Journal of Clinical Nephrology and Renal Care
Nephrologist Personality Traits and Optimal Renal Replacement Therapy Modality Initiation - "Teamwork Makes the Dream Work"
Agnes Masengu1,2* Melanie Wolfenden1, Alexander P Maxwell1,2 and Jennifer B Hanko1
1Regional Nephrology Unit, Belfast City Hospital, UK
2Nephrology Research Group, Queen's University Belfast, UK
*Corresponding author:
Agnes Masengu, (MRCP) Belfast Health and Social Care Trust, Regional Nephrology Unit, Belfast City Hospital, Lisburn Road, Belfast, BT9 7AB; Nephrology Research Group, Centre for Public Health, Queen's University Belfast, Royal Victoria Hospital, Grosvenor Road, Belfast BT12 6BA, UK, Tel: +44-0-28-95049751, E-mail: amasengu@doctors.org.uk
J Clin Nephrol Ren Care, JCNRC-2-014, (Volume 2, Issue 2), Research Article
Received: August 11, 2016; Accepted: October 10, 2016; Published: October 12, 2016
Citation: Masengu A, Wolfenden M, Maxwell AP, Hanko JB, et al (2016) Nephrologist Personality Traits and Optimal Renal Replacement Therapy Modality Initiation - "Teamwork Makes the Dream Work". J Clin Nephrol Ren Care 2:014.
Copyright: © 2016 Masengu A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background:Personality traits have been associated with job performance. Previous studies have explored nephrologist preferences regarding optimal renal replacement therapy (RRT) outcomes in patients with end-stage renal disease. The role of physician personality traits and patient outcomes has not been investigated. A pilot study was carried out at a single centre to investigate this.
Methods:Eight nephrologists in a single centre were invited to complete a questionnaire examining personality traits (The Big Five Inventory). Incident RRT data for patients under their care from 2011-2014 (n = 185) was collated, and outcomes divided into "optimal" (pre-emptive transplantation, peritoneal dialysis, arteriovenous fistula [AVF] at dialysis start or central venous catheter [CVC] following AVF attempt) and "sub-optimal" RRT initiation (CVC without assessment for AVF creation). The nephrologists were split into two groups: Group A had the highest "optimal" outcome rates while Group B had the lowest. Personality traits were compared between the two groups.
Results:Group A had an optimal start rate of 78% compared to 69% in Group B. Group A had higher levels of Conscientiousness and Neuroticism but this was not statistically significant (P = 0.11). The most common cause of sub-optimal outcome for Group B was late referral for vascular access assessment and for Group A modality change. Using logistic regression, the only predictors of optimal outcome in this cohort was age > 65 years and diabetes.
Conclusions:Nephrologist personality was not a significant predictor of optimal RRT initiation. The power of this pilot study is significantly limited by sample size. However, it suggests that the effects of nephrologist personality may be mitigated by a high functioning, multidisciplinary team and streamlined process pathways which enhance RRT outcomes and patient survival.
Keywords
Decision making, Personality, Renal replacement therapy
Introduction
The nephrologist is a crucial driver in renal replacement therapy (RRT) planning and its delivery for patients with end-stage renal disease (ESRD), which is associated with significant morbidity and mortality [1,2]. Renal replacement therapy (RRT) can take the forms of renal transplantation, in-centre haemodialysis or home dialysis (haemodialysis or peritoneal dialysis). The incident rate of RRT for ESRD in Europe is 117 per million population with a prevalence rate of 692 per million population [3]. The nephrologist must safely navigate an often anxious patient and their family through the convoluted process of adjustment to diagnosis, acceptance of potential treatment plans, multiple interactions between a large multi-disciplinary team [nurses, other specialist medical teams, surgeons, laboratory services, radiologists] and uncertainty with respect to knowing the exact timing of RRT initiation. This complex decision making regarding RRT options is often negotiated with patients who have additional multiple medical problems.
