International Journal of Radiology and Imaging Technology
Inferior Mesenteric Arteriovenous Malformation Presenting as Ischemic Colitis After an Acute Episode of Campylobacter Jejuni Colitis
Roy Hajjar1*, Patrick Gilbert2, Marie-France Giroux2, Frank Schwenter1 and Herawaty Sebajang1
1Département de chirurgie oncologique, Centre hospitalier de l'Université de Montréal (CHUM), Hôpital Notre-Dame, Québec, Canada
2Département de radiologie, Centre hospitalier de l'Université de Montréal (CHUM), Hôpital Notre-Dame, Québec, Canada
*Corresponding author:
Roy Hajjar, M.D., Resident Doctor in General Surgery, Département de chirurgie oncologique, Centre hospitalier de l'Université de Montréal (CHUM), Hôpital Notre-Dame, Montréal, Québec, Canada, Tel: 438-989-8113, E-mail: roy.hajjar@umontreal.ca
Int J Radiol Imaging Technol, IJRIT-3-021, (Volume 3, Issue 1), Case Report
Received: September 12, 2016 | Accepted: January 09, 2017 | Published: January 12, 2017
Citation: Hajjar R, Gilbert P, Giroux MF, Schwenter F, Sebajang H (2017) Inferior Mesenteric Arteriovenous Malformation Presenting as Ischemic Colitis After an Acute Episode of Campylobacter Jejuni Colitis. Int J Radiol Imaging Technol 3:021.
Copyright: © 2017 Hajjar R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
An arteriovenous malformation (AVM) of the inferior mesenteric artery is a rare entity that could be associated with ischemia. We present the case of a 54-year-old male with ischemic colitis after an acute episode of Campylobacter jejuni colitis. A computed tomography (CT) angiography confirmed the presence of an AVM in the inferior mesenteric vascular region, probably causing the ischemia through a steal phenomenon. After embolization of the incriminated vessels in conventional angiography, a surgical resection was necessary because of an aggravation of the ischemic process. To the best of our knowledge, this is the first reported case of an AVM-associated ischemic colitis appearing in the context of an acute bacterial gastrointestinal infection. We question the possible role of infectious colitis in the exacerbation of ischemic colitis in patients with AVMs.
Keywords
Mesenteric arteriovenous malformation, Campylobacter jejuni, Ischemic colitis
Introduction
Arteriovenous malformations (AVMs) are aberrant vascular connections between the arterial and venous vascular beds, with a relatively direct blood passage from the communicating afferent arteries to the efferent vein(s) [1-3]. These abnormal networks are believed to be congenital, usually in the form of a fine network of arteriovenous communications (the so-called nidus) with hypertrophied feedings arteries, arteriovenous shunting and dilated draining vein(s) [1-4]. Although AVMs on cutaneous or epithelial surfaces can be clinically evident, their presence in the intra-abdominal cavity, in the mesenteric vascular network for instance, can make them asymptomatic. Their initial clinical manifestation can thus be in the form of bleeding, ischemia or portal hypertension [1-7].
Mesenteric ischemia is due to an inadequate blood supply to the bowel, usually because of an embolic or thrombotic obstruction of the arterial blood flow [8]. It can less frequently be related to a non-occlusive cause [8]. Impaired large bowel perfusion can lead to ischemic colitis with either partial or full thickness involvement of the colonic wall [9].
Campylobacter jejuni enterocolitis is usually caused by ingestion of contaminated food [10]. In this bacterial infection, the germ adheres to, and invades, the epithelial cells of the host [11]. Its clinical presentation ranges from a self-limiting watery diarrhea to a more severe form of bloody stool, and even toxic megacolon in the most serious cases [10]. It is usually treated with antibiotic therapy [10]. Infectious colitis has not been previously associated with exacerbation of an AVM-associated ischemia.
Case Presentation
A 54-year-old man was evaluated for abdominal pain, tenesmus and bloody diarrhea. The medical history of this non-smoking patient comprises asthma, gastroesophageal reflux disease (GERD), dyslipidemia and high blood pressure, all well controlled with standard drug therapies. A latent tuberculosis infection was previously treated with Isoniazid until 3 months before his symptoms began. Neither the patient nor his family had a history of ischemic or inflammatory bowel disease.
