International Journal of Radiology and Imaging Technology
Visualization of Vascular Anastomosis as Responsible Sites of Hemoptysis by Three-Dimensional Angiography for the Guidance of Endovascular Treatment
Kembu Nakamoto*, Hiroshi Hashiyada, Toshiyuki Fujii, Motohiro Takeshige, Kazuya Yoshida and Kaido Ooishi
Division of General Thoracic Surgery and Division of Vascular Surgery, Department of Surgery, Shunan Memorial Hospital, Kudamatsu, Yamaguchi, Japan
*Corresponding author:
Kembu Nakamoto, Division of General Thoracic Surgery, Shunan Memorial Hospital, 1-10-1 Ikunoya-minami, Kudamatsu, Yamaguchi 744-0033, Japan, Tel: +81-833453330, Fax: +81-833453331, E-mail: nakamoto@hcsdojinkai.or.jp
Int J Radiol Imaging Technol,
IJRIT-1-004, (Volume 1, Issue 1),
Case Report
Received: August 27, 2015: Accepted: October 20, 2015: Published: October 22, 2015
Citation: Nakamoto K, Hashiyada H, Fujii T, Takeshige M, Yoshida K, et al. (2015) Visualization of Vascular Anastomosis as Responsible Sites of Hemoptysis by Three-Dimensional Angiography for the Guidance of Endovascular Treatment. Int J Radiol Imaging Technol 1:004
Copyright: ©2015 Nakamoto K. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The major site of bronchial hemorrhage in inflammatory hemoptysis is vessel anastomoses (VA) between pulmonary and systemic arteries. Three-dimensional computed tomographic angiography (3D-CT angio) was applied to depict VA for accurate access in endovascular treatment (EVT) for two patients with bronchiectasis. Fusion of the images of pulmonary and systemic 3D-CT angio visualized VA of potential hemorrhagic bronchi. VA depiction allowed successful EVT for hemoptysis with exclusion of non- responsible vessels.
Introduction
Endovascular treatment (EVT) for hemoptysis in inflammatory lung diseases is now the standard strategy since Remy reported the effect of bronchial arterial embolization [1]. However, the detection of responsible arteries is difficult because some cases have ectopic or non-bronchial arteries for potential hemorrhage [2]. Three-dimensional reconstructed computed tomographic angiography (3D-CT angio), which produced high-resolution three-dimensional images of small peripheral pulmonary vessels to the level of daughter segments [3], was applied for the detection of responsible arteries by visualization of vessel anastomoses (VA) as a sign of potential hemorrhagic bronchi. We experienced two patients undergoing successful EVT for hemoptysis with VA depiction.
Methods and Case Presentation
Individual patient consent was obtained.
Visualization of VA by 3D-CT angio: A contrast-enhanced chest CT scan (64 multi-detector row CT scanner; Optima 664, General Electronics Medical Japan, Tokyo) was taken after detecting the bleeding sites on bronchoscopy or a plane chest CT scanner. Helical CT data concerning pulmonary and systemic arteries were acquired at 25 and 35 seconds of maximum enhanced phase after intravenous contrast medium infusion (Iopamiro 100 ml, 4 ml/seconds; Bayer Schering Pharma; Berlin, Germany) with 0.625 mm of axial transverse slice in 20 seconds breathe hold. Each enhanced vessel around the target pulmonary lesions on the axial transverse CT images was traced to the proximal arteries. Traced arteries were reconstructed in 3D topographic angiography by volume rendering method with 350 of window width and 40 of window level, as well as pulmonary arteries. VA sites were depicted by the fusion of images of systemic and pulmonary 3D-CT angio, and the connections between pulmonary and systemic arteries were defined as VA. Arteries with VA were defined as vessels responsible for potential hemoptysis [4]. 3D-CT angio was reconstructed using workstation (Ziostation, Ziosoft Inc., Tokyo) software. The detailed process of 3D-CT angio was as previously described [3]. The numbering and symbols for pulmonary vascular branches followed the consensus reached by the Japanese Committee on the Nomenclature for Bronchial Branching [3].
