International Journal of Women's Health and Wellness
Recommendations for Caffeine Intake Reduction in Women with Urinary Incontinence: A Systematic Review of Literature
Marcela Gurovich1, Cristhel K Fagerstrom2*, Maria J Prieto3 and Hugo Sanchez3
1Women's Health Department, University of Chile, Chile
2Faculty of Health and Odontology, University Diego Portales, Chile
3National Institute of Food Technology, INTA University of Chile, Chile
*Corresponding author:
Cristhel K Fagerstrom, School of Obstetrics and Neonatology, Faculty of Health and Odontology, University Diego Portales, Manuel Rodriguez Sur 415, Santiago, Chile, E-mail: cristhel.fagerstrom@mail.udp.cl
Int J Womens Health Wellness, IJWHW-2-035, (Volume 2, Issue 3), Review Article; ISSN: 2474-1353
Received: July 08, 2016 | Accepted: September 19, 2016 | Published: September 22, 2016
Citation: Gurovich M, Fagerstrom CK, Prieto MJ, Sanchez H (2016) Recommendations for Caffeine Intake Reduction in Women with Urinary Incontinence: A Systematic Review of Literature. Int J Womens Health Wellness 2:035. 10.23937/2474-1353/1510035
Copyright: © 2016 Gurovich M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In light of the wide spread recommendation to reduce caffeine consumption in women who report urinary incontinence (UI) in order to diminish leakage episodes, we performed a systematic review of the literature to evaluate the evidence that supports this recommendation.
Objective: To determine the relationship between caffeine consumption and incidence or progression of UI.
Design: Systematic review of literature.
Data sources: Using medical subject headings and keywords, we conducted an electronic literature search of PubMed, The Cochrane Library, Springer Link, and LILACS databases.
Study selection: All articles describing prevalence and/or incidence and reporting an effect statistic for caffeine consumption and UI were included. Articles with no data reported were excluded, as were articles in languages other than English, Spanish and French. Studies that did not report age specific prevalence of UI as those conducted in non-human subjects were excluded. Complete searches (shown in appendix) was conducted. All retrieved papers were reviewed.
Data extraction: Three investigators independently extracted the data.
Results: 60 articles were found after excluding for subject characteristics or methodology. We selected a total of ten studies: two randomized trials, one prospective cross over, four longitudinal cohort, and three cross-sectional studies.
Conclusions: Low and moderate caffeine consumption in healthy women was not associated with incidence and/or progression of UI. Caffeine restriction did not improve symptoms. There is insufficient evidence supporting caffeine restriction for an improvement of symptoms.
Keywords
Urinary incontinence, Women, Caffeine, Intake, Coffee
Introduction
Urinary incontinence (UI) affects millions of people around the world and affects quality of life (QoL) [1]. Even though public exposure to this problem in recent years through commercial advertisements has facilitated women seeking care, the frequency is still low [2]. Prevalence of the condition varies according to study participants and measurement of UI. The different methodologies used across studies accounts for some of the variation. Methods of data collection and rate of response is another factor which can bias prevalence estimates since incontinent subjects may deny having UI, or may respond in greater numbers because they are drawn to the subject. We do not currently know how these factors affect prevalence estimates.
A population based prevalence of 45% urinary incontinence has been described in American women aged 30 years and over [3]. The impact of UI is much higher among middle aged and older women, and in these age categories, its prevalence is estimated to be 40% and 50%, respectively [4]. Epidemiological research has revealed several factors associated with UI in women, the most commonly reported being age, pregnancy and childbirth. Alterations in lifestyle are frequently recommended as they are relatively low in cost and have no side-effects, essentially smoking and diet, namely caffeine [5]. In order to assess the intake of caffeine and its relation to UI, various studies have included specific beverages (coffee) rather than total dietary caffeine in their analyses and no significant association has been found. The habits associated with coffee consumption differ in different areas of the world [6,7]. In the United States, caffeine is regularly consumed by more than 85% of adults [8,9] and approximately 20-30% of Americans consume more than 5 cups of coffee per day (equivalent to about 600 mg of caffeine), while 10% consume over 1000 mg of caffeine per day [10].
