International Journal of Radiology and Imaging Technology
Emergency Embolization of a Rupture of the Left Colic Aneurysm
Domenico Laganà1*, Maria Petullà1, Ierardi Anna2, Gianpaolo Carrafiello2 and Oscar Tamburrini1
1Department of Radiology, University of Magna Grecia, Catanzaro, Italy
2Department of Radiology, University of Insubria, Varese, Italy
*Corresponding author:
Domenico Laganà, Department of Radiology, University of Magna Grecia, Catanzaro, Italy, Tel: +3909613647285, Fax: +3909613647395, E-mail: donlaga@gmail.com
Int J Radiol Imaging Technol,
IJRIT-1-005, (Volume 1, Issue 1),
Case Report
Received: October 22, 2015: Accepted: November 23, 2015: Published: November 25, 2015
Citation: Laganà D, Petullà M, Anna I, Carrafiello G, Tamburrini O (2015) Emergency Embolization of a Rupture of the Left Colic Aneurysm. Int J Radiol Imaging Technol 1:005
Copyright: © 2015 Laganà D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
This is a case report of an emergency embolization of a left colic aneurysm performed on a 72 year-old woman. The abdominal CTA scan showed a large retroperitoneal hematoma and an aneurysm of a branch of the inferior mesenteric artery. A selective angiography of the inferior mesenteric artery confirmed an aneurysm of the left colic artery. An endovascular ligation was performed with platinum microcoils. The 3-month follow-up confirmed the complete exclusion of the aneurysmatic vessel.
Keywords
Visceral artery aneurysm, Ruptured left colic aneurysm, Coil embolization
Introduction
Visceral artery aneurysms (VAAs) are uncommon, with a reported incidence of 0.1-2%. [1,2]. The aneurysms of the inferior mesenteric artery and its branches are particularly rare and estimated to account for less than 0.5% of all VAAs, yet they are an important vascular lesion due to their ruptured clinical presentation in 30-40% of the cases, with a mortality rate of 70% [1,2].
However, the increasing diffusion of cross-sectional imaging ultrasound and, above all, computed tomography (CTA), has led to the diagnosis of a higher percentage (40-80%) of symptomatic colic aneurysm [2]. We present one case of an emergency embolization of a left colic aneurysm (LCA).
Case Report
An ultrasound examination, performed on a 72 year-old woman in the Emergency Department due to acute lumbar pain, showed a large buildup of blood in the pre-sacral space. The patient had previously undergone to a laparoscopic cholecystectomy. The CTA, performed after two hours, due to a sudden hemorrhagic shock (arterial pressure 90/50), showed a large retroperitoneal hematoma and an aneurysm at greater longitudinal axis of 18 mm of a branch of the inferior mesenteric artery (Figure1a, Figure 1b and Figure 1c). Generally this would indicate a traumatic or iatrogenic pseudo-aneurysm.
.
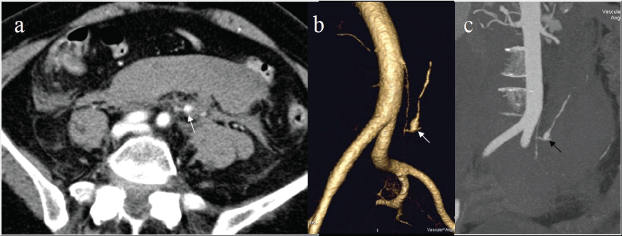
Figure 1a: CT showing a large retroperitoneal hematoma and a small aneurysm of a branch of inferior mesenteric artery (arrow).
1b and 1c: 3D VR (b) and MIP (c) reconstruction allows a precise localization of the aneurysm at the proximal tract of the left colic artery (arrows).
View Figure 1
Due to the poor hemodynamic conditions and the age of the patient an endovascular treatment was proposed. The procedure was performed through a percutaneous approach of the right common femoral artery under local anesthesia (10 ml of carbocaine 2%) where a 5F sheath (Terumo, Tokyo, Japan) was positioned. The inferior mesenteric artery was selectively catheterized using a 5F catheter (Simmons 1, Cordis, and Miami, FL, USA). The diagnostic angiography confirmed an aneurysm of the left colic artery with contrast media extravasation (Figure 2a). The aneurysm was crossed using a micro-catheter 2.7F and a 0.014" Hydrophilic Guide Wire (Progreat, Terumo, Tokyo, Japan).
.