EVT for hemoptysis: Target arteries detected on 3D-CT angio were accessed using appropriate guiding catheters (Destination, Terumo, Tokyo, or Goodtec Catheter, Goodman, Nagoya) through the femoral or humeral approach under digital subtraction angiography (DSA). A micro-catheter (Asahi Veloute VEL150-16S, Asahi Intecc J-sales, Tokyo) through the guiding catheter was wedged into the target artery, and then micro-coils (ED Coil, Kaneka Medical Products, Osaka, or C-Stopper Coil, Piolax Medical Devices, Yokohama) for embolization were repeatedly inserted into the artery until the blood flow was shown to be completely blocked.
Patient 1: A 68-year-old male was admitted to our hospital for repeated hemoptysis. He had bronchiectasis in the right upper lobe. The hemorrhagic bronchus was shown to be segment bronchus B2 on bronchoscopy. 3D-CT angio depicted bronchial and systemic arteries branching from the right subclavian artery just peripheral of the vertebral artery communicating with pulmonary artery A2b (Figure 1A and Figure 1B). The aberrant artery might be a pre-existing vessel. EVT was applied via femoral access for the right bronchial artery, and humeral access for the aberrant artery. Both arteries were successfully embolized with micro-coils. The patient had no complaints of hemoptysis for the next 3 and a half years.
.
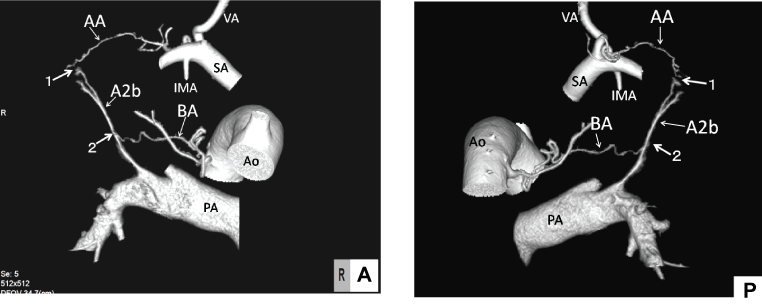
Figure 1: Patient 1: A 68-year-old male with hemoptysis of bronchiectasis in the right upper lobe.
Anastomotic sites in the 3D angiography: right antero-medial direction (A) and right posterior direction (B). Unrelated vessels were deleted.
Figure 1A: The aberrant artery originated from the right subclavian artery connected to pulmonary artery A2b with hyper vascularization (arrow 1). The right crooked bronchial artery (BA) communicated to the A2b pulmonary artery of the posterior segment in the right upper lobe (arrow 2).
Figure 1B: Aberrant artery (AA) that branched just peripheral of the vertebral artery (VA) communicated with A2b (arrow 1) with hyper vascularity. One of the bi-branching bronchial arteries (BA) connected with A2b (arrow 2).
(AA: aberrant artery, Ao: aorta, BA: bronchial artery, IMA: right internal mammary artery, PA: right truncal pulmonary artery, SA: right subclavian artery, VA: right vertebral artery)
View Figure 1
.
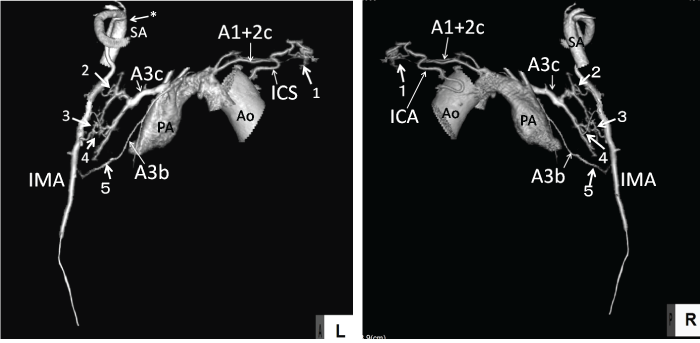
Figure 2: Patient 2: A71-year-old male with hemoptysis of bronchiectasis in the left upper lobe.
Anastomotic sites in the 3D angiography: antero-lateral direction (A) and postero-medial direction (B). Unrelated vessels were deleted.
Figure 2A: The left 5th intercostal artery (ICA) communicated with pulmonary artery A1 + 2c of the apical posterior segment in the left upper lobe with hyper vascularity (arrow1). Four small aberrant arteries (arrows 2 ~ 5) branching from the left internal mammary artery (IMA) communicating with pulmonary arteries A3b and A3c of the anterior pulmonary segment with or without hyper vascularity. IMA orifice was tortured and stenotic (arrow asterisk).