While in a travel to a South American country, the patient began to complain of bloody diarrhea and left lower abdominal pain. Having previously experienced traveler's diarrhea, the patient started an empirical antibiotic treatment, without complete recovery of the symptoms. When back to the country, stool samples revealed the presence of Campylobacter jejuni that was treated with azithromycin, and then changed to doxycycline in order to accommodate the antibiogram's results. Although his diarrhea and rectal bleeding had resolved, significant tenesmus and localized left lower abdominal pain persisted.
History did not reveal any chronic symptoms suggestive of a possible inflammatory bowel disease. A first colonoscopy revealed a non-specific colitis affecting the last 35 cm of the rectosigmoid colon. Biopsies of the affected area revealed, unexpectedly, histological findings of dilated blood vessels, thickened subepithelial collagen band and vascular congestion, suggestive of an ischemic phenomenon rather than an infectious one. No ulcers, dysplasia or other chronic pathological signs of inflammatory bowel disease were identified. The patient was meanwhile hospitalized for management of a persistent pain and for further investigation his symptoms' etiology. A second colonoscopy was performed less than a month after the first one, with a slight macroscopic improvement and microscopic findings consistent with the first one. A CT angiography revealed adequate permeability of the mesenteric arterial vessels. Venous dilations where however noticed in the left lower abdominal quadrant along with circumferential thickening of the rectosigmoid colon.
The patient was transferred to an academic center for further evaluation and management of a possible vascular malformation with conventional angiography. A CT angiography was performed and revealed an AVM consisting of several branches originating from the inferior mesenteric artery with an arteriovenous shunting phenomenon and early filling of the inferior mesenteric vein.
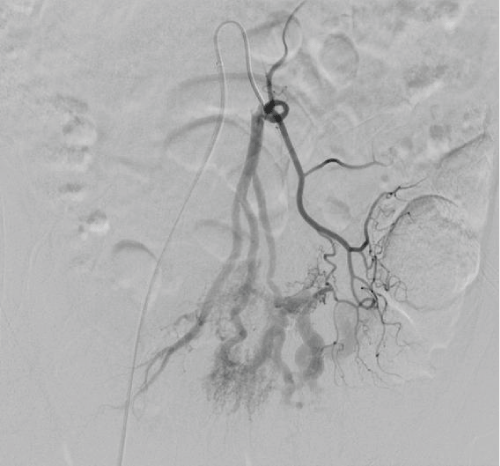
The patient underwent angiographic embolization of the inferior mesenteric artery branches contributing to the malformation with the Onyx technology (Figure 1 and Figure 2). Onyx was chosen as AVMs are usually embolized with pure alcohol in our hospital but this was deemed dangerous with a risk of sigmoid perforation. A 4th lateral branch was not embolized because of a vasospasm that occurred during the procedure. The patient was closely followed for symptoms or signs of recurrent or exacerbating ischemia. The next day, his abdominal pain significantly increased and was unbearable despite lidocaine and ketamine infusions, and rebound tenderness in the left iliac fossa was noted. Acute or chronic ischemic colitis was highly suspected and a surgical exploration was performed, which showed a gray-colored unperforated distal sigmoid with a thickened mesentery, suggesting a chronic ischemic process. A Hartmann's procedure was performed. Pathologic evaluation of the resected colon showed parietal ischemic necrosis with vascular congestion in the rest of the colonic wall. No dysplastic or neoplastic lesions were noted.
.
Figure 1: The selective inferior mesenteric arteriogram shows 4 branches feeding the sigmoid, three of which are increased in size, and giving vascularization to the so-called "nidus" of the AVM, detected as a very small network of anarchic arteries, shunting into dilated venules on this precocious arteriography.
View Figure 1
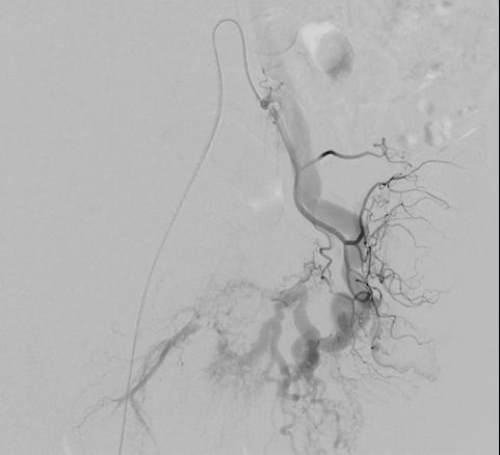
.