A few studies have explored optimal RRT modality selection from the perspective of the nephrologist. These have relied on questionnaires exploring attitudes, personal preferences and perceived barriers to ideal RRT commencement rather than actual practice [4-7]. A survey of British nephrologists suggested that ideally 50% of patients should be on home dialysis therapies [5]. A survey of American nephrologists revealed that 50% would opt for home dialysis if they faced the prospect of ESRD. Confronted with a similar scenario, 58% of French nephrologists surveyed would opt for pre-emptive renal transplant listing, 21% haemodialysis (HD) and 21% peritoneal dialysis (PD); when limited to dialysis only, 50% chose PD and 50% HD.
Previous work has shown that personality traits can predict job performance [8]. Five core aspects of personality have been described in the literature [9,10] which are independent of cognitive ability [11]. These five dimensions are: Extraversion (seeking fulfilment in sources outside oneself), Agreeableness (reflects how much individuals adjust their behaviour to suit others), Conscientiousness (the trait of being honest and hardworking), Neuroticism (characterised by fear, anxiety and worry) and Openness (the trait of seeking new experiences and intellectual pursuit). Personality traits tend to remain consistent over an individual's life-span [11,12]. Conscientiousness has been correlated with job performance over a variety of occupations [13]. The other four aspects of personality have been associated with performance only in specific settings; for example Extroversion has been associated with performance in jobs where the focus is on influencing others and enhancing status [13].
The role of physician personality and optimal patient outcomes has not been explored. The purpose of this pilot study was to examine nephrologist personality traits and determine if there was any association with increased optimal RRT initiation for patients.
Subjects and Methods
Following ethical approval, eight nephrologists at the Belfast City Hospital, all in post since at least 2011, were invited to participate in the pilot study. Individual consent for the study was obtained. The nephrologists were asked to complete the "Big Five Inventory" [14], which explores the five areas of personality: Extraversion, Agreeableness, Conscientiousness, Neuroticism and Openness. The Big Five Inventory questionnaire (BFI) does not label the individual according to a particular trait per se, but merely suggests the characteristics that the given individual is more likely to display. The BFI has been used to explore the role of personality traits in work performance across multiple professions [13,15-17]. More recently it has been used to explore the role of personality traits in the teaching performance of physicians [15], in stress and burn out in anaesthetists [17] and in the operative role of surgeons [18].
Completed BFI forms were anonymised and coded.
Incident RRT data for all patients under the care of the eight nephrologists (restricted to first ever RRT modality) from January 1, 2011 to December 31, 2014 was collected from the regional nephrology database system eMEDRenal (Mediqual).
Clinical information regarding age, race, gender, ethnicity, primary renal disease, type of vascular access, RRT modality and co-morbidities (diabetes, coronary artery disease, vascular disease, cerebrovascular accident, left ventricular impairment and history of malignancy) was collated. Patients were included in the analysis if they had been followed by a nephrologist for at least 3 months. Patients known to nephrology for more than 3 months were excluded if they had a precipitous start on to RRT due to rapid decline in renal function in the setting of acute illness or unplanned emergency surgical intervention (baseline estimated glomerular filtration rate [eGFR] > 15 mL/min/1.73 m2 for those aged > 75 years or baseline eGFR > 20 mL/min/1.73 m2 for those aged < 75 years at 3 months prior to RRT start). Incident RRT outcomes were divided into "optimal" and "sub-optimal".
"Optimal" RRT starts were defined as patients who received a pre-emptive renal transplant, commenced PD, started HD via an arteriovenous fistula (AVF), or started HD via a central venous catheter (CVC) following either failed AVF attempts or the detection of unsuitable vasculature on ultrasound vessel mapping. "Sub-optimal" starts were defined as those patients who commenced HD via a CVC without timely assessment for AVF creation.
The nephrologists were subsequently divided into two anonymised groups for comparison. The nephrologists with the highest proportion of optimal starts (Group A) were compared to those with the lowest proportion of optimal starts (Group B).
