International Journal of Radiology and Imaging Technology
Adaptive Radiotherapy for Limited Stage Small Cell Lung Cancer
Lindsay Rowe2, Andra Krauze2, John Hanson3 and Don Yee1*
1Department of Radiation Oncology, Cross Cancer Institute, Edmonton, Alberta, Canada
2Radiation Oncology Branch, National Cancer Institute/NIH, Bethesda, MD, USA
3Department of Oncology, Cross Cancer Institute, Edmonton, Alberta, Canada
*Corresponding author:
Dr. Don Yee, Department of Radiation Oncology, Cross Cancer Institute 11560 University Avenue, Edmonton, Alberta, T6G 1Z2, Canada, Tel: +1 780 432 8783, Fax: +1 780 432 8380, E-mail: dony@ualberta.ca
Int J Radiol Imaging Technol, IJRIT-2-013, (Volume 2, Issue 2), Research Article
Received: February 11, 2016: Accepted: April 11, 2016: Published: April 13, 2016
Citation: Rowe L, Krauze A, Hanson J, Yee D (2016) Adaptive Radiotherapy for Limited Stage Small Cell Lung Cancer. Int J Radiol Imaging Technol 2:013.
Copyright: © 2016 Rowe L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background and purpose:We conducted a trial of adaptive radiotherapy (RT) for limited stage small cell lung cancer (LS-SCLC) to quantify the dosimetric advantages, toxicity, survival and failure patterns associated with this technique.
Material and methods:Study patients underwent planning CT scans before treatment (CT-1), after fractions 5 (CT-2) and 10 (CT-3). RT plans were adapted to measured tumor volume changes. Tumors were treated to the maximum safe dose based on critical structure dosimetry. Non-adapted mock RT plans were created using each CT-1 to determine maximum non-adapted dose. Adapted and mock non-adapted plans were compared for tumor and normal tissue doses. Patients were followed for toxicity, failure patterns and survival.
Results:Ten patients were accrued. All patients completed protocol RT. Median total adapted dose was 60 Gy versus 47 Gy in the mock non-adapted plans. Adapted plans provided significantly reduced V20 (mean 31% vs. 36%, p = 0.009), mean lung dose (14.7 vs. 17.3 Gy, p = 0.009), and dose to 1/3 of esophagus (median 35 vs. 49 Gy, p = 0.03) compared to non-adapted plans. Maximal acute RT toxicity was grade 2 esophagitis. There were 2 thoracic and 5 distant failures. Median progression-free and overall survival was 13.4 and 16.1 months.
Conclusion:Adaptive radiotherapy facilitates RT dose escalation for LS-SCLC without overdosing normal structures.
Introduction
The addition of thoracic RT to chemotherapy for limited stage small cell lung cancer (LS-SCLC) patients provides improved local control and overall survival [1,2]. Despite the improved outcomes provided by thoracic RT, LS-SCLC has a high local recurrence rate and low survival after contemporary treatments. Local control rates remain 47% at 2-years, and 5-year overall survival remains 5-10% [1,3].
In an effort to improve local control and survival, various radiation dose/fractionation regimes have been proposed [4-7], based on the observation that SCLC has a radiation dose-response relationship [6,8-11]. However, the application of RT dose escalation into routine clinical practice for LS-SCLC is limited at least partly due to normal tissue toxicity, as the commonly high intrathoracic tumor burden at the time of diagnosis often poses a significant obstacle to delivering a radical dose of chest radiotherapy without exposing the patient to unacceptable risk of radiotherapy-related toxicities to normal critical structures.
Modern radiotherapy technologies which couple linear accelerators with three dimensional imaging capability have allowed for a strategy of adaptive radiotherapy which can facilitate tumor RT dose escalation while minimizing normal tissue toxicity [12,13]. This treatment technique involves adjusting the radiation plan over the course of treatment to account for changes in tumor size and/or position.
