Journal of Clinical Nephrology and Renal Care
Surveillance of Hemodialysis Vascular Access with Temperature Biosensor Combined with Doppler-Ultrasound to Prevent Vascular Failure
Milagros Fernández-Lucas1*, Fernando Caravaca-Fontán2, Antonio Chinchilla3, José-Luis Teruel2, Nuria Rodríguez-Mendiola2, Estefanía Yerovi2, Laura Blanco2, María Delgado2 and Fernando Liaño2
1Department of Nephrology, Hospital Ramón y Cajal, Universidad de Alcalá, Spain
2Department of Nephrology, Hospital Ramón y Cajal, Spain
3Vascular Surgery, Hospital Ramón y Cajal, Spain
*Corresponding author:
Milagros Fernández-Lucas, MD, Department of Nephrology, Hospital Ramón y Cajal
Ctra. Colmenar, Km 9,100, 28034-Madrid, Spain, E-mail: milagros.fernandez@salud.madrid.org
J Clin Nephrol Ren Care, JCNRC-2-016, (Volume 2, Issue 2), Research Article
Received: October 03, 2016; Accepted: December 09, 2016; Published: December 12, 2016
Citation: Fernández-Lucas M, Caravaca-Fontán F, Chinchilla A, José-Luis T, Rodríguez-Mendiola N, et al. (2016) Surveillance of Hemodialysis Vascular Access with Temperature Biosensor Combined with Doppler-Ultrasound to Prevent Vascular Failure. J Clin Nephrol Ren Care 2:016.
Copyright: © 2016 Fernández-Lucas M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Regular surveillance and pre-emptive correction of subclinical stenosis have been shown to be useful procedures for reducing the rate of vascular access (VA) failure. Blood flow (Qa) measurement is considered the best procedure for VA surveillance. Qa below 500 ml/min or reductions over 25% from preceding Qa measurements are predictors of VA thrombosis.
This study shows our experience in monitoring VA by Qa measurements with the temperature biosensor and doppler- ultrasound (DUS). Sixty-four patients recruited in our Dialysis Unit from January to December 2015 were studied at least for six months. Data were collected from the clinical report after informed consent to participate in the study was obtained. All patients had an autologous AVF. Distribution of AVF was: radiocephalic (47%), brachiocephalic (34%), and brachiobasilic (19%). When the patients were recruited, the mean Qa (ml/min) of radiocephalic, brachiocephalic and brachiobasilic was 790 ± 515, 1239 ± 933 and 1452 ± 1109, respectively p = 0.02. AVF Qa below 500 ml/min was detected in 17 patients (26%). DUS revealed a significant stenosis in 11 cases (65%) and poor arterial flow in 6 cases. Despite adequate treatment, thrombosis rate in patients with significant stenosis was 45% (5/11). None of the patients with poor arterial flow developed thrombosis in the follow-up period. AVF Qa higher of 500 ml/min was observed in most patients, 47 (74%). In this group, the thrombosis rate was significantly lower (2/47, 4%) and it was related with ahypercoagulable state.
Conclusions: Regular surveillance of AVF flow with the BTM combined with DUS is an effective method for early detection of autologous AVF dysfunction and prevention of thrombosis, which in turn allow successful AVF repair in a high percentage of cases.
Abbreviations
VA: Vascular Access; Qa: Blood Flow; BTM: Temperature Biosensor; DUS: Doppler-Ultrasound, AVF: Arteriovenous Fistula; AVG: Arteriovenous Grafts; PTA: Percutaneous Transluminal Angioplasty
Background
Native arteriovenous fistula (AVF) is the vascular access (VA) of choice for chronic hemodialysis treatment. Compared with central vein catheters or arteriovenous grafts (AVG), AVF are associated with lower morbidity and mortality rates [1].
Nonetheless, AVF dysfunction is a very common problem in patients on chronic hemodialysis, which causes numerous complications (i.e., decreased dialysis efficiency, use of temporal VA, infections, hospitalizations, etc.) [1,2].
Stenotic lesions due to intimal hyperplasia are the most common cause of AVF malfunction. In most patients, subclinical AVF dysfunction precedes its failure or thrombosis by weeks or months [3,4]. Hence, close monitoring can be a helpful measure for detecting potential treatable lesions.