Figure 2: A slightly more delayed picture of the same arteriogram shows the importantly dilated sigmoid venules and inferior mesenteric vein even though the normal arterial branch is still opacified, further showing the arteriovenous shunting.
View Figure 2
Six days after the procedure, the patient had fever. An abdominal CT was performed, and its findings included portal vein thrombosis of the 8th hepatic segment. Dense material was identified in that vein, probably corresponding to fragments of embolized Onyx that had migrated through the inferior mesenteric vein into a terminal portal branch secondary to surgical manipulation of the embolized region. This material was visible on the first CT performed after the surgery but not on a preoperative CT obtained after the embolization. The patient was discharged after a postoperative hospitalization lasting 23 days.
Discussion
We report the case of a patient with a chronic ischemic colitis due to an AVM-associated steal phenomenon that seems to be triggered by a Campylobacter jejuni infection. Arteriovenous malformations of the inferior mesenteric artery are a rare entity with only few reported cases [1,3,4,12]. To the best of our knowledge, less than 40 cases of inferior mesenteric arteriovenous malformations (AVMs) or fistulas (AVFs) are reported in the literature [1-7,12-40]. Complications related to this vascular aberration are even scarcer, with only 19 previous possible cases of ischemic colitis being reported as a consequence of the ensuing abnormal arterial blood flow [1-4, 6,7,12,14-25]. AVMs are believed to be congenital, but acquired forms, sometimes identified as fistulas, are usually due to surgical procedures or traumatic injuries [1-4]. Despite the anatomopathological difference between anomalies, the clinical significance and general management can be comparable, and no evident distinction is always made between them in the literature [2].
The differential diagnosis of abdominal pain, rectorragia and tenesmus in this context is extensive. In addition to infectious causes that were ruled out with negative cultures after antibiotic treatments, inflammatory bowel disease (IBD) had to be investigated. The literature does not seem to correlate gastrointestinal infections to IBD flare-ups, with antibiotics having even a protective effect against Crohn's disease [41-43]. The results of colonoscopies and biopsies did not raise suspicion for IBD. The pain that was out of proportion for the physical examination in a hemodynamically stable patient suggested an ischemic phenomenon rather than an inflammatory disease. The patient did not have past history of abdominal trauma or intra-abdominal surgeries suggestive of an AVF rather than an AVM. The angiographic images were also typical of an AVM and not an AVF, which was most probably a congenital malformation.
To our knowledge, colonic infectious episodes have not been previously linked to AVM-associated ischemic colitis. This raises the question of the possible effect of infectious events on the delicate balance that colonic vasculature attempts to maintain in blood flow to the left and sigmoid colon. An obvious causal relation between Campylobacter jejuni and AVM-associated ischemic colitis is not easy to establish. We assume that infectious gastrointestinal events induce a release of chemical mediators of inflammation. Nitric oxide (NO), which is an important inflammatory vasodilator and neurotransmitter, has been shown to be significantly increased in the rectal lumen of patients with infectious gastroenteritis [44,45]. The vasodilation induced by the infectious inflammatory response could therefore be rather deleterious in the case of AVM, as it will possibly worsen the arteriovenous shunt and venous congestion, in an already high-flow vascular bed. Moreover, increased vascular resistance in the portal system has been described in mesenteric AVMs, as a phenomenon better known as "hyperkinetic" portal hypertension [2]. We question thus the possible effect of this high-resistance phenomenon on the mesenteric venous outflow and consequently the arterial supply to the affected colonic segment. Besides, it has been suggested that a prolonged ischemia could probably eventually lead to vasoconstriction, worsening in this way the ischemic process [8,46]. A question mark is thus raised over the capacity of a fragile AVM to cope with the significant inflammatory response that a Campylobacter jejuni infection induces. From another perspective, Campylobacter jejuni has been associated with autoimmune manifestations such as reactive arthritis and Guillain-Barré syndrome [11]. Immune markers were suggested to be present in chronic ischemic colitis [47]. This raises once again the question on whether an immune response was elicited by the infectious process and disrupted the blood flow balance of an already fragile vasculature. Nevertheless, these assumptions remain purely hypothetical and have evidently yet to be further assessed and confirmed with experiments or observational physiological evidence.
