International Journal of Radiology and Imaging Technology
Neuroblastoma: Radiological Diagnosis of a Case with Pulmonary Metastases
Yessoufou-Bakary N1, Kouamé N2*, Manewa S2, Gaimou Blé P1, Agoda A-K2 and N'Goan Domoua AM2
1Department of Radiology, University Hospital Sylvanus Olympio, Ivory Coast
2Department of Radiology, University Hospital of Yopougon, Ivory Coast
*Corresponding author:
Dr. Kouame N, Senior lecturer, Diagnostic radiology and medical imaging, University Felix Houphouet Boigny, Abidjan, 21 BP 2716 Abidjan 21, Ivory Coast, Tel: 22505190002, E-mail: kngoran@yahoo.fr
Int J Radiol Imaging Technol, IJRIT-1-007, (Volume 1, Issue 1), Review Article
Received: November 24, 2015: Accepted: December 21, 2015: Published: December 23, 2015
Citation: Yessoufou-Bakary N,, Kouamé N, Manewa S, Gaimou BP, Agoda AK, et al. (2015) Neuroblastoma: Radiological Diagnosis of a Case with Pulmonary Metastases. Int J Radiol Imaging Technol 1:007.
Copyright: © 2015 Yessoufou-Bakary N,, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective:To report a case of neuroblastoma with lung metastases and demonstrate the importance of thoracic-abdominal-pelvic scan in the exploration of abdominal pelvic masses in the child.
Material and Methods:We report the case of a large abdominal pelvic mass in a three year-old girl, in whom a thoracic-abdominal pelvic CT was performed without and with iodinated contrast medium injection after a non-contributory abdominal ultrasound.
Results:CT helped bring out a heterogeneous left renal tissue mass of 15 cm in diameter, ill-defined and without internal calcifications. The retro-peritoneal vessels were encompassed. The mass crossed the median line and the spinal canal was widened. There were lung metastases. The diagnosis of neuroblastoma was selected and confirmed at pathology.
Conclusion:Medical imaging, particularly CT is essential in the positive diagnosis, pre therapeutic staging and monitoring of treatment of neuroblastoma. The technical protocol should include a thoracic-abdominal-pelvic acquisition or add chest radiography to abdominal pelvic CT.
Keywords
Abdominal pelvic CT, Abdominal pelvic mass, Neuroblastoma, Childhood cancer
Introduction
Neuroblastoma is one of the most common malignant tumors in children [1,2]. Its abdominal location is the most met (70%) giving an aspect of abdominal-pelvic mass. It raises a problem of differential diagnosis with wilms tumor with which it does not have the same treatment or the same prognosis. Hence the importance of a positive diagnosis and an accurate staging and monitoring of appropriate treatment for which medical imaging plays a major role [2]. It is represented by plain film of the abdomen, ultrasound, computed tomography, scintigraphy, MIBG scan and MRI. But CT, although very radiant for the pediatric field, remains essential in this approach because of the unavailability of MRI or the volume of the mass and sometimes is the first-line examination [3]. We report the case of a large abdominal pelvic mass that occurred in a three year-old-girl in whom CT suggested the diagnosis of neuroblastoma with lung metastases. Our objective is to report a rare case of neuroblastoma with lung metastases and demonstrate the importance of the thoracic-abdominal-pelvic scanner in the exploration of abdominal-pelvic masses of the child.
Observation
SK a 3-year-old girl has a large abdominal mass with impaired general condition. She had an ultrasound that objectified a large abdominal pelvic mass of heterogeneous tissue structure repressing the surrounding structures with an absence of visualization of the left kidney, ovaries and uterus. A thoracic-abdominal pelvic CT was requested to clarify the diagnosis. It was performed without and after iodinated contrast medium injection. At the Abdominal pelvic stage, it was demonstrated a large heterogeneous tissue formation containing areas with necrosis without internal calcification image measuring 154 × 95 millimeters in diameter, developed in contact with the left kidney and enhancing heterogeneously after contrast medium injection (Figure 1). It crossed the median line. The left pyelocalyceal cavities were difficult to assess as well as the left renal vein. The median vascular structures (aorta, inferior vena cava) were encompassed (Figure 2). The liver was of homogeneous density without defect of the trunk door or the bile ducts. At the Thoracic stage, it was noted multiple pulmonary parenchymal nodules "ball drop". The CT scan then suggested that it was a neuroblastoma with lung metastases (Figure 3). The patient was transferred to the pediatric oncology department for better management. The diagnosis was confirmed at pathology after surgery preceded by chemotherapy.
