International Journal of Psychology and Psychoanalysis
Psychological Progress in Schizophrenic Patients undergoing Psychoanalytic Psychotherapy
Gillian Steggles*
Department of Centre for Psychoanalytic Studies, University of Essex, UK
*Corresponding author:
Gillian Steggles, Department of Centre for Psychoanalytic Studies, University of Essex, 54 Temple Avenue, Whetstone, London, UK, E-mail: gill.steggles@btopenworld.com
Int J Psychol Psychoanal, IJPP-2-012, (Volume 2, Issue 1), Review Article
Received: November 09, 2015: Accepted: May 16, 2016: Published: May 18, 2016
Citation: Steggles G (2016) Psychological Progress in Schizophrenic Patients undergoing Psychoanalytic Psychotherapy. Int J Psychol Psychoanal 2:012.
Copyright: © 2016 Steggles G. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Psychoanalytic psychotherapy uses psychoanalytic principles in delivering psychotherapy which supports patients as well as informing them about themselves and the external world through psychoanalytic interpretations. Undergoing a psychoanalysis can be very stressful, and requires ego strength that allows assimilation of personal knowledge by the patient and its utilization within the personality. Classical psychoanalysis makes heavy demands on the analysand's, or patient's, stamina, and schizophrenic patients are not equipped to utilize it. However, with sufficient support they can be helped to undergo a psychoanalysis that applies the technique of psychoanalytic psychotherapy.
Jonathan Shedler, in his paper The Efficacy of Psychodynamic Psychotherapy, makes the case very clearly for the valuable therapeutic scope of psychodynamic, or psychoanalytic, psychotherapy [1]. He collects together the evidence for this and presents the ways in which it's strongly beneficial effects promote health in patients of different kinds, including those suffering from depression, anxiety, panic, somatoform disorders, eating disorders, substance-related disorders and personality disorders. He writes that 7 features reliably distinguish psychodynamic therapy from other therapies. These 7 features largely determine the illnesses that can be helped by it, although schizophrenia and schizoaffective disorder are not included in his analysis of the technique. The 7 features include a focus on affect and expression of emotion, exploration of attempts to avoid distressing thoughts and feelings, identification of recurring themes and patterns, discussion of past experience, focus on interpersonal relations and on the therapy relationship, and exploration of fantasy life. Shedler demonstrates that the effect sizes of psychodynamic therapy compare very favourably with all other psychological therapies and with antidepressant medication, and ventures to assert that several other psychological treatment techniques utilize without acknowledgement the benefits of psychodynamic techniques; indeed he suggests that the efficacy of these other psychological treatments such as CBT are as effective as they are because of the loan they have taken from psychodynamic ideas.
There is, however, a distinguished history of the application of psychoanalytic psychotherapy for schizophrenia. Each author contributed to theoretical concepts, mooted psychoanalytical mechanisms underlying symptoms, and to clinical practice. Freud originally held that the narcissism of schizophrenic patients prevented them from being able usefully to relate to the analyst and so develop the therapeutic relationship of transference with him or her. For this reason, Freud believed that schizophrenic patients could not be treated with psychoanalysis. Melanie Klein, however, discovered that both positive and negative transference could be established with them [2]. Three of her distinguished students, Wilfred Bion, Herbert Rosenfeld and Hanna Segal went on to work with schizophrenic patients, and each of them made their own contributions to the field. Bion believed that, ignoring the effects of the external environment, the schizophrenic personality depends on four factors: (i) a conflict that is never resolved between life and death instincts (ii) a preponderance of destructive impulses (iii) hatred of external and internal reality and (iv) a tenuous but tenacious object relationship [3]. If the psychoanalyst bears these features in mind he may understand better how to tackle the relationship difficulty in the consulting room. Bion also believed that psychotic patients possess a non-psychotic component of their personality [4] which offers hope to the therapist in accessing parts of the patient which, if modified, could lead to their decreased subjection to psychosis. Melanie Klein identified the importance of projective identification in the schizophrenic mind, that is, casting out one's bad feelings into another person and sometimes trying to control this person. Bion continued this idea. As he wrote, "Projective identification of conscious awareness and the associated inchoation of verbal thought is the central factor in the differentiation of the psychotic from the non-psychotic personality" [3]. Rosenfeld worked with narcissistic patients, and came to believe that there are two forms of narcissism, destructive and libidinal narcissism [5]. He also believed that there are several types of projective identification, for example one form is used for communication, one tries to unburden the self of unwanted parts, and another tries to control the analyst's body [6]. Hanna Segal differed from Rosenfeld's views on narcissism, believing that only destructive narcissism exists [7], but she agreed with him that projective identification can be used by schizophrenic patients to evacuate unwanted parts of the self into other people [8].