As for diagnostic modalities, imaging techniques remain essential in the evaluation of the intestinal integrity and vascular supply as well as the intra-abdominal concomitant causes and/or complications of AVMs. CT angiography remains a fast and easily accessible imaging modality for the initial investigation of a possible mesenteric vascular abnormality. Poullos, et al. described the different imaging findings characterizing AVMs on CT and MR angiography [2]. As stated by the author, the feeding arteries can be "serpentine and hypertrophied" on CT angiography, with early filling of a prominent venous circulation, a finding that was objectified on our patient's abdomino-pelvic CT angiography [2]. This imaging modality allows also an assessment of the disease extent and of its potential complications' signs, such as pneumatosis, perforation, pneumoperitoneum, ascites, intra-abdominal fluid collections, pericolic fat infiltration, bleeding and the presence of possible atheromatosis in the affected vascular network. As for magnetic resonance angiography, it is a very helpful technique in the three-dimensional and real time representation of visceral AVMs [2]. However, despite its remarkable contrast resolution, MR angiography remains a less accessible imaging modality than CT angiography, with less spatial resolution. Also, it does not provide the therapeutic interventional advantage that conventional angiography grants.
The diagnosis of an AVM-associated ischemic colitis in the context of non-specific abdominal pain remains a challenge. As stated by Athanasiou, et al. proper diagnosis and management require a combination of clinical, imaging and intraoperative evidence of the ischemic process [3]. A high index of suspicion should be thus present whenever an ischemic phenomenon is suspected without obvious cardiovascular risk factors. Nonetheless, even when an AVM-associated ischemic colitis is diagnosed, a careful evaluation of the possible therapeutic options should be made. As expressed by Noor, et al. in a recent report of an AVM-associated ischemic colitis managed with sigmoid colectomy, embolization of the aberrant vessel is an alternative, which could however be associated with a bowel infarction risk [12]. Similarly, an ischemic process was already present in our patient as shown by CT angiography and pathological reports, but an acute post-embolization exacerbation warranted an emergent surgical resection. Nevertheless, embolization can still provide a useful adjunct to surgery, even in the setting of subsequent perforation, as it may help to prevent significant bleeding per-procedure. Consequently, embolization remains a less invasive option than surgical resection, but a close surveillance is essential to watch for the possible ischemic, hemorrhagic and/or thrombotic complications that can ensue.
Conclusion
AVM was repeatedly reported as a rare possible cause of ischemic colitis. Although infectious and inflammatory causes remain the most potential etiologies in healthy patients presenting with colitis, AVM-associated ischemia should be ruled out via appropriate imaging modalities, especially in those with persistent symptoms. If ischemic colitis is suspected, CT angiography is a fast, accessible and reliable assessment method, but conventional angiography remains the gold standard as it allows therapeutic interventions. We presented a case where an ischemic complication of the anomaly occurred after an infectious episode. This raises a question mark over a possible relationship between AVM-associated ischemia and bacterial colitis, though no previously proven causal association could be demonstrated. Future reports on similar presentations including the possible triggers or clinical context are required to clarify further the effect of gastrointestinal infections on colonic ischemia in patients with AVMs.
References
-
Türkvatan A, Ozdemir Akdur P, Akdoğan M, Cumhur T, Olçer T, et al. (2009) Inferiormesenteric arteriovenous fistula with ischemic colitis: multidetector computed tomographic angiography for diagnosis. Turk J Gastroenterol 20: 67-70.
-
Poullos PD, Thompson AC, Holz G, Edelman LA, Jeffrey RB (2014) Ischemic colitis due to a mesenteric arteriovenous malformation in a patient with a connective tissue disorder. J Radiol Case Rep 8: 9-21.
-
Athanasiou A, Michalinos A, Alexandrou A, Georgopoulos S, Felekouras E (2014) Inferior mesenteric arteriovenous fistula: case report and world-literature review. World J Gastroenterol 20: 8298-8303.
-
Gorospe EC, Leggett CL, Sun G (2012) Inferior mesenteric arteriovenous malformation: an unusual cause of ischemic colitis. Ann Gastroenterol 25: 165.
-
Okada K, Furusyo N, Sawayama Y, Ishikawa N, Nabeshima S, et al. (2002) Inferior mesenteric arteriovenous fistula eight years after sigmoidectomy. Intern Med 41: 543-548.
-
Capron JP, Gineston JL, Remond A, Lallement PY, Delamarre J, et al. (1984) Inferior mesenteric arteriovenous fistula associated with portal hypertension and acute ischemic colitis. Successful occlusion by intraarterial embolization with steel coils. Gastroenterology 86: 351-355.