Our group has characterized the tumor shrinkage dynamics in LS-SCLC patients undergoing curative-intent chemoradiotherapy [14]. Data from this study indicates that SCLC tumor volumes regress significantly during chemoradiotherapy treatments, mostly during the first ten fractions of radiotherapy. Based on these observations, we initiated a clinical trial of adaptive radiotherapy for LS-SCLC patients in which radiotherapy plans were adjusted according to observed tumor regression. This phase II trial was undertaken to assess the feasibility and dosimetry of adaptive radiation plans, as well as assess rates of local control and survival associated with this technique.
This clinical trial is the first to our knowledge that investigates the novel use of adaptive radiotherapy for small cell lung cancer. Demonstrating the feasibility and safety of exploiting the rapid response rates to chemoradiotherapy this tumor typically exhibits is important in that it may provide a means through which radiotherapy dose escalation can be achieved for a tumor type which historically has been extremely difficult to treat with adequate radiotherapy doses due to the typical tumor bulk that exists at the time of diagnosis.
Patients and Methods
Eligibility
Accrual to the protocol commenced after institutional research ethics approval was granted. Eligible patients had pathologically-confirmed newly diagnosed SCLC with chest-confined disease at the time of diagnosis, adequate pulmonary function tests (FEV-1 >1.0 L, DLCO > 50%), age at least 18 years, Karnofsky Performance Status ≥ 70, undergoing concurrent chemoradiotherapy, and signed a study-specific consent form. Patients were excluded if they had insufficient renal function to have IV contrast for CT scans (creatinine clearance < 60 ml/minute), as patients required adequate renal function to metabolize IV constrast used for planning CT scans. Study patients could not have any kind of surgical resection for their lung cancer. If study patients had had a previous non-superficial skin cancer, they had to be disease-free for at least 5 years at the time of study enrollment. Study patients could not have had any kind of chest radiotherapy in the past and had to have a minimum forced vital capacity of 1.0 litre and diffusion capacity of carbon monoxide of 50% on pre-radiotherapy pulmonary function testing. Pregnant patients and/or those with pleural or pericardial effusions caused by their lung cancer were excluded.
Pretreatment evaluations
Pre-RT evaluations included complete history and physical examination, CT scan of the thorax and abdomen, bone scan, CT or MRI brain and pulmonary function tests, with FDG-PET at the discretion of the oncologist. If a staging PET scan was performed, the bone scan was not required.
Chemotherapy
Patients were prescribed 4 cycles of platinum-based (cisplatin or carboplatin) chemotherapy according to institutional tumor group treatment guidelines. Choice of specific platinum agent and chemotherapy dose reductions and delays were carried out at the medical oncologist's discretion.
Thoracic radiotherapy
Study patients commenced thoracic RT concurrent with as early a chemotherapy cycle as logistically possible and no later than the start of the second chemotherapy cycle. Adaptive radiotherapy was given on this trial based on three separate planning CT scans obtained for each study patient. Planning scans were obtained prior to starting radiotherapy, days 5 and 10 of radiotherapy. This planning CT scan schedule is based on our previously-published data which demonstrated the majority of SCLC tumors shrinkage occuring during the first 2 weeks of concurrent chest radiotherapy [14]. In this study we found the amount of tumor shrinkage occuring after the first 2 weeks of radiotherapy to be minimal and as such did not feel that for the current study adapting a radiotherapy plan after the first 2 weeks of radiotherapy would provide any significant dosimetric benefits.
All planning CT scans were obtained with IV contrast along with a 4D CT on a Philips Brilliance Big Bore spiral CT in 3 mm slices. Planning CT scans were transferred to a Varian Eclipse treatment planning station (Varian Medical Systems) for target volume and critical structure definition. The gross tumor volume (GTV) was defined as all visible disease as seen on the free-breathing portion of each planning CT scan, including pathologic-sized lymph nodes (greater than 1.0 cm in short axis measurement). Free breathing scans were merged with their corresponding 4D-CT scans to create an internal target volume (ITV). The ITV was expanded isotropically by 10 mm to define the clinical target volume (CTV) and account for microscopic extension of tumor beyond what is seen on the planning CT scan. Each CTV was edited to respect anatomic boundaries such as bone or vasculature. The edited CTV on each planning scan was expanded by 5 mm isotropically to define a planning target volume (PTV) which accounted for daily set-up variations. Spinal cord, heart, esophagus and lungs were contoured for each patient’s radiotherapy plan as critical normal structures.
