International Journal of Radiology and Imaging Technology
A Case of Spontaneous Bacterial Peritonitis after Radiofrequency Ablation of an Early Hepatocellular Carcinoma
Pierleone Lucatelli, Beatrice Sacconi*, Emanuele Arcangelo d'Adamo, Carlo Catalano and Mario Bezzi
Department of Radiological, University of Rome, Italy
*Corresponding author:
Beatrice Sacconi, Sapienza, Department of Radiological, Oncological and atomopathological Sciences, University of Rome, Viale Regina Elena 324, 00161, Rome, Italy, Tel: 39-06-44-55-602, Fax: 39-06-49-02-43, E-mail: beatrice.sacconi@fastwebnet.it
Int J Radiol Imaging Technol,
IJRIT-1-003, (Volume 1, Issue 1),
Case Report
Received: August 16, 2015: Accepted: September 12, 2015: Published: September 14, 2015
Citation: Lucatelli P, Sacconi B, d'Adamo AE, Catalano C, Bezzi M (2015) A Case of Spontaneous Bacterial Peritonitis after Radiofrequency Ablation of an Early Hepatocellular Carcinoma. Int J Radiol Imaging Technol 1:003
Copyright: © 2015 Lucatelli P. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Radiofrequency ablation (RFA) is frequently used to treat small hepatocellular carcinoma (HCC), with similar outcome to surgery [1-3]. The procedure is relatively safe, with low morbidity and mortality rates [4-6]. The most common major complications are both intra-hepatic (bleeding, abscess and biliary injury) and extra-hepatic (peritoneal bleeding, gastrointestinal perforation, pleural effusion) [7-9]. We report a successfully managed case of spontaneous bacterial peritonitis (SBP) after RFA of a left liver lobe HCC.
Keywords
Spontaneous bacterial peritonitis, SBP, Radiofrequency ablation, RFA, Carcinoma, HCC
Case Report
A 78 year-old woman was referred to our Department to undergo a radiofrequency ablation (RFA) of a 20 mm hepatocellular carcinoma (HCC) nodule located in the left lobe of the liver, in segment 3. She was affected by a hepatitis C virus-related cirrhosis (Child-Pugh A). She had a previous chemoembolization for HCC (segment 6) two years before, without any evidence of residual or recurrent tumor. No previous episodes of hepatic encephalopathy, spontaneous bacterial peritonitis or gastrointestinal bleeding were reported. The patients did not have ascites at the moment of the procedure.
RFA was performed in standard fashion under sterile conditions using a RFA system (AMICATM, HS Hospital Service, Aprilia, Italy); previous skin antisepsis was performed with iodine solution and a sterile field was prepared with sterile drapes. A LeVeen multiple tined needle (Boston Scientific Marlborough, MA, USA) was inserted under ultrasound (US) guidance and RF current was applied for a total of 19 minutes, until the ablation was considered complete (Figure 1). The needle tract was ablated at the end of the procedure. No complications were observed during or after the ablation. The conditions of the patient were stable and she was dismissed the day after the procedure with antibiotic therapy (Amoxicillin Clavulanate - 2 g/die).
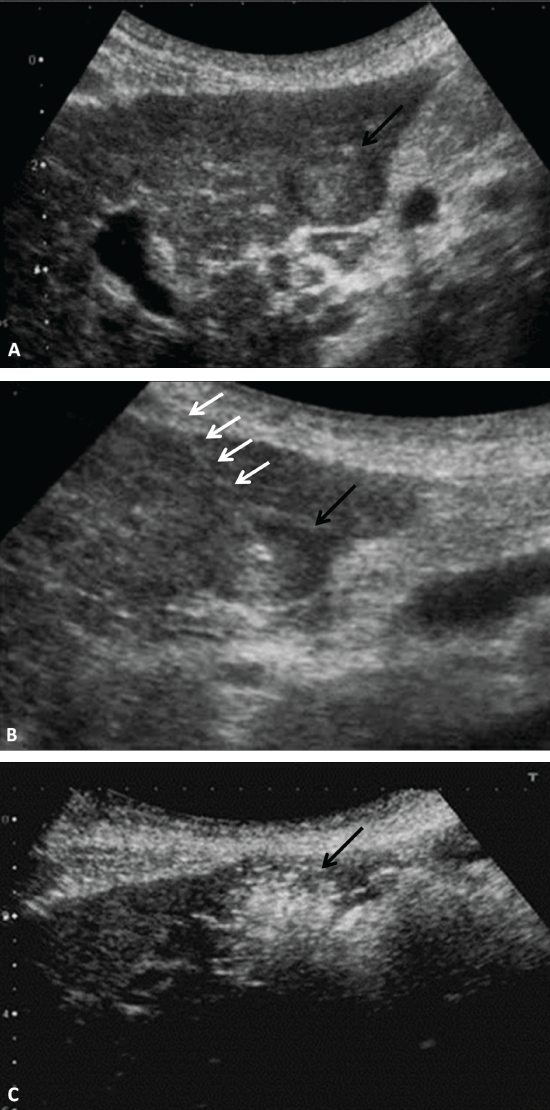
.