The chemical nomenclature for caffeine is 1,3,7-trimethylxanthine, which occurs naturally in coffee beans, tea leaves and cocoa beans [6,11]. Although the mechanisms by which caffeine may acutely induce diuresis are not well defined, there has been a widely held concept that it acts as a diuretic. This concept arose from early studies involving rabbits and humans, published by Myers and Eddy N.B. Downsin 1924 and1928 respectively. Two studies assessed the diuretic effect of caffeine (versus placebo) when urine was collected after ingestion of 250 and 360 mg caffeine. Findings showed no differences from placebo in acute urine production associated with low oral doses of caffeine (90 and 180 mg). This suggested that regulation of total body water could be affected only above a certain caffeine ingestion threshold (between 180 and 360 mg) [7,12].
Even though previous investigations have assessed the acute effects of caffeine upon fluid-electrolyte balance, the study conducted by Armstrong, et al. in 2005 posed this question during a continuous period of eleven days of caffeine intake. This research determined that variables were unaffected by different caffeine doses, and were within normal clinical ranges: 24h urine volume, 24h, Na+ and K+ excretion, 24h creatinine, blood urea nitrogen, serum Na+ and K+, hematocrit, and total plasma protein. Therefore, these findings question the notion that caffeine consumption acts chronically as a diuretic [13].
Since conservative medical management for UI is the first line treatment reported [14] numerous health professionals prescribe interventions such as caffeine restriction to UI sufferers claiming that caffeine incites a diuretic effect, increasing pressure and excitability over detrusor muscle fibers [15,16]. Previous publications have shown controversial results, which is the motivation for this systematic review. ¬Our research question is as follows: Is there a relationship between caffeine consumption and incidence or progression of UI?
Methods
"Urinary incontinence" was defined as the complaint of any involuntary urinary leakage [17] and measured by pad testing (a validated methodology to quantify urine loss). To determine the severity of incontinence, the only instrument which correlates with the pad testis the ICIQ-SF, which is easier to administer and incorporates both symptom severity and QoL variables [18].
"Caffeine consumption" was defined as the amount of caffeine present in coffee, tea and chocolate intake in a regular diet, using food frequency questionnaires (FFQ) to assess consumption and measuring caffeine content as grams per cup and units per bar. Systematic searches to answer the clinical research question, formulated and agreed by the reviewers, were executed using the following databases: NCBI MEDLINE and PubMed, The Cochrane Library (Cochrane Central Register of Controlled Trials), Springer Link and LILACS. All searches between1999 and 2015. Journal Citation Report database was used to determine impact factors in selected publications. All abstracts were initially reviewed by the primary author (MG) and relevant abstracts were short-listed. These were then independently reviewed by two other authors (CKF and MJP).
Study selection
Study searches included randomized controlled trials (RCT), prospective cohort, case-control, and cross-sectional studies. Inclusion criteria were: women with or without UI, caffeine consumption, and 25 years and older. Studies including pregnant women or subjects with current diuretic drugs or surgery record for any pelvic organ prolapse or UI were excluded.
Language restrictions were applied to searches, covering publications in English, French and Spanish. Hand searching of journals not indexed on the databases searched was also undertaken. Articles that presented no data, such as review articles and editorials, as well as literature extracted from conferences or unpublished trials were excluded (Figure 1).