Volumes of GTV, ITV, CTV and PTV were generated from each of the 3 planning scans done for each study patient. Radiotherapy planning was performed using forward-planned 3D conformal techniques. The PTV was covered with the 93% isodose as a minimum level of coverage. Megavoltage equipment with effective photon energies ≥ 6 MV was used for treatment. The dose was prescribed to the isocentre of a conformal treatment plan (ie. the ICRU50 reference point), centered on the PTV. In homogeneity in the target volume was kept ± 7%. Thoracic RT planning dose distributions were corrected for tissue heterogeneities. Weekly verification films were reviewed by the treating physician.
1400 cGy/7 daily fractions was prescribed based on the pre-RT planning scan. Fractions 8-12 were planned and delivered based on target volumes generated from the second planning CT scan (ie. the planning CT scan performed on day 5 of RT). 1000 cGy/5 fractions was prescribed for fractions 8-12. The remainder of the chest radiotherapy was planned based on target volumes generated from the third planning CT scan (ie. the planning CT scan obtained on day 10 of RT). The final RT prescription was determined by an analysis of anticipated cumulative RT doses to critcial structures.
RT planning dose constraints for normal critical structures were based largely on Emami's published TD 5/5 values [15]. Added cumulative dose plans for each study patient were obtained by applying each planned phase of radiotherapy to each patient's original planning CT image set. Patients whose RT planning could not meet the defined normal structure dose constraints were excluded from the study. RT planning dose constraints are summarized in table 1.
![]()
Table 1: Radiotherapy planning dose constraints.
View Table 1
Off-line planning comparison
Separate non-adaptive RT plans were created using each patient's original planning CT scan. The final total RT dose prescribed for each patient using their adaptive RT plans was applied to the plan used for fractions 1-7. The final adaptive cumulative dose plan for each patient was compared with the mock plan created using each patients' original CT scan. The maximum prescribable RT dose for each patient was determined if one was restricted to planning with the original planning CT only (ie. using a non-adaptive approach). Dose volume histogram comparisons between the non-adapted and adapted plans were performed with respect to: prescribed total dose, lung dose, cord dose, esophagus dose and heart dose.
Prophylactic cranial irradiation (PCI)
All study patients underwent follow-up CT chest/abdomen, bone scan and CT head 4 weeks after chemoradiotherapy completion. As per standard clinical practice guidelines for this patient population, PCI was offered to study patients if they achieved at least a partial response to concurrent chemoradiotherapy. The PCI dose-fractionation was 25 Gy/10 fractions using parallel-opposed right and left lateral fields to encompass the whole brain planning target volume. PCI was administered 4-6 weeks after completion of concurrent chemoradiotherapy.
Patient evaluations and follow-up
Patients were evaluated weekly during RT by their radiation oncologist for toxicity assessment. Toxicity data was recorded as per the National Cancer Institute (NCI) Common Toxicity Criteria for Adverse Events (CTCAE) v4.0. Acute events were defined as side effects that occur less than 90 days from the start of radiation, and late events occurred after 90 days from the start of radiation, or persisted beyond 90 days.
Patients were assessed one month after completion of RT, then every 3 months until 2 years, then every 6 months up to 5 years. At each post-RT visit patients underwent a history and physical examination and chest x-ray. Each follow-up history focussed on symptoms of an intrathoracic disease recurrence (eg. increased cough, shortness of breath, hemoptysis, dysphagia, odynophagia or chest pain) or RT-related toxicity. CT scan of the chest was obtained 4-6 weeks after completing chemoradiotherapy treatments, then every 6 months for 2 years and then annually to year 5. Additional CT, MRI or nuclear imaging scans were performed at the physician's discretion based on clinical suspicion. All study patients were followed until death.
Patients diagnosed with disease recurrence after undergoing chemoradiotherapy were managed as per institutional tumor group practice guidelines. Any salvage chemotherapy treatments were prescribed and supervised by a medical oncologist. Further palliative RT was administered if clinically indicated and technically feasible.