Figure 1: Seventy-eight year old woman with hepatocellular carcinoma. Radiofrequency ablation was performed with a RF generator system (AMICATM, HS Hospital Service, Aprilia, Italy), using a LeVeen multiple tined needle (Boston Scientific Marlborough, MA, USA), under ultrasound (US) guidance with a convex array transducer (3-6MHz, Esaote MyLab Twice, Genova, Italy). A 20 mm HCC nodule (arrow) was firstly identified in the left liver lobe at the US examination performed before starting the procedure (Figure 1a). A LeVeen multiple tined needle (white arrows) was inserted inside the nodule (black arrow (Figure 1b). The size of the ablation zone could be roughly evaluated by an expanding hyperechoic area arising within the tumor during the procedure (arrow); RF current was applied for 19 minutes: at that point the ablation was considered complete (Figure 1c).
View Figure 1
Two days after being discharged, the patient was readmitted due to a small leak of ascites from the needle entry site in the subxyphoid region, increasing anorexia and painful abdominal distension. Physical examination showed clinically evident ascites, without signs of hepatic encephalopathy. The patient's temperature was 37.4 ℃; lab tests were unremarkable.
A color-doppler US study demonstrated a moderate amount of ascites; the main portal vein and its branches were patent, as much as the superior mesenteric vein. The celiac trunk and the superior mesenteric artery were unremarkable. There was no bile duct dilatation. There was no evidence of intrahepatic or subcapsular fluid collections (Figure 2). A CT scan was performed without iodinated contrast media administration, due to referred allergy. CT demonstrated a conspicuous amount of ascites; a marked thickening of the greater omentum and parietal peritoneum was also observed (Figure 3). During the first two days after admission, the patient showed quite stable conditions, with one episode of biliary vomiting and three episodes of diarrhea; her body temperature constantly remained in the range of 36.8-37, 5 ℃. A paracentesis was performed the day after the admission, revealing a polymorphonuclear (PMN) count of 2800 cell/mm3, a total protein content of 1.84 g/dL, an albumin content of 1,02g/dl, LDH level of 117 U/l, a glucose level of 100 mg/dL and a bilirubin level of 0.45mg/dL. Ascitic fluid and blood cultures did not show any bacterial growth. Therefore, a diagnosis of Spontaneous Bacterial peritonitis was made by physicians; an empiric oral antibiotic therapy was started immediately with Amoxicillin-Clavulanate (2gr/die)]. Another US-guided paracentesis performed two days later revealed a PMN count of 1.400 cell/mm3, a total protein content of 2.19 g/dL, an albumin content of 1,31g/dl, a LDH level of 116 U/l, a glucose level of 178 mg/dL and RBC count > 10.000/mm3. Ascitic fluid and blood cultures were negative. Because of the healing PMN cell count, the same therapy was maintained. Five days later, due to a slightly worsening of the clinical conditions, a third paracentesis was performed, revealing a PMN count of 1.500 cell/mm3, a total protein content of 2.5 g/dL, an albumin content of 1,5 g/dl, a LDH level of 161 U/l, a glucose level of 118 mg/dL. Ascitic fluid culture was negative again. The antibiotic therapy was then changed to Cefotaxime (6gr/die). The patient's clinical conditions remained substantially stable in the following two days, showing only three vomiting episodes. A fourth US guided paracentesis revealed a PMN count of 1.160 cell/mm3, a total protein content of 2.7 g/dL, an albumin content of 1,8 g/dl, a LDH level of 144 U/l and glucose level of 89 mg/dL. The ascitic fluid cultures were still negative. Cefotaxime (6gr/die) was continued; Imipenem-Cilastatin (2g/die i.v.) and Teicoplanin (400 mg/die) were added in order to enlarge the spectrum activity. A fifth US-guided paracentesis, performed at day 15 after the admission, revealed a PMN cell count of 880 cell/mm3, a total protein content of 3,1 g/dL, an albumin content of 2 g/dl, a LDH level of 141 U/l and a glucose level of 111 mg/dL. The symptoms gradually reduced and signs of peritonism were no more observed. The same therapy was maintained; then, only daily US examinations were performed, demonstrating progressive reduction of the amount of the ascitic fluid. The patient was discharged 28 days after the RFA in good general conditions; the oral antibiotic therapy was continued for ten days. During the hospitalization, a supportive therapy was also administered (Albumin, Glucosate and Potassium Canrenoate, Ondasentron).