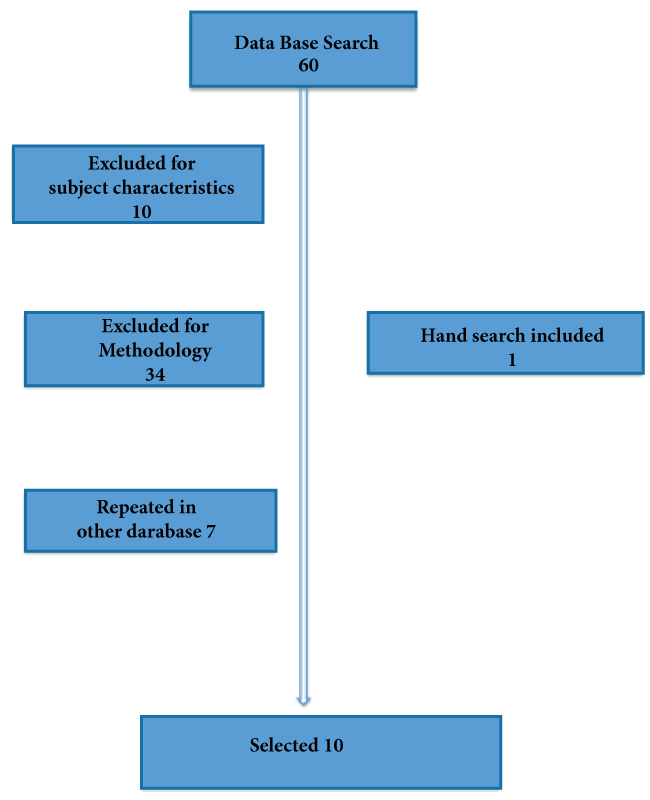
.
Figure 1: Study flow diagram.
Data were synthesized qualitatively by summarizing the content of papers in tables and agreeing brief statements that accurately reflected the evidence. Sixty publications were identified, and a total of ten studies were selected (three randomized trials, four longitudinal cohort, and three cross-sectional studies).
View Figure 1
Results
Three trials
Three trials involving 424 women in total, demonstrated different results. A prospective cross over trial by Swithinbank, et al. in 110 British women showed no association between caffeine restriction and improvement of symptoms; an effect was only demonstrated when fluid intake was decreased [17]. On the other hand, two trials demonstrated association: a quasi- experimental trial by Tomlinson in Florida and a RCT by Bryant in Australia [19,20]. Tomlinson conducted the study in 218 women aged 55 years and older with UI. The treatment group was encouraged to decrease caffeine intake and received recommendations about daytime voiding intervals. Results showed association (not significant) between caffeine restriction and reduction of episodes of involuntary urine loss. The RCT by Bryant, et al in 96 women with UI demonstrated that the experimental group experienced a significant reduction in caffeine consumption (less than 100 mg) and significant less occasions of incontinence (P = 0.002).
Four prospective studies
The first by Townsend, et al. [18] demonstrated no association with caffeine intake reduction and fewer symptoms among women with moderate incontinence in a four year follow-up period, OR 0.87 (0.70-1.08). In detail, they observed 21,564 women, aged between 39 and 81 years living in the United States. After adjusting for confounding factors authors found no association between baseline level of caffeine intake and subsequent odds of UI progression over 2 years. The second study by Jura, et al. [18], investigated the association between caffeine intake and incidence of UI over four years follow-up in a cohort of 65,176 women aged between 37 and 79 years without incontinence. The authors reported that an absolute effect of caffeine consumption on UI was among women who consumed ≥ 450 mg (≥ 4 cups) of caffeine per day. Attributable risk figures show that 16% of frequent UI could be avoided by reducing caffeine intake to 0-149 mg per day. The third study, a case control design by Arya, et al. in a cohort of 259 participants, showed that very high intake of caffeine (> 400 mg/day) was associated with higher odds of detrusor instability (DI) and that women with DI were more likely to be current smokers and their caffeine intake was higher than the group without the condition. Adjusted OR for detrusor instability for women with high caffeine intake (> 400 mg) OR 2.4 (CI 1.1- 6.5 P 0.018) [15].
The fourth longitudinal study by Bradley, et al. [21] in 297 women almost exclusively Caucasian, with a mean age of 68.2 years enrolled in the Women's Health Initiative study (WHI) four years prior to study initiation, reported that two variables associated with obstructive urinary symptoms were caffeine consumption and increasing age (OR 5.3 95% CI 1.2 - 23.0), although the difference did not reach statistical significance (p = 0.06). Symptoms were found in 15% of coffee drinkers compared with 3% in other participants.
