Journal of Family Medicine and Disease Prevention
Rationing of Healthcare Services: An Economic Critique
Peter Zweifel*
Department of Economics, University of Zurich, Switzerland
*Corresponding author: Peter Zweifel, Professor of Economics em., Department of Economics, University of Zurich, Switzerland, E-mail: peter.zweifel@uzh.ch
J Fam Med Dis Prev, JFMDP-1-005, (Volume 1, Issue 1), Orginal Research; ISSN: 2469-5793
Received: April 18, 2015 | Accepted: June 03, 2015 | Published: June 06, 2015
Citation: Zweifel P (2015) Rationing of Healthcare Services: An Economic Critique. J Fam Med Dis Prev 1:005. 10.23937/2469-5793/1510005
Copyright: © 2015 Zweifel P. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The starting point of this contribution is the fact that budgets imposed by health policy makers induce rationing, causing inefficiencies in the market for medical services. In addition, inefficiencies spill over into the market for health insurance. In a second step, rationing itself is explained as the outcome of supply and demand for regulation. It is shown that the mere existence of health insurance creates a demand for rationing that increases over time. The contribution concludes with a description of the instruments at the disposal of health insurers designed to make the insured opt for policies with self-limitation features. Thus, insurers can help to limit the demand for rationing and the inefficiencies that come with it.
Keywords
Rationing, Economic theory, Health care, Health insurance
1. Motivation and Objective
Triggered by Callahan (1987), there has been a debate in the media as well as in medical science Klein et al. [1] and health economics [2] revolving about the rationing of healthcare services. From an economic point of view, the amazing fact is that this debate does not create a revolt of public opinion. After all, rationing is a feature of the war economy, constituting a means for the government to rapidly appropriate a greater share of the social product - an endeavor that normally would cause prices of goods and services to rise substantially. By imposing rationing, a wartime government seeks to attain two objectives. On the one hand, citizens with modest incomes are to be protected from the price hike, which would force them to go without certain goods and services considered essential. On the other hand, producers and distributors are prevented from reaping windfall profits, which would undermine the social cohesion of a country at war. Therefore, rationing health care services could be justified if major groups of the population did not have access to medical care anymore due to quickly rising fees or if the incomes and profits of service providers in health care were rising at a rate that constitutes a threat to the social fabric of the country.
Neither condition seems to be satisfied in the industrial countries at present. True, the health share of the Gross Domestic Product (GDP) has increased substantially over the years; the OECD average now is at 9.3 percent, up from 6 percent in 1970 (OECD, Health Statistics, 2015). In a few countries, the increase has been even more dramatic. However, the surge is still a far cry from e.g. the one caused by the war effort of the United States after the start of World War II, causing the GDP share of federal government to increase from 1.7 percent in 1939 to 5.7 percent in 1945 (U.S. Census Bureau, 1999). Yet, there is a parallel between rationing of healthcare services and rationing in the war economy, viz. excess demand at given prices. In the case of the war economy, excess demand is the consequence of the government's claim on additional resources that is imposed without increasing the rate of taxation. In the case of the healthcare sector, excess demand is fueled by health insurance in combination with subsidies (usually to hospitals) that put increasing pressure on the public budget, while the government seeks to avoid an increase in the tax rate. As will be argued in this paper, it is sufficient for the government to impose a binding budget constraint on healthcare outlays to induce rationing. For, this constraint in all likelihood is incompatible with individual decisions in the healthcare sector.
Rationing is a method to overcome scarcity. It calls on individual demanders of healthcare services to scale back their demands, while service providers must assume additional responsibilities in the allocation of scarce resources. Both aspects have legal and ethical implications that will not be addressed in this paper. Rather, economic argument will be at center stage. For this purpose, it is appropriate to emphasize the parallels between rationing and the war economy. More generally, rationing can be viewed as a type of regulation. This view can be justified by noting that rationing in health care is not conceived of as an emergency measure that will be repealed after a relatively short period of time. For several years now, rationing increasingly has been governing the provision of healthcare services, very much like public regulation of any market.