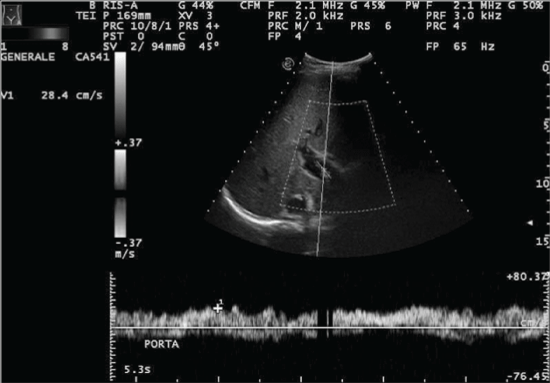
.
Figure 2: Seventy-eight year old woman with hepatocellular carcinoma. The abdominal grayscale US scan was performed with a convex array transducer (3-6 MHz, EsaoteMyLabTwice, Genova, Italy). The color-doppler US study demonstrates that the main portal vein and its branches are patent, as much as the superior mesenteric vein. There is no bile duct dilatation. There is no evidence of intrahepatic or subcapsular fluid collections
View Figure 2
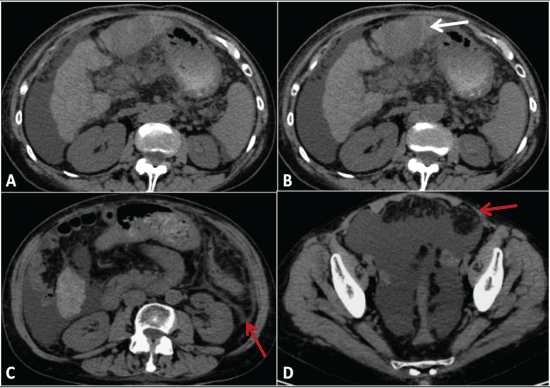
.
Figure 3: Seventy-eight year old woman with hepatocellular carcinoma. An unenhanced low dose CT of the abdomen was performed with a 64 slice-CT scanner (Somatom Sensation Cardiac, Siemens). Axial reconstructions (thickness: 3 mm) demonstrate a moderate amount of ascites; the ascitic fluid is quite limpid (around 10 HU), without any obvious hemorrhagic components (A, D); a marked thickening of the parietal peritoneum and greater omentum is also respectively observable in (C) and (D) (red arrows). The ablated lesion appears as an ovale hypodense area in the left liver lobe (B).