Study endpoints and statistics
The primary endpoint was the differences in 1) total accumulated dose deliverable to the planning target volume and 2) accumulated doses to critical structures of spinal cord, heart, normal lung and esophagus when comparing adaptive versus non-adaptive RT plans. Secondary endpoints were acute RT toxicity, local control, patterns of failure and overall survival. Disease free and overall survival were measured from the day patients consented to participate in the study.
The primary objective of this study was to quantify the dosimetric advantages of incorporating an adaptive RT planning approach for LS-SCLC patients undergoing chemoradiotherapy treatments. Specifically, adaptive RT plans used to treat study patients were compared to mock non-adaptive plans on the basis of:
1) Total safe prescribable dose
2) Doses to normal critical structures (cord, normal lung, esophagus, heart). For this pilot study, we aimed to accrue 10 patients.
Results
Patient characteristics
Ten eligible patients signed study-specific consent to participate in the protocol. Median age was 62.5 years (range 57-80 years). Patient characteristics, chemotherapy regimens used, and treatment responses are summarized in table 2.
![]()
Table 2: Chemotherapy and response details.
View Table 2
Treatment compliance
All patients completed both adapted RT and chemotherapy. 90% of patients required at least one delay in their chemotherapy due to grade 3 or greater neutropenia. No patients received a dose reduction in their chemotherapy. Eight patients received cisplatin with etoposide for 4 cycles and two were prescribed carboplatin in lieu of cisplatin due to pre-existing hearing loss. Radiation was initiated for all patients by cycle 2 of chemotherapy. Eight patients had a partial response to therapy, and two had a complete response. All patients received PCI.
Tumor and target volume changes during RT
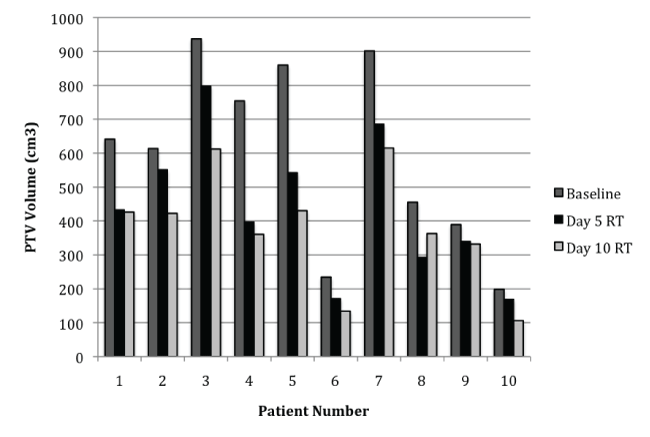
Mean GTV volume reduction between CT-1 and CT-3 was 51.7% (range 39.6-63.8%). The mean GTV was 131.3cc on baseline scan, regressing to 58.1cc at CT-3. Mean PTV volume was reduced by 35.8% between CT-1 and CT-3 (range 27-44.6%), and mean initial PTV volume was 598.6cc and regressing to 380.2cc. Individual patients’ GTV and PTV volumes measured during the course of radiotherapy are summarized in table 3 and figure 1.
![]()
Table 3: Volume characteristics.
View Table 3
Maximum prescribable dose and critical structure tolerence
Maximum prescribable RT doses in the adaptive and non-adaptive plans are presented in table 3. Median safe total prescribe dose in the adaptive plans was 60 Gy (range 28-70 Gy) versus 47 Gy (range 24-70 Gy) in the mock non-adaptive plans. Lung dose was the factor that limited the total prescribed RT dose for each patient. When the final prescribed RT dose was applied to both adaptive and non-adaptive plans, the adaptive plans provided significantly reduced V20 (mean 31% vs. 36%, p = 0.009), mean lung dose (14.7 Gy vs. 17.3 Gy, p = 0.009), and dose to 1/3 of the esophagus (median 35 Gy vs. 49 Gy, p = 0.03).
