Journal of Family Medicine and Disease Prevention
Family Oriented Care: Opportunities for Health Promotion and Disease Prevention
Diego Garcia-Huidobro1,2* and Tai Mendenhall2
1Department of Family Medicine, School of Medicine, Pontificia Universidad Catolica de Chile
2Department of Family Social Science, University of Minnesota, USA
*Corresponding author: Diego Garcia-Huidobro, Departamento de Medicina Familiar, Vicuña Mackenna 4686, Macul, Santiago, Chile; Tel: 56223548535, E-mail: dgarciah@med.puc.cl
J Fam Med Dis Prev, JFMDP-1-009, (Volume 1, Issue 2), Review Article; ISSN: 2469-5793
Received: July 16, 2015 | Accepted: August 28, 2015 | Published: August 31, 2015
Citation: Garcia-Huidobro D, Mendenhall T (2015) Family Oriented Care: Opportunities for Health Promotion and Disease Prevention. J Fam Med Dis Prev 1:009. 10.23937/2469-5793/1510009
Copyright: © 2015 Garcia-Huidobro D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Even though life expectancy has increased in industrialized countries, chronic diseases and mental illnesses are continuous health challenges. Thus, new strategies to further improve health must be implemented. Because family contexts are where health behaviors are usually learned, developed, maintained and changed, targeting family systems (rather than individual patients) is an option to further improving the health status of individuals, families, and communities. This article will review possibilities for including family members in health services and provide suggestions for clinicians, clinic managers, researchers and policy makers for the implementation of this clinical approach.
Introduction
Today is the era of prevention. The epidemics of chronic and non-communicable diseases - including depression, diabetes, cardiovascular disease and cancers - all of which lead to higher rates of morbidity and mortality, are expected to increase their burdens during the next 20 years [1,2]. Worldwide cardiovascular diseases, including ischemic heart disease and cerebrovascular disease, are the leading cause of death, accounting for nearly 30% of total mortality [1,3]. High blood pressure, elevated glycaemia, high blood cholesterol levels, tobacco use, physical inactivity, overweight, obesity, and low fruit intake are responsible for 27.8% of world's deaths [1,3], about 60% of cardiovascular and 35% of cancer related deaths, and for 10.7% of world's disability adjusted life years (DALYs) [4].
Annually, almost 7 out of 10 deaths among Americans are caused by chronic diseases, where cardiovascular, cancer and chronic respiratory diseases are the leading causes of death [5]. More than 75% of health care spending is concentrated on people with chronic conditions [6].
Even though a sustained reduction of heart disease and stroke death rates in the last decades has been achieved [7], the increasing prevalence of risk factors and poor control of those conditions threaten the maintenance of the achieved outcomes.
From 1976 to 2008, the prevalence of obesity increased from 15% to 34% among adults and has more than tripled in children and adolescents from 5% to 17% [8]. Likewise, diabetes, the leading cause of kidney failure, blindness, and non-traumatic lower- limb amputations among adults in the Unites States (U.S.), was estimated to affect 25.8 million people (8.3% of the population in 2010) [9]. This represents an increase in previous years' rates, particularly among minorities and groups with low educational levels [10]. Also, while hypertension has maintained its prevalence and patients have achieved higher control rates, about half of the diagnosed patients do not have their blood pressure under control [11]. Cigarette smoking, the leading cause of preventable morbidity and mortality in the U.S., has declined in youth and adults. However during the past 5 years this decline has stalled among adults, particularly in low socioeconomic groups [12]. Even though these findings are from the U.S., they are not rare for other countries [1,3,4,13].
Despite the fact that life expectancy has increased in most countries [1], further health improvement could be achieved [13]. The World Health Organization has estimated that if the major risk factors for chronic disease were eliminated, at least 80% of all heart disease, stroke, and more than 40% of all cancer cases would be prevented [13]; now is therefore the time for prevention. Research has repeatedly demonstrated the contributions to health of factors beyond the physical environment, medical care, and health behaviors. These include socioeconomic level, ethnic origin, participation and support in social networks, work conditions, and social capital, among others [1,2,3,13-15]. Even though the influence of these factors on health outcomes is widely recognized, they are rarely considered in clinical preventive care.
Most preventive interventions are directed towards particular diseases, overlooking the possible impact on health conditions that share similar pathophysiological pathways. Behavioral and preventive services and research are currently directed towards individuals and have assessed outcomes primarily among sick persons, ignoring the effects of clinical interventions on other people that might also benefit. Because of this, broader interventions, focusing on families instead of individuals could be particularly useful in health promotion and disease prevention.