View Figure 3
Discussion
RFA is commonly used to treat early HCC [1-3]. It is a relatively safe procedure, with mortality and major complication rates ranging from 2.2 to 4.0% and 0.1% to 0.5% respectively, with similar outcome to surgery in treating small HCC; in comparison with other mini-invasive treatments, such as percutaneous ethanol injection and percutaneous acetic acid injection, RFA shows even better results in terms of efficacy, despite a higher complication rate [4-6]. The most frequent intra-hepatic major complications are bleeding, abscess and biliary injury; peritoneal bleeding, gastrointestinal perforation and pleural effusion are the most commonly reported extra-hepatic complications [7-10] (see Table1). Infective complications other than liver abscess are rarely observed and only a few cases of secondary peritonitis are described in literature. Livraghi et al. reported one death related to a secondary peritonitis in a large multi center study regarding 3.554 RFA; the patient died from Staphylococcus Aureus infection due to a break in the sterile technique [7]. Two deaths ascribed to peritonitis, respectively due to an ileal perforation and a biliary leak, were reported by Tateishi et al. occurring in their experience of 1000 ablations performed over a 4-year period [9]. The only case of suspected SBP was described by Lucey et al; however, even in that case, the authors could not be sure the infection was effectively related to the ablation, because the patients already had ascites before the procedure [11]. To our knowledge, no other cases of SBP following liver RFA are reported in literature.
![]()
Table 1: Complications after Radiofrequency ablation of hepatic tumor [22].
View Table 1
Spontaneous bacterial peritonitis is a bacterial infection of the ascitic fluid (AF), usually associated with a positive bacterial culture and an AF PMN-cell count of > 250/mm3, in the absence of surgically treatable intra-abdominal sources of infection. SBP mainly occurs in patients with decompensated liver disease; 70% of patients are Child-Pugh class C, with the remainder being class B [12]. Infections are usually monomicrobial, caused by Gram-negative bacterias, such as Haemophilus influenzae or Klebsiella pneumoniae, in more than 60% of cases. Bacterial Translocation (BT) in the ascitic fluid is the key mechanism in the onset of SBP, consisting in the inability of the gut to contain bacteria; once they translocated across the mucosa, bacteria can spread in other tissues, including the bloodstream [12]. Cirrhotic patients showed higher susceptibility to ascitic fluid contamination, due to intestinal flora overgrowth, increased intestinal permeability and alterations in the systemic and local immune defense; in those patients, the immune system cannot be able to eradicate organisms once they have escaped [12-14]. The patients usually presented with fever, abdominal pain and increased amount of ascitic fluid. Less common signs and symptoms are hepatic encephalopathy, diarrhea, abdominal tenderness and shock; almost 10% of patients have no symptoms [12,13]. The diagnosis of SBP is based on paracentesis and AF analysis. The PMN cell count in the AF represents the main element: cell count cut-off of 250/mm3 and 500/mm3 are respectively associated with the highest sensitivity and specificity in the diagnosis of SBP, according to the EASL clinical practice guidelines [12,15]. Serum and AF albumin levels should be obtained from the first specimen from a given patient, in order to calculate the serum-ascites albumin gradient (SAAG), that can suggest the presence of portal hypertension with an accuracy of 97% [12,14]. Other tests could be performed, such as those for glucose and LDH levels, which are usually increased, probably due to the bacterial activity and the peritoneal inflammation respectively [12,15,16]. As previously stated, the classic variant of SBP is also characterized by the isolation of bacteria in cultures of AF (monomicrobial in 92% of cases) [15]. However, basing on the AF PMN count and the culture results, other variants of SBP are described (such as Culture Negative Neutrocytic Ascites or CNNA, monomicrobial non-neutrocytic ascites, polymicrobial bacteriascites) [12,17]; all variants of AF infections are summarized in Table 2. In presence of positive PMN cell count, waiting for bacterial cultures is not necessary: an empiric antibiotic therapy can be immediately started, because classic SBP and CNNA are usually treated in a similar fashion [12,16,17].
![]()
Table 2: Differential diagnosis for ascitic fluid infection [23].
View Table 2
In the above reported case, the diagnosis of SBP was based on AF features and criteria for the exclusion of other pathologies. Although her cultures were negative, the patient was likely to be affected by a classic variant of SBP. These negative results were probably due to the post- procedural antibiotic prophylaxis; a single dose of an effective antibiotic mostly leads to a negative bacterial culture [18]. CNNA variant was to be excluded either way, because no antibiotic treatment within 30 days is a required criterion for such diagnosis [19]. In literature, there is no consensus in the routine use of antibiotics when performing RFA; most authors routinely administer antibiotic prophylaxis with Ceftriaxone sodium or gentamicine sulphate and Ampicillin to patients at high risk of complications, such as those with diabetes and previous history of bilio-enteric fistula [11,12]. At our Department, the patient is usually dismissed the day after the procedure with antibiotic therapy (Amoxicillin-Clavulanate-2 g/die).