More recently, Richard Lucas devised the concept of "The Psychotic Wavelength", where the therapist has to bring himself into the patient's arena of thinking by conceptualizing concretely [9]. Marcus Evans has also written about this clinical technique of working with psychotic patients [10]. Leslie Sohn accepted that psychotic patients have a non-psychotic part of their mind [11], and opined that a mental state examination should be performed every five minutes when giving psychotherapy to a schizophrenic patient to check for psychotic elements that may be currently operating. Murray Jackson has strongly upheld the application of psychoanalytic principles to the treatment of mental illness including schizophrenia, and understood how it should be applied. For example, he recognised that therapy for severely disturbed patients should always be planned on a long term basis [12].
All Psychiatrists, and many Psychoanalysts working with psychotic patients, accept the unassailable place of medication in their treatment and management. Invaluable in the early stabilization of patients when they newly arrive in a psychiatric ward, but only given when the patient has been listened to and talked to as much as possible to gain knowledge about their individual mental state, medications then control psychotic symptoms to a greater or lesser extent. Full benefit from them may only become apparent after several weeks' use. Their correct use is to help the patient to tolerate their mental life, dealing with hallucinations and delusions as far as possible and freeing up the non-psychotic part of the patients mind into becoming accessible for the therapist to relate to, usefully. The therapist becomes able to uncover more underlying aspects of the patient's mind by gentle probing and a tactful approach when speaking with the patient once the psychotic symptoms no longer interfere with communication. The therapist may discover useful aspects of the patient's thinking that can be used in their treatment programme, especially if the patient regards them favourably. The patient's personality may blossom when the symptoms are controlled, if they live within a loving family or, more usually, the patient may continue to suffer psychologically from the causative psychogenic factors in their life. But their requirement for medication is almost always long term. Non-compliance is unfortunately quite common, and if persistent then injections are usually resorted to therapeutically in place of pills.
As mentioned above, strictly applied psychoanalysis is too stringent and stressful for a schizophrenic or schizoaffective patient to be able to benefit from it. It requires a much stronger sense of self or ego functions than a schizophrenic patient possesses. A schizophrenic patient would probably be unable to understand their role in a classical psychoanalysis. Equally, supportive psychotherapy would not be exploratory or intensive enough to effect the changes at a deep level sometimes sought by a schizophrenic patient. Fundamental self-scrutiny and discovery generally only result from analytic therapy, but this can, indeed, be performed and bring healing even in schizophrenic patients. Whether or not a particular patient does seek radical healing has to be determined from what is known about them in their earlier history, their background in studies and work, and their expressed views while mentally ill but calm. Psychoanalytic psychotherapy is both supportive and analytical, and therefore in capable hands has the potential to resolve the patient's mental pathology while supporting them psychologically.
Michael Robbins, in Massachusetts, USA, has developed a psychoanalytic psychotherapy technique for treating schizophrenic patients. The patients he has treated all conform to the DSM-III-R symptom classification of schizophrenia, most often paranoid schizophrenia, and their ages range from late teens to their twenties. His personal portfolio of 18 patients, together with other patients, is an excellent example of pioneering work, which he has written up in his book "Experiences of Schizophrenia" and many papers, and in which he provides rich details of his clinical findings, views and conclusions [13]. His lifetime's work relates his successes as well as those of his cases that did not succeed in alleviating the patient's distress. He looks objectively at the possible reasons that might account for the failures, and has been able to describe half of his patients, 9 out of 18, as having had "positive outcomes", 6 of these being "very successful". A further patient's therapy has been written up in his paper "The successful psychoanalytic therapy of a schizophrenic woman" [14]. He is a trained Psychiatrist and Psychoanalyst, and has been able to gain understanding of schizophrenia and schizophrenic patients at a deep level. He adheres to a hierarchical understanding of the illness that involves molecular biology, neurobiology, neurochemistry, psychoanalysis, interpersonal psychology, family systems, sociology and cultural anthropology. Like almost every clinician who works with schizophrenia, he acknowledges the place of medication in the treatment of his patients, who have been based at the Maclean Hospital in Massachusetts while they received psychoanalytic treatment from him in his consulting room. In his book he expresses intense gratitude to the staff there for their management of his patients, as is the case for most therapeutic clinicians who work with very mentally ill individuals who require hospitalization while receiving their treatment.