Statistical analysis
Statistical analysis was carried out using SPSS version 22 (IBM Corp, Armonk, NY, USA). The independent samples t-test was used to compare continuous variables while the χ2 test was used to compare the proportions. The Mann-Whitney test was used to compare personality characteristics between Group A and B. Binary logistic regression was used to explore for predictors of optimal RRT starts in this cohort. A P value of less than 0.05 was deemed to be significant.
Results
Three hundred and eighty patients commenced RRT for the first time at Belfast City Hospital during the period of January 2011 - December 2014. Of these, 216 (57%) were followed by the eight nephrologists for more than 3 months. Thirty-one patients (14%) had a rapid unpredictable decline preceding the need for RRT start due to acute illness and were excluded from the final analysis which therefore consisted of 185 patients.
As described in the methods section, the eight nephrologists were split into two groups based on the numbers of optimal starts with Group A having the highest number of optimal starts and Group B the lowest number. The total patient population was 98% Caucasian with a mean age of 60 years. Comparing the patients affiliated to Group A and Group B (mean age 59.9 years versus 60.7 years); both sets of patients had a similar prevalence of diabetes, peripheral vascular disease and ischaemic heart disease. Demographic data on these two subsets of patients are shown in table 1.
![]()
Table 1: Demographics of patients affiliated to group A (n = 114) and group B (n = 71).
View Table 1
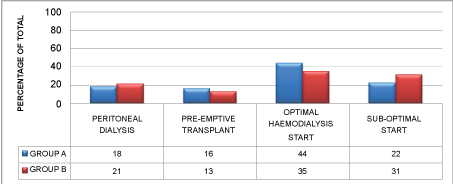
Group A had a total of 114 patients and an optimal start rate of 78% compared to Group B which had 71 first time incident RRT patients with an optimal start rate of 69% (P < 0.001). Group A patients had significantly higher rates of pre-emptive transplantation (P = 0.0001) and optimal dialysis start (P = 0.0001). The optimal and sub-optimal RRT modality rates expressed as the percentage of the total number of Group A and Group B patients respectively is shown in figure 1. Annual optimal RRT rates for patients undergoing RRT initiation from 2011 - 2014 inclusive were 51%, 77%, 91% and 81% respectively.
.
Figure 1: Comparison of optimal and sub-optimal incident renal replacement therapy modalities between nephrologist group A and B.
View Figure 1
Each group of nephrologists had the mean scores of Extraversion, Agreeableness, Conscientiousness, Neuroticism and Openness calculated from the completion of the Big Five Inventory. Group A scored higher on the Conscientiousness (mean score 40 versus 34) and Neuroticism (mean score 22.3 versus 16) traits. The mean scores of each of the five personality traits of the nephrologists are shown in table 2. The Mann-Whitney test was subsequently used to compare the personality component scores between the two groups. The trait of Openness was borderline for significance (P = 0.056) with a higher score for Group B. The other traits showed no statistical difference between the two groups.
![]()
Table 2: Comparison of mean scores on big five personality inventory between nephrologist group A and B.
View Table 2
The reasons for sub-optimal outcomes were elicited from clinical records and compared between the two nephrology groups. In Group B patients, the group with the lower optimal RRT starts, the most common cause of sub-optimal outcome was late referral for vascular access assessment; while for Group A patients, the commonest reason for sub-optimal RRT start was late modality change. Reasons underlying sub-optimal RRT outcomes in each group are listed in table 3.
![]()
Table 3: Causes of sub-optimal outcomes in group A and Group B associated patients.
View Table 3
Binary logistic regression was subsequently used to analyse for predictors of optimal RRT outcome in our cohort. After adjusting for correlated explanatory variables and accounting for confounders, the odds of an optimal RRT outcome were doubled for every year increase in age > 65 years (P = 0.04, OR 2.1, CI 1.0-4.2) and increased three-fold in the presence of diabetes (P = 0.001, OR 3.4, CI 1.6-7.1).