The blood flow (Qa) measurement is considered the best procedure for VA surveillance [1,5,6]. Most of the available diagnostic techniques for Qa measurement include: Doppler ultrasound (DUS), ultrasound dilution technique, the Crit-line monitor, and those based on differential conductivity or in line dialysance [1,7,8].
DUS provides accurate measures of Qa, although the higher cost, operator skill, and obstacles for its full application during the dialysis session can limit its use [9].
Modern hemodialysis machines are able to directly measure AVF blood flow (AVFQa) through biosensors of temperature or ionic dialysance. These measures can be easily taken during the hemodialysis session with no significant extra cost [10,11].
The Kidney Dialysis Outcome Quality Initiative Guidelines (KDOQI) recommend referral for more comprehensive diagnostic evaluation when the Qa of any AVF falls below 500 ml/min [1]. In addition, the Spanish Guidelines expands this recommendation to any significant reduction of Qa (> 25% from preceding measurement) [12].
The present study shows our experience in monitoring VA and preventing VA failure by Qa measurements with blood temperature (BTM) combined with DUS when a low or a significant drop Qa is detected.
Patients and Methods
Patients
We included stable patients on chronic hemodialysis that were treated in our dialysis unit from January to December 2015 at least for six months. Data were collected from the clinical report after informed consent to participate in the study was obtained. All patients have a native arteriovenous fistula (AVF) because we had not patients with AV grafts during the study period. All of these participants underwent thrice-weekly hemodialysis sessions, and their AVF Qa was regularly examined as a part of routine hemodialysis care.
We analyze the AVF Qa measures at recruitment and 6 months later.
The following clinical information was collected in each patient: demographic, comorbidity (Charlson index) [13], diabetes mellitus, therapy with antiplatelets or anticoagulants, type and vintage of AVF, and time on dialysis treatment. Vascular mapping was performed before AVF creation in all patients. Assisted primary patency (thrombosis-free access survival) was defined as the interval from time of access placement to access thrombosis or the time of measurement of patency [14]. Diabetes mellitus was considered as patients that had prescribed oral hypoglycemic agents or insulin.
Arteriovenous fistula (AVF) blood flow (Qa) measurement
Blood temperature monitor (BTM®) was used to measure Qa (Fresenius machines, 5008). Qa measurements in each patient were performed with the same monitor throughout the entire study period.
The thermodilution method with BTM® was described and validated by Schneitz, et al. [15]. The BTM® induces an initial brief decrease of hemodialysis fluid temperature (-2 °C for 2.5 minutes). This temperature bolus is transferred to the venous blood and detected by the venous sensor. Then this bolus is partially transported through the cardiopulmonary circulation and finally detected by the arterial sensor. The difference between the temperature boluses measured by arterial and venous sensors is equivalent to the percentage of recirculation. AVF Qa is measured by means of the difference in recirculation with normal and inverted lines, with the following equation:
Qa = Qs × (1 - Rx) (1 - Rn)/(Rx - Rn),
Where Qs is the effective blood flow (ml/min), Rx is the recirculation with inverted lines, and Rn is the recirculation obtained with normal lines.
All the above measurements were completed within the first hour of the hemodialysis session, with a constant blood flow and ultrafiltration rate. In most patients, needles were placed at least 5 cm apart to reduce the vascular access recirculation.
Patients returned to normal hemodialysis prescription with the bloodlines in the normal position after measurements were taken. The value of Qa was analyzed as an early predictor of vascular access dysfunction.
Surveillance algorithm
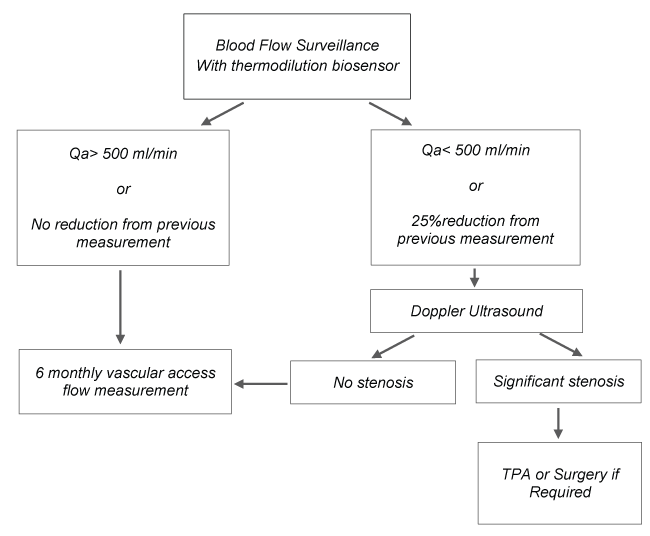
The surveillance method is displayed in figure 1. AVF Qa was measured in all patients at the start of dialysis treatment and subsequently every six months.