Economic theory has a good deal to say about public regulation [3]. The concept is one of a market for regulation consisting of demanders and suppliers, whose equilibrium may shift over the course of time.
Against this backdrop, this contribution has three objectives. First, it seeks to recall the fact that rationing, even if only indirectly induced by public budgeting, causes losses of efficiency. It will be shown that these losses do not only burden the market for medical care, but also the market for health insurance. Next, it seeks to demonstrate that the present financing of healthcare, be it through health insurance or tax revenues, serves to induce demand for the regulatory service called 'rationing of health care'. Under rather general conditions, this results in a future increase in the intensity of rationing and hence of the efficiency losses imposed. For this reason, the third objective is to describe alternatives to rationing. Particular emphasis will be put on the contribution that both public and private health insurers can make to obviate rationing imposed by the government.
The plan of this paper is as follows. Section 2 introduces basic economic theory in order to show that a fixed public budget allocated to health typically induces a rationing of healthcare services that causes efficiency losses in the market for medical services. Moreover, the economic theory of insurance demand points to efficiency losses also in the insurance economy. Section 3 returns to the basic idea, sketched in the preceding paragraph, of viewing rationing as a type of public regulation for which a market can be defined. It introduces potential demanders and suppliers of rationing and explains the properties of the market clearing price of regulation. Moreover, demand for rationing is closely related to the well-known concept of 'moral hazard' in insurance theory. Section 4 takes a normative stance, asking the question of how the efficiency losses caused by rationing of healthcare services can be avoided or at least reduced. In important insight here is the observation that individuals successfully ration themselves in their daily lives by keeping their consumption expenditures within the limits prescribed by their income and wealth. In the case of the healthcare sector, the mission of health insurers may be to create the potential for such self-limitation by designing their policies accordingly. However, they must offer compensation in the guise of reduced contributions. Section 5 is devoted to the summary and a restatement of the principal conclusions.
2.Effects of Rationing
2.1 Rationing and efficiency losses on the market for healthcare services
Clearly, the rationing of healthcare services affects the market for medical services. However, it also has effects on the market for health insurance, regardless of whether the managed care type prevalent in the United States, the statutory type as in Germany, or again of the National Health Insurance type such as in Canada. As to reimbursement health insurance (typically the domain of private health insurers), there might even be efficiency gains. These considerations are relegated to Section 2.2.
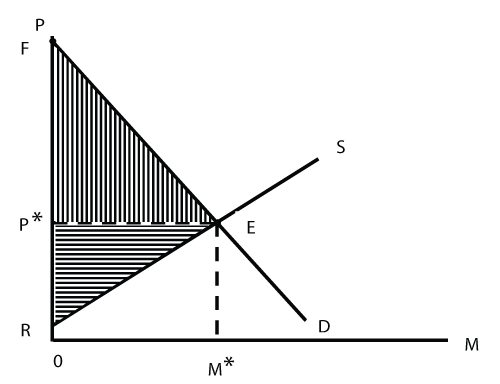
In order to illustrate the effects of rationing, a competitive market for healthcare services is assumed. This is for simplification only; the main results carry over to the cases of monopoly and oligopoly. Thus, the fact that providers typically are organized in associations that negotiate fees with health insurers or public authorities is neglected. Since outcomes of negotiations cannot deviate too much from market outcomes, this simplification does not cause a major loss of generality. However, the existence of health insurance raises the issue of whether a normal demand function decreasing in price may be drawn as in figure 1 because it is designed to protect patients from the cost (and hence the price) of health care. However, a normal demand function D is appropriate as long as health insurance imposes a degree of copayment, which causes higher prices for healthcare services to be passed on to patients. Therefore, the quantity demanded M decreases with a higher price P.
On the supply side, the function S (especially in the case of physicians) could be backward bending, implying that the amount of services provided diminishes with an increasing fee level. However, once the time period considered is extended to several years, higher fees attract more individuals into the practice of medicine (and into supplying healthcare services in general). These considerations justify the positive slope of the supply function in figure 1. In equilibrium E, conditional dispositions of the two groups are in accordance with the volume of services transacted being M* at a price level P*.