Discussion
RRT planning involves a complex multi-disciplinary approach whose process time-line is not always predictable and the facets of which cannot always be controlled by the nephrologist despite their best efforts. Transplantation offers superior outcomes with regard to morbidity and mortality in the ESRD population [19]. The use of AVFs has consistently been associated with improved survival for haemodialysis patients across all ages [20]. Peritoneal dialysis has been suggested to be superior to HD in the first 3 years of chronic dialysis treatment [21] and is associated with higher quality of life reports including in the very elderly [22]. Quality of life is a crucial element of good clinical care in chronic illness. In our cohort of 185 patients, 75% achieved an "optimal" outcome.
Timing the initiation of discussions regarding RRT planning is not always straightforward, particularly in the elderly who have a more unpredictable course of decline in eGFR [23]. Actual discussions about RRT modality selection can also be difficult. Despite a long follow-up period, patients are sometimes not quite ready to face the consequences of their disease and the nephrologist may feel guilty burdening them with the reality of potential management options and information regarding expected morbidity and mortality. The patient may not fully trust their physician and the nephrologist can be frustrated by the patient's apparent difficulty in believing and/or understanding the severity of their illness as well as its associated implications [24]. In addition to this, the nephrologist may not feel well equipped to tease-out patient concerns [24]. Recent work exploring health-care decision making in over 500 patients with ESRD has alluded to the fact that while patients may prefer to receive information, this does not always imply active involvement in decision making [25].
Tenacity, focus, agreeableness, conscientiousness, extraversion, and emotional sensitivity may all be required to negotiate various stages of the voyage towards achieving optimal patient outcomes. Although not statistically significant (which may be a reflection of the small sample size), the nephrologists in Group A exhibited higher levels of Conscientiousness and Neuroticism. It is interesting to note that although their associated patients had equal amounts of co-morbidity, Group A patients had a superior optimal RRT start compared to Group B. Might this reflect a thorough, vigilant and more dogged approach by their nephrologist or did it simply occur by chance? On the other hand, a nephrologist who is more anxious about a patient may begin RRT discussions earlier than necessary. A prolonged interval between RRT modality choice and modality initiation has been associated with a change in preference [26]. This may account for modality change being the biggest cause of sub-optimal outcome in Group A. Group B had higher levels of Openness of borderline significance. There is a paucity in the literature regarding information linking the trait of Openness and decision making. Openness has been associated with greater risk taking [27].
It is interesting to note that in this cohort older age and diabetes were associated with optimal outcomes. Older patients have a slower rate of decline of renal function which may buffer process delays to some extent [23]. Due to the increasing number of co-morbidities associated with age, it is often easier to identify which patients are unsuitable for transplantation and then focus on dialysis modality type and access early. Older adults in our experience are also more likely to be concordant with management strategies and exhibit less resistance to the creation of an AVF.
Diabetic nephropathy has been associated with the most rapid decline in eGFR compared to other systemic diseases with each unit decline being associated with double the risk of arriving at ESRD in patients with an eGFR less than 30 mL/min/1.73 m2 [28]. As a consequence patients with progressive diabetic nephropathy are followed up closely by nephrologists and guidelines suggest this sub-group of patients commence RRT planning once the eGFR has fallen below 30 mL/min/1.73 m2 [29]. Often diabetic patients with progressive CKD have poor diabetic control that may preclude them from PD and coupled with other co-morbidities that may co-exist such as significant coronary artery disease, in the absence of a live donor, the majority of diabetic patients will commence HD [30]. These factors allow for a more focused approach to RRT planning.
Our study has a number of limitations. It is restricted to a single centre with a small sample of nephrologists which affects the power to detect significant differences regarding the effects of physician personality traits on patient outcomes. It is, however, the only study to date that has sought to compare physician personality and patient outcomes, not just nephrologist preferences for what RRT outcomes we should target [5].