One of his remarkable results has been that he has been able to stage the progress in treatment of all of the patients whom he has treated, a sequence of 7 Stages (Table 1). All of his patients follow this process, even if they were not able to complete their therapy. His approach has been to deliver psychoanalytic psychotherapy to all his patients, and to observe how they have progressed in his care. He writes of the healing power of love, and with this ethos has nurtured all of his patients as far as they were able to proceed in treatment with him. The full therapy process involves two major phases; initially the patient is very ill and can only relate to him from their unhealthy, schizophrenic perspective. Then comes a particularly difficult period from the patient’s perspective, which can also affect the analyst, and can lead to premature termination through therapeutic stalemate. After this the patient goes through the second phase, that of relating more normally to the analyst, in which phase the Stages of the process lead to therapeutic termination.
![]()
Table 1: Stages in the psychological resolution of schizophrenia.
View Table 1
When the patient enters therapy they are invariably severely afflicted mentally. They have been unable to develop normally, whatever their individual experiences have been, and their minds are unhealthily distorted so that they have become unable to function properly where they have found themselves trying to live. As a result, they find interaction with others very difficult indeed, and experience great if not impossible difficulty in asserting themselves as they would like to in order to overcome the frustrations of one situation after another. Relating to their analyst is no exception. Apart from the anxiety that this unusual situation causes them, where they are, and where they experience being under the scrutiny of a professional person, they generally suffer acute difficulty in comprehension and emotional pain at some level during their clinical interactions. Dr Robbins describes this relationship, in Stage 1, as "Protopathosymbiosis" or "parasitism". The patient contributes little to the relationship, being completely dependent upon the analyst for steering it along therapeutic lines. The patient's identity is invested in her psychotic state and she is incapable of helping herself very much at this Stage. That she has turned up, and continues to turn up daily at her analyst's consulting room is as much as she can do for herself. She has been selected for therapy because of previous evidence of stamina and achievement in her earlier life, but now she has disintegrated due to circumstance, and all of what is still healthy in her psyche, her non-psychotic mind, strains to co-operate with the analyst to move forward psychologically.
Due to her efforts, she may succeed in engaging with the analyst. If she has given him a chance by listening to him and drawing some benefit from his words, she may develop for herself some lifelines of emotional security, good humour, tolerance, appreciation of his interest in her and absorb some of his tenacity for continuing with her sessions. However, her sense of her individuality is threatened, because he may be saying things to her with which she disagrees but has to continue to listen to. This is hard for her. She may feel that some of her loyalties are threatened, but that she can do nothing about this, even apparently in her own self-defence. Most patients in this Stage, Stage 2, continue to assert their own, schizophrenic and ill, perspective, consequently finding the sessions irksome and annoying, frustrating and sometimes miserable. She has become used to her own false assumptions, biased opinions, unrealistic expectations and possibly questionable family values. But the analyst must continue to assert reality to her. It is essential that if she is to become well she must renounce every part of the false world within which she has been living. She is probably unaware at the commencement of her treatment of just how distorted her schizophrenic thinking is. It is the distorted views, biased perspectives and egregious interpretations of reality which together largely underpin her schizophrenia or schizoaffective disorder, compounded by emotional difficulties, and probable slight brain dysfunction affecting her reward centres, executive function and cognition. It is extremely taxing for her to attend her analyst, return to hospital for ward care, and return to her analyst the next day, 4 or 5 days every week for years between short breaks for holidays. Her perspective on the world is extremely bleak, and she may at a deep level be extremely miserable. The hospital staff must be alert at all times on a continuous suicide watch, for her as for all their other patients. This is the main reason why patient selection for this treatment has to be so cautious, and why care by the hospital unit must be so effectively secure. Schizophrenia and schizoaffective disorder are life-threatening conditions, but this therapy can lower the suicide threshold for intervals of time during phases of growth in the treatment, and the hospital staff cannot always know, within their daily routines, exactly when these times are occurring. Kindness and firmness are probably the nursing techniques that are most effective in sustaining patient morale, within the consistent environment and ambience of security.
This relationship between the patient and her analyst, where the patient is very ill and trying to hang on to her sessions while feeling confused and misunderstood, except on the few occasions when her analyst says something to her which she understands clearly, and can accept without feeling threatened, is termed by Dr Robbins as "Pathosymbiosis". It spells difficulty for the patient, as outlined above. But it can also present particular difficulties for the analyst. It may be tempting for him to collude with the patient. For whatever reason, possibly flattery by a weaker individual, or enjoyment of the patient's dependence upon him, or a sense of power over her, the analyst may unconsciously wish and enact that the treatment continues on an indefinite, interminable path. This is very rare, but the analyst should be aware of its possibility in himself with each of his patients, as it will definitely interfere with the patient's progress and may prevent her otherwise expected recovery. The analyst is responsible for avoiding collusion because the patient can do nothing about it. She turns up for treatment, and the analyst must guide the treatment process towards its intended conclusion. If he does not avoid collusion, therapeutic stalemate ensues, and consequent premature termination of therapy. This is Stage 3 of Dr Robbins' 7 Stages of psychoanalytic psychotherapy for schizophrenic patients.