.
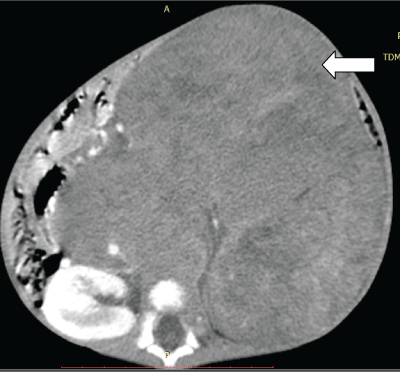
Figure 1: Abdominal pelvic scan. Axial section with iodinated contrast medium injection. Large retro peritoneal tissue mass crossing the median line (arrow) in a 3-year-old girl.
View Figure 1
.
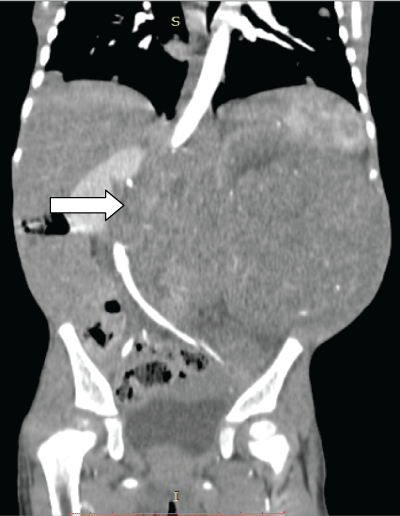
Figure 2: Abdominal pelvic scan. Coronal reconstruction with iodinated contrast medium injection. The mass includes the abdominal aorta (arrow).
View Figure 2
Comments
Neuroblastoma, according to the literature, occurs before the age of 5 years in 90% of cases with prevalence between 2 and 3 years [3,4]. In our case it was a 3-year-old girl. Neuroblastoma is a solid tumor can be located throughout the body [4]. But the retro-peritoneal localization then abdominal is the most common. According to Plantaz [4], this retroperitoneal location would be adrenal. Hence the possible confusion with wilms tumor [5]. In the presence of a large abdominal mass of the child, the first imaging solicited in daily practice is the plain film of the abdomen. Although very little contributory, the plain film of the abdomen can bring out, besides the mass syndrome, the presence of powdery calcifications [3,5] in opposition to coarse calcifications and may allow to distinguish neuroblastoma from Wilms tumor.
.
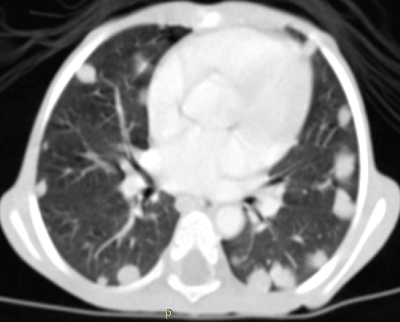
Figure 3: Same patient. The chest CT objectifies lung metastases as pulmonary nodules: Neuroblastoma in stage IV.
View Figure 3
The second imaging, the most commonly required after the plain film of the abdomen is the abdominal-pelvic ultrasound. This modality of medical imaging has the advantage of not being radiant, so preferable for the pediatric field. We performed in first-line intention in our observation. It distinguishes the solid or liquid nature of the mass but is limited by its important volume. It is before this limit related to the volume of our mass (15 cm in diameter) that we opted for the thoracic-abdominal-pelvic CT in our case. CT is an imaging modality which is based on the measurement of X-ray attenuation from a multitude of view angles around the patient. According to Bruisse [3], the scanner should be the first-line examination in cases of suspected neuroblastoma. The CT protocol is not univocal and depends on teams. We performed a thoracic-abdominal pelvic CT in order to evoke a positive diagnosis but also to assess the locoregional tumor extension and remotely. This CT was performed without and with iodinated contrast injection. It highlighted the ill-defined nature of the tumor (Figure 1) as opposed to the well limited even encapsulated one of nephroblastoma. There was no calcification within the mass. But above all the mass included the large retro-peritoneal vessels [3,6,7] and crossed the median line (Figure 2). Unlike nephroblastoma which represses vessels without encompassing them and never crosses the median line. Paradoxically the liver was homogeneous and the metastases were more pulmonary (Figure 3). It was therefore neuroblastoma at stage IV [3,8] which is not exceptional because according to the literature in over 50% of cases, neuroblastoma is discovered in the metastatic stage. Several authors [9-11] are agreeing with us to think that lung metastases are more common in wilms tumors than in neuroblastoma. According to Gaetan [10], the most common sites of metastasis in neuroblastoma are the bone and bone marrow, with involvement of these sites found in the majority of children with newly diagnosed metastatic neuroblastoma. In contrast, lung metastasis is a distinctly uncommon finding in children presenting with metastatic neuroblastoma and remains a useful prognostic marker of unfavorable outcome while lung metastases are frequent in Wilms tumor.