It is not easy to tease out the individual factors involved in the complexities of RRT planning and optimal outcomes. Patients have reported that poor understanding of their chronic kidney disease prior to arriving at ESRD, inadequate educational preparation and limited support with decision making after dialysis initiation are all significant contributors to sub-optimal outcomes [24]. Nephrologists on the other hand have reported the following barriers to optimal outcomes; difficulty establishing working partnerships with patients, difficulties determining their worries and concerns, and failure to truly confirm patient understanding regarding treatment options. It is likely that individual personality traits do play a role in circumventing some of these barriers.
Effective processes and systems that allow for each individual team member in the multi-disciplinary team to focus on areas of their strengths, from the home dialysis education nurse to the vascular surgeon, are more likely to result in long lasting and effective patient gains than the lone actions of a single nephrologist. In our unit, over the last 5 years the creation of pathways that actively support streamlined pre-dialysis, vascular access planning and pre-emptive transplantation work-up processes have resulted in an increase of optimal incident RRT rates from 51% in 2011 to 80% in 2014.
While the power of this pilot study is limited by a small sample size, it does provide a platform for larger studies investigating the role of clinician personality not only in delivering optimal renal replacement therapy but also in selecting non-dialysis care in frail elderly individuals.
Nephrologists face many challenges trying to deliver the best care to persons with ESRD. These difficulties are compounded by the increasing co-morbidity and older average age of ESRD populations. Personality factors, inherent in some clinicians, such as higher levels of Conscientiousness and Neuroticism may play useful roles in achieving good individual patient outcomes. The creation of a high performing multi-disciplinary team driven by the goal of individualised optimal patient outcomes coupled with streamlined care pathways is a more sustainable and effective model for RRT initiation.
Disclosures
None to declare. AM is funded by a grant from the Northern Ireland Kidney Research Fund.
Conflicts of Interest
The results presented in this paper have not been published previously in whole or part including in abstract form.
References
-
Collins AJ, Foley RN, Herzog C, Chavers BM, Gilbertson D, et al. (2010) Excerpts from the us renal data system 2009 annual data report. Am J Kidney Dis 55: S1-420.
-
Carmine Zoccali, Anneke Kramer, Kitty J Jager (2010) Chronic kidney disease and end-stage renal disease-a review produced to contribute to the report ‘the status of health in the european union: Towards a healthier europe'. NDT Plus 3: 213-224.
-
Noordzij M, Kramer A, Abad Diez JM, Alonso de la Torre R, Arcos Fuster E, et al. (2014) Renal replacement therapy in europe: A summary of the 2011 era-edta registry annual report. Clin Kidney J 7: 227-238.
-
Jung B, Blake PG, Mehta RL, Mendelssohn DC (1999) Attitudes of canadian nephrologists toward dialysis modality selection. Perit Dial Int 19: 263-268.
-
Jassal SV, Krishna G, Mallick NP, Mendelssohn DC (2002) Attitudes of british isles nephrologists towards dialysis modality selection: A questionnaire study. Nephrol Dial Transplant 17: 474-477.
-
Schiller B, Neitzer A, Doss S (2010) Perceptions about renal replacement therapy among nephrology professionals. Nephrol News Issues 24: 36-44.
-
Lorcy N, Turmel V, Oger E, Couchoud C, Vigneau C (2015) Opinion of french nephrologists on renal replacement therapy: Survey on their personal choice. Clin Kidney J 8: 785-788.
-
Barrick MR, Mount MK (2005) Yes, personality matters: Moving on to more important matters. Hum Perf 18: 359-372.
-
Norman WT (1963) Toward an adequate taxonomy of personality attributes: Replicated factors structure in peer nomination personality ratings. J Abnorm Soc Psychol 66: 574-583.
-
McCrae RR, John OP (1992) An introduction to the five-factor model and its applications. J Pers 60: 175-215.
-
McCrae RR, Costa PT (1987) Validation of the five-factor model of personality across instruments and observers. J Pers Soc Psychol 52: 81-90.
-
Costa PT, McCrae RR (1997) Longitudinal study of adult personality. In: Hogan R, Johnson J, Briggs S, Handbook of personality psychology. Academic Press, San Diego, 269-290.