-
Kamo M, Yagihashi K, Okamoto T, Nakamura K, Fujita Y, et al. (2016) High-Flow Vascular Malformation in the Sigmoid Mesentery Successfully Treated with a Combination of Transarterial and Transvenous Embolization. Cardiovasc Intervent Radiol 39: 1774-1778.
-
Clair DG, Beach JM (2016) Mesenteric Ischemia. N Engl J Med 374: 959-968.
-
Doulberis M, Panagopoulos P, Scherz S, Dellaporta E, Kouklakis G (2016) Update on ischemic colitis: from etiopathology to treatment including patients of intensive care unit. Scand J Gastroenterol 51: 893-902.
-
Ina K, Kusugami K, Ohta M (2003) Bacterial hemorrhagic enterocolitis. J Gastroenterol 38: 111-120.
-
O Cróinín T, Backert S (2012) Host epithelial cell invasion by Campylobacter jejuni: trigger or zipper mechanism? Front Cell Infect Microbiol 2: 25.
-
Noor M, Cooper K, Lujan H, Pena C (2016) Arteriovenous malformation of the inferior mesenteric artery presenting as ischemic colitis. Vasc Med 21: 555-557.
-
Van Way CW III, Crane JM, Riddell DH, Foster JH (1971) Arteriovenous fistula in the portal circulation. Surgery 70: 876-890.
-
Houdard C, Helenon C, Carles JF, Botella R, Favre M, et al. (1970) [Inferior mesenteric arteriovenous fistula and ulcerative rectocolitis]. Arch Fr Mal App Dig 59: 463-474.
-
Kamo M, Huwa S, Ishiyama M, Nozaki T, Onoda Y Oikado K (2012) A case of ischemic colitis caused by inferior mesenteric arteriovenous fistula. Japanese Journal of Clinical Radiology 57: 309.
-
Kim IH, Kim DG, Kwak HS, Yu HC, Cho BH, et al. (2008) Ischemic colitis secondary to inferior mesenteric arteriovenous fistula and portal vein stenosis in a liver transplant recipient. World J Gastroenterol 14: 4249-4252.
-
Akgun V, Sari S, Verim S, Bozlar U (2013) Arteriovenous malformation of the inferior mesenteric artery in a patient with ischaemic colitis. BMJ Case Rep 2013.
-
El Muhtaseb MS, Gorgun E, Liu M (2013) Arteriovenous malformation: a potential cause of ischaemic colitis. ANZ J Surg 83: 93-94.
-
Pietri J, Remond A, Reix T, Abet D, Sevestre H, et al. (1990) Arterioportal fistulas: twelve cases. Ann Vasc Surg 4: 533-539.
-
Metcalf DR, Nivatvongs S, Andrews JC (2008) Ischemic colitis: an unusual case of inferior mesenteric arteriovenous fistula causing venous hypertension. Report of a case. Dis Colon Rectum 51: 1422-1424.
-
Fabre A, Abita T, Lachachi F, Rudelli P, Carlier M, et al. (2005) Inferior mesenteric arteriovenous fistulas. Report of a case. Ann Chir 130: 417-420.
-
Plotkin E, Assis D, Boyer J (2013) Now you see it, now you don't. Hepatology 58: 446-447.
-
Doppl WE, Kuttner D, Stolte M, Breithecker A, Padberg W, et al. (2007) Clinical challenges and images in GI. Segmental ischemic colitis owing to vascular malformation of the inferior mesenteric artery. Gastroenterology 133: 15.
-
Hendy P, Cheng EH, Livsey R, Mortimore M (2015) Curative embolization of an inferior mesenteric arteriovenous fistula causing ischaemic proctosigmoiditis. ANZ J Surg.
-
Justaniah AI, Molgaard C, Flacke S, Barto A, Iqbal S (2013) Congenital inferior mesenteric arteriovenous malformation presenting with ischemic colitis: endovascular treatment. J Vasc Interv Radiol 24: 1761-1763.
-
Peer A, Slutzki S, Witz E, Abrahmsohn R, Bogokowsky H, et al. (1989) Transcatheter occlusion of inferior mesenteric arteriovenous fistula: a case report. Cardiovasc Intervent Radiol 12: 35-37.
-
Nemcek AA Jr, Yakes W (2005) SIR 2005 Annual Meeting Film Panel case: inferior mesenteric artery to inferior mesenteric vein fistulous connection. J Vasc Intervent Radiol 16: 1179-1182.