Conclusion
The management of neuroblastoma, a common malignancy of children requires medical imaging. It is a tumor that is most often of retro-peritoneal location and raises a problem of differential diagnosis with nephroblastoma. A perfect knowledge of radiological semiology helps distinguish it from wilms tumor. Its discovery at the metastatic stage is not restricted to Africa (with its late consultation reputation) because in 50% of cases these metastases are described in the literature. These metastases are usually liver but the discovery of pulmonary metastases in our observation should lead us to reconsider CT protocol for an acquisition rather thoracic-abdominal-than the usual abdominal-pelvic CT. In the contrary case, it would be necessary, to add to the abdominal pelvic CT a chest X-ray.
References
-
Michon J, Couturier J, Brisse H, Edeline V, Schleiermacher G, et al. (2003) Neuroblastomes : roles respectifs de la clinique, de l'imagerie, de la pathologie et de la biologie dans les décisions thérapeutiques. Médecine thérapeutique/pédiatrie 6: 172-184.
-
Aloui-Kasbi N, Felah S, Bellagha I, Barsaoui S, Hammou A, et al. (2004) Le neuroblastome : apport de l'imagerie. Journal de Pédiatrie et de Puériculture 17: 28-33.
-
Brisse H, Edeline V, Michon J, Couanet D, Zucker J, et al. (2001) Current strategy for the imaging of neuroblastoma. J Radiol 82: 447-454.
-
Plantaz D, Pasquier D, Dyon JF, Favrot M, Bost M (2001) Neuroblastomes : aspects cliniques, biologiques et thérapeutiques actuels. Médecine Nucléaire - Imagerie fonctionnelle et métabolique 25: 207-212.
-
Olukayode AA, Richard IO, Rachael AA, Babajide OB, Ireti OF, et al. (2014) Pattern of computed tomography scan findings in children with Wilms' tumor in a tertiary hospital in Lagos, Nigeria. Indian J Med Paediatr Oncol 35: 31-35.
-
Kembhavi SA, Shah S, Rangarajan V, Qureshi S, Popat P, et al. (2015) Imaging in neuroblastoma: An update. Indian J Radiol Imaging 25: 129-136.
-
Chu CM, Rasalkar DD, Hu YJ, Cheng FW, Li CK, et al. (2011) Clinical presentations and imaging findings of neuroblastoma beyond abdominal mass and a review of imaging algorithm. Br J Radiol 84: 81-91.
-
Pérel Y, Valteau-Couanet D, Michon J, Lavrand F, Coze C, et al. (2004) Prognosis of neuroblastoma in childhood. Methods of assessment and clinical use. Arch Pediatr 11: 834-842.
-
Gaetan G, Ouimet A, Lapierre C, Teira P, Sartelet H (2014) Neuroblastoma presenting like a Wilms' tumor with thrombus in inferior vena cava and pulmonary metastases: a case series. Springerplus 3: 351.
-
Dubois SG, London WB, Zhang Y, Matthay KK, Monclair T, et al. (2008) Lung metastases in neuroblastoma at initial diagnosis: A report from the International Neuroblastoma Risk Group (INRG) project. Pediatr Blood Cancer 51: 589-592.
-
Farmakis SG, Siegel MJ (2014) Intrarenal neuroblastoma with pulmonary metastases mimicking a Wilms tumor. J Pediatr Surg 49: 1864-1866.





