International Journal of Surgery Research and Practice
Modified Vertico-Sagittal Osteotomy Technique
Renato de Toledo Breguez*, Giovanni Gasperini and Jose Nazareno Gil
Hospital das Clinicas, Federal University of Goias, Brazil
*Corresponding author: Renato de Toledo Breguez, Hospital das Clinicas, Federal University of Goias, Rua Albertina Q.1 L.1, Vila Nossa Senhora D'Abadia, CEP 75.120-240 - Anápolis, GO, Brazil, Tel: 55(62) 37022084/55(62) 93040510, E-mail: rbucomaxilo@bol.com.br
Int J Surg Res Pract, IJSRP-2-023, (Volume 2, Issue 2), Review Article; ISSN: 2378-3397
Received: February 04, 2015 | Accepted: July 24, 2015 | Published: July 29, 2015
Citation: Breguez RT, Gasperini G, Gil JN (2015) Modified Vertico-Sagittal Osteotomy Technique. Int J Surg Res Pract 2:023. 10.23937/2378-3397/1410023
Copyright: © 2015 Breguez RT, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Among the techniques used to correct mandibular deformities, intraoral vertico-sagittal ramus osteotomy is indicated for small mandibular rotations and forward or backward movements. Although it is still little used by oral and maxillofacial surgeons, it presents advantages compared to intraoral vertical ramus osteotomy because of a greater contact between bone fragments, and in relation to sagittal split ramus osteotomy, it introduces a parallelism to the sagittal plane, thereby decreasing the possibility of a post-operative dislocation of the mandibular condyle and leading to a lower incidence of neurovascular bundle lesions. This work describes a modification of the vertico-sagittal osteotomy technique with advantages in terms of the simplicity and safety of the procedure.
Keywords
Osteotomy, Vertico-sagittal osteotomy, Mandibular osteotomy
Introduction
Choung first described a mandibular osteotomy alternative in 1992 that was indicated primarily for the treatment of mandibular prognathism and, subsequently, for the treatment of hyperplasia and condylar fractures [1,2]. This procedure was called Intra-oral Vertico-Sagittal Ramus Osteotomy (IVSRO). A similar technique to vertical ramus osteotomy, it is a relatively safe procedure that has low complication rates [3-5].The possible complications that are inherent to mandibular osteotomies performed close to important anatomical structures are reported in the literature [4-6], and alternative techniques have been pursued that minimise these problems [1,3,7]. In addition to potentially reducing such problems, IVSRO has the advantages of simplicity and speed of execution [8]. Since the first description of the vertico-sagittal osteotomy technique, other authors have reported modifications in order to improve it, presenting cut alternatives that are safer in relation to anatomical structures, provide greater visibility and are easier to execute [3,7]. One such modified vertico-sagittal osteotomy technique is described in this work in order to simplify this already well-established technique, reducing the time of execution and maintaining safety in relation to the adjacent anatomical structures.
Surgical Technique
An incision is made along the oblique line of the mandible approximately 4 cm in length, and the mucosa and the periosteum are displaced over the buccal surface of the mandibular ramus by exposing the mandibular notch, the mandibular angle and the posterior edge of the mandibular ramus. Bauer retractors are placed in the region of the sigmoid notch, and the other on the pre-angular area of the mandible, which enables a total visualisation of the area to be osteotomised. The marking for the osteotomy is done with a conical drill stem from the centre of the mandibular notch to the bottom base of the mandible in the antegonial region, where the probable distance of the Inferior Alveolar Nerve (IAN) is measured with a LeVasseur-Merrill retractor. The external cortex of the mandibular ramus is then worn before the marking with the same drill until complete exposure of the medullary bone. The weakening of the cortex just below the mandibular notch, where the inner and outer cortex meet, is done with a conical drill stem and extends to the support of the Bauer retractor, where the protection of lingual tissues is performed by the retractor itself. Chisels are introduced 1 cm below the mandibular notch to the antegonial region in a sequence of 1mm to 2.5mm wide. They are placed as parallel as possible to the external cortex, bypassing the medial side of the outer cortex. The chisels are introduced until approximately 1 cm inside the marrow and exchanged in sequence in order to promote bone separation. A sagittal separator can be used to complete the bone fracture if this has not yet occurred. In the step in which chisels are placed to promote bone separation, these can be replaced by ultrasonic tips. The technique follows the same order, but ultrasound is used instead of chisels. The active ultrasound tip is placed in the posterior direction as parallel as possible to the external cortex of the mandibular ramus, cutting from the mandibular to the antegonial notch, and to complete the osteotomy a digital separator can be used.
