International Journal of Virology and AIDS
Elimination of Mother-to-Child Transmission of HIV in Democratic Republic of Congo: Implementation of "Test &Treat" Approach at Primary Health Centers
Mulamba Diese1*, Susie Villeneuve2, Emile Numbi2, Freddy Salumu2, Guy Clarysse2, Hilo Ilunga3, Franck Fwamba3, Theodore Assani3 and Abel Mukengeshayi Ntambue1,4
1Center for Applied Research and Development (CRAD), Kinshasa, Democratic Republic of Congo
2UNICEF Democratic Republic of Congo, Democratic Republic of Congo
3National Program of AIDS and STD Control, Democratic Republic of Congo
4University of Lubumbashi, Democratic Republic of Congo
*Corresponding author: Mulamba Diese, Center for Applied Research and Development (CRAD), Kinshasa, Democratic Republic of Congo, E-mail: mdiese@crad-rdc.org
Int J Virol AIDS, IJVA-3-026, (Volume 3, Issue 2), Review Article; ISSN: 2469-567X
Received: June 02, 2016 | Accepted: July 27, 2016 | Published: July 30, 2016
Citation: Diese M, Villeneuve S, Numbi E, Salumu F, Clarysse G, et al. (2016) Elimination of Mother-to-Child Transmission of HIV in Democratic Republic of Congo: Implementation of "Test &Treat" Approach at Primary Health Centers. Int J Virol AIDS 3:026. 10.23937/2469-567X/1510026
Copyright: © 2016 Diese M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: The "Test & Treat" approach, also called option B+, using combination antiretroviral treatment (cART) for prevention of mother-to-child transmission (PMTCT) has been very effective in controlled clinical trials in resource-limited settings. We report on our experiences with implementing this approach at primary healthcare settings in Katanga province, Democratic Republic of Congo (DRC). The objective of this study was to evaluate « Test & Treat » approach for PMTCT interventions implemented between September 2013 and June 2015 at local health centers (LHC) in the DRC, in order to learn on the challenges for its scale up at national level.
Methods: We conducted a cross-sectional study. In September 2015, data related to the coverage of "Test & Treat" approach for PMTCT interventions were collected using two techniques: interview and analysis of routinely collected medical data. Interview was conducted with PMTCT focal points at selected LHC using a questionnaire developed and tested on the following: i) administrative status of health facility, ii) number of cART prescribers, as well as iii) availability of renal and liver function tests. The analysis of medical records (registers, patient's medical records) included data of patients recorded between September 2013 and June 2015 according to PMTCT cascades. Data were analyzed using Statav13.0 (College Station, TX). Logistic regression was used to identify factors associated with initiation of cART on the same day with tests for all variables having p-value less than or equal to 10% in univariable analysis. The adjustment of the model was made by using the Hosmer and Lemeshow test. The odds ratio adjusted and confident interval at 5% were calculated. The significance level was 5%.
Results: Of 19,932 pregnant women who received PMTCT services between October 2013 and April 2015 at 85 LHC, 5,381 (27%), 12,557 (63%), 1,395 (7%), and 598 (3%) consulted during the first, second, and third trimester of pregnancy and in labor, respectively. In total, 569 (2.9%) and 19,633 (98.5%) were tested positive and negative for HIV, respectively. All 569 pWLHIV received cotrimoxazole prophylaxis (CP); 557 (97.9%) received cART; blood samples were collected from 373 (65.6%) for kidney and liver function (K&L) tests, and 128 (22.5%) underwent screening for tuberculosis co-infections.
Women in rural areas were twice as likely to receive cART on the day of HIV diagnosis compared to those in urban areas (prevalence risk ratio [PRR] = 2.0; 95% CI = 1.7-2.3; p < 0.001); a similar trend was observed for those who were attended by one cART prescriber at antenatal care compared to those attended by many prescribers (PRR = 0.4; 95% CI = 0.1-0.5; p < 0.001). A longer time gap of K&L results delayed cART on the day of HIV diagnosis (PRR = 0.3; 95% CI = 0.01-0.5; p < 0.001). At 6 to 10 weeks of age, 3.7% (4/108) infants were HIV positive. At 12 months of age; 7.5% (37/493) infants were HIV positive, with 6.8% (22/322) in urban versus 8.8% (15/171) in rural areas (p = 0.47).
Conclusions: The "Test & Treat" approach can be well implemented at LHC in DRC with most pWLHIV being identified and administered cART and CP on the same day; and < 10% instead of < 5% as targeted by the global plan for the elimination mother to child transmission, MTCT rates were likely to be observed by 12 months of age. However, retention in care and infant HIV diagnosis services are challenging.