Treatment toxicities
There were no RT-related deaths. The maximum acute RT toxicity was grade 2 acute RT esophagitis which occurred in 5 patients. Five other patients experienced grade 1 RT esophagitis. Maximum individual acute RT toxicities are summarized in table 3. There were no pulmonary toxicities observed. All cases of grade 1 or 2 acute RT esophagitis completely resolved after thoracic RT completion. No patients had grade 3 or greater radiation-related toxicity.
Patterns of failure
There have been seven recurrences. Two recurrences were isolated within the chest. Patient 2 recurred in the hilum. This was considered a local failure outside of the irradiated field. Patient 3 recurred in the mediastinum; this was considered an infield recurrence. The other five recurrences were purely distant: 1 adrenal (Patient 7), 1 brain (Patient 6), 2 liver (Patients 5 and 8) and 1 brain/liver (Patient 4). At the time of recurrence, management consisted of palliative chemotherapy (2 patients), palliative RT (2 patients), or supportive care alone (3 patients). At the latest follow-up point, Patients 1 (treated to 70 Gy), 9 (treated to 60 Gy) and 10 (treated to 70 Gy) were recurrence-free.
Survival
Median follow-up was 23.7 months. The median progression-free survival was 13.4 months and median overall survival was 16.1 months.
Discussion
Treatment for limited- stage SCLC remains challenging and patient outcomes remain poor, despite contemporary chemoradiotherapy treatments. Incremental gains in local control and overall survival have been provided by addition of chest radiotherapy to chemotherapy and subsequent prophylactic cranial radiotherapy. RT dose intensification enhances these benefits albeit at the price of RT toxicity such as esophagitis [9].
Our group has quantified the dramatic regression rates in LS-SCLC tumor volumes that occur during a course of chemoradiotherapy [14]. Modern advanced RT planning and delivery technology featuring treatment units coupled with imaging capability has enabled the paradigm of adaptive RT whereby RT plans are adjusted during the course of therapy to accomodate for observed changes in tumor volume position and/or size [12]. This adaptive RT strategy has been implemented for treatment of certain tumors which change rapidly in size/configuration, require a high dose of radiotherapy but are in close proximity to normal critical structures such as head and neck squamous cell cancers [16]. SCLC may be another tumor site for such a strategy given the rapid anatomic changes SCLC tumors undergo during therapy and requirement of a high RT dose.
This clinical trial was initiated to exploit the rapid volume changes SCLC tumors exhibit during chemoradiotherapy treatments with an adaptive radiotherapy strategy in an attempt to achieve higher RT dose delivery without exposing patients to excessive RT toxicities. Our data demonstrates an adaptive RT strategy for SCLC is feasible and facilitates delivery of higher RT doses to target volumes while maintaining acceptable radiotherapy doses to normal critical structures compared to conventional RT planning based on one static CT dataset.
Our trial is to our knowledge the first reported prospective evaluation of the clinical implementation of adaptive radiotherapy planning for small cell lung cancer. Previously published planning studies of adaptive RT for lung cancer focused primarily on NSCLC (non-small cell lung cancer) patient cases and reported modest changes in tumor volumes occurring during treatments and inconsistent dosimetric gains [13,17-21]. Spoelstra's planning study included 21 NSCLC and 3 SCLC cases and reported only a mean reduction in PTV volume of 8% (only one patient experiencing a > 20% drop in PTV volume), reflecting the lower radio- and chemo-sensitivity of NSCLC tumors [20]. Conversely we previously reported and observed in the present study a much higher reduction in PTV volumes (mean 35.8%) during the course of therapy which better facilitated adaptation of our RT plans to achieve dose escalation without overdosing normal critical structures. In this study, we observed a 51.7% reduction in GTV volume and 35.8% reduction in PTV volume after two weeks of treatment, compared to baseline. These dramatic volume reductions facilitated dose escalation via an adaptive radiotherapy planning approach featuring re-planning during the times of maximal volume reduction. Delays in chemotherapy and type of platinum chemotherapy may have affected tumor shrinkage. The least amount of GTV change was seen with the two patients who received carboplatin in lieu of cisplatin, however, our study is not powered to determine a significant difference in tumor regression depending on chemotherapy used.