Discussion
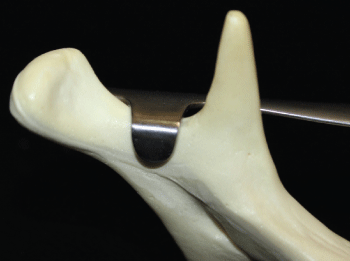
When Choung described IVSRO in 1992, he presented a mandibular osteotomy technique that minimised the displacement of the condyle of the mandible in the post-operative period due to the direction of the osteotomies [1]. Neither sagittal split ramus osteotomy (SSRO) nor intraoral vertical ramus osteotomy (IVRO) is performed parallel to the real sagittal plane nor can this generate a medial and lateral displacement of the condyle, respectively. IVSRO, however, achieves this parallelism, in addition to having other advantages in relation to these two osteotomies [1]. Compared with to SSRO, the advantages are that the osteotomy can be performed more quickly and in a thinner mandibular ramus with safety, lower risk of injuring the neurovascular bundle and greater efficiency in reducing temporomandibular joint dysfunction symptoms (Figure 1). When compared with IVRO, it presents a better stabilization and a more favorable situation in relation to the marrow/cortex contact for bone consolidation [1]. In addition to presenting the advantages of IVSRO, this work aims to simplify the traditional technique: by wearing the outer cortex and weakening the internal cortex with a conical drill stem and minimum lingual tissue detachment only to position the Bauer retractor support (Figure 2), the potential damage to the adjacent neurovascular structures is minimized. In this way, the safety of the procedure is maintained and, consequently, surgery time is reduced. Concerns over damaging structures such as the maxillary artery were reported [6], which analyzed the anatomical variations and possible complications caused by IVSRO. They also highlighted the importance of performing procedures in the mandibular notch region with caution and using a spacer in the region to protect the area. In addition, they recommended tomographic images to localize the mandibular foramen in the preoperative period in order to avoid injury to the inferior alveolar nerve. A modification of the classical osteotomy technique that is very similar to IVSRO was proposed [7] whereby an inverted L-shaped osteotomy was performed and presented smaller risks of injuring the neurovascular bundle, greater overlap of bone fragments, good visualization of the region and the possibility of rigid internal fixation as advantages. Although this technique has its advantages, it differs from IVSRO in that it requires several cuts and angulations, and lingual detachment is greater, reaching the lingula where the position of the mandibular foramen should be checked. According to the authors, the location of the mandibular foramen should be established by Computed Tomography (CT) in the preoperative period to avoid damage to the neurovascular bundle. The technique described in this work requires a minimum lingual detachment limited to 10mm, which is the length of the support of the Bauer retractor. Furthermore, its use in the region of the sigmoid notch with the support positioned above the notch restricts the invasion of the drill into adjacent soft tissues. The bone cut is simpler because the marking and wear of the branch are performed with just one drill bit, and although CT has its usefulness, it is not mandatory in our technique. There are few complications related to the IVSRO technique, as shown in a study [4] with 237 patients who were submitted to IVSRO, presenting a complication rate of 3.8% of inferior alveolar nerve disorders. In another study [5] involving 40 patients (80 sides), the complication rate was 2%, without any nerve lesions, but with two poorly positioned fractures and two cases of post-operative haemorrhaging. In modified IVSRO, oscillating saws are not used and replaced the osteotomy only weakens the lingual cortical and the Bauer retractor provides protection for the lingual portion of the mandibular ramus. Also, for safety, we used the LeVasseur-Merril retractor positioned in the posterior portion of the ramus of the mandible, which enables the cutting instrument to be positioned in a region that is considered safe in terms of injuries to the inferior alveolar nerve [9], assessing the reliability of the LeVasseur-Merril retractor in protecting the mandibular foramen from lesions by vertical osteotomy of the mandibular ramus, placed in the posterior edge of the mandible with the saw positioned correctly, in 280 dry mandibular rami, observed that the average cutting provided by the spacer, measured from the posterior mandible edge to the cutting line (the so-called critical value of 6.65mm), did not touch the inferior alveolar nerve in 98.9% of cases. An alternative to chisels is the use of an ultrasound device. This only cuts through hard tissue and provides more safety during cutting. According [10], who evaluated post-operative complications in 83 patients after 183 osteotomies performed with an ultrasound device divided into 49 Le Fort I, 19 maxillary expansions, five mandibular expansions, 102 sagittal jaw osteotomies, eight genioplasties and 40 combined procedures. The authors did a three-year follow-up and observed a complete absence of dental lesions, haemorrhages, facial paralysis and perforations of the nasal mucosa, as well as reductions in the formation of oedemas and bruising and only two cases (1.96%) of hypoesthesia of the inferior alveolar nerve. The IVSRO technique allows greater bone contact than IVRO and is recommended for small mandibularrotations, forward or backward movements and temporomandibular joint dysfunction. However, surgery in the mandible requires care not to damage important anatomical structures such as the neurovascular bundle and the maxillary artery. Therefore, the modified IVSRO is a technique that combines the simplicity and safety of a surgical procedure. We have used this technique for approximately seven years with an average surgical time of approximately eight minutes for each side of the jaw. To date, no undesired fracture, vascular accident or paresthesias have been reported.