Keywords
Combined antiretroviral treatment, Cotrimoxazole prophylaxis, Local health center, PMTCT, Retention in care
Abbreviations
AIDS: Acquired Immunodeficiency Syndrome; ARV: Antiretroviral; cART: combination Antiretroviral Treatment; CP: Cotrimoxazole Prophylaxis; DRC: Democratic Republic of Congo; EID: Early Infant Diagnosis; eMTCT: elimination of Mother-To-Child Transmission of HIV and Keeping mothers alive; K & L: Kidney and Liver function; LHC: Local Health Centers; MNCH: Maternal, Newborn and Child Health; PCR: Polymerase Chain Reaction; pWLHIV: pregnant Women Living with HIV; WHO: World Health Organization
Background
A majority of children acquire Human Immunodeficiency Virus (HIV) infection from mothers during pregnancy, delivery, or breastfeeding [1]. Worldwide, new infection cases of HIV among children declined from an estimated 530,000 in 2000 to 260,000 in 2013; overall 35% decline was observed since 2000 (from 58% among children); acquired immunodeficiency syndrome (AIDS)-related deaths declined to 42% since the peak value observed in 2004 as a result of national and concerted global efforts and resources invested in prevention of mother-to-child transmission (PMTCT) programs [1]. Despite this progress, many pregnant women living with HIV (pWLHIV) still do not receive antiretroviral therapy and children continue to be infected and eventually die from AIDS. In 2014 alone, the number of women requiring PMTCT services remained high at 1.3 million, and three out of four children living with HIV were still not receiving HIV treatment in 21 priority countries most affected by HIV [2].
The Global Plan for elimination of mother-to-child transmission of HIV and keeping mothers alive (eMTCT) and keeping mothers alive launched by the United Nations General Assembly High-Level Meeting on AIDS in July 2011 called for the reduction of mother-to-child transmission rate below 5% and universal access (100%) to pediatric HIV treatment and care by 2015. This plan adopted the World Health Organization (WHO) recommendation for lifelong combined antiretroviral treatment (cART) that must be initiated as soon as the diagnosis of HIV is made during pregnancy, and the nevirapine prophylaxis given from birth up to 6 weeks to all HIV-exposed infants [3].
The key factor to success for this virtual eMTCT is the effective provision of cART to mothers during pregnancy and lactation period, which is likely to get translated into undetectable plasmatic levels of viral load [4]. To achieve this level of viral load detectability during pregnancy, cART should be provided early during the pregnancy [5-10]. In resource-limited settings that house most HIV infection cases in the world, pregnant women attend health facilities usually late during pregnancy because of cultural and socio-economic factors [11]. For pregnant women who do not know their HIV status, late attendance to antenatal care (ANC) also means late screening for their status [12]. Even if pWLHIV are identified, access to cART is still limited as these therapies are provided mainly at hospitals and/or international community supported specialized HIV clinics or primary healthcare clinics run by resident or visiting HIV-trained physicians [4].
Local health centers (LHC), where only nurses provide healthcare, are usually not considered for the provision of cART except for HIV testing and, sometimes, follow-ups of people living with HIV (PLHIV) whose condition has been stabilized using cART [11]. However, these facilities offer healthcare services including ANC to majority of low-income class women, who have the highest fertility rates [12,13].
The Democratic Republic of Congo (DRC) is the second largest country in Africa located in sub-Saharan region. The provision of health services is done through Health Zones (HZ), the Congolese equivalent of health district. HZ has a referral general hospital and is divided into 10-20 Health Areas (HA) depending on the size. Each HA has a LHC that offers health services to the community, including ANC services.
In 2013, DRC had HIV prevalence rates of 1.1% among adults (age; 15-49 years) and 3% among pregnant women [1]. The country PMTCT program was introduced in 1999 and mainly implemented with support of international organizations, including United Nations Children Funds (UNICEF); The United States President's Emergency Plan for AIDS Relief (PEPFAR); and Global Fund for malaria, tuberculosis (TB), and HIV. Because of low HIV prevalence rates in some geographic areas, HIV services were provided only in limited LHCs in each HZ. Therefore, PMTCT services were introduced at maternal, newborn, and child health (MNCH) facilities that have at least 30 deliveries per month. By the end of 2013, PMTCT activities were integrated only at 33% (2482 /7520) health facilities, and MTCT prevalence rates were 13% at 6 weeks of age [14].
In this country, an LHC is a public or private health facility and is run by a non-physician, where majority of its clients and patients are members of the community where it is located. Only LHC that has ANC and maternity services were considered for PMTCT services. In 2013, in order to achieve objectives of the global plan for eMCT, DRC introduced task shifting for non-physician clinicians to allow them to prescribe and provide cART. Thus, nurses and midwives were allowed to initiate and follow up PLHIV including pWLHIV.