Stage 4 is also a difficult hurdle for the patient to overcome. Here she must succeed in relinquishing the views, attitudes, assumptions and some of the beliefs that she held when her treatment began. As explained above, it is these aspects of her mind that her family may have inculcated into her as a family member, and which hold her in her schizophrenic mindset. If there has really been a very serious problem for her in her family, such as molestation or another form of difficulty or abuse, these aspects of her mindset will probably have developed in her because of the ways she has tried to overcome the pain and trauma of what happened to her in the family. So from a process of generalization, most of her mind is related to this trauma in the family, eg: all her family relationships have developed awry due to misunderstandings and objections and despair. Consequently, to alleviate herself of her schizophrenia she has to reject all of this pathology and turn her back on all the ideas that her family use and which trapped her in her pathogenic situation within which she had no room or scope to flex her mind constructively. She has to construct her whole life again, ignoring the influence of her family. This can be very hard for her, because if there was otherwise a lot of love in the family, or from a good parent, as well as with her siblings, what in effect she has to do is to throw her family out with the bathwater, ie. her illness. If she is especially vulnerable, or quite young, or unable to assert herself adequately, she may not be able to achieve all this. The success of her therapy depends as much on her resilience and determination as on all the other factors that have been mentioned, never forgetting patient security. Disengagement from her false, family-influenced self, and engaging fully with her analyst on his terms of full and comprehensive reality-testing and psychic strength may coincide with her determination to be well and to live her own active and productive life. Early on in her treatment she may scarcely be aware of some of these factors, but trust and belief in goodness can help her persevere, despite sometimes feeling this is against the odds. As always, the enduring kindness of her analyst and kind hospital staff help on a daily basis to maintain her morale and feed into her own systems of survival and optimism.
Stage 5 of Dr Robbins' therapeutic process consists of more normal symbiosis, in which the patient now appreciates normality in what the analyst says to her in his interpretations, and its realism. She becomes ever better able to apply what he says to her in her life during the 23 hours around her therapeutic hour with him. This Stage is growth-promoting, and now she may find that she begins to flourish somewhat in her other relationships besides her therapeutic relationship. It is gratifying for her to experience happiness in these, and to be able to organize her life now seen in a positive light rather than as utterly without light at all, when she floundered in darkness and misery. The despair felt by schizophrenic patients cannot be overestimated, and it is brave hospital staff as well as psychoanalysts who work daily to sustain the hope and wellbeing of schizophrenic patients on their wards and in the community. Schizophrenia is an illness where absolutely nothing seems to fit with anything else, and it is experienced like this because the patient's separate, individual experiences over their lifetime are not internally consistent. Part of themselves gets left behind during one experience, and another part of themselves gets left behind during another experience. They lose track of who they are because when addressed by another person they have responded while something else lay heavily on their mind so that they were unable to absorb the full meaning of what was said to them. Then, assumptions are made by the other person that are beyond what the schizophrenic patient can work out. Misunderstandings of this kind recur time after time for the patient, who feels like the loneliest person in the world, understood by no-one they know, which in a young person is commonly their entire family. This terrible situation is addressed by the psychoanalyst, who makes themselves available to struggling and terrified patients such as these. By now the patient has learned what it is about themselves that needs rectification, they have rectified some of this, and in Stage 5 they continue to put it into practice.
In Stage 6, the patient has achieved psychic differentiation, so that they have developed some of their own healthy attitudes to important aspects of their lives eg. in their relations with other people, ethical values, and principles of living that will be relevant to their future in the communities around them. They have also integrated, so that all of their outward looking and inward looking perspectives, their feelings for other people and parts of their environments, and their daily experiences have become confluent with each other, and this seamlessness within themselves gives the patient confidence in themselves as a person they understand. They are not, now, afflicted with self-doubt in the way that prior to treatment they suffered repeatedly. By Stage 7, the patient's mind is self-sufficient and independent, and they are able to leave treatment after a therapeutic termination.