Three cross-sectional studies
The first by Hirayama, et al. [22] of 296 Japanese women found no significant association between caffeine intake and UI, which could be attributed to the low caffeine intake by Japanese adults. Indeed, similar levels of caffeine and total fluid intake were observed between subjects with and without UI, and none of the participants reported any change in dietary and drinking habits within the past five years. The second study by Hannestad, et al. [5] of 27,936 Norwegian women from the Epicont Study, did not find any significant association between coffee intake and UI. However, daily tea drinkers had higher odds of UI for all outcomes, although results for urgency UI did not reach statistical significance. Tea may contain components other than caffeine that might aggravate incontinence and thus account for this difference. Coffee had no effect on any incontinence and a weak but insignificant effect on incontinence of severe mixed type. The third cross-sectional study by Gleason, et al. [23] found association between UI and caffeine intake above 204 mg/dl (POR 1.47, 95% CI 1.07-2.07) but the type of UI was not associated with caffeine intake (Table 1).
![]()
Table 1: Study characteristics and outcomes.
View Table 1
Discussion
This study provides needed information about pelvic floor symptoms and caffeine consumption in women at different ages. We have located a representative subset of all studies and have not selectively reported on trials that provide overly optimistic or pessimistic estimates of the effects of intervention. All included trials had adequate sample sizes, from 69 to 65,000 participants and ample follow-up. Participants were resident in the community therefore, the applicability of findings to men and particularly frail elderly people in care home settings, is uncertain. We mention the fact that within some cohorts of incontinent women, caffeine intake was low, probably due to self-restriction and management of information with reference to habits and risk factors, which may account for observed results in certain studies. On the other hand, fluid intake might be a confounding factor, which should be further assessed. Overall, the majority of cross sectional studies did not find association between caffeine and UI, one research (Gleason) observed a higher prevalence of UI in women with high intake of caffeine.
Limitations
The role of confounding factors should be considered in interpreting the results of our synthesis. Firstly, increasing age may over shadow the effect of risk as observed in the study by Bradley. Available data did not allow stratification by age, which would have been more appropriate approaches. Smoking could be another confounding as showed in longitudinal study by Arya. Trials that found association between lowering consumption and diminishing symptoms, as that conducted by Tomlinson, included several protocol interventions such as reducing caffeine consumption, altering the quantity and timing of fluid intake, decreasing long daytime voiding intervals, and changing bowel habits, which could have influenced results.
Studies are not able to find association as the one conducted by Hirayama, et al. in Japanese women, whose observations could be attributed to Japanese regular diet or to low consumption of caffeine in women, hinder a broader generalization of results to other ethnic backgrounds. One trial failed to express in detail the basal amounts of caffeine intake and two prospective cohort studies selected subjects whose ethnicity (Caucasian), high educational level, and profession (nurses) restricted generalization of its results.
Conclusions
This systematic review does not seem to support an association between exposure to low and moderate caffeine consumption and incidence of UI. No association was found between consumption and progression of the pathology. Moderate to high caffeine intake was rarely associated with specific symptoms and its restriction did not improve them. However, very high intake (≥ 400 mg) of caffeine was associated with a modest increment of UI incidence. More RCTs are needed to establish the direct relationship of caffeine consumption an UI.
In conclusion, there is insufficient evidence to support caffeine restriction for the improvement of symptoms, except in women with high caffeine intake; therefore, the widespread recommendation of caffeine restriction is not supported by the current literature. Nevertheless, it appears reasonable that women whose intake is greater than 450 mg/day should be advised to diminish caffeine consumption.
Ethical Approval
Not necessary.
Sources of Funding
Self funding.
Conflicts of Interest
None.
References
-
Richter HE, Kenton K, Huang L, Nygaard I, Kraus S, et al. (2010) The impact of obesity on urinary incontinence symptoms, severity, urodynamic characteristics and quality of life. J Urol 183: 622-628.
-
Son YJ, Kwon B (2010) Predictive risk factors for impaired quality of life in middle-aged women with urinary incontinence. Int Neurourol J 14: 250-255.