In case of AVF Qa below 500 ml/min and/or a reduction over 25% from preceding Qa measurements, a DUS survey would be indicated. DUS was performed with a Toshiba Xario® SSA-660A machine by a nephrologist with more than five years' experience in the field of AVF DUS.
Stenosis diagnosed by 50% reduction of the vessel lumen with impact on the fistula flow was treated with percutaneous transluminal angioplasty (using a 5-French sheath) and stent placement if required. When angioplasty was not indicated or failed, surgical examination and new anastomosis creation was the most usual procedure for trying to maintain AVF patency.
Design and statistical analysis
This study is a single-center observational cohort study. Results are expressed as the arithmetic mean ± standard deviation, or median and interquartile range [IQR], as appropriate.Quantitative variables were compared between groups by ANOVA or the Kruskal-Wallis test if the conditions for ANOVA were not satisfied. Kaplan-Meier survival analysis was used to calculate the survival rate for each AVF type. Cox-Mantel log-rank test was used to assess differences in patency rates among AVF types. A p value < 0.05 was considered statistically significant. Data were analyzed using SPSS software version 15 (IBM SPSS Statistic, New York, USA).
Results
The study group consisted of 64 patients. Their main clinical characteristics are summarized in table 1. Twenty-three patients (29%) were diabetics. Only 8 (12%) out of the 64 study patients were on anticoagulant therapy, and 23 (36%) on anti-platelet therapy.
![]()
Table 1: Characteristics of the study patients.
View Table 1
Five patients were transplanted and 9 died during the study period.
The most common AVF type was radio-cephalic (47%) followed by brachio-cephalic (34%), and brachio-basilic (19%). As would be expected, significant differences in mean Qa among AVF types were found (Table 1). No differences were found in AVF Qa between sexes.
Recirculation was measured with BTM®, and the median value of this parameter was 13.8% [IQR 5-40 %].
According the AVF Qa measurement at recruitment, the patients were divided into those with a lower or higher flow of 500 ml/min.
Patients with Qa lower than 500 ml/min
The AVF Qa below 500 ml/min was detected in 17 patients (26%). In this group of patients, 47% were diabetics (n = 8). The follow-up of the AVF patency was 6 ± 3 (1-11.5) months. Table 2 summarizes the main characteristics and outcomes of the AVF of this group of patients. DUS revealed a significant stenosis in 11 cases (65%), and primary atherosclerotic narrowing of the feeding artery with poor blood flow in 6 cases. All but one patient with poor artery blood flow were diabetics.
![]()
Table 2: Patients with AVF Qa lower than 500 ml/min at recruitment, procedures and clinical outcomes.
View Table 2
Nine of the 11 patients with significant stenosis had a previous AVF flow measurement before the recruitment, and all but one showed a reduction over 25% from preceding Qa.
All significant stenosis were confirmed by fistulography.
Nine patients with significant stenosis were treated with balloon-catheter angioplasty and 2 with surgery. Five of them eventually developed AVF thrombosis after 1 (two cases), 3, 4 and 8 months of the procedure (case 1, 2, 5, 8 and 14, table 2). In three patients we could not measure the flow after the procedure due to they had an early thrombosis, but in the two patients who had a flow’ measure after the procedure, the flow had not increased significantly.
The six patients whose flow increased significantly after the procedure had no vascular complications during the whole study period (case 3, 7, 10, 12, 13 and 17) (Table 2).
Despite treatment, the thrombosis rate in patients with significant stenosis was 45% (5/11).