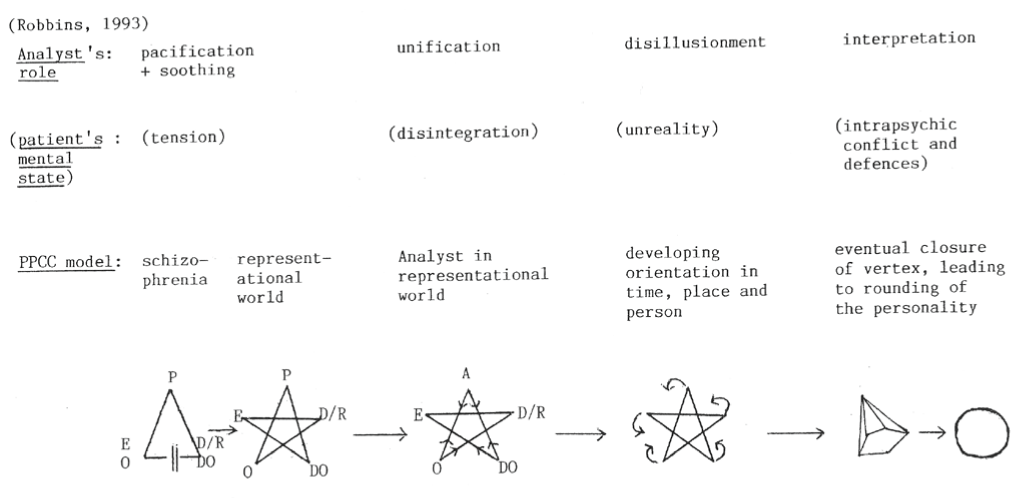
The PPCC Theory [15] is a psychoanalytic theory of the functional psychoses that illustrates the progress of a schizophrenic or schizoaffective patient treated with psychoanalytic psychotherapy into mental health. It provides evidence from a schizoaffective patient of how the patient's mind changes in psychoanalytic psychotherapy [15]. The PPCC Theory uses shapes to represent features of the schizoaffective mind as it changes, for example when the analyst is internalized by the patient; when the patient becomes able to endorse and encapsulate calmly the totality of their psychotic experiences lived through in the past, orientated healthily in time, place and person; and when their mind loses its sharp or disorganized edges and becomes a mature, rounded personality (Figure 1). These changes were documented in the schizoaffective patient studied by Dr Steggles [15].
.
Figure 1: The overall changes in the schizophrenic patient’s mind through therapy.
View Figure 1
The PPCC Theory was developed from a case study of an individual schizoaffective patient who identified, through a small study of her own mind, her Representational World [16]. This is a mental representation within the mind of particular features of the external world around a person that have been significant for him or her, as his or her life progressed. The representational world starts to be formed in children, and is modified as the person grows older. In this schizoaffective patient, 29 features of her representational world emerged from her mind, in 5 groups. Names were given to these 5 groupings, as variables, 24 years before identical variables were quoted in the Shorter Oxford Textbook of Psychiatry [17] as providing data during psychoanalytic treatment upon which psychoanalytic theories mainly depend. The PPCC model of the schizophrenic or schizoaffective mind in therapy illustrates the patient's progress in the form of geometric shapes, so that the overall changes in the mind can be appreciated visually, thus making the therapeutic process perhaps more accessible to understanding for those not familiar with psychological processes.
Table 1 sets out parallel Stages between Dr Robbins' Stages and the PPCC's steps towards recovery. In Stage 1 the patient is assailed by the inadequacies of her representational world, within which she has not found it possible to thrive normally. In Stage 2 she has managed to include the analyst in her representational world in an influential position, so she has agreed to let him address her with a view to helping her out of her illness. Stage 3 illustrates her "blocked" psychology, where the non-psychotic or sane part of her mind cannot access the psychotic part of her mind and she cannot interact optimally with her analyst. Therapeutic stalemate may ensue if she cannot use her sane mind to overcome this schizophrenic "block" and concentrate on what her analyst is saying to her, take it in and apply it to her own mentality. It may be that this is only a temporary phase, in which case the analyst may visit her in hospital and tend her until she recovers and can continue with her treatment. If it is not a temporary phase and the analyst is unable to intervene successfully into her thinking to bring about a healthier state of mind, then after several months he may have to decide that a premature termination of therapy is appropriate for her. This is very sad for all concerned. However, it is usually the case that even a short experience of psychoanalytic therapy can be helpful in the long term, so the therapy may by no means necessarily be regarded as a waste of either the patient's or the analyst's time. And Stages 4 to 7 describe the parallel processes between Dr Robbins' Stages and the PPCC model's changes that the successful patients undergo when proceeding towards their ultimately achieved good mental health.