-
Matsui A, Iwai K, Kawasaki R, Wada T, Mito Y, et al. (2007) Transcatheter embolization of an inferior mesenteric arteriovenous fistula with frequent mucous diarrhea. Nihon Shokakibyo Gakkai Zasshi 104: 194-199.
-
Sabatier JC, Bruneton JN, Drouillard J, Elie G, Tavernier J (1978) [Inferior mesenteric arteriovenous fistula of congenital origin. A report on one case and review of the published literature (author's transl)]. J Radiol Electrol Med Nucl 59: 727-729.
-
Baranda J, Pontes JM, Portela F, Silveira L, Amaro P, et al. (1996) Mesenteric arteriovenous fistula causing portal hypertension and bleeding duodenal varices. Eur J Gastroenterol Hepatol 8: 1223-1225.
-
Oyama K, Hayashi S, Kogure T, Kirakawa K, Akaike A (1980) Inferior mesenteric arteriovenous fistula. Report of a case and review of the literature. Nihon Igaku Hoshasen Gakkai Zasshi 40: 944-950.
-
Hirner A, Haring R, Bost H, Sorensen R (1978) Hyperkinetic portal hypertension. Arterioportal fistula: problems-- case reports--review of the literature. Chirurg 49: 303-310.
-
Vauthey JN, Tomczak RJ, Helmberger T, Gertsch P, Fors- mark C, et al. (1997) The arterioportal fistula syndrome: clinicopathologic features, diagnosis, and therapy. Gastroenterology 113: 1390-1401.
-
Manns RA, Vickers CR, Chesner IM, McMaster P, Elias E (1990) Portal hypertension secondary to sigmoid colon arteriovenous malformation. Clin Radiol 42: 203-204.
-
Slutski S, Peer A, Abramsohn R, Weitz E, Bogokowsky H (1998) Early postoperative inferior mesenteric arteriovenous fistula-A case report. Vasc Endovascular Surg 22: 432-435.
-
Takahashi K, Kashida H, Kudo M (2012) Hepatic nodules associated with an inferior mesentric arteriovenous malformation. Intern Med 51: 2753-2755.
-
Bettenworth D, Rijcken E, Muller KM, Mosch-Messerich A, Heidemann J (2012) Rare cause of upper gastrointestinal bleeding in a 27-year-old male patient. Gut 61: 1367.
-
Faghihi Langroudi T, Shabestari AA, Pourghorban R, Pourghorban R (2015) Idiopathic inferior mesenteric arteriovenous fistula: a rare cause of pulsatile abdominal mass. Indian J Surg 77: 84-86.
-
Carbonell S, Ortiz S, Enriquez P, Lluis F (2014) Arteriovenous fistula in the inferior mesenteric territory. Cir Esp 92: e23.
-
Brucher N, Moskovitch G, Otal P, Chaufour X, Rousseau H (2014) Inferior mesenteric arteriovenous fistula treated by percutaneous arterial embolization: a breathtaking story! Diagn Interv Imaging 95: 85-86.
-
Aberra FN, Brensinger CM, Bilker WB, Lichtenstein GR, Lewis JD (2005) Antibiotic use and the risk of flare of inflammatory bowel disease. Clin Gastroenterol Hepatol 3: 459-465.
-
Singh S, Graff LA, Bernstein CN (2009) Do NSAIDs, antibiotics, infections, or stress trigger flares in IBD? Am J Gastroenterol 104: 1298-1313.
-
Bernstein CN, Singh S, Graff LA, Walker JR, Miller N, et al. (2010) A prospective population-based study of triggers of symptomatic flares in IBD. Am J Gastroenterol 105: 1994-2002.
-
Sharma JN, Al-Omran A, Parvathy SS (2007) Role of nitric oxide in inflammatory diseases. Inflammopharmacology 15: 252-259.
-
Herulf M, Svenungsson B, Lagergren A, Ljung T, Morcos E, et al. (1999) Increased nitric oxide in infective gastroenteritis. J Infect Dis 180: 542-555.
-
Boley SJ, Brandt LJ, Sammartano RJ (1997) History of mesenteric ischemia. The evolution of a diagnosis and management. Surg Clin North Am 77: 275-288.
-
Brandt LJ, Aroniadis OC, Feuerstadt P (2015) On the prevalence and utility of IBD-immune markers in colon ischemia. Am J Gastroenterol 110: 1507.