-
Barrick MR, Mount MK (1991) The big five personality dimensions and job performance: A meta-analysis. Pers Psychol 44: 1-26.
-
John OP, Srivastava S (1999) The big-five trait taxonomy: History, measurement, and theoretical perspectives.; in Pervin LA, John OP (eds): Handbook of personality: Theory and research. New York, Guilford Press: 102-138.
-
Scheepers RA, Lombarts KM, van Aken MA, Heineman MJ, Arah OA (2014) Personality traits affect teaching performance of attending physicians: Results of a multi-center observational study. PLoS One 9: e98107.
-
Drosdeck JM, Osayi SN, Peterson LA, Yu L, Ellison EC, et al. (2015) Surgeon and nonsurgeon personalities at different career points. J Surg Res 196: 60-66.
-
van der Wal RA, Bucx MJ, Hendriks JC, Scheffer GJ, Prins JB (2016) Psychological distress, burnout and personality traits in dutch anaesthesiologists: A survey. Eur J Anaesthesiol 33: 179-86.
-
Daly SR, Nygaard RM, Van Camp JM (2015) Impact of personality, sex, and generation on resident operative role. J Surg Res 194: 52-56.
-
Wolfe RA, Ashby VB, Milford EL, Ojo AO, Ettenger RE, et al. (1999) Comparison of mortality in all patients on dialysis, patients on dialysis awaiting transplantation, and recipients of a first cadaveric transplant. N Engl J Med 341: 1725-1730.
-
Hicks CW, Canner JK, Arhuidese I, Zarkowsky DS, Qazi U, et al. (2015) Mortality benefits of different hemodialysis access types are age dependent. J Vasc Surg 61: 449-456.
-
Kumar VA, Sidell MA, Jones JP, Vonesh EF (2014) Survival of propensity matched incident peritoneal and hemodialysis patients in a united states health care system. Kidney Int 86: 1016-1022.
-
Brown EA, Johansson L, Farrington K, Gallagher H, Sensky T, et al. (2010) Broadening options for long-term dialysis in the elderly (bolde): Differences in quality of life on peritoneal dialysis compared to haemodialysis for older patients. Nephrol Dial Transplant 25: 3755-3763.
-
O'Hare AM, Allon M, Kaufman JS (2010) Whether and when to refer patients for predialysis av fistula creation: Complex decision making in the face of uncertainty. Semin Dial 23: 452-455.
-
Greer RC, Ameling JM, Cavanaugh KL, Jaar BG, Grubbs V, et al. (2015) Specialist and primary care physicians' views on barriers to adequate preparation of patients for renal replacement therapy: A qualitative study. BMC Nephrol 16: 37.
-
Cornelis T, Tennankore KK, Goffin E, Rauta V, Honkanen E, et al. (2014) An international feasibility study of home haemodialysis in older patients. Nephrol Dial Transplant 29: 2327-2333.
-
Keating PT, Walsh M, Ribic CM, Brimble KS (2014) The impact of patient preference on dialysis modality and hemodialysis vascular access. BMC Nephrol 15: 38.
-
Marco Lauriolaa, Irwin P Levinb (2001) Personality traits and risky decision-making in a controlled experimental task: An exploratory study. Pers Indiv Differ 31: 215-226.
-
Weng SC, Tarng DC, Chen CM, Cheng CH, Wu MJ, et al. (2014) Estimated glomerular filtration rate decline is a better risk factor for outcomes of systemic disease-related nephropathy than for outcomes of primary renal diseases. PLoS One 9: e92881.
-
Tordoir J, Canaud B, Haage P, Konner K, Basci A, et al. (2007) Ebpg on vascular access. Nephrol Dial Transplant 22: 88-117.
-
Locatelli F, Pozzoni P, Del Vecchio L (2004) Renal replacement therapy in patients with diabetes and end-stage renal disease. J Am Soc Nephrol 15: S25-29.