Viewed from below, the demand function D indicates the amount of money that insured patients are willing to pay for an additional unit of medical care. Thanks to competition, they have to pay only the market price P*, creating a net benefit (called consumer surplus) amounting to the area P*FE in figure 1. Conversely, the supply function S indicates the price that service providers must be paid at a minimum for them to be active on this market. The market price exceeds this minimum for efficient suppliers, creating a net benefit for them as well (called producer surplus, area P*RE). It can be shown that in market equilibrium the sum of consumer and producer surplus is maximized, which demonstrates the efficiency of competitive markets [4].
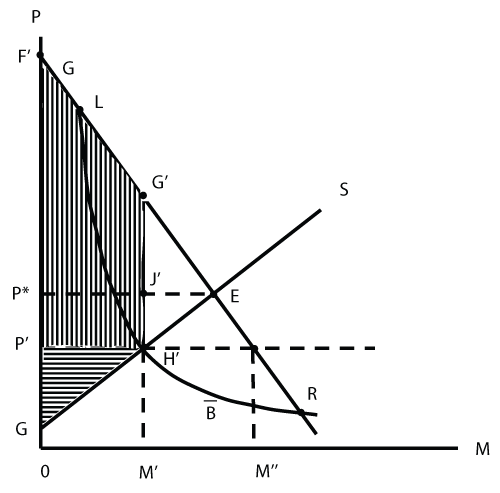
The particularity of health care is that the government contributes to its financing in many ways, ranging from subsidization of medical education to financing the investment of hospitals and on to premiums subsidies for the poor [5]. The problem with these contributions is that once they have become law, they do not contribute much to the chance of (re)election of politicians, compared to the targeted subsidization of pivotal voter groups [6], who show that in the Netherlands, social transfers generally increase during and around election years]. For the subsidies considered here, politicians seek to keep them stable; specifically, deficits of hospitals and of social insurance schemes are to be avoided because they would reduce the public budget that is available for manipulation in the interest of (re-)election. For the healthcare system, this argument implies a predetermined budget for a given period. Recalling that expenditure is the product of price P times quantity M, this restriction is shown in figure 2 as a hyperbola at the level . The supply and demand functions are carried over unchanged from figure 1 because patients and service providers can be assumed to cling to their dispositions regardless of the budget constraint imposed by the government.
From figure 2, it becomes evident that imposing a budget designed to save money entails rationing. True, the hyperbola could in principle go through point E if the budget is high enough. But since both price and quantity (and hence healthcare expenditure) would be left unchanged, budgeting would not generate any savings. The logic of budgeting implies that the hyperbola has to run closer to the origin than point E, as drawn in figure 2. Points L and R, while compatible with the dispositions of patients because they lie on the demand function, are incompatible with the dispositions of service providers. The one solution within the budget that lies on their supply function S and therefore is compatible with their dispositions is indicated by point H'.
However, at the corresponding (low) price P', patients would like to have access to the quantity M'' of healthcare services whereas service providers are prepared to supply the quantity M'<M'' only. To bridge this discrepancy, they must therefore resort to rationing. The devices used range from making patients wait (causing some of them to go without an office visit) to denying certain types of surgery especially to older patients. A comparison between figures 1 and 2 reveals that rationing causes a reduction in both consumer surplus (the vertically hashed area) and producer surplus (the horizontally hashed area) and hence a loss in efficiency. These effects have been known to economists for a long time [7].
Rationing is likely to become harsher over time. Advances in medical therapy and technology serve to enhance demand by patients. In terms of figure 2, their demand curve shifts outward, indicating that at a given price, patients would like to have more health care. With an unchanged budget , the discrepancy between the (shifted) market equilibrium and point H' increases. This increasing tightness of rationing can be easily related to the intensification of the debate about rationing in the healthcare sector that has occurred since the 1990s. Finally, the model also predicts pressure on medical fees (see the transition from P* to P in figure 2). This pressure may not have resulted in nominal reductions of physician fees but rather a failure to adjust them to inflation, causing them to decrease in real terms. Indeed, several OECD countries have seen the medical incomes approach the average wage in the course of the 1990s. However, this may not only be the effect of rationing but also of increasing density of physician supply [8].