The primary end point of this study was to quantify the dosimetric advantages of an adaptive radiotherapy strategy in limited stage SCLC. The feasibility of adaptive radiation for SCLC was validated in this study, with all patients able to complete all planning scans and receive RT without any breaks for adaptive planning. We found that significantly higher RT doses were safely deliverable in adapted plans compared to non-adapted plans. Adapted plans also had significantly lower RT doses to lung and esophagus, which are the usual dose-limiting structures in small cell lung cancer radiotherapy [7,9].
There is a potential to under dose microscopic disease while adjusting RT portals in an adaptive plan. We observed no disease failures in a region which a radiotherapy field edge was moved away from as a visible tumor volume shrunk, but given our small sample size, failure pattern outcomes from more patients treated in this fashion need to be assessed before definitive conclusions can be made about the potential of under dosing microscopic disease. Furthermore, PET imaging may aid in defining more accurate target volumes in SCLC.
Published evidence indicates that giving concurrent chest RT as early as possible with chemotherapy confers better outcomes [22,23]. Many SCLC patients are not eligible for a radical dose of chest RT or any chest RT at all due to extent of intrathoracic disease as a result of bulky disease, atelectasis, or pleural effusion present at the time of diagnosis. These patients therefore lose the local control and survival benefits conferred by early concurrent chest RT and usually are treated with non-curative treatments.
The adaptive RT approach we report here may make concurrent chest RT a feasible option for SCLC patients who before were felt to be ineligible for chest RT (pleural effusion, atelectasis, bulky intrathoracic disease) at the time of diagnosis. Delivery of concurrent chest RT to this patient group may perhaps improve local control and survival for this group of patients who usually have a grim prognosis [24]. Additionally, given the evidence that RT dose escalation/intensification improves outcomes for SCLC, utilizing an adaptive method for SCLC chest RT may facilitate safe delivery of higher RT doses for patients who previously may not have been eligible to receive a high dose of chest RT.
The three patients in our study cohort who are free of cancer recurrence received 70, 60 and 70 Gy, facilitated through our adaptive RT planning approach. This trend is consistent with the published evidence indicating an existence of a RT dose response curve for small cell lung cancers [10], but with a patient cohort of ten, we could not find any statistical significance to this trend in our data.
This pilot study demonstrated that 90% of our patients were able to receive dose escalated RT via an adaptive RT plan, with a 20% complete, and 80% partial response rate. However, our observed median overall survival in this cohort was only 16.1 months, which is at the low end of the range of quoted median survival outcomes for LS-SCLC. However, many patients in our cohort had very large intrathoracic tumor volumes at the time of diagnosis and traditionally would have been considered to have a target volume un-encompassable with a radiotherapy portal and therefore by definition to have extensive stage disease and ineligible for a full radical dose of thoracic RT concurrent with their chemotherapy. Our institution guideline recommends a dose of 50 Gy delivered in 25 daily fractions with concurrent chemotherapy to small cell lung cancer patients treated with curative intent. By this measure, six of the patients in our study cohort would have only been eligible for a sub-optimal radiotherapy dose less than 50 Gy if radiotherapy planning was done based on the size of their pre-treatment tumor volume. Inclusion of such patients in our study cohort likely skewed our observed survival outcomes.
Randomized chemotherapy trials where patients with extensive stage small cell lung cancer were treated with chemotherapy alone demonstrate poorer outcomes to our patient cohort with median survivals ranging from 9.4-12.8 months [25,26]. Small cell lung cancer patients treated with chemotherapy alone uniformly experience chest recurrences, and despite these dismal outcomes for patients with advanced small cell lung cancer, the addition of early concurrent chest radiotherapy, optimized through an adaptive radiotherapy planning approach, may at least improve their local control rates and quality of life, particularly from a pulmonary standpoint. A recent randomized trial investigating addition of post-chemotherapy consolidation chest radiotherapy in extensive stage small cell lung cancer patients reported a median survival of 8 months in both patient arms [27]. We reported a similar median survival of 8.3 months in extensive stage small cell lung cancer patients treated with post-chemotherapy consolidative chest radiotherapy from a previous institutional clinical trial [28].