As many health changes were needed before a nationwide implementation of this new approach, DRC decided to start with a pilot program that would allow changes to address long-standing health-systems issues. Thus, "Test & Treat" approach for pWLHIV was introduced at LHC with support from the Swedish International Development Authority (SIDA) in Katanga province. PMTCT services were introduced at all LHCs to include those that were not previously considered for HIV treatment services in six HZ. These efforts have been technically assisted by UNICEF.
In this study, we used the term "Test & Treat" approach for PMTCT for option B+ according to the World Health Organization guidelines of 2012. According to this approach, HIV infected pregnant women will be initiated cART after the HIV diagnosis is made regardless of the level of CD4 counts. Technically, option B+ is indeed a ‘test and treat" approach for HIV infected pregnant women. The package of ‘Test & Treat" efforts for PMTCT included routine HIV testing for pregnant women including their male partners, collection of blood samples for renal and liver function tests, initiation of cART irrespective of CD4 levels, infant ART prophylaxis from birth up to 6 weeks of age, cotrimoxazole prophylaxis (CP), and virologic tests using polymerase chain reaction (PCR) techniques for infants from 6 weeks of age. The use of simplified ten of ovir-based cART was recommended for pWLHIV and breastfeeding HIV-infected mothers, and the same approach for their HIV seropositive male partners. Mothers are encouraged to exclusively breastfeed until 6 months. As the country has adopted this approach for its national program, eventual challenges to be addressed for its scale up at national level have not yet been documented. Therefore, this study aimed to evaluate this « Test & Treat » approach for PMTCT implemented between September 2013 and June 2015 at LHC in DRC.
Methods
Settings
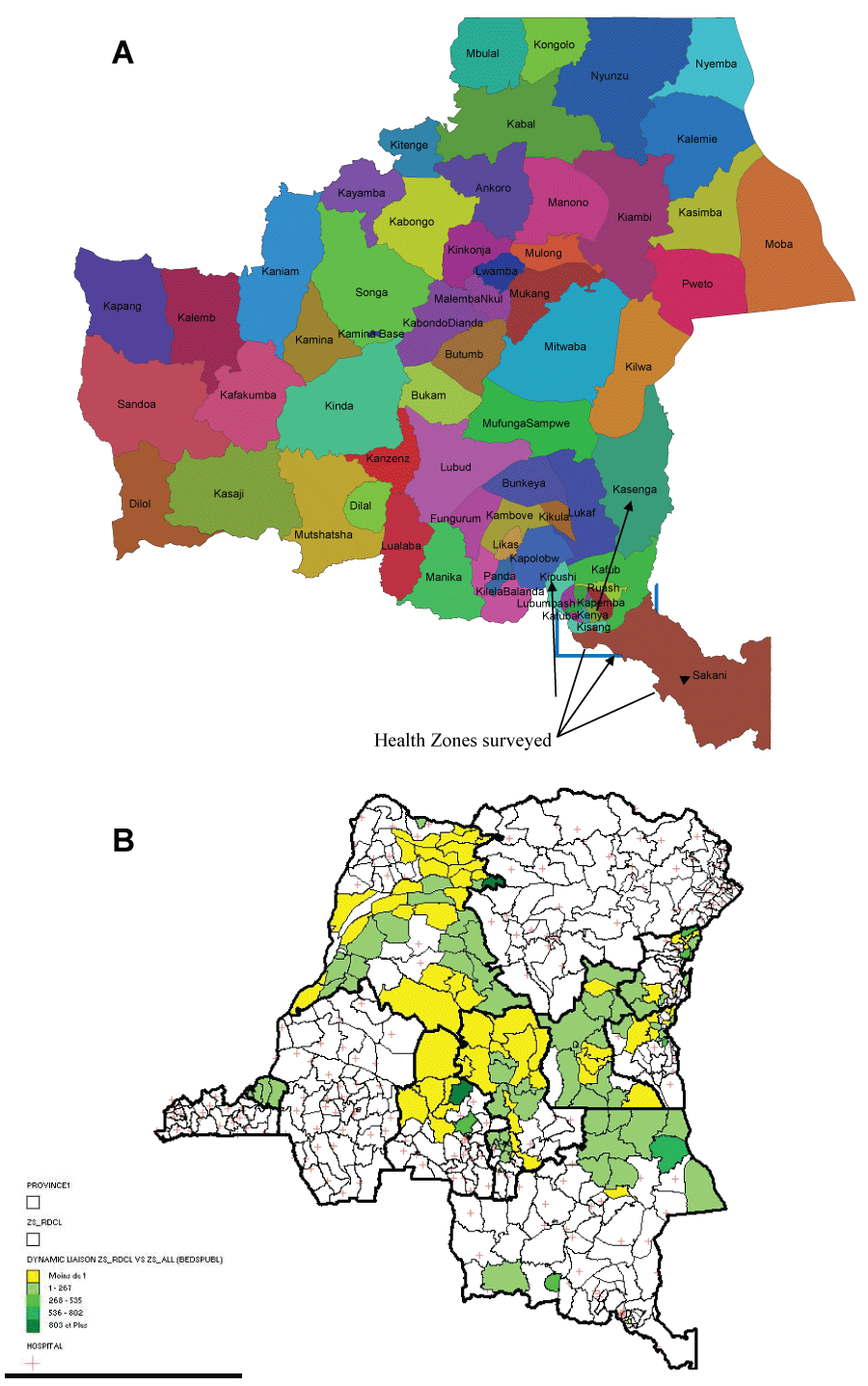
This is the review of routinely collected data at 85 LHC among 128 health facilities of the pilot phase for "Test & Treat" approach supported by UNICEF. These LHCs were located in the 6 health (HZ) in Katanga province, that is, 3 urban HZ (Kapemba, Tshamilemba, and Kisanga) in the city of Lubumbashi, and 3 rural HZ (Kasenga, Sakania, and Kipushi) (Figure 1). Data were collected from the medical records over 15 days. Medical records with incomplete data (0.5%) were excluded. Not-for-profit LHC included those that are owned and managed by churches. For-profit LHC included those that were built for moneymaking business by individual or association of individuals.