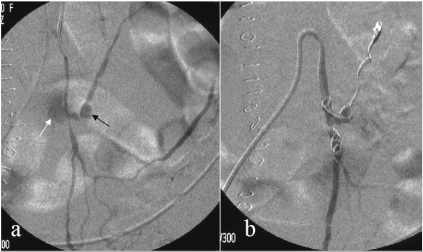
Figure 2a: Pre-procedural selective angiography of the inferior mesenteric artery showed an active bleeding (white arrow) from the small aneurysm (black arrow) of the left colic artery and confirmed aneurysmal location, dimensions and morphology.
2b: Selective angiography after endovascular ligature with microcoils displaced distally and proximally to the aneurysm.
View Figure 2
An endovascular ligation was performed with 3 platinum microcoils (Vortx-18 Diamond Shapep) (Figure 2b). Post-procedural angiography showed the complete exclusion of the aneurysmatic vessel. No complications, (such as intestinal infarction) occurred. The pain was eased after the procedure.
The follow-up was performed by a clinical examination and a CTA 1 week after the procedure and after 3 months (Figure 3a and Figure 3b).
.
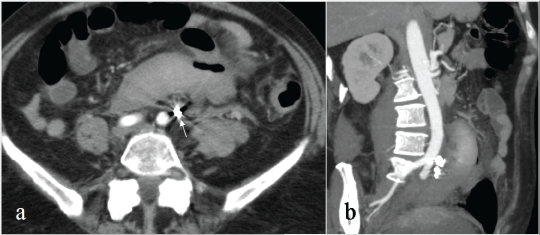
Figure 3a-b: Axial image (a) and MIP reconstruction (b) of a CT scan performed 1 week later, demonstrating the complete exclusion of the aneurysm with artifacts due to the metallic coils (arrow); the retroperitoneal hematoma was almost unchanged.
View Figure 3
Discussion
An LCA accounts for a small percentage of VAAs, but their significance arises from their potentially lethal consequences. In fact, literature states that inferior mesenteric aneurysms usually require urgent surgical intervention and the mortality rate of the rupture is 70% [3]. Among the aneurysms of the inferior mesenteric artery, the colic artery aneurysms are rare. LCA appears to occur as a result of a periarterial inflammation secondary to an atherosclerotic destruction of the artery wall. Alternatively, it has been proposed that they may occur as result of a periarterial inflammation leading to medial de-generation [3,4].
Hypertension may also be important in the pathogenesis of LCAs and their rupture. Many cases probably remain asymptomatic and, unless accidentally discovered, remain undiagnosed throughout life. The majority of the ruptured mesenteric aneurysms are presented as vascular emergencies with few premonitory signs or symptoms. Rarely patients describe abdominal discomfort before the rupture, and so early diagnosis is rare [3-5]. Mesenteric aneurysm can be classified into two groups, intramural (about 70%), with rupture into the lumen of the colon presenting acute or chronic gastrointestinal bleeding; and extravisceral (about 30%), with rupture into the retroperitoneum presenting severe abdominal pain and hemorrhagic shock [3]. Currently, there are various therapeutic options available for VAAs including conventional open surgery [1], laparoscopic surgery [6], and endovascular treatment [5,7].
In the past, the surgery was the treatment of choice for mesenteric aneurysm; extraintestinal aneurysms were traditionally treated with ligation or resection, whereas intramural aneurysms usually require excision of the adjacent colic wall. However, the surgical approach to mesenteric aneurysm is complex and presents high mortality and morbidity, especially in an emergency [8]. In the last few years, endovascular treatment of VAAs has been reported as a safe and effective alternative [5,7] and it could be carried out, depending on the site and the morphology of the aneurysm, with different techniques and devices [8]. These devices include coils [7], cyanoacrylate [9] and thrombin [10]. Arterial patency can be preserved in saccular aneurysms, where catheterization of the neck allows embolization to be limited to the sac. This is done using coils and/or cyanoacrylate or thrombin [8]. In these aneurysms, where it is necessary to fill the aneurysmal sac or occlude its neck, it is important to take care to avoid intraluminal pressure increase because of the risk of sudden rupture during the procedure [7]. Fusiform aneurysms and aneurysms involving the collateral vessels, such as our case, require endovascular exclusion. Endovascular ligation needs the positioning of the coils in the efferent branches and then in the afferent artery to obtain complete exclusion of the aneurysmatic tract [8]. It is essential to exclude both, inflow and outflow vessels, to reduce the risk of anterograde and retrograde reperfusion. In these cases, the perfusion of the colon can be at least partially maintained by the collateral vessels (left hypogastric artery and superior mesenteric artery through Riolan's Arch).