.
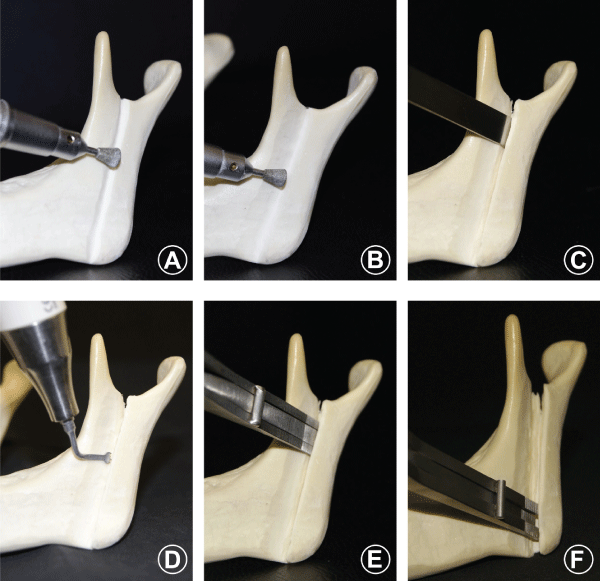
Figure 1: Sequence of the osteotomy: (A) Marking of the mandibular ramus with a conical drill stem, (B) Wear with the same drill of the outer cortex of the mandibular ramus, (C) Placement of chisels in sequence and parallel to the outer cortex of the mandibular ramus, (D) Replacement of chisels by ultrasonic tip, (E) Beginning of bone separation with the digital separator in the upper portion of the jaw, (F) Separation of the proximal stump from the distal stump.
View Figure 1
Conclusion
The described modification of the vertico-sagittal osteotomy technique provides yet another alternative for mandibular surgery, offering a method that has technical simplicity, safety in terms of avoiding damage to adjacent anatomical structures, lower costs and fast execution.
References
-
Choung PH (1992) A new osteotomy for the correction of mandibular prognathism: techniques and rationale of the intraoral vertico-sagittal ramus osteotomy. J Craniomaxillofac Surg 20: 153-162.
-
Choung PH, Nam IW (1998) An intraoral approach to treatment of condylar hyperplasia or high condylar process fractures using the intraoral vertico-sagittal ramus osteotomy. J Oral Maxillofac Surg 56: 563-570.
-
Manor Y, Blinder D, Taicher S (2001) Intra-oral vertical ramus osteotomy: a modified technique for correction of mandibular prognathism. Int J Oral Maxillofac Surg 30: 443-444.
-
Hashemi HM (2008) Evaluation of intraoral verticosagittal ramus osteotomy for correction of mandibular prognathism: a 10-year study. J Oral Maxillofac Surg 66: 509-512.
-
Lima Júnior SM, Granato R, Marin C, de Souza Maliska MC, Gil JN (2009) Analysis of 40 cases of intraoral verticosagittal ramus osteotomies to treat dentofacial deformities. J Oral Maxillofac Surg 67: 1840-1843.
-
Fujimura K, Segami N, Kobayashi S (2006) Anatomical study of the complications of intraoral vertico-sagittal ramus osteotomy. J Oral Maxillofac Surg 64: 384-389.
-
Muto T, Akizuki K, Tsuchida N, Sato Y (2008) Modified intraoral inverted "L" osteotomy: a technique for good visibility, greater bony overlap, and rigid fixation. J Oral Maxillofac Surg 66: 1309-1315.
-
Kuroda S, Murakami K, Morishige Y, Takano-Yamamoto T (2009) Severe Class II malocclusion with facial asymmetry treated with intraoral vertico-sagittal ramus osteotomy and LeFort I osteotomy. Am J Orthod Dentofacial Orthop 135: 809-819.
-
Fontoura RA, Vasconcellos HA, Campos AE (2002) Morphologic basis for the intraoral vertical ramus osteotomy: anatomic and radiographic localization of the mandibular foramen. J Oral Maxillofac Surg 60: 660-665.
-
Gilles R, Couvreur T, Dammous S (2013) Ultrasonic orthognathic surgery: enhancements to established osteotomies. Int J Oral Maxillofac Surg 42: 981-987.