Conclusion 1: Imposing a budget on health care entails a rationing of healthcare services that causes a fall in both consumer and producer surplus and hence efficiency losses in the market for healthcare services, which tend to increase over time.
2.2 Effects on the market for health insurance providing in-kind benefits
The rationing of healthcare services affects not only the market for medical care but has repercussions on the market for health insurance, especially that providing in-kind benefits (as is typical of social and public insurers). Although these insurers are not-for-profit, an increasing supply function is assumed as in figure 1, very much as would be derived from the maximization of expected profits. This can be justified by noting that competitive social insurers cannot deviate too far from the for-profit benchmark because they would be jeopardizing their economic survival. In particular, a low price of insurance (given not by the premium but by the so-called 'loading', i.e. the excess contained in the premium over and above what is needed to cover the expected value of benefits paid), forces them to back scale operations and may even cause their exit from the market.
Conversely, a high premium (again in relation to expected benefits) makes a health insurer unattractive for consumers, causing it to lose market share. At the aggregate level, more individuals try to avoid mandatory health insurance (notably by working in the shadow economy). Therefore, again as in figure 1, a negative slope of the demand function obtains. Since a demand function reflects (marginal) willingness-to-pay, any reduction in willingness-to-pay for insurance coverage causes it to shift toward the origin. As can be easily read off from figure 1, this results in a loss of both consumer surplus (vertically hatched area) and producer surplus (horizontally hatched area) in the market for health insurance providing in-kind benefit.
However, the rationing of healthcare services entails precisely such an inward shift of the demand function. The reason is that willingness to pay for insurance depends (for a given degree of risk aversion on the part of the consumer) on the variance of the asset at risk [9]. Willingness-to-pay is maximum if insurance provides perfect security by reducing the variance of the asset to zero. Failing perfect security, willingness to pay decreases. Now any rationing in health care causes asset volatility to increase because it makes patients uncertain as to whether they will have access to healthcare services. This uncertainty spills over to in-kind health insurance, which does not provide access to health care under all circumstances anymore. Therefore, willingness to pay for health insurance providing in-kind benefits must fall due to rationing. In analogy to figure 1, the demand function (for health insurance this time) shifts towards the origin 1, causing the quantity of insurance transacted, producer surplus, and consumer surplus to decrease. This amounts to another, more indirect loss of efficiency.
2.3 Effect of rationing on reimbursement health insurance
Private health insurance typically reimburses patients rather than providing in-kind benefits. Rationing of healthcare services has two effects on the demand for reimbursement health insurance. On the one hand, rationing can be so strict as to effectively block access to the pertinent medical service even though the patient, being covered for much extra healthcare expenditure, is prepared to pay a high price. This again confronts the insured with an increased volatility of their asset 'health', as argued in Section 2.2. Therefore, willingness to pay for insurance coverage of the reimbursement type decreases.
The second possibility appears to be more realistic in most cases. By having reimbursement insurance paying an extra amount, patients can avoid rationing, granting them unfettered access to the desired service. This means that rationing of healthcare services boosts the demand for reimbursement health insurance, provided always that the health insurer does not cap payment on a per-service basis. Therefore, the quantity transacted on the market for reimbursement health insurance typically increases, and with it, consumer and producer surplus.
The findings so far have been that rationing of medical care entails a reduction in the demand for insurance with in-kind benefits but an increase in the demand for reimbursement health insurance. Since the reduction and the increase in willingness to pay for insurance coverage need not balance, the overall impact on efficiency is ambiguous in principle. However, in most industrial countries, public and social health insurance with their in-kind benefits account for the lion share of the financing of health care. Therefore, rationing of health care is likely to result in a loss of efficiency at the level of the aggregate health insurance market.
Conclusion 2: Rationing of health services curtails demand for health insurance with in-kind benefits and may boost demand for reimbursement health insurance. At the aggregate level, a loss of efficiency is likely to prevail.