Study and data collection
We conducted a cross-sectional study. In September 2015, data related to the coverage of "Test & Treat" approach for PMTCT were collected using two techniques: interview and abstraction of routinely collected medical data. Interview was conducted with PMTCT focal point at selected LHC using a questionnaire developed and tested on the following bases: i) administrative status of health facility, ii) number of cART prescribers, as well as iii) availability of renal and liver function tests. The analysis of medical records (registers, patient's medical records) included data of patients recorded between September 2013 and June 2015 according to PMTCT cascades. The term "PMTCT cascades" refers to critical pathway [15,16] of PMTCT intervention, which normally includes the following events: HIV testing; blood sample tests for liver and kidney (L & K) function; initiation of cART; CP for women, and infants; early infant HIV diagnosis; exclusive breastfeeding; and retention in care. "Test & Treat" in this study implies to PMTCT option B+ approach, that is, a "systematic provision" of cART irrespective of CD4 counts and for life. "cART" is defined here as a combination of three antiretroviral drugs that have synergic action on HIV; and if received over time, it suppresses the HIV load to undetectable levels, which reduces MTCT during pregnancy and breastfeeding.
From each LHC, we collected data related to the number of following: i) pregnant women tested for HIV, ii) pregnant women tested HIV positive, iii) pWLHIV with blood samples collected for L & K function tests, iv) pWLHIV being provided cART, v) pWLHIV screened for TB, vi) breastfeeding HIV-infected mothers who received monthly cART, vii) HIV-exposed infants who received an antiretroviral (ARV) prophylaxis at birth until 6 weeks of age, viii) HIV exposed infants who received CP until end of breastfeeding, ix) HIV exposed infants tested for HIV using PCR technology, and x) HIV exposed children who were tested for HIV at 12 months of age.
Statistical Analysis
Data analysis was performed using Statav15.0 (College Station, TX). Fisher exact test with 95% confidence intervals (95% CI) were used to compare proportions of initiation of cART among the following independent variables: i) urban versus rural location of LHC, ii) sex of prescribers, iii) site having one cART nurse prescriber compared to those having more than two, iv) sites conducting L & K function tests prior to initiation of cART compared to those where these tests were not conducted, and v) sites with on-site collection of dried blood samples for early infant diagnosis (EID) compared to those where such test were not conducted. Less factors associated with the organization, for example: the availability of ARV drugs at LHC and health administrative status, were not taken into account in this analysis. Logistic regression [17] was used to identify factors associated with initiation of cART on the same day with tests for all variables having p-value less than or equal to 10% in univariable analysis. The adjustment of the model was made by using the Hosmer and Lemes how test. Less odds ratio adjusted and confident interval at 5% were calculated. The significance level was 5%.
Ethical Considerations
This assessment was submitted to the National Ethical Review Committees of DRC. In addition to the National Ethics Committee approval, this protocol was also reviewed and approved by the Institutional Review Board of the University of Kinshasa (No UNIKIN/CE/MB/05/2015). In view of securing confidentiality, all recording materials were anonymously collected and codes were used to identify each woman and each child. Data were accessible only to our research team.