A small-caliber micro-catheter is highly reliable in achieving super-selective catheterization in small-caliber arteries as the colic arteries. It minimizes the volume of infracted tissue and allows maximal preservation of the organic function and effective navigation through the tortuous arteries.
Treatment with a stent graft, an advanced device with large caliber, is usually impractical due to the small caliber of the subdivision vessels of the inferior mesenteric artery.
The embolization success rates in literature have varied from 75 to 100% with morbidity rates ranging from 14 to 25% [5,7].
Most of the complications reported in the endovascular exclusion of VAAs in literature concern end-organ ischemia, pain, fever and the transitory increase of necrosis enzymes (post-embolization syndrome), technical complications concerning migration of the embolising materials, and complications in accessing the site [2,8].
Few works have been published that compare the mortality and morbidity of surgery with that of endovascular treatment. From literature, we can see that the endovascular treatment presents several advantages due to its minimal invasiveness, especially in emergency. Surgical case studies reflect a higher mortality rate between 3 and 10%, which increases to 19-56% in emergency. The complication rate is between 11 and 18% in election and more than 50% in emergency.
The mortality rate of endovascular treatment borders on 0%, even in emergency with a morbidity rate of 8-20% [1,2,7]. A reperfusion rate of 5% was reported; all cases of reperfusion occurred soon after treatment [9,10]. No medium-long term cases of recanalization are reported. Given our experience, a follow-up with Colour Doppler Ultrasound or CTA of 6 months would appear to be sufficient, along with other checks carried out only in the event of symptoms returning. Moreover, in the aneurysms treated with coils, the evaluation with CTA was made difficult by other metallic objects.
The percutaneous approach offers many advantages compared to the traditional surgical therapy. These advantages include the non-invasiveness of the treatment, the possibility of treating those aneurysms that are difficult to operate on surgically, and the fact that the surgical approach involves resection of the intestinal look concerned, especially in cases of distal or intraparenchymal aneurysms [1,2].
Moreover, should the treatment not be successful, surgical intervention is not ruled out [7]. As reported in recent literature, surgical treatment would only be chosen for cases diagnosed during a laparotomy where an endovascular approach is not appropriate, or in cases of prior unsuccessful endovascular treatment [1].
Conclusion
In conclusion, endovascular therapy can be considered as the treatment of choice for mesenteric aneurysms in an emergency.
References
-
Saltzberg SS, Maldonado TS, Lamparello PJ, Cayne NS, Nalbandian MM, et al. (2005) Is endovascular therapy the preferred treatment for all visceral artery aneurysms? Ann Vasc Surg 19: 507-515.
-
Sessa C, Tinelli G, Porcu P, Aubert A, Thony F, et al. (2004) Treatment of visceral artery aneurysms: description of a retrospective series of 42 aneurysms in 34 patients. Ann Vasc Surg 18: 695-703.
-
Khan S, Cheatle T (1997) Left gastric artery aneurysm--a case report. Eur J Vasc Endovasc Surg 14: 413-414.
-
Lee MK, Vrazas JI (2006) Ruptured left gastric artery aneurysm: unique presentation with hemothorax and hemomediastinum. Cardiovasc Intervent Radiol 29: 438-442.
-
Thomford NR, Yurko JE, Smith EJ (1968) Aneurysm of gastric arteries as a cause of intraperitoneal hemorrhage. Review of literature. Ann Surg 168: 294-297.
-
Sasaki A, Bandoh T, Shiraishi N, Adachi Y, Kitano S, et al. (2001) Laparoscopic ligation of an aneurysm of the left gastric artery. Surg Laparosc Endosc Percutan Tech 11: 225-227.
-
Balderi A, Antonietti A, Ferro L, Peano E, Pedrazzini F, et al. (2012) Endovascular treatment of visceral artery aneurysms and pseudoaneurysms: our experience. Radiol Med 117: 815-830.
-
Laganà D, Carrafiello G, Mangini M, Dionigi G, Caronno R, et al. (2006) Multimodal approach to endovascular treatment of visceral artery aneurysms and pseudoaneurysms. Eur J Radiol 59: 104-111.
-
Yamakado K, Nakatsuka A, Tanaka N, Takano K, Matsumura K, et al. (2000) Transcatheter arterial embolization of ruptured pseudoaneurysms with coils and n-butyl cyanoacrylate. J Vasc Interv Radiol 11: 66-72.
-
Kemmeter P, Bonnell B, VanderKolk W, Griggs T, VanErp J (2000) Percutaneous thrombin injection of splanchnic artery aneurysms: two case reports. J Vasc Interv Radiol 11: 469-472.