-
Melville JL, Katon W, Delaney K, Newton K (2005) Urinary incontinence in US women: a population-based study. Arch Intern Med 165: 537-542.
-
Stothers L, Friedman B (2011) Risk factors for the development of stress urinary incontinence in women. Curr Urol Rep 12: 363-369.
-
Hannestad YS, Rortveit G, Daltveit AK, Hunskaar S (2003) Are smoking and other lifestyle factors associated with female urinary incontinence? The Norwegian EPINCONT Study. BJOG 110: 247-254 .
-
Monteiro JP, Alves MG, Oliveira PF, Silva BM (2016) Structure-Bioactivity Relationships of Methylxanthines: Trying to Make Sense of All the Promises and the Drawbacks. Molecules 21: 974.
-
González-Alonso J, Heaps CL, Coyle EF (1992) Rehydration after exercise with common beverages and water. Int J Sports Med 13: 399-406.
-
Moore T, Tubman I, Levy G, Brooke G (2010) Age as a Risk Factor for Perioperative Complications in Women Undergoing Pelvic Reconstructive Surgery. Female Pelvic Med. Reconstr Surg 16: 290-295.
-
Hashim H, Al Mousa R (2009) Management of fluid intake in patients with overactive bladder. Curr Urol Rep 10: 428-433.
-
Stookey JD (1999) The diuretic effects of alcohol and caffeine and total water intake misclassification. Eur J Epidemiol 15: 181-188.
-
Brice CF, Smith AP (2002) Factors associated with caffeine consumption. Int J Food Sci Nutr 53: 55-64.
-
Passmore AP, Kondowe GB, Johnston GD (1987) Renal and cardiovascular effects of caffeine: a dose-response study. Clin Sci (Lond) 72: 749-756.
-
Armstrong LE, Pumerantz AC, Roti MW, Judelson DA, Watson G, et al. (2005) Fluid, electrolyte, and renal indices of hydration during 11 days of controlled caffeine consumption. Int J Sport Nutr Exerc Metab 15: 252-265.
-
Riesenhuber A, Boehm M, Posch M, Aufricht C (2006) Diuretic potential of energy drinks. Amino Acids 31: 81-83.
-
Arya LA, Myers DL, Jackson ND (2000) Dietary caffeine intake and the risk for detrusor instability: a case-control study. Obstet Gynecol 96: 85-89.
-
Ghoniem G, Stanford E, Kenton K, Achtari C, Goldberg R, et al. (2008) Evaluation and outcome measures in the treatment of female urinary stress incontinence: International Urogynecological Association (IUGA) guidelines for research and clinical practice. Int Urogynecol J Pelvic Floor Dysfunct 19: 5-33.
-
Swithinbank L, Hashim H, Abrams P (2005) The effect of fluid intake on urinary symptoms in women. J Urol 174: 187-189.
-
Jura YH, Townsend MK, Curhan GC, Resnick NM, Grodstein F (2011) Caffeine intake, and the risk of stress, urgency and mixed urinary incontinence. J Urol 185: 1775-1780.
-
Tomlinson BU, Dougherty MC, Pendergast JF, Boyington AR, Coffman MA, et al. (1999) Dietary caffeine, fluid intake and urinary incontinence in older rural women. Int Urogynecol J Pelvic Floor Dysfunct 10: 22-28.
-
Bryant CM, Dowell CJ, Fairbrother G (2002) Caffeine reduction education to improve urinary symptoms. Br J Nurs 11: 560-565.
-
Bradley CS, Kennedy CM, Nygaard IE (2005) Pelvic floor symptoms and lifestyle factors in older women. J Womens Health (Larchmt) 14: 128-136.
-
Hirayama F, Lee AH (2012) Is caffeine intake associated with urinary incontinence in Japanese adults? J Prev Med Public Health 45: 204-208.
-
Gleason JL, Richter HE, Redden DT, Goode PS, Burgio KL, et al. (2013) Caffeine and urinary incontinence in US women. Int Urogynecol J 24: 295-302.