The differentiation between spontaneous and secondary bacterial peritonitis is of critical importance, because the mortality rate of the former is about 80% in case of unnecessary surgery, whereas the mortality rate of the latter is close to 100% in case of conservative treatment. In the specific case, the diagnosis of secondary peritonitis was less likely for several reasons; firstly, a CT scan and lab tests were performed in order to exclude other intra-abdominal sources of infection (gastrointestinal perforation, urinary infections, and pancreatitis); secondly, RFA was performed in adequate conditions, without any suspicions of break in the sterile technique. Moreover, several AF features can suggest diagnosis of secondary peritonitis; the main element is the lack of PMN healing after 48 h of treatment. Other features are very high total protein content, lactate dehydrogenase greater than the upper limit of normal for serum, and glucose less than 50 mg/dL; most of these features were absent in our case. Secondary peritonitis due to biliary leak was also excluded, because high albumin levels and SAAG were usually observed in these cases [12,16,18].
In this case, the causal relationship between RF procedure and SBP is not clear. On one hand, the close temporal relationship could not be overlooked. On the other hand, we should also consider that the patient had no previous episodes of peritonitis and was affected by a compensated Child-Pugh A cirrhosis, thus she was at low risk of SBP [12]. A hypothesis could be that the necrosis induced during the procedure may lead to alterations in the local immune defense and be the key mechanism inciting for simple colonization to become infection; Lucey et al. suggested that these alterations could happen when treating lesions closer to the liver capsule [11]. In our case, the ablated lesion was located in the segment III and was almost superficial; the patient did not have ascites before the procedure. Thus, the possibility that the RFA acted as an independent local factor inciting the SBP onset should be taken into account.
SBP resolves with antibiotic therapy in approximately 90% of patients; broad-spectrum therapy is warranted in patients with ascitic fluid infection if bacterial cultures are negative or susceptibility tests are not available. Cefotaxime or a similar third-generation cephalosporin is usually considered the treatment of choice for suspected SBP, covering 95% of the most frequent pathogens [18,19]. In the reported case, an empiric antibiotic therapy was immediately started (Amoxicillin Clavulanate, 2 g/die), then therapy was changed to Cefotaxime (6 g/die), Tinidazole (1 g/die) and Ciprofloxacin ((1 g/die); lately Imipenem/Cilastatin (2 g/die i.v.) and Teicoplanin (400 mg/die) were added in order to enlarge the spectrum activity [17,19-22].
This is the first report attesting patient survival to a SBP episode after RFA; the positive outcome was obtained thanks to an early diagnosis and a therapy with scientifically proven effects.
References
-
Crocetti L, de Baere T, Lencioni R (2010) Quality improvement guidelines for radiofrequency ablation of liver tumours. Cardiovasc Intervent Radiol 33: 11-17.
-
Cho YK, Rhim H, Noh S (2011) Radiofrequency ablation versus surgical resection as primary treatment of hepatocellular carcinoma meeting the Milan criteria: a systematic review. J Gastroenterol Hepatol 26:1354-1360.
-
Huang J, Hernandez-Alejandro R, Croome KP, Yan L, Wu H, et al. (2011) Radiofrequency ablation versus surgical resection for hepatocellular carcinoma in Childs A cirrhotics-a retrospective study of 1,061 cases. J Gastrointest Surg 15: 311-320.
-
Koda M, Murawaki Y, Hirooka Y, Kitamoto M, Ono M, et al. (2012) Complications of radiofrequency ablation for hepatocellular carcinoma in a multicenter study: An analysis of 16 346 treated nodules in 13 283 patients. Hepatol Res 42: 1058-1064.
-
Sato M, Tateishi R, Yasunaga H, Horiguchi H, Yoshida H, et al. (2012) Mortality and morbidity of hepatectomy, radiofrequency ablation, and embolization for hepatocellular carcinoma: a national survey of 54,145 patients. J Gastroenterol 47: 1125-1133.