Figure 2B: ICA and aberrant arteries communicated with A1 + 2c, A3b, and 3c through the pleura (arrows 1~5).
(A1 + 2c, A3b, A3c: pulmonary artery A1 + 2c, 3b, 3c, Ao: aorta, ICA: 5th intercostal artery, IMA: left internal mammary artery, PA: left pulmonary artery, SA: left subclavian artery).
View Figure 2
Patient 2: A 71-year-old male was admitted to our hospital for hemoptysis with bronchiectasis in the left upper lobe. He had a history of left bronchial arterial ligation under open thoracotomy against massive hemoptysis two years previously. The 3D-CT angio depicted the left 5th intercostals and the left internal mammary artery communicating with pulmonary arteries of the left upper division (Figures 2A and Figure 2B). The intercostal artery entered the pulmonary parenchyma through the peripheral pleura and communicated with pulmonary artery A1 + 2c of the apical-posterior pulmonary segment. Four small aberrant arteries branched from the internal mammary artery communicated with pulmonary arteries A3b and A3c of the anterior pulmonary segment. Test injection of contrast medium in these arteries showed massive shunts to pulmonary arteries. The 5th intercostal artery was successfully embolized with micro-coils. EVT for the internal mammary artery failed because it had a tortuous and stenotic orifice at the branching site. The mammary artery was embolized by open access to the internal mammary artery through the 4th costal cartilage bed under local anesthesia. Hemoptysis was completely blocked thereafter with low dose antibiotics for controlling chronic infection, for half a year.
Discussion
The major causes of EVT failure for hemoptysis were reported to be the overlooking of potential aberrant arteries or ectopic bronchial arteries [2]. Non-bronchial aberrant arteries may originate from intercostal, subclavian, axillary, internal mammary or infraphrenic arteries [5]. 3D-CT angio with a currently available multi-detector row CT scanner (MDCT) provided high-resolution images of 3D pulmonary or systemic arterial trees to the small peripheral level with 0.5 ~ 2 mm caliber [3,5]. MDCT can assist in the identification of arteries responsible for potential hemorrhage with signs of vessel enlargement or coursing on multiplanar reconstruction images [6]. However, the direct sign of bleeding bronchi is the extra vasation of contrast medium into them, while this sign is quite rare [6]. VA are considered the most reliable findings of potential hemorrhagic bronchi, except in pulmonary cavities, aneurysm due to vasculitis or trauma [6], as Liebow pointed out in the bronchial circulation [4]. Image fusion of both pulmonary and systemic 3D-CT angio visualized VA. Visualization of VA allowed the exclusion of non-responsible vessels and guided successful EVT to accurate target lesions. 3D-CT angio also provided detailed characteristics of responsible arteries for the choice of access sites, catheters and coils for EVT. The current software process for 3D-CT angio takes a relatively long time (3 ~ 4 hours) for tracing tiny vessels, which may be vital enough to delay emergent EVT under respiratory supports. However, 3D-CT angio with visualization of VA provides more reliable guidance for successful EVT of hemoptysis.
Acknowledgement
We thank Yuya Nakamura, RT, for help with the software for 3D-CT angio.
References
-
Remy J, Arnaud A, Fardou H, Giraud R, Voisin C (1977) Treatment of hemoptysis by embolization of bronchial arteries. Radiology 122: 33-37.
-
Vujic I, Pyle R, Hungerford GD, Griffin CN (1982) Angiography and therapeutic blockade in the control of hemoptysis. The importance of nonbronchial systemic arteries. Radiology 143: 19-23.
-
Nakamoto K, Omori K, Nezu K (2010) Superselective segmentectomy for deep and small pulmonary nodules under the guidance of three-dimensional reconstructed computed tomographic angiography. Ann ThoracSurg 89: 877-884.
-
Liebow AA, Hales MR, Harrison W, Bloomer W, Lindskog GE (1950) The genesis and functional implications of collateral circulation of the lungs. Yale J Biol Med 22: 637-650.
-
Bruzzi JF, Remy-Jardin M, Delhaye D, Teisseire A, Khalil C, et al. (2006) Multi-detector row CT of hemoptysis. Radiographics 26: 3-22.
-
Khalil A, Fartoukh M, Tassart M, Parrot A, Marsault C, et al. (2007) Role of MDCT in identification of the bleeding site and the vessels causing hemoptysis. Am J Roentgenol 188: 117-125.





