International Journal of Surgery Research and Practice
Extraluminal Migration of a Metal Needle in a Child: Case Report of Unusual Complication
Btissaam Belhoucha*, Youssef Rochdi, Hassan Nourinouri, Lahcen Aderdour and Abdelaziz Raji
Department of ENT, CHU Med VI, Morocco
*Corresponding author: Btissam Belhoucha, Department of ENT, CHU Med VI, Abbad BP: 7234, Marrakech 40000, Morocco, T�l: 00212662390208, E-mail: btissambelhoucha@gmail.com
Int J Surg Res Pract, IJSRP-1-015, (Volume 1, Issue 1), Case Report; ISSN: 2378-3397
Received: October 14, 2014 | Accepted: November 24, 2014 | Published: November 28, 2014
Citation: Belhoucha B, Rochdi Y, Nourinouri H, Aderdour L, Raji A (2014) Extraluminal Migration of a Metal Needle in a Child: Case Report of Unusual Complication. Int J Surg Res Pract 1:015. 10.23937/2378-3397/1410015
Copyright: © 2014 Belhoucha B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Foreign bodies of pharynx and oesophagus are encountered in otolaryngology practice. One of the rare complications of a swallowed foreign body is its migration from the site of entry into the subcutaneous tissues of neck, which requires immediate attention and treatment. We present a case of a sharp metallic foreign body, which migrated from pharynx through the subcutaneous tissues of neck and penetrated the internal jugular vein.
Case Report
We report the case of a 5-year old girl who was admitted to our ENT outpatient clinic with severe odynophagia while eating. The parents gave history of ingesting a metal needle 15 days prior to presentations following which the complaints started.
Otolaryngological examination was without abnormalities. Flexible fibreoptic endoscope of laryngopharynx showed a pooling of saliva at the right pyriform fossa.
Neck x-ray revealed linear radio opacity suggestive of a foreign body at the level of C5-6 vertebrae. A computed tomography (CT) scan was then done that showed a 2cm long metallic foreign body in the subcutaneous tissues of neck at the level of C5-6 vertebrae (Figure 1,2).
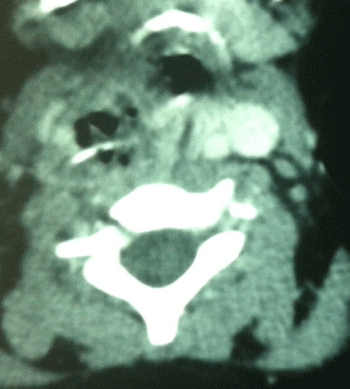
Figure 1: CT axial image of neck showing the metallic foreign body.
View Figure 1
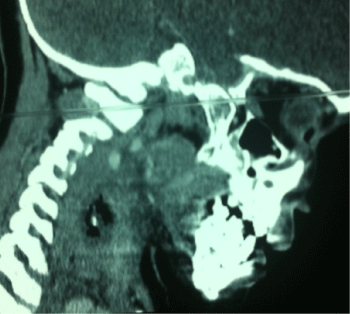
Figure 2: CT sagittal image of neck showing the metallic foreign body.
View Figure 2
An emergency neck exploration was performed under general anaesthesia through a lateral cervical incision. After incising the skin and subcutaneous tissue, the sternocleidomastoid muscle was retracted laterally. A metallic forgein body was found (Figure 3). The foreign body was withdrawn without any bleeding. sternocleidomastoid muscle was sutured back, and the wound was closed in layers. Postoperative period was uneventful and the patient was doing well on follow-up without any complications.

Figure 3: Foreign body after removal.
View Figure 3
Discussion
Accidental ingestion of foreign bodies is a relatively common presentation at any otorhinolaryngology clinic [1-3].
These foreign bodies usually get impacted along the upper digestive tract at the tonsils, vallecula and cricopharynx and are easily removed via a flexible or rigid endoscopy [1-3].
However, sharp and pointed foreign bodies get impacted in the surrounding walls of the lumen. The mechanism by which these foreign bodies propelled through the soft tissues is due to movement of neck muscles and combination of esophageal peristalsis [2,4].
Some authors think that carotid pulsations, tissue reaction as well as infection and abscess formation could also play a role in migration of foreign bodies [1,3,4].
Generally, a swelling in the neck after a history of impaction of foreign body must alert the surgeon of the possibility of perforation and migration of the foreign body into the soft tissues of the neck with subsequent infection and inflammation .and can cause potentially fatal complications depending on the direction and site of the migration [2,4].
Tsunoda et al. [6] reported a pseudo vocal paralysis caused by a fish bone lodged between the arytenoid cartilage and the thyroid cartilage, making it impossible for the arytenoid cartilage to rotate. Another postulation was neuropraxia of right vagus nerve in carotid sheath while manipulations to remove the fish bone as the right vagus nerve was identified and preserved introperatively [1,6].
Hypopharyngeal foreign bodies are usually found intraluminally, cases with extraluminal foreign body has been reported rarely in the literature. A plain radiograph is usually used to confirm the diagnosis of an ingested metallic foreign body, but diagnosis and the exact location of these extraluminal foreign bodies and its relation to the vital structures can be established with CT scan of neck which provides a road map for surgical intervention which was imperative in our case [1,2,5,6].
Generally, immediate localization and removal of all foreign bodies in the upper aerodigestive tract is imperative, particularly in cases of migrating sharp foreign bodies to prevent secondary complications of haemorrhage, haematoma, infection, neurovascular compromise, and the potential migration into the vascular structures [1,2,6]. In our case we were able to remove it easily without any bleeding.
Conclusion
Foreign body ingestion is a common problem encountered in clinical practice. Most of them pass spontaneously but some are really problematic. The possibility of perforation and migration of the foreign body in the soft tissues of the neck must always be borne in mind especially if the patient presents with a tender neck swelling. Though these are rare occurrences, prompt investigation and appropriate treatment should be instituted to avoid complications associated with its subsequent migration. Therefore, a CT scan of the neck preoperatively is helpful in locating the site of penetration and the direction for the search.
References
-
Tang IP, Singh S, Shoba N, Rahmat O, Shivalingam S, et al. (2009) Migrating foreign body into the common carotid artery and internal jugular vein--a rare case. Auris Nasus Larynx 36: 380-382.
-
Sharma NK, Yadav VK, Pokharna P, Devgaraha S, Mathur RM (2013) Surgical management of an impacted sharp mettalic foreign body in esophagus. IJCRI 4: 463-466.
-
Pang KP, Pang YT (2002) A rare case of a foreign body migration from the upper digestive tract to the subcutaneous neck. Ear Nose Throat J 81: 730-732.
- Joshi AA, Bradoo RA (2003) A foreign body in the pharynx migrating through the internal jugular vein. Am J Otolaryngol 24: 89-91.
-
Akulwar CAV, Dwivedi MG, Dwivedi MD (2010) Migrating Extraluminal Foreign Body Hypopharynx MJAFI 66: 196-197.
-
Tsunoda K, Sakai Y, Watanabe T, Suzuki Y (2002) Pseudo vocal paralysis caused by a fish bone. Lancet 360: 907.