-
Lin SM, Lin CJ, Lin CC, Hsu CW, Chen YC (2005) Randomised controlled trial comparing percutaneous radiofrequency thermal ablation, percutaneous ethanol injection, and percutaneous acetic acid injection to treat hepatocellular carcinoma of 3 cm or less. Gut 54: 1151-1156.
-
Livraghi T, Solbiati L, Meloni MF, Gazelle GS, Halpern EF, et al. (2003) Treatment of focal liver tumors with percutaneous radio-frequency ablation: complications encountered in a multicenter study. Radiology 226: 441-451.
-
Kasugai H, Osaki Y, Oka H, Kudo M, Seki T; Osaka Liver Cancer Study Group (2007) Severe complications of radiofrequency ablation therapy for hepatocellular carcinoma: an analysis of 3,891 ablations in 2,614 patients. Oncology 72 Suppl 1: 72-75.
-
Tateishi R, Shiina S, Teratani T, Obi S, Sato S, et al. (2005) Percutaneous radiofrequency ablation for hepatocellular carcinoma. An analysis of 1000 cases. Cancer 103: 1201-1209.
-
Rhim H (2005) Complications of radiofrequency ablation in hepatocellular carcinoma. Abdom Imaging 30: 409-418.
-
Lucey BC, Maher MM, Gervais DA, Mueller PR (2002) Bacterial peritonitis: a postulated cause of death associated with hepatic radiofrequency ablation. Clin Radiol 57: 765-767.
-
Such J, Runyon BA (1998) Spontaneous bacterial peritonitis. Clin Infect Dis 27: 669-674.
-
Koulaouzidis A, Bhat S, Saeed AA (2009) Spontaneous bacterial peritonitis. World J Gastroenterol 15: 1042-1049.
-
Runyon BA, Montano AA, Akriviadis EA, Antillon MR, Irving MA, et al. (1992) The serum-ascites albumin gradient is superior to the exudate-transudate concept in the differential diagnosis of ascites. Ann Intern Med 117: 215-220.
-
European Association for the Study of the Liver (2010) EASL clinical practice guidelines on the management of ascites, spontaneous bacterial peritonitis, and hepatorenal syndrome in cirrhosis. J Hepatol 53: 397-417.
-
Alaniz C, Regal RE (2009) Spontaneous bacterial peritonitis: a review of treatment options. P T 34: 204-210.
-
Baskol M, Gursoy S, Baskol G, Ozbakir O, Guven K, et al. (2003) Five days of ceftriaxone to treat culture negative neutrocytic ascites in cirrhotic patients. J Clin Gastroenterol 37: 403-405.
-
Runyon BA; AASLD (2013) Introduction to the revised American Association for the Study of Liver Diseases Practice Guideline management of adult patients with ascites due to cirrhosis 2012. Hepatology 57: 1651-1653.
-
Runyon BA, Hoefs JC (1984) Culture-negative neutrocytic ascites: a variant of spontaneous bacterial peritonitis. Hepatology 4: 1209-1211.
-
Ricart E, Soriano G, Novella MT, Ortiz J, Sàbat M, et al. (2000) Amoxicillin-clavulanic acid versus cefotaxime in the therapy of bacterial infections in cirrhotic patients. J Hepatol 32: 596-602.
-
Cartier M, Terg R, Lucero R, A. Muñoz, G. Romero, et al. (2010) Pilot study: Gelafundin (polygeline) 4% plus antibiotics in the treatment of high-risk cirrhotic patients with spontaneous bacterial peritonitis. Alimentary pharmacology & therapeutics 32: 43-48.
-
Kaymakoglu S, Eraksoy H, Okten A, DEMIR K, CALANGU S, et al. (1997) Spontaneous ascitic infection in different cirrhotic groups: prevalence, risk factors and the efficacy of cefotaxime therapy. European journal of gastroenterology & hepatology 9: 71-76.
-
Mendiratta-Lala M, Brook OR, Midkiff BD, Brennan DD, Thornton E, et al. (2010) Quality initiatives: strategies for anticipating and reducing complications and treatment failures in hepatic radiofrequency ablation. RadioGraphics 30: 1107-1122.
-
Sheer TA, Runyon BA (2005) Spontaneous bacterial peritonitis. Dig Dis 23: 39-46.