Results
Profile of health facilities
In total, 85 LHC were surveyed. Sixty-six (77.6%) and 19 (22.4%) LHC were located in urban and rural areas, respectively. In addition, 16.0% (14/85), 32.9% (28/85), and 50.6% (43/85) were not-for-profit, for-profit, and faith-based institutions, respectively. In the urban areas, 34.0% LHCs (29/85) had twice-a-week visiting physicians. HIV treatment services were provided by nurses; 55.3% (48/85) were women, and 44.7% (37/85) were men. Moreover, 56.0% (48/85), 28.3% (24/85), and 15.3% (13/85) had one, two, and more than two prescribers, respectively. Blood sample tests for evaluation of L & K functions were not conducted in 17.6% (15/85) LHCs (Table 1). CD4 count measurement was not a requirement for initiation of cART.
![]()
Table 1: Local health centers providing PMTCT "Test & Treat" services.
View Table 1
No difference was observed between the profile and administrative status of LHC (p = 0.14) and the number of cART prescribers (p = 0.98) in urban and rural areas. However, the sex-ratio, that is, F/M was 0.57 in urban area versus 2.8 in rural area (p < 0.001). In urban areas, compared to rural areas, physicians visited LHCs located in urban area more frequently (p = 0.01).
PMTCT cascade
Between September 2013 and April 2015, 19,932 pregnant women were observed in selected LHCs (Table 2). Of these pregnant women, 5,381 (27.0%), 12,557 (63.0%), 1,395 (7.0%), and 598 (3.0%) consulted during the first, second, third trimester of pregnancy, at second, and in labor, respectively; 1.5% (299/19,932) and 0.6% (1/19932) women from urban and rural areas, respectively delivered without knowing their HIV status. Among 98.5% (19,337/19,632) pregnant women who accepted undergoing tests for HIV, 569 (2.6%) were found positive for HIV. The HIV prevalence was 3.0% (366/12,362) and 2.8% (203/7,270) in urban and rural areas, respectively.
![]()
Table 2: PMTCT cascade services at selected local health centers.
View Table 2
Proportions of pWLHIV aged less than 20 years, 21-29 years, 30-39 years, and above 39 years were 15.6% (89/569), 46% (262/569), 34.6% (197/569), and 3.8% (21/569), respectively. pWLHIV education levels indicated that 2.6% (15/569), 14.6% (83/569), 41.8% (245/569), 29.3% (173/569), and 11.7% (68/569) had no formal education, primary level, some secondary level, secondary graduation, and tertiary level education, respectively. Further, 29.9% (170/569) pWLHIV were never married; however, 63.4% (361/569) were married, and 6.7% (38/569) were widowed (Table 2).
Among 128 (22.5%) pWLHIV who were systematically screened for Tuberculosis (TB)/HIV co-infections, 89.8% (115/128) and 10.2% (13/128) were from urban and rural areas, respectively (Table 2). Active pulmonary tuberculosis (PTB) and past medical history of TB of less than 2 years were observed in 1.6% (2/128) and 2.3% (3/569), respectively (Table 2).
CP was provided to all pWLHIV on the same day of HIV diagnosis. Repeat prescriptions of CP were provided to 89.1% (326/366) and 95.1% pWLHIV (193/203) during pregnancy versus 64.2% (235/366) and 61.6% (125/203) pWLHIV in postnatal period in urban and rural areas, respectively. All HIV-exposed infants received CP from 6 weeks of age (Table 2).
Blood tests for L & K function were not conducted prior to the initiation of cART in 34.4% (196/569) pWLHIV, and 86% (168/196) of these were from rural and urban area respectively. Among all the stages of PMTCT cascade, only screening of TB and evaluation of renal and liver function tests were different for both the locations (p < 0.001). TB prevalence rates in urban areas were twice higher than in rural areas (31.4% versus 6.4%). This trend was similar for evaluation of renal and liver function tests (92.3% versus 17.2%).
We observed that 34.4% of women received cART without renal and liver function tests; 22.3% received this treatment 2 days after HIV diagnosis and availability of the results of renal and liver function tests; 24.8% tests were conducted from 2 weeks to 1 month, while18.5% were conducted after 1 month as shown in figure 1.
As shown in table 3, CP was provided to all alive HIV-exposed infants at 6 weeks of age. Monthly prescription of CP was not repeated after EID results for 17.4% (81/468). HIV-exposed infants and for 21% (98/468) pWLHIV after 1 month during the neonatal period; among 13% (11/85) and 7.9% (7/85) LHC in the urban and rural areas, respectively. By 12 months of age, 12.2% (69/565) could not be followed up; of these, 7.7% (28/362) and 17.6% (41/233) were from rural and urban areas, respectively. Retention at LHC level was associated with: (1) less than three cART prescribers (74.2%), (2) infant CP provided during the entire lactation period (89.6%), and (3) community support services provided to the mothers on the site (69.3%).
![]()
Table 3: Infant mortality, EID, and mother-to-child transmission of rates.