3. The market for rationing in health care
3.1 Theoretical background
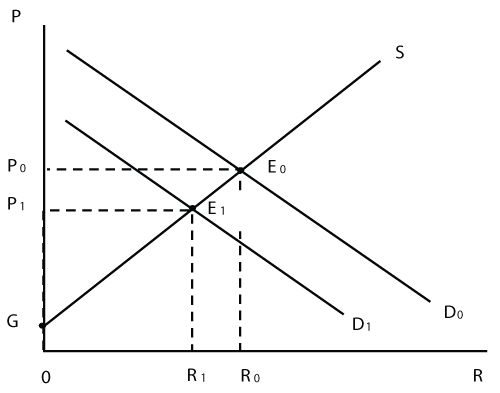
While rationing is related to the war economy, it may in fact be imposed permanently in peacetime by governments who seek to impose budgetary limits, as shown in section 1. In this way, rationing amounts to a type of public regulation. The analogy between rationing of healthcare services and regulation permits to relate to Peltzman's theory of regulation [3]. It posits a market for the service called 'regulation'. For simplicity, the fact is neglected here that there may be only one demander and one supplier of regulation (in some cases, only government demands regulation, while only public administration can be its supplier. Rather, the level R0 shown in figure 3 pertains to a competitive market.
On the demand side of the market for the regulatory service called 'rationing of health care', there are two groups of demanders. On the one hand, government can only implement its budget limit if the volume of services in the healthcare sector is indeed reduced (to M' in figure 2). In a democracy, governments pay the price of rationing in the guise of votes lost, entailing an increased risk of losing the next election. Members of government may see their income as well as other benefits curtailed. If these disadvantages are important (i.e. price is high), the government has a small demand for regulation. Therefore, the demand function in figure 3 has negative slope as far as the government is concerned.
The second groups of demanders for the regulatory service 'rationing of health care' are the health insurers. As will be shown in Section 4, they dispose of their own means that can substitute for rationing. However, they may be constrained in their development of policies through cartelistic collusion or by legislation, making rationing by the government a viable alternative in spite of its disadvantages. After all, rationing does mitigate the effects of co-called moral hazard (see Section 3.2). For health insurers, the price of rationing is its negative effect on the demand for coverage, causing a loss of clientele (see Sections 2.2 and 2.3). If this reaction by consumers causes substantial losses in terms of contribution to profit or cost recovery, insurers' demand for rationing is limited as well. On the other hand, if such losses are minor, rationing has a low price, inducing a higher propensity to resort to it. Therefore, the demand function of this second group has negative slope as well. The two components of demand combine to form the function D0 shown in figure 3.
3.2 Health insurance as a determinant of the demand for rationing
As expounded in Sections 2.2 and 2.3, rationing of healthcare services has a negative impact on the overall demand for health insurance. At this juncture, the objective is to show that the very existence of health insurance (private, social, or public) may induce demand for the regulatory service 'rationing'. The reason is moral hazard, as explained with the help of figure 4.
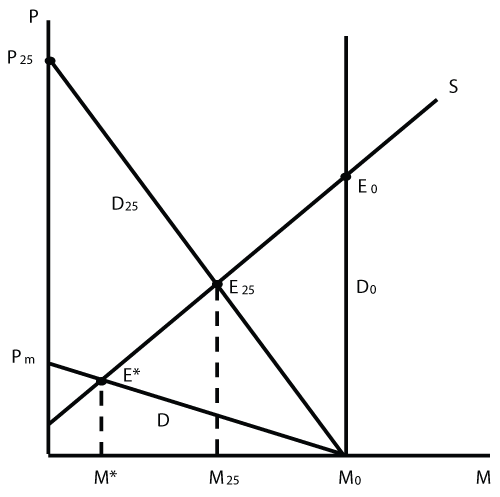
This time, the market for a specific medical service such as a drug is depicted. In figure 4, the true demand function D reflects patients' willingness-to-pay out of pocket. Price Pm symbolizes the amount that a patient who depends on the drug to the highest degree is prepared to pay. Let this maximum price be $100. In view of the supply function S, the equilibrium without health insurance would be characterized by E*, entailing a relatively limited quantity of the drug transacted M*.