The patient's therapy (Table 1) has two main phases. In the first phase, up to Stage 3, the patient's mind remains affected by schizophrenic thinking but they nonetheless continue to relate in this way to their analyst. The second phase is where the patient's schizophrenic thinking is challenged. Stage 3 represents a therapeutic watershed where they either are able to adopt the reality suggested and emphasized by their analyst, or they are unable to do this and remain indefinitely within their familiar, pathological world. Stages 1 and 2 are introductory for the patient, testing their loyalty to the treatment process when they cannot fully understand the nature or content of the analyst's words. Stage 4 is the treatment's greatest challenge for the patient: having faced the difficulties of Stage 3 where they address the falsity of their own schizophrenic mind, in Stage 4 they have to actively reject all their previous pathological mental tendencies and try hard to accept and adopt the direction of thinking promoted by their analyst. This is very difficult for the patient; it necessitates an act of faith, a leap into the unknown, for them, although being accompanied for the duration of the treatment by their analyst. Stages 5 to 7 represent the patient's therapeutic progress in a learning process, from accepting the veracity of what their analyst says to them, to becoming enabled to think along these healthier lines for themselves. Once they are capable of thinking healthily for themselves they become enabled to terminate their treatment therapeutically with their analyst.
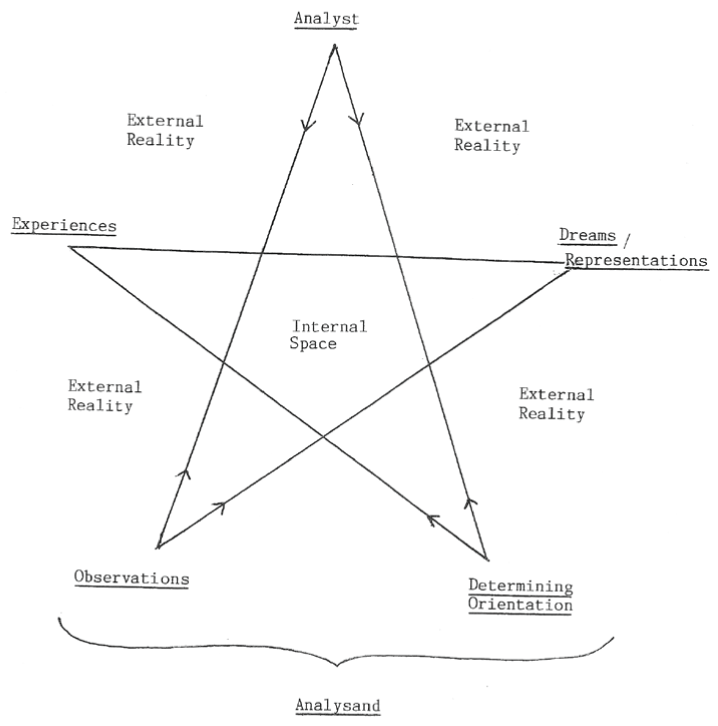
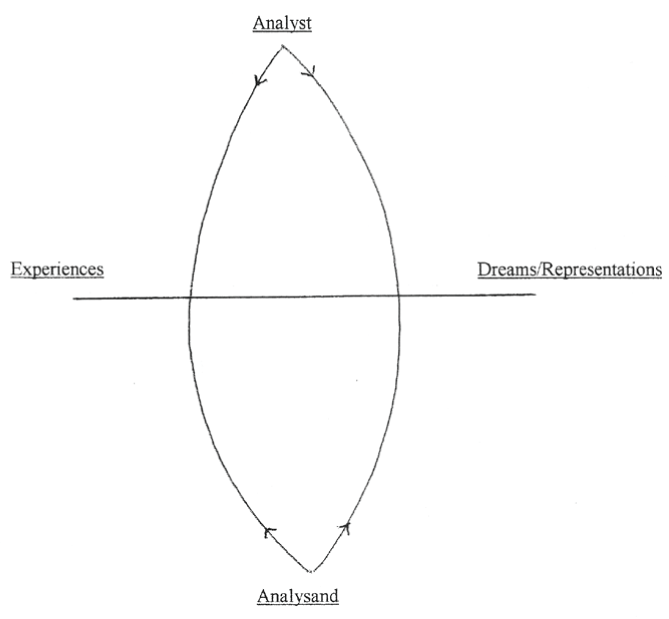
The PPCC Theory describes changes in the patient's mind from her being lost in her unhelpful representational world to becoming a smoothly-functioning, independent individual. The diagrams illustrate the lines of communication between the analyst and the patient, with arrows indicating the initial directions of flow. The paranoid-schizoid position (Figure 2) demonstrates the restricted movement possible between the active non-psychotic part of the analysand's mind, Observations, and the active psychotic part, the Determining Orientation. The Experiences and the Dreams/Representations variables are more established, long term variables, including as they do past Experiences and past Dreams and Representations. When the patient has done much more therapy they may become able to manifest the depressive position (Figure 3) where, instead of splitting people or objects into all-good or all-bad categories in their own mind, they are able to feel remorse for perhaps having hurt them, and want to make reparations towards helping the other person into feeling better.