View Table 3
Out of 569 deliveries of pWLHIV, 0.7% (4/569) were stillbirths and 99.3% (565/569) were alive infants; the latter received nevirapine prophylaxis from birth. All the four pWLHIV who had stillbirths started cART during the second trimester; 0.6% (3/565) infants died before 6 weeks of age. Of those, one stillbirth was delivered by a pWLHIV who had received cART during the third trimester; the remaining two stillbirths were delivered by women who had received cART during the second trimester. EID services were limited, with only 20.7% (108/523) infants being tested for HIV using PCR technology at 6 to 10 weeks of age. There were three times infants tested between 6 to 10 weeks in urban area than in rural area (27.6% versus 8.4%; p < 0.001). Of these, 3.7% (4/108) infants tested positive for HIV. Almost six percent (5.7%; 30/523) HIV-exposed infants died between 10 weeks and 12 months of age. At 12 months of age, 7.5% (37/493) infants tested positive for HIV through rapid test (Table 2). The mother-to-child transmission rates in urban areas were 6.8% (22/322) compared to 8.8% (15/171) in rural area. This was not statistically significant (p = 0.47).
Factors associated with providing cART among pWLHIV
In table 4, univariable analysis reveals that the location of LHC, age of patient, her level of education, marriage status, number of attending cART prescribers as well as the availability of renal and liver function tests were associated with the initiation of cART among pWLHIV for PMTCT services (p < 0.001), as shown in table 3. The same factors were associated with immediate initiation of cART observed in multivariable analysis using logistic regression.
![]()
Table 4: pWLHIV and providing cART.
View Table 4
Thus, women in rural area were twice likely to start the treatment on the same day after the HIV diagnosis was made compared to women in urban areas(p < 0.001); similar trend was observed for women aged 20-39 years of age compared to the young mothers below 20 years of age (p < 0.001). Concerning education levels, women with secondary and tertiary level education had twice the chance to receive cART on the day of HIV diagnosis compared to those with lower education levels (p < 0.001); this was equally true for married women in comparison to unmarried ones (p < 0.001). Women visiting health facilities that had one cART prescriber were more likely to start cART on the day of HIV diagnosis than those who visited health centers with many prescribers (p < 0.001). Finally, as the time gap for renal and liver function tests increased, the number of women receiving cART on the same day of HIV diagnosis decreased (p < 0.001).
Discussion
The implementation of PMTCT cascade using "Test & Treat" protocol at the lowest level of health system of DRC is possible. There are six major findings. First, the identification of pWLHIV is universally accepted. The review suggested that most of the pregnant women have been tested for HIV during the first visit at ANC and that neither education level of women nor marriage status influenced this as shown by other investigators [8,12-14]. This identification is done mainly during the second trimester when most of the pregnant women had their first visit at ANC as found by other investigators [13,14,18,19].
Second, the pWLHIV start their cART in less than a month after the HIV diagnosis has been made. This was due to the fact that the measurement of CD4 counts were not performed in most of the settings even for the purpose of follow-ups as demonstrated by other investigators [13,14].
Thirdly, the global plan for the elimination of MTCT and keeping mothers alive 2011-2015, which has adopted option B+ or "Test & Treat" approach for pregnant WLHIV, targeted < 5% MTCT rates at 12 months of age [2]. However, on the routine implementation of this plan at lowest level of health system in DRC, this study has found that the MTCT rates were < 10% instead of < 5% by 12 months of age.
Fourthly, there have been the following three major challenges in implementing this approach at the primary healthcare level: (1) the capacity of staff to assess the possibility of TB/HIV co-infections was weak. The review has shown that few staff collected medical TB history and did not systematically screen clients for co-infections as demonstrated by other investigators [20,21]; (2) Healthcare providers were weak in adhering to the national guidelines in terms of the assessment of L&K function tests. The review has shown that over half of the pWLHIV have never undergone these tests even if these were free of charge, as found by other investigators [22]; (3) Shortage of cART prescribers delay the initiation of cART for pWLHIV. We observed a limited number of prescribers, especially in rural areas where most of the facilities were mainly faith-based facilities; (4) Most of the HIV-exposed infants had no access to EID services, as other investigators have found it [23-25]; therefore, those who could already be infected by HIV virus have no timely accessed to treatment.
Fifthly, retention and lost to follow up were still a huge challenge. We observed that clients in rural area had more challenges in keeping their appointments. This situation could have been due to socio-economic factors such as cost of transportation, stigma, and lack of support from community as shown by other investigators [26,27].
Sixthly, at 6 weeks of age, the mother-to-child HIV transmission rates were similar to the 2-4% post-neonatal mortality observed in the Africa region [2]. In addition, we observed that infant mortality occurred in utero, early before EID test, and during lactation period as shown by other investigators [28-30].