The situation changes under the influence of health insurance. In the interest of simplicity, a few facts are neglected, notably that a premium must be paid out of current income, that there may be a deductible, and that insurers may pay reference prices only. Given these simplifications, and with an assumed rate of coinsurance of 25 percent (say), the drug considered here may cost as much as $ 400 at the pharmacy. For, this price results precisely in the maximum net price of $ 100 that insured consumers are willing to pay. As shown in figure 4, the effective demand function is now given by D25, causing the equilibrium to shift to E25. The volume of medical services increases, as does the fee level. If there is no copayment, the quantity demanded even attains M0 (see D0), causing the equilibrium on the market to be shifted as far out as E0.
The effect of moral hazard is usually equated with the expansion of utilization of the insured service [10]. However, this applies only to goods and services that are supplied with an infinite price elasticity (causing the supply function S to run horizontal). When it comes to healthcare services however, quite likely the price elasticity of supply is less than infinity. In that case, the supply function S has a positive slope (Figure 4), implying that moral hazard also affects price. This causes healthcare expenditure to be boosted even more strongly, as both price and quantity increase due to health insurance coverage. From the point of view of a health insurer, there is the additional consideration that the effects of moral hazard shown apply to each item on the benefit list. Neglecting substitution effects, there is therefore a tendency for moral hazard effects to accumulate. Finally, they increase over time since service providers have a strong interest in adjusting existing therapies in a way as to meet with increased willingness to pay on the part of patients. In addition, entirely new therapies are launched again and again, calling for an expansion of the benefit list and adding on to the cumulative effect of moral hazard.
A health insurer who is aware of these effects will write contracts with copayment only. However, legislation may prevent the introduction of cost sharing or its increase. Then, rationing may constitute a viable alternative, and since moral hazard effects increase over time, so will the demand for it.
Conclusion 3: The very existence of health insurance results in both increased quantities and prices of services transacted in the healthcare sector and hence increased healthcare expenditure. In principle, insurers have the means to limit the effects of moral hazard; however, if prevented from using them, they join the government to exert a demand for rationing that increases over time.
3.3 The suppliers of rationing
In order to complete the description of the market for the regulatory service called 'rationing of health care'; this section is devoted to a more detailed analysis of the three possible suppliers of rationing of healthcare services. The supply function shown in figure 3 reflects the assumption that rationing is provided by the least-cost supplier. This assumption need not to be true, but depends on the nature of the political process. Only if the task of regulation is not assigned to a particular authority to begin with but the result of a certain amount of competition for this task is cost effectiveness of regulation assured.
Table 1 below lists the strengths and weaknesses of the three suppliers to be considered here. First, public administration is the only authority that is capable of enforcing a limit on public healthcare expenditure and thus implementing the budget relief sought by politicians. However, their rationing activity can result in e.g. a hospital running out of money towards the end of the fiscal year. This would create the risk of demand for medical care spilling over to other sources of supply, e.g. nursing homes. For avoiding this risk, regulation must cover also these alternative sources; yet detailed allocations block the substitution of healthcare services that is necessary to assure efficiency in their provision.
![]()
Table 1: Comparative performance of suppliers of rationing.
View Table 1
The second group of potential suppliers of rationing are the health insurers themselves, acting in collusion, i.e. as a cartel. Without such collusion, each insurer would individually test the market to find out whether market share can be gained by expanding the list of benefits in return for higher premiums. However, even given cartellistic collusion, health insurers have difficulty implementing rationing. They would have to have the right to vertically integrate the production of healthcare services, becoming the proprietors of medical practices, pharmacies, and hospitals. Moreover, rationing imposed on private providers may induce the shifting of cost to public ones, thus obviating the budgetary relief that is important to politicians.
A third group of potential suppliers of rationing are the healthcare providers. Physicians in particular are capable of implementing the detailed norms prescribed by public administration while redistributing healthcare services between different patient groups according to political criteria benefiting of the protection of the professional secret [11]. However, rationing entails a loss of income that needs to be compensated by honoring providers for the non-provision of services by lavishing income and power on them, especially on the representatives of their professional associations.