The PPCC model illustrates graphically the overall progress of a schizophrenic or schizoaffective patient in psychoanalytic psychotherapy. From the unhelpful representational world, the analyst becomes incorporated into it, rendering it a constructive and actively helpful agency. A great amount of work needs to be done in treatment to help the patient interact with reality rather than with the strange idiosyncrasies of her family's psychological arena. Several years can be spent on this phase alone. Eventually, the patient becomes able to look back upon her past life with all its unhappy and unpleasant experiences and her own unhelpful responses which made bad situations worse, in such a way that all the people and events from the past can be related to positively and constructively. She can forgive all the people involved, and herself, and re-internalize them innocuously so that they no longer can hurt her or make her psychotic. Medications may still be needed if the traumata were very severe, or if the patient is having difficulty containing all the emotional effects of them on herself. This is not a failure of treatment. Medications can be a blessing for a very disturbed patient, and most patients would agree that peace of mind in terms of no longer being confused, or feeling angry or bewildered or very sad is the most important part of recovering from mental illness. If this can be achieved then the therapy has been truly successful. Sometimes ongoing dependence on medication is viewed as a failure of therapy, but many Psychiatrists and some patients, and also Psychoanalysts if they have been psychiatrically trained, feel that psychological adjustment can of itself be its own reward.
When the patient has fully adjusted to her life, the vertex of the PPCC model closes (Figure 4). In achieving this phase, the patient encloses all of her life, difficulties and all, in her mind. All her life's events, and the people she has interacted with, are internalized in terms of Time, Place and Person. No longer can figures in her life make her psychotic or confused. This is real progress for her. The misunderstandings that her family members created in her no longer have this effect. It may be necessary for her not to expose herself to them, however, for fear of all the old influences re-establishing their effects on her; and this may be the case even if in the absence of these people in her family she can look after herself perfectly well. So she may have to leave her family behind, which may cause her much pain and sadness.
The final phase in the PPCC's description of the patient's progress is the emergence of a smooth, comfortably functioning sphere, where "all of the patient's rough corners have been rubbed off" (Figure 5). Here she does not feel unduly anxious or disturbed while living her life. Her successful overall progress can be described graphically by the PPCC model (Figure 1). Undoubtedly there will be some sequelae of having been psychotic, such as unpleasant memories or feelings. But the psychosis-generating effects of these mental features is now absent, because of the overall benefit of having been in her analyst's consulting room with him and remembering how kind, warm and cheerful he always was. This power of such intensive, prolonged human communication is something that not all kinds of psychological clinician may fully understand. Every Analysand who has received a successful analysis knows this power to have been what healed them. People with many different kinds of problems are accepted for a psychoanalysis. And all those who emerge from their problems are aware of their debt of gratitude to their Analyst. Health Service Governors and Funders need to be made aware of the transformative power of this form of talking treatment so that more people could be returned to the working economy, happy and well. The enthusiasm of people, including a number of schizophrenic patients, is what the working economy is based upon. Hard working people who require a heart transplant are admired when they have their heart transplant and return to work. In exactly the same way, schizophrenic patients who show intense desire to be well, try extremely hard to co-operate, and have demonstrated enormous effort in different ways in their past should be given their chance to live their life productively if that is what they choose to do. Human hope and determination should never be crushed or dismissed or overlooked. Possibly lack of knowledge or awareness is the reason why schizophrenic patients are not treated as intensively as they should be. Most clinical staff already work their absolute hardest, and mental health teams are grievously overstretched. But Dr Robbins' work demonstrates clearly that, if intelligently applied, there are ways in which a proportion of schizophrenic patients can be radically helped. What we need in Britain now is a feasibility and viability study and a pilot study to replicate Dr Robbins' work. If successful, we could establish a National Health Schedule for schizophrenic patients in which all schizophrenic patients would receive the form of treatment most appropriate to their needs.
Both Dr. Robbins and Dr. Steggles found that psychoanalytic psychotherapy helpfully permitted the schizophrenic difficulties of their patients to be addressed in such a way as to promote learning, self-reflection and insight. This process was never smooth or without setbacks, and progress was never rapid, but through mutual trust, effort and shared loyalty the patients who remained committed to their treatment with Dr Robbins had a nearly 1 in 2 chance of emerging from their schizophrenic illness. Six of Dr Robbins' series of 18 patients emerged "very successfully" into good health. Many different pitfalls were responsible for preventing 9 of the 18 patients from successfully resolving their illness, and 3 of the treatments were only moderately successful or incomplete. Difficulties encountered included repeated hospitalizations for chronic illness, lack of motivation, and inability to resolve a psychotic transference to Dr Robbins. Dr Steggles' patient successfully concluded her treatment despite a serious detrimental incident.