No relationship was found between the thrombosis rate and anticoagulant or anti-platelet therapy. Two patients died for reasons not related to vascular access one and three months after the treatment of the stenosis (case 10 and 13).
No interventions were performed in the 6 patients with poor arterial blood supply except regular surveillance, and none of them developed AVF thrombosis during the study period (case 4, 6, 9, 11, 15 and 16). In this group, the AVF flow determination six months later showed similar values.
Patients with Qa higher than 500 ml/min
The AVF Qa higher of 500 ml/min was detected in 47 patients (74%). The follow-up of the AVF patency in this group was 8 ± 2.6 months (1-11).
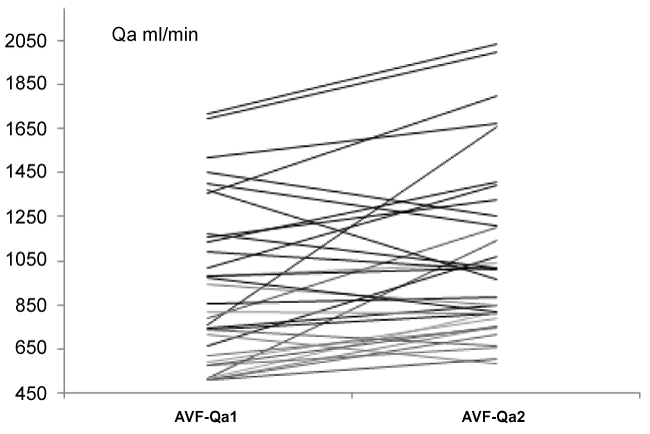
The fistula flow was measured six months later in 40 patients, and anyone had a flow bellow 500 ml/min (Figure 2).
.
Figure 2: AVF flow in patients with Qa higher than 500 ml/min at recruitment and six months later.
AVF-Qa1: VA flow at recruitment; AVF-Qa2: VA flow after 6 months.
View Figure 2
The thrombosis rate in this group was 4% (2/47). Two patients developed a thrombosis one and three months after the basal Qa determination (VA flow: 962 and 1143 ml/min, respectively) but in both cases it was associated with a hypercoagulable state.
DUS was not performed routinely in this group of patients.
Discussion
A multidisciplinary approach with strong commitment of nephrologists, vascular surgeons and radiologists seem crucial to achieve optimal AVF care in chronic hemodialysis patients [7]. KDOQI guidelines outline the basic tools to early detect AVF dysfunction, including monitoring and surveillance methods [1]. The results of this study show that regular surveillance of AVF blood flow with the BTM combined with Doppler-ultrasound when detected a low flow is an effective method for early detection of AVF dysfunction.
Non-modifiable factors such as ageing and comorbidity, and modifiable factors such as smoking, obesity, or post-dialysis hypotension could affect AVF patency [8]. In the present study, all patients have an autologous AVF and pre-surgery mapping to indicate the type of AVF is made in all of them. The age and comorbidity of patients were similar to those described in other studies. Of note, a high proportion of the study patients were diabetics, and arterial blood supply problems were mainly found in this group of patients, despite of routine vessel mapping before AVF creation. However, no interventions were performed in the 6 patients with poor arterial blood supply except regular surveillance, and none of them developed AVF thrombosis during the study period.
Although the number of thrombosis was low, we did not find relationship between antiplatelet or anticoagulant therapy and thrombosis.
Surveillance is defined as the periodic evaluation of the vascular access with tools and instrumentation that may suggest the presence of dysfunction [1]. Different approaches have been reported, although a combined step-by-step screening algorithm may increase accuracy [10,16,17]. The surveillance protocol used in this observational study has several advantages: it is fairly easy to perform and measurements can be taken by hemodialysis personnel during the dialysis session, with no need to administer isotonic saline indicator. In addition, as BTM biosensor is incorporated in hemodialysis machines, no additional investment is needed.
In a previous study we observed as flow measurement with temperature biosensor has a good correlation with the ultrasound dilution method, both hemodialysis and online hemodiafiltration [18]. But it has been also reported that AVF Qa measurement may differ between different techniques [11,19]. However, we observed that the measuring method is reproducible if the same type of biosensor is used to track the flow in each patient [20].