In this article, the benefits of adopting a systemic/family orientation in clinical preventive care will be discussed, and suggestions for clinicians, clinic managers, researchers, and decision makers about how to implement this practice will be provided. Because primary care is where most patients receive services, and health providers care for multiple family members, are responsible for screening for health problems, and treat most of the risk factors for highly prevalent and burdensome diseases, we consider that this approach could be particularly beneficial in this setting, and will center the discussion on this level of care.
Benefits of Family-Oriented Clinical Prevention
Several reasons support the adoption of family-oriented care in clinical prevention (Table 1). However, the use of this approach is in its early stages, and further research is required to make strong conclusions, and to expand its implementation.
![]()
Table 1: Arguments to develop a family oriented preventive care
View Table 1
Beneficial Effect of Positive Family Factors on Health Outcomes
Multiple family characteristics have been related to good and poor health outcomes. Family closeness, caregiver coping skills, mutually supportive relationships, clear family organization, flexibility and adaptability, and direct communication about the illness and its management have been linked to better clinical outcomes and have been identified as family protective factors [15]. Correspondingly, negative family characteristics, such as intra- family conflict, criticism, blaming, lack of an extra- family support system, rigidity, and patient and family member's pre- illness psychopathology are associated with poorer clinical outcomes and therefore, are identified as family risk factors. Interestingly, all these characteristics of families are related to health outcomes across different disorders, and also within different family developmental stages [16], grounding bases for common interventions to multiple diseases, affecting several family members.
Families with members with chronic diseases are at increased risk of problematic functioning compared to families with healthy members [17,18]. However, positive family dynamics have been related to improved outcomes in multiple health conditions across the human lifespan. In children evidence supports this association for: type 1 diabetes [19], asthma [20], obesity [21], delayed child development [22], attention deficit and hyperactivity disorder (ADHD) [23], behavioral and sphincter control disorders [24], and cystic fibrosis [20,25]. In adults, this relationship has been established for hypertension [26], diabetes [27], mood and anxiety disorders [28,29], tobacco, alcohol and illicit substances use [1-33], dementia [34], and physical functioning decline among elders [35]. Individuals with these disorders are commonly served by primary care, thus this type of approach could be particularly useful in that clinical setting.
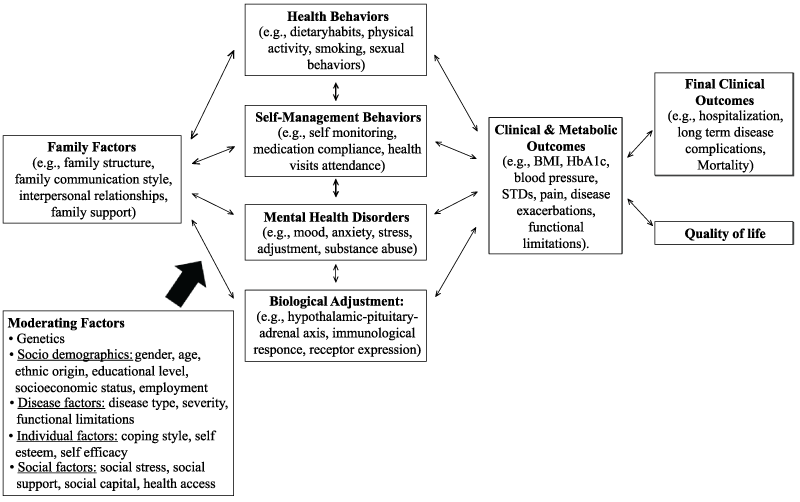
Figure 1 explains the potential pathophysiological processes that relate family factors and health outcomes. These include mutually dependent pathways: health and self- management behaviors, mental health disorders, and biological adjustment.
.
Figure 1: Pathways through which family factors can affect clinical outcomes
BMI: Body Mass Index; HbA1c: Hemoglobin A1c; STDs: Sexually Transmitted Diseases
View Figure 1
People living in families with a positive functioning style develop healthier lifestyles and self- management behaviors [18]. By modeling and supporting their members in the achievement of positive outcomes, these behaviors are taught and maintained among the family group.
Through observation and interaction, individuals learn and sustain behaviors practiced by their relatives, mutually influencing healthy and unhealthy behavior development. Also, by using multiple types of social support (emotional, instrumental, informational, and appraisal), the family promotes and reinforces positive health among their members [15]. Thus, families with better relational styles among their members attain healthier behaviors, and families with negative relational styles reach poorer health outcomes.