DRC has adapted the recommendations of the WHO guidelines for its PMTCT program to reach the UNGASS and millennium development goals and the global plan for the elimination of mother to child transmission of HIV and keeping mothers alive [3,5]. Archives of medical files and patients' records were not well maintained at most of the health faci, 30lities, and clinical observations in patient's folders are poorly documented. Moreover, there is no national indicator to record adherence, lost follow ups, and retention in care for patients. Integration with community-based services have been limited because of lack of information in patient medical folders.
Conclusions
The study demonstrated that the implementation of "Test & Treat" (option B+) approach for PMTCT is possible at LHCs (primary healthcare) in resource-limited settings such as DRC. Most of pWLHIV were identified and were provided cART for life, and MTCT rates were maintained below 10% among breastfed infants of 12 months of age in both settings. The prevalence rates of TB/HIV co-infections among pWLHIV were low among pWLHIV, despite that these pregnant women were more likely to be screened for TB in urban area where its prevalence was twice higher compared to rural area. Although very low, still birth was not uncommon neither were the early deaths among HIV-exposed neonates.
Many HIV- exposed infants were still not having access to EID services at local health centers in both locations. The point-of-care techniques may be appropriate in this setting. In spite that the MTCT prevalence rates were low at 6 weeks of age, these rates increased through breastfeeding during postnatal period. This situation may prompt the need for strengthening follow up and support for exclusive breastfeeding practices. Factors associated with this effective implementation included on-site presence of more than one trained healthcare providers, balanced workload per day, and infant CP during the entire postnatal period.
The retention, adherence to cART, and follow-ups of mother-infant pairs were still challenging. Ultimate performance of PMTCT services at this level of health system may require strengthen of health system especially for postnatal period. Further research should be conducted to assess the best strategies to improve adherence and retention among pWLHIV and HIV-exposed infants.
Consent for Publication
Not applicable.
Competing Interests
The authors declare that they have no conflict of interest in the present research.
Authors' Contributions
MD has designed and written the protocol of this study; he conducted data analysis, wrote the first draft of this manuscript, and finalized the last version of this manuscript. SV, EN, FS, GC, HI, FF, and TA validated the protocol, reviewed, and corrected the first version of this manuscript and analyzed the data of this manuscript. MAN validated the protocol, analyzed data, and wrote the last version of the manuscript. All authors have read and approved this manuscript before its submission.
Acknowledgements
This review was funded by the UNICEF Democratic Republic of Congo. The authors would like to express their appreciation to all the staff of LHCs who contributed to the study.
References
-
(2015) World Health Organization and UNAIDS. Global AIDS response progress reporting 2015.
-
(2014) UNAIDS The Gap Report.
-
(2011) UNAIDS. The Global Plan for the elimination of mother to child transmission of HIV and keeping mothers alive 2011-2015.
-
(2010) PMTCT strategic vision 2010_2015: Preventing mother-to-child transmission of HIV to reach the UNGASS and millennium development goals. Geneva, Switzerland: World Health Organization.
-
World Health Organization (2013) Consolidated Guidelines on the use of Antiretroviral Drugs for treating and preventing HIV infection. Recommendations for a public health approach.
-
Mary S Ngoma, Amita Misir, Wilbroad Mutale, Emmanuoil Rampakakis, John S Sampalis, et al. (2015) Efficacy of WHO recommendation for continued breastfeeding and maternal cART for prevention of perinatal and postnatal HIV transmission in Zambia. J Int AIDS Soc 18: 19352.
-
Read PJ, Mandalia S, Khan P, Harrisson U, Naftalin C, et al. (2012) When should HAART be initiated in pregnancy to achieve an undetectable HIV viral load by delivery? AIDS 26: 1095-1103.
-
Lise Denoeud-Ndam, Camille Fourcade, Aurore Ogouyemi-Hounto, Azon-Kouanou A, Marcelline d'Almeida, et al. (2013) Predictive factors of plasma HIV suppression during pregnancy: A prospective cohort study in Benin. PLoS ONE 8: e59446.
-
Muhwava LS, Morojele N, London L (2016) Psychosocial factors associated with early initiation and frequency of antenatal care (ANC) visits in a rural and urban setting in South Africa: A cross-sectional survey. BMC Pregnancy Childbirth 16: 18.
-
Kawungezi PC, AkiiBua D, Aleni C, Chitayi M, Niwaha A, et al. (2015) Attendance and Utilization of Antenatal Care (ANC) Services: Multi-Center Study in Upcountry Areas of Uganda. Open J Prev Med 5: 132-142.
-
Auld AF, Nuwagaba-Biribonwoha H, Azih C, Kamiru H, Baughman AL, et al. (2016) Decentralizing Access to Antiretroviral Therapy for Children Living with HIV in Swaziland. Pediatr Infect Dis J 35: 886-893.
