (Level 3 evidence). Special attention should be paid to possible mesh related complications and long-term sequelae that could have a significant impact on quality of life [14].
Possible mesh related complications in POPS include infection, fistulas, perforation, chronic pelvic pain, dysuria, overactive bladder etc. However, in this case mesh erosion into the bladder appears unlikely. The bladder leakage arose directly after the operation followed by persistent urinary tract infections. This suggests an unrecognized bladder injury during the operation. It can be assumed that the clamp that was inserted under laparoscopic vision via a subperitoneal tunnel penetrated the bladder. Covered by peritoneum the malposition of the mesh probably did not become apparent during the operation. It took 15 months until the reason for the patient's complaints had been found. The operative removal of the mesh managed this unusual complication following POPS effectively.
This case report shows that even though POPS is a minimally invasive procedure potential pitfalls might possibly lead to severe complications. This is an argument for the carrying out of this procedure in specialized centers which have acquired expertise and experience in this surgical technique. In the case of postoperative bladder leakage the surgeon has to be sensitive and at an early stage possible bladder injury has to be taken in mind. In case the suspicion of bladder injury exists as soon as possible a cystourethrography and cystoscopy should be performed in order to avoid further complications. The risk of intraoperative damage of the bladder can be reduced by a preoperatively placed foley catheter.
Laparoscopic POPS is now an accepted surgical treatment for POP. Although POPS gains more and more widespread use, it remains a relatively new procedure and up to now it has been subject to limited research. The fact that at present there exist only publications of one study group makes an objective evaluation of this procedure impossible. The follow-up of patients is limited to 12 months. This means, that there is a lack of data about possible complications and long-term results. Further studies are necessary to assess the value of this technique and to reveal typical complications. In our view this case report let us acknowledge that the rapid implementation of POPS with such limited evidence is a cause of concern. In view of serious and possibly even life-threatening mesh related complications after the treatment of a benign disorder we argue for a certain scepticism and the well-considered implementation of meshes in rectal prolapse surgery.
References
-
Handa VL, Garrett E, Hendrix S, Gold E, Robbins J (2004) Progression and remission of pelvic organ prolapse: a longitudinal study of menopausal women. Am J Obstet Gynecol 190: 27-32.
-
Hendrix SL, Clark A, Nygaard I, Aragaki A, Barnabei V, et al. (2002) Pelvic organ prolapse in the Women's Health Initiative: gravity and gravidity. Am J Obstet Gynecol 186: 1160-1166.
-
Maher C, Feiner B, Baessler K, Schmid C (2013) Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 4: CD004014.
-
Bump RC, Norton PA (1998) Epidemiology and natural history of pelvic floor dysfunction. Obstet Gynecol Clin North Am 25: 723-746.
-
Longo A (1998) Treatment of haemorrhoidal disease by reduction of mucosa and haemorrhoidal prolapse with a circular suturing device: A new procedure. Proceedings of the 6th World Congress of Endoscopic Surgery, Rome, MonduzziEditore, Bologna: 777-784.
-
Ceci F, Spaziani E, Corelli S, Casciaro G, Martellucci A, et al. (2013) Technique and outcomes about a new laparoscopic procedure: the Pelvic Organ Prolapse Suspension (POPS). Il Giornale di chirurgia 34: 141-144.
-
Dickgiesser U, Ohlenroth G, Opitz V, Dickgiesser A (1983) The Williams-Richardson vaginopexy as a surgical therapy in vaginal inversion in vaginal stump prolapse. Geburtshilfe Frauenheilkd 43: 620-624.
-
Heidenreich W (1997) Williams-Richardson vaginopexy. An abdominal suspension operation in prolapse and extensive vaginal descent. Zentralbl Gynakol 119: 378-382.
-
Kapandji M (1967) Treatment of urogenital prolapse by colpo-isthmo-cystopexy with transverse strip and crossed, multiple layer, ligamento-peritoneal douglasorrhaphy. Annales de chirurgie 21: 321-328
-
Ceci F, Spaziani E, Casciaro G, Corelli S, Martellucci A, et al. (2013) Multiorgan female pelvic prolapse: pelvic organ prolapse suspension (P.O.P.S.) stapled transanalrectale resection (S.T.A.R.R.): new surgical tecniques and results. Annaliitaliani di chirurgia 84: 711-713.
-
Nazemi TM, Kobashi KC (2007) Complications of grafts used in female pelvic floor reconstruction: Mesh erosion and extrusion. Indian J Urol 23: 153-160.
-
Food and Drug Administration, HHS (2016) Obstetrical and Gynecological Devices; Reclassification of Surgical Mesh for Transvaginal Pelvic Organ Prolapse Repair; Final order. Fed Regist 81: 353-361.
-
D'Hoore A, Cadoni R, Penninckx F (2004) Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg 91: 1500-1505.
-
Lundby L, Laurberg S (2015) Laparoscopic ventral mesh rectopexy for obstructed defaecation syndrome: time for a critical appraisal. Colorectal Dis 17: 102-103.