Our patient cohort in this present study is a unique group that does not have overt distant metastases, but at the same time have bulky intrathoracic tumors that usually are not considered to represent limited stage disease. These patients possibly would benefit from chest radiotherapy given with an adaptive approach to provide better local control and potentially improve their survival compared to if they were only treated with chemotherapy alone or even post-chemotherapy consolidative chest radiotherapy. This hypothesis requires further investigation in future clinical trials properly powered to answer this question.
Conclusion
Adaptive radiotherapy is a feasible radiotherapy planning technique for small-cell lung cancer treatment and facilitates delivery of higher RT doses to target volumes compared with a non-adaptive approach. Compared with non-adaptive plans, adapted plans conferred improved dosimetry to critical structures of lung and esophagus. Further research into the use of adaptive radiotherapy is warranted based on this initial pilot study as it may allow for radiotherapy dose escalation in small-cell lung cancer patients, particularly among those patients with bulky intrathoracic disease.
Acknowledgements
This research was funded through a grant from the Alberta Cancer Foundation.
Potential Conflicts of Interest
None
References
-
Warde P, Payne D (1992) Does thoracic irradiation improve survival and local control in limited-stage small-cell carcinoma of the lung? A meta-analysis. J Clin Oncol 10: 890-895.
-
Pignon JP, Arriagada R, Ihde DC, Johnson DH, Perry MC, et al. (1992) A meta-analysis of thoracic radiotherapy for small-cell lung cancer. N Engl J Med 327: 1618-1624.
-
Gaspar LE, Gay EG, Crawford J, Putnam JB, Herbst RS, et al. (2005) Limited-stage small-cell lung cancer (stages I-III): observations from the National Cancer Data Base. Clin Lung Cancer 6: 355-360.
-
Fried DB, Morris DE, Poole C, Rosenman JG, Halle JS, et al. (2004) Systematic review evaluating the timing of thoracic radiation therapy in combined modality therapy for limited-stage small-cell lung cancer. J Clin Oncol 22: 4837-4845.
-
Yee D, Hanson J, Butts C, Reiman A, Joy A, et al. (2010) Phase I dose escalation trial of hypofractionated limited-field external beam thoracic radiotherapy for limited-stage small cell carcinoma of the lung. Radiother Oncol 96: 78-83.
-
Komaki R, Paulus R, Ettinger DS, Videtic GM, Bradley JD, et al. (2012) Phase II study of accelerated high-dose radiotherapy with concurrent chemotherapy for patients with limited small-cell lung cancer: Radiation Therapy Oncology Group protocol 0239. Int J Radiat Oncol Biol Phys 83: e531-536.
-
Choi NC, Herndon JE 2nd, Rosenman J, Carey RW, Chung CT, et al. (1998) Phase I study to determine the maximum-tolerated dose of radiation in standard daily and hyperfractionated-accelerated twice-daily radiation schedules with concurrent chemotherapy for limited-stage small-cell lung cancer. J Clin Oncol 16: 3528-3536.
-
Arvidson NB, Khuntia D, Tomé WA (2009) Dose escalation model for limited-stage small-cell lung cancer. Radiother Oncol 91: 379-385.
-
Turrisi A Tr, Kim K, Blum R, Sause WT, Livingston RB, et al. (1999) Twice-daily compared with once-daily thoracic radiotherapy in limited small-cell lung cancer treated concurrently with cisplatin and etoposide. N Engl J Med 340: 265-271.
-
Choi NC, Carey RW (1989) Importance of radiation dose in achieving improved loco-regional tumor control in limited stage small-cell lung carcinoma: an update. Int J Radiat Oncol Biol Phys 17: 307-310.
-
Papac RJ, Son Y, Bien R, Tiedemann D, Keohane M, et al. (1987) Improved local control of thoracic disease in small cell lung cancer with higher dose thoracic irradiation and cyclic chemotherapy. Int J Radiat Oncol Biol Phys 13: 993-998.
-
Dawson LA, Sharpe MB (2006) Image-guided radiotherapy: rationale, benefits, and limitations. Lancet Oncol 7: 848-858.