Schizophrenic patients' illness severely limits their thinking and ability to self-care effectively whilst in treatment. Cognitive functions including especially memory may be markedly adversely affected. Anger, rage and indignation was particularly found by Dr Robbins in the USA to be a salient feature in his patients at the time when in retrospect the true horrific reality of their earlier lives became evident to them. In the UK this reaction would probably be modulated as far as possible to sadness by the psychodynamic staff caring for the patient on their hospital ward. Blame is not helpful therapeutically to anyone, and tolerance, patience, forgiveness and generosity are emphatically striven for on psychodynamic wards in the UK. This promotes kinder acceptance of the past and smoother movement into a brighter future for the patient.
Successfully treated patients emerge into the fullness of life with a range of achievements including marriage, completion of a university course or coming off medication. They have developed autonomy and independence, and can rely upon themselves to an extent unattainable prior to their treatment. They no longer think as they did in their earlier situation within their family, where they could only react to the unpleasantness they experienced there. Becoming capable of healthier perceptions, they could now see the reality of their previous limitations pointed out to them by their analyst. This was what had given rise to their phases of rage and indignation around Stages 3 and 4. But in understanding their previous predicament they could recognise how far they had come, and could act on their sense of rightful self-esteem and self-respect in attaining the success they were fully entitled to in their lives.
The contents of this paper are reproduced with kind permission by BMJ Publishing Group Ltd from "The process of recovery of a schizoaffectively disordered mind: a psychoanalytic theory of the functional psychoses, the psychodynamic pentapointed cognitive construct theory" in BMJ Case Reports 2015, doi: 10.1136/bcr-2012-006683, Copyright BMJ 2015. Kind permission has been granted by Dr Michael Robbins for reference to his work herein.
References
-
Shedler J (2010) The efficacy of psychodynamic psychotherapy. Am Psychol 65: 98-109.
-
Melanie Klein (1952) The origins of transference. In: In Envy and Gratitude and Other Works (1946-1963) M. Klein (1984) p.53. The Hogarth Press and the Institute of Psychoanalysis: London.
-
Bion W (1984) Second Thoughts. Karnac London 38.
-
Bion W (1984) Second Thoughts. Karnac London 56.
-
Rosenfeld H (2009) A clinical approach to the psychoanalytic theory of the life and death instincts: an investigation into the aggressive aspects of narcissism. In Rosenfeld in Retrospect, Ed. J Steiner: 122. Routledge: New York.
-
Rosenfeld H (2009) Contribution to the psychopathology of psychotic states: the importance of projective identification in the ego structure and the object relations of the psychotic patient. In Rosenfeld in Retrospect, Ed. J Steiner: 134-135. pp.134-135. Routledge: New York.
-
Segal H (2009) Discussion of Ron Britton's paper. In Rosenfeld in Retrospect, Ed J Steiner: 35. Routledge: New York.
-
Segal H (1986) The Work of Hanna Segal: A Kleinian Approach to Clinical Practice: 12. Free Association Books, Maresfield Library: London.
-
Richard Lucas (2009) The Psychotic Wavelength. Routledge New York.
-
Evans M (2010) Tuning into the Psychotic Wavelength: Psychoanalytic supervision for mental health professionals. Psychoanalytic Psychotherapy 22: 248-261.
-
Sohn L (1999) Psychosis and violence. In Psychosis (madness) Ed. P. Williams: 15. Institute of Psychoanalysis: London.
-
Murray Jackson, Paul Williams (1994) Unimaginable Storms: A Search for Meaning in Psychosis. Karnac London.
-
Robbins M (1993) Experiences of Schizophrenia: An Integration of the Personal, Scientific and Therapeutic. The Guilford Press New York.
-
Robbins M (2012) The successful psychoanalytic therapy of a schizophrenic woman. Psychodynamic Psychiatry 40: 575-608.
-
Steggles G (2012) The process of recovery of a schizoaffectively disordered mind: a psychoanalytic theory of the functional psychoses, the psychodynamic pentapointed cognitive construct theory. BMJ Case Rep pii: bcr2012006683
-
Sandler J, Rosenblatt B (1962) The concept of the representational world. Psychoanal St Child 17:128-145.
-
Gelder M, Harrison P, Cowen P (2006) Shorter Oxford Textbook of Psychiatry (5) Oxford University Press: Oxford 89.