4. Alternatives to Rationing and the Possible Contribution of Health Insurers
In view of the efficiency losses due to rationing, in this section the objective of avoiding it in the healthcare sector is posited as an objective. From figure 2, one can see that the discrepancy between M'' and M', given the budget amount , can be overcome in two ways. The first is an increase in supply (indicated by a shift of the supply function S away from the origin). However, this typically requires an expansion of capacity in medical education, which would in most countries constitute a charge on the public budget in favor of health. Moreover, in an insured market such as health care, the demand function would likely also shift away from the origin because it is almost exclusively the cost of travel, waiting, and other inconveniencies that prevent people from utilizing healthcare services. These costs go down when the density of supply increases.
The other possibility to avoid rationing (or at least mitigate its effect) would be to shift the demand function of figure 2 towards the origin. This amounts to a self-limitation of individuals. Indeed, this is what consumers do in their daily lives; after all, few of them drive luxury cars. However, once a person is ill, the contribution of medical care to re-establishing health often becomes of such crucial importance that self-limitation is very difficult to achieve. A binding commitment before the event of illness may be feasible, however. Such a commitment can be brought about by the choice of a particular health insurance policy, to be developed by health insurers. However, the limitations to be accepted need always to be compensated in the guise of a reduced premium. The amount of compensation depends on individual properties of consumers and must be discovered in the competitive process. For example, recent evidence from Switzerland suggests that the French-speaking minority requires compensations to voluntarily accept restrictions of the Managed-Care type that are at least twice and up to five times as much as the amounts required by the German-speaking majority [12]. For this reason, it is crucial that health insurers act not in collusion but use product differentiation for competitive purposes.
A first variant is to directly limit moral hazard on the part of consumers. This calls for a fixed and proportional copayment. It may also be appropriate to single out services that are subject to monopolistic price fixing and to have patients pay out of pocket beyond a certain price. This means that above that threshold price, service providers are confronted with the true demand function D of figure 4. Consumers may also opt for managing their cost sharing over time. This can be achieved using bonus options honoring no claims (or also claims below a certain limit) by a reduction in premiums [11]. Especially consumers of higher age may also agree to avoid heroic efforts in favor of unlikely survival by accepting their contract not to cover the most recent (and hence usually most expensive) medical technology anymore. This constitutes an alternative to widely debated age-based rationing. The reduction in contribution required to compensate for these limitations could be financed by the achievable cost savings, at least in the case of Switzerland [12].
Moral hazard may also be controlled indirectly through the selection of healthcare providers. The requisite for this is freedom of contracting. The contract can e.g. provide for a gate-keeping model, requiring that consumers accept a family physician who decides about referral to specialists and hospitals. The savings achieved must be shared with participating physicians in order to motivate them for accepting such rules, but also to consumers in the guise of a reduced contribution. Another possibility is creating physician and hospital lists that comprise only those providers featuring a favorable benefit-cost ratio. In some cases, this may entail the non-provision of medical care. However, the crucial difference from rationing is that consumers knowingly accept such limitations and are compensated by lower premiums.
Finally, health insurers may negotiate payment systems with providers. Some payment systems contain incentives for a less intensive treatment style (e.g. prospective capitation). However, the reduction in premium may not be sufficient for many consumers to compensate them for the downside that healthcare providers will now act under the influence of changed incentives. Conversely, some providers may be unwilling to accept new forms of payment that shifts risk to them. In sum, some consumers may continue to prefer fee-for-service payment for at least certain types of illness, while some healthcare providers may prefer to agree on fee-for-service payment with at least one or several health insurers.