-
Kataria T, Gupta D, Bisht SS, Karthikeyan N, Goyal S, et al. (2014) Adaptive radiotherapy in lung cancer: dosimetric benefits and clinical outcome. Br J Radiol 87: 20130643.
-
Yee D, Rathee S, Robinson D, Murray B (2011) Temporal lung tumor volume changes in small-cell lung cancer patients undergoing chemoradiotherapy. Int J Radiat Oncol Biol Phys 80: 142-147.
-
Emami B, Lyman J, Brown A, Coia L, Goitein M, et al. (1991) Tolerance of normal tissue to therapeutic irradiation. Int J Radiat Oncol Biol Phys 21: 109-122.
-
Chen AM, Daly ME, Cui J, Mathai M, Benedict S, et al. (2014) Clinical outcomes among patients with head and neck cancer treated by intensity-modulated radiotherapy with and without adaptive replanning. Head Neck 36: 1541-1546.
-
Ding XP, Zhang J, Li BS, Li HS, Wang ZT, et al. (2012) Feasibility of shrinking field radiation therapy through 18F-FDG PET/CT after 40 Gy for stage III non-small cell lung cancers. Asian Pac J Cancer Prev 13: 319-323.
-
Gillham C, Zips D, Pönisch F, Evers C, Enghardt W, et al. (2008) Additional PET/CT in week 5-6 of radiotherapy for patients with stage III non-small cell lung cancer as a means of dose escalation planning? Radiother Oncol 88: 335-341.
-
Guckenberger M, Kavanagh A, Partridge M (2012) Combining advanced radiotherapy technologies to maximize safety and tumor control probability in stage III non-small cell lung cancer. Strahlenther Onkol 188: 894-900.
-
Spoelstra FO, Pantarotto JR, van Sornsen de Koste JR, Slotman BJ, Senan S (2009) Role of adaptive radiotherapy during concomitant chemoradiotherapy for lung cancer: analysis of data from a prospective clinical trial. Int J Radiat Oncol Biol Phys 75: 1092-1097.
-
Weiss E, Fatyga M, Wu Y, Dogan N, Balik S, et al. (2013) Dose escalation for locally advanced lung cancer using adaptive radiation therapy with simultaneous integrated volume-adapted boost. Int J Radiat Oncol Biol Phys 86: 414-419.
-
Pijls-Johannesma M, De Ruysscher D, Vansteenkiste J, Kester A, Rutten I, et al. (2007) Timing of chest radiotherapy in patients with limited stage small cell lung cancer: a systematic review and meta-analysis of randomised controlled trials. Cancer Treat Rev 33: 461-473.
-
De Ruysscher D, Pijls-Johannesma M, Bentzen SM, Minken A, Wanders R, et al. (2006) Time between the first day of chemotherapy and the last day of chest radiation is the most important predictor of survival in limited-disease small-cell lung cancer. J Clin Oncol 24:1057-1063.
-
Møller DS, Khalil AA, Knap MM, Hoffmann L (2014) Adaptive radiotherapy of lung cancer patients with pleural effusion or atelectasis. Radiother Oncol 110: 517-522.
-
Noda K, Nishiwaki Y, Kawahara M, Negoro S, Sugiura T, et al. (2002) Irinotecan plus cisplatin compared with etoposide plus cisplatin for extensive small-cell lung cancer. N Engl J Med 346: 85-91.
-
Murray N, Livingston RB, Shepherd FA, James K, Zee B, et al. (1999) Randomized study of CODE versus alternating CAV/EP for extensive-stage small-cell lung cancer: an Intergroup Study of the National Cancer Institute of Canada Clinical Trials Group and the Southwest Oncology Group. J Clin Oncol 17: 2300-2308.
-
Slotman BJ, van Tinteren H, Praag JO, Knegjens JL, El Sharouni SY, et al. (2015) Use of thoracic radiotherapy for extensive stage small-cell lung cancer: a phase 3 randomised controlled trial. Lancet 385: 36-42.
-
Yee D, Butts C, Reiman A, Joy A, Smylie M, et al. (2012) Clinical trial of post-chemotherapy consolidation thoracic radiotherapy for extensive-stage small cell lung cancer. Radiother Oncol 102: 234-238.