-
Abongomera G, Kiwuwa-Muyingo S, Revill P, Chiwaula L, Mabugu T, et al. (2015) Population level usage of health services, and HIV testing and care, prior to decentralization of antiretroviral therapy in Agago District in rural Northern Uganda. BMC Health Serv Res 15: 527.
-
(2016) Population Division of the Department of Economic and Social Affairs of the United Nations Secretariat. World Population Prospects. The 2010 Revision.
-
Günther I, Harttgen K (2016) Desired Fertility and Number of Children Born Across Time and Space. Demography 53: 55-83.
-
(2015) UNICEF/DRC Annual report 2014. Democratic Republic of Congo.
-
Stringer JS, Sinkala M, Maclean CC, Levy J, Kankasa C, et al. (2005) Effectiveness of a city-wide program to prevent mother-to-child HIV transmission in Lusaka, Zambia. AIDS 19: 1309-1315.
-
Tsague L, Tsiouris FO, Carter RJ, Mugisha V, Tene G, et al. (2010) Comparing two service delivery models for the prevention of mother-to-child transmission (PMTCT) of HIV during transition from single-dose nevirapine to multi-drug antiretroviral regimens. BMC Public Health 10: 753.
-
Feinstein L, Dimomfu BL, Mupenda B, Duvall S, Chalachala JL, et al. (2013) Antenatal and delivery services in Kinshasa, Democratic Republic of Congo: Care-seeking and experiences reported by women in a household-based survey. Trop Med Int Health 18: 1211-1221.
-
Bwirire LD, Fitzgerald M, Zachariah R, Chikafa V, Massaquoi M, et al. (2008) Reasons for loss to follow-up among mothers registered in a prevention-of-mother-to-child transmission program in rural Malawi. Trans R Soc Trop Med Hyg 102: 1195-1200.
-
Hoffmann CJ, Variava E, Rakgokong M, Masonoke K, van der Watt M, et al. (2013) High prevalence of pulmonary tuberculosis but low sensitivity of symptom screening among HIV-infected pregnant women in South Africa. PLoS One 8: e62211.
-
Pillay T, Khan M, Moodley J, Adhikari M, Padayatchi N, et al. (2001) The increasing burden of tuberculosis in pregnant women, newborns and infants under 6 months of age in Durban, KwaZulu-Natal. S Afr Med J 91: 983-987.
-
Edmonds A, Feinstein L, Okitolonda V, Thompson D, Kawende B, et al. (2015) Implementation and Operational Research: Decentralization Does Not Assure Optimal Delivery of PMTCT and HIV-Exposed Infant Services in a Low Prevalence Setting. J Acquir Immune Defic Syndr 70: e130-139.
-
Zolfo M, De Weggheleire A, Schouten E, Lynen L (2010) Time for "test and treat" in prevention of mother-to-child transmission programs in low- and middle-income countries. J Acquir Immune Defic Syndr 55: 287-289.
-
Kim MH, Ahmed S, Hosseinipour MC, Yu X, Nguyen C, et al. (2015) Impact of Option B+ on the Infant PMTCT Cascade in Lilongwe, Malawi. J Acquir Immune Defic Syndr 70: 99-103.
-
Kieffer MP, Mattingly M, Giphart A, Van de Ven R, Chouraya C, et al. (2014) Lessons learned from early implementation of option B+: The Elizabeth Glaser Pediatric AIDS Foundation experience in 11 African countries. J Acquir Immune Defic Syndr 67: S188-S194.
-
Diese M, Shrestha L, Pradhan B, Singh D, Raaijmakers H, et al. (2016) Bottlenecks and opportunities for delivering integrated pediatric HIV services in Nepal. Curr Opin HIV AIDS 11 Suppl 1: S21-29.
-
Msellati P, Hingst G, Kaba F, Viho I, Welffens-Ekra C, et al. (2001) Operational issues in preventing mother-to-child transmission of HIV-1 in Abidjan, Côte d'Ivoire, 1998-99. Bull World Health Organ 79: 641-647.
-
Tenthani L, Haas AD, Tweya H, Jahn A, van Oosterhout JJ, et al. (2014) Retention in care under universal antiretroviral therapy for HIV-infected pregnant and breastfeeding women ('Option B+') in Malawi. AIDS 28: 589-598.
-
Dick Chamla, Dorothy Mbori-Ngacha, Morkor Newman, Scott E Kellerman, Nandita Sugandhi, et al. (2013) Evidence from the field: missed opportunities for identifying and linking HIV-infected children for early initiation of ART. AIDS 2: S139-S146.
-
Diana M. Gibb, Hilda Kizito, Elizabeth C. Russell, Ennie Chidziva, Eva Zalwango, et al. (2012) Pregnancy and infant outcomes among HIV-infected women taking long-term ART with and without ten of ovir in the DART trial. PLoS Med 9: e1001217.