One of the main drawbacks when using thermodilution sensors is that the same vein must be punctured in order to take subsequent measurements with normal and inverted lines.
We note that the flow of radio-cephalic AVF is significantly lower than braquio-cephalic and braquio-basilic without implying pathology at the level of the AVF, but no differences were found in AVF flow between sexes.
In our surveillance method, if the flow is below 500 ml/min or a reduction over 25% from preceding Qa measurements is detected, a DUS was indicated. DUS was performed by a nephrologist with more than five years' experience in the field of AVF DUS. If significant stenosis is not detected, regular checks flow AVF are performed every six months.
The use of DUS is time-consuming, and cannot be used routinely for the screening of vascular access dysfunction, however the routine measurement of the AVF flow allows us to identify patients at special risk who could benefit from a specific ultrasound scan.
Most patients with lower flow at 500 ml/min had disturbances in Doppler ultrasound, showing an excellent sensitivity to detect any dysfunction. The low flow mainly when associated with a significant decrease from prior checking is strongly suggestive of significant stenosis, but it should be noted that AVF DUS requires specific training to differentiate hemodynamic significant from non-significant stenosis. In this respect, it’s also important to point that the ultrasound is performed by an experienced nephrologist that can better relate the morphological findings to the functional impact.
Preemptive percutaneous transluminal angioplasty has been advocated as the treatment of choice for underlying AVF stenosis [21,22]. Our results are similar to that found in other studies, with a highly successful AVF repair after angioplasty, and significant improvement of AVF Qa [5,10,19].
However, this treatment is not always successful, and thrombosis may occur after the initial intervention, especially if the flow does not increase after the procedure. Despite treatment, the thrombosis rate in our patients with significant stenosis was 45%, so it would be better to do the regular surveillance every three months to improve early detection of stenosis.
There were no found relationship between thrombosis and anticoagulant or anti-platelet therapy.
AVF lesions considered unsuitable for angioplasty were remitted for further surgical evaluation. However, the small number of these cases in our study does not allow us to compare both procedures.
In five diabetic patients an arterial poor flow was detected and did not have to make any therapeutic procedure. The flow was stable compared the next control and none of these patients had thrombosis of the fistula during a mean follow-up of eight months.
The AVF Qa was higher than 500 ml/min in most patients, and no major complications were observed during a mean follow-up of eight months except in two patients who developed an unexpected thrombosis that was related to a hypercoagulable state. The percentage of diabetics in this group was lower. The thrombosis rate in this group was significantly lower compared to patients with AVF Qa lower than 500 ml/min.
The main limitation is that it is an observational single-center study. Besides, due to the small number of events observed, other major risk factors for AVF thrombosis could not be identified. In addition, the surveillance method could not be applicable for AVF grafts, considering there were not patients with grafts in our dialysis unit.
Conclusions
Regular surveillance of AVF blood flow with the BTM combined with Doppler-ultrasound is an effective method for early detection of autologous AVF dysfunction and prevention of thrombosis. The routine measurement of the AVF flow with the BTM is enough easy to perform during the dialysis sessions with no additional extra-costs and itis useful to identify patients at special risk who could benefit from an ultrasound scan. Nevertheless in our experience, the regular surveillance every six months could delay the diagnosis of some vascular access stenosis, so we recommend to do the regular surveillance every three months to improve the early detection of stenosis. Finally, the surveillance method could not be applicable for AVF grafts, considering there were not patients with grafts in our dialysis unit.
Authors' Contributions
All authors read and approved the final manuscript.
Informed Consent
Informed consent to participate in the study and to publish the results was obtained from all participants. As data obtained were derived from routine clinical practise no further consents were obtained.
Availability of Data
The data will not be shared because there were derived from the clinical report of the patients.
Competing Interests
None of the authors have competing interests.
References
-
National Kidney Foundation (2006) KDOQI Clinical Practice Guidelines and Clinical Practice Recommendations for 2006 Updates: Haemodialysis Adequacy, Peritoneal Dialysis Adequacy and Vascular Access. Am J Kidney Dis 48: 1-350.
-
Allon M, Robbin ML (2002) Increasing arteriovenous fistulas in hemodialysis patients: problems and solutions. Kidney Int 62: 1109-1124.