Provided the contractual alternatives prepared by health insurers are successful, the demand function of figure 2 indeed moves towards the origin, causing the discrepancy between the quantities of healthcare services demanded (M") and supplied (M') to decrease. Therefore, at a given price or fee level, there also will be less of a demand for rationing. The implications for the market for rationing can be seen in figure 3. There, the demand function shifts from the D0 to D1. Unless public administration adopts less costly alternatives of rationing in response, the supply function S remains unchanged. Therefore, a transition from equilibrium E0 to E1 is predicted that also causes the intensity of rationing to drop from R0 to R1. In this way, the efficiency losses that exist on the market for medical services and health insurance can be mitigated. Specifically, since the gap between budget and healthcare expenditure caused by consumers decreases, politicians are not willing anymore to pay as much for the service 'rationing of health care', whose price therefore goes down (e.g. in the guise of compensations paid to service providers for the non-provision of services). Total expenditure being given by the product of price time's quantity, expenditure on regulatory services also is reduced. The fact that the incentive for suppliers of the service 'rationing' is weakened can be read off from the reduction of producer surplus, from GP0E0 to GP1E1.
Conclusion 4: Health insurers have at their disposal several possibilities of combating moral hazard through the structuring of their contracts, thus contributing to a reduction in the demand for rationing in the healthcare sector.
5. Summary and Conclusions
This contribution takes as its point of departure to show that the imposition of a limit on healthcare expenditure (which is the consequence of a corresponding limit on the public budget) induces rationing of healthcare services. This causes efficiency losses that have been emphasized by economic theory for a long time (Conclusion 1). However, rationing also impacts on the demand for health insurance. Concerning health insurance with in-kind benefits, the prediction is a reduction in demand, causing additional efficiency losses. In the case of reimbursement health insurance, however, an increase in demand may result. While ambiguous at first sight, the total effect on the market for health insurance is likely to be negative (Conclusion 2). In a second step, the intensity of rationing is determined. Viewing rationing as a particular kind of regulation, there is a market for such a service, with politicians and health insurers constituting the demand side and public administration, service providers, and health insurers themselves being potential suppliers. There is a certain tragedy to health insurance that its very existence induces moral hazard effects that in their turn boost the demand for rationing in the healthcare sector. In addition, this demand is likely to increase over time due to innovation in medical technology (Conclusion 3). If in view of these efficiency losses, one adopts the avoidance of rationing as an objective, the alternative is to give consumers the opportunity to commit to limitations before the advent of illness. Designing and launching the appropriate contractual variants constitutes an important task of health insurers (Conclusion 4). However, especially social health insurers at present need to make particular effort to attain the necessary freedom from regulatory constraint to proceed in this direction.
References
-
Klein R, Day P, Redmayne S (1995) Rationing in the NHS: the dance of the seven veils-in reverse. Br Med Bull 51: 769-780.
-
Maynard A, Bloor J (1998) Our Certain Fate: Rationing in Health Care. Office of Health Economics, London.
-
Peltzman S (1976) Towards a more general theory of regulation. Journal of Law and Economics 19: 211-240.
-
Carlton DW, Perloff JM (2000) Modern Industrial Organization, Reading MA.
-
Kreier R, Zweifel P (2010) Health insurance in Switzerland: a closer look at a system often offered as a model for the United States. Hofstra Law Review 39: 89-110.
-
Van Dalen HP, Swank OA (1996) Government spending cycles: ideological or opportunistic? Public Choice 89: 183-200.
-
Tobin J (1952) Survey of the theory of rationing. Econometrica 20: 521-533.
-
Zweifel P, Grandchamp Ch (2002) Measuring the effect of cartelization in medicine: an international study. In: Slottje DJ. Measuring Market Power, Amsterdam: 47-66.
-
Arrow KJ (1970) Aspects of the theory of risk-bearing. In: Yrj� Johnsson, Helsinki. Essays in the Theory of Risk-bearing.
-
Zweifel P, Manning WG (2000) Moral hazard and consumer incentives in health care. In: Culyer AJ, Newhouse JP. Handbook of Health Economics, Boston, North Holland: 409-459.
-
Zweifel P, Eichenberger RE (1992) The political economy of corporatism in medicine: Self-regulation or cartel management? J Regul Econ 4: 89-108.
-
Zweifel P, Telser H, Vaterlaus S (2006) Consumer resistance against regulation: the case of health care. J Regul Econ 29: 319-332.