-
Lok CE, Bhola C, Croxford R, Richardson RM (2003) Reducing vascular access morbidity: a comparative trial of two vascular access monitoring strategies. Nephrol Dial Transplant 18: 1174-1180.
-
Gallieni M, Martini A, Mezzina N (2009) Dialysis access: an increasingly important clinical issue. See Int J Artif Organs 32: 851-856.
-
Tessitore N, Bedogna V, Poli A, Mantovani W, Lipari G, et al. (2008) Adding access blood flow surveillance to clinical monitoring reduces thrombosis rates and costs, and improves fistula patency in the short term: a controlled cohort study. Nephrol Dial Transplant 23: 3578-3584.
-
Polkinghorne KR, Lau KK, Saunder A, Atkins RC, Kerr PG (2006) Does monthly native arteriovenous fistula blood-flow surveillance detect significant stenosis-a randomized controlled trial: Nephrol Dial Transplant 21: 2498-2506.
-
Vachharajani TJ (2012) Diagnosis of arteriovenous fistula dysfunction. Semin Dial 25: 445-450.
-
Smith GE, Gohil R, Chetter IC (2012) Factors affecting the patency of arteriovenous fistulas for dialysis access. J Vasc Surg 55: 849-855.
-
Zamboli P, Fiorini F, D'Amelio A, Fatuzzo P, Granata A (2014) Color Doppler ultrasound and arteriovenous fistulas for hemodialysis. J Ultrasound 17: 253-263.
-
Fontsere N, Mestres G, Burrel M, Barrufet M, Montana X, et al. (2014) Observational study of surveillance based on the combination of online dialysance and thermodilution methods in hemodialysis patients with arteriovenous fistulas. Blood Purif 37: 67-72.
-
Merino JL, Teruel JL, Galeano C, Fernández Lucas M, Ocaña J, et al. (2006) Blood flow determination in vascular access with ionic dialysance. Nefrologia 26: 481-485.
-
Rodriguez Hernandez JA, Gonzalez Parra E, Julian Gutierrez JM, Segarra Medrano A, Almirante B, et al. (2005) Vascular access guidelines for hemodialysis: Nefrología 25: 3-97.
-
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40: 373-383.
-
Sidawy AN, Gray R, Besarab A, Henry M, Ascher E, et al. (2002) Recommended standards for reports dealing with arteriovenous hemodialysis accesses. J VascSurg 35: 603-610.
-
Schneditz D, Wang E, Levin NW (1999) Validation of haemodialysis recirculation and access blood flow measured by thermodilution. Nephrol Dial Transplant 14: 376-383.
-
Mercadal L, Hamani A, Bene B, Petitclerc T (1999) Determination of access blood flow from ionic dialysance: theory and validation. Kidney Int 56: 1560-1565.
-
Coentrao L, Turmel-Rodrigues L (2013) Monitoring dialysis arteriovenous fistulae: it's in our hands. J Vasc Access 14: 209-215.
-
Fernández-Lucas M, Diaz F, Teruel JL, Gomis A, Elias S, et al. (2011) Estudio comparativo de la determinacion del flujo de la FAV por dilucion ultrasonica, modulo de temperatura de sangre (BTM) y ecografia doppler. Nefrología 31: 78.
-
Sacquepee M, Tivollier JM, Doussy Y, Quirin N, Valery JC, et al. (2012) Comparison of different techniques of hemodialysis vascular access flow evaluation: blood temperature monitoring thermodilution and dopplerdebimetry. NephrolTher 8: 96-100.
-
Raoch V, Fernandez-Lucas M, Hernandez R, Caravaca F, Pampa S, et al. (2014) Quereda. Medicion del flujo del acceso vascular por termodilucion y por dialisancia ionica. Nefrologia 34: 68.
-
Tessitore N, Lipari G, Poli A, Bedogna V, Baggio E, et al. (2004) Can blood flow surveillance and pre-emptive repair of subclinical stenosis prolong the useful life of arteriovenous fistulae? A randomized controlled study. Nephrol Dial Transplant 19: 2325-2333.
-
Agarwal AK, Thakkar A, Haddad NJ (2015) How is arteriovenous fistula longevity best prolonged? The role of percutaneous balloon angioplasty. Semin Dial 28: 27-29.