Second, mental health disorders are intimately related to the development of physical illnesses, and are correlated among family members [36]. These disorders and family functioning style are mutually reinforcing. Members of families with poor functioning develop mental health diseases more frequently [18,28,29], but also, families with members suffering mental health illness suffer a decline in functioning [32].
Finally, individuals in stressed families face the activation of the neuroendocrine system (hypothalamic-pituitary-adrenal axis), modifying their metabolic and immunological response [37]. Higher levels of cortisol and sympathetic nervous system activation could explain the elevated rates of mental, respiratory, cardiovascular and nutritional disorders found in families with worse functioning styles [38-40].
Clustering Diseases and Health Behaviors in Families
Heath and associated illnesses are developed, maintained and changed within the family. Even though genetics influences the risk of certain illnesses [41], family members tend to share the same lifestyle behaviors, including similar diets, amount of physical activity, and use of substances (tobacco, alcohol, illicit drugs) [42,43]. Parents' lifestyle influences what kind of behaviors their children will develop. For example, children of families where none of the parents smoke are less likely to initiate tobacco use than when one or both of them does so [44]. Similarly, children tend to share similar eating behaviors to their parents, and if their relatives are overweight or obese, they are at increased risk of those disorders [21,45]. Finally, simultaneous changes occur in family members for a number of health habits, such as smoking, drinking, involvement in physical activity, initiating screening, and getting flu shots [46]. Thus, once a person initiates a behavioral change, it is likely that their relatives will follow, affecting multiple family members with a single intervention.
Pleiotropic Effect of Family Inte rventions
Because of the mutual interconnectedness of family members and their health outcomes, family oriented interventions are likely to have large effects on health outcomes. These interventions affect multiple members at the same time. For example, when mothers with major depression receive treatment, their children are more likely to decrease their experience of psychiatric symptoms according to maternal symptom improvement [47]. Also, when parents receive lifestyle advice, besides improving their own health outcomes, their children reduce their own levels of fasting glycaemia, lipids, and blood pressure, as we ll [48], similarly when partners receive screening and health counseling [49].
Also, these interventions have the potential to affect multiple disorders concomitantly. For example, parenting skill development programs have systematically reported benefits in the areas of youth smoking, illicit substance use, unsafe sexual behaviors, obesity, and mental health outcomes [47,50-52]. Family interventions in the case of patients with diabetes, besides improving metabolic control, also have reported participant improvement in mental health scores [53,54]. Moreover, because some disorders share similar pathophysiological pathways, these interventions are likely to also have various effects on the different stages of diseases (risk factor, asymptomatic or symptomatic illness and rehabilitation), increasing the effectiveness of this clinical approach.
Effectiveness of Family Interventions
During the last decade, multiple reviews and meta-analyses have been published assessing the effectiveness of family-oriented interventions in prevention and treatment of physical diseases [15,42,55-59]. All of them concur on the superiority of this approach compared to usual care, for disorders in children, adults and elders, in physical health, mental health, and health of family members.
Interventions directed towards improving family relations while living with the demands of the chronic disease appear to achieve better results than pyschoeducational interventions directed to improve knowledge and skills in the management of the particular illness [42,57,58]. Also, these types of interventions have minimal secondary effects. However research in family interventions is scarce and is frequently centered on specific health conditions (e.g., asthma, obesity, dementia, arthritis, cancer, or coronary heart disease), and focused on treatment rather than prevention [15,42,55-59]. Few studies analyze the effect of family interventions in the most prevalent adult diseases: overweight/obesity, hypertension, diabetes, asthma/chronic obstructive pulmonary disease (COPD), cardiovascular risk, and unhealthy behaviors, which are significant health challenges. Also, there is a lack of research including minorities, and underserved populations, building opportunities for future studies.
Other Benefits of Family Interventions
Research has shown positive effects of family interventions in short-term, and up to 12- 24 month follow-up periods [15,42,55-59]. Moreover, because these approaches are directed at modifying the health behaviors of family members longer term benefits, even transgenerational effects, could be expected for these type of interventions, especially if they are oriented towards the relational dynamics of the family; however this needs to be tested.
Beside all the potential benefits discussed above, this type of approach has the potential to be easily implemented. Family oriented interventions do not require the use of advanced technology, but necessitate a change in how health is conceived. The potential cost-effectiveness of this method promises high population impact, however this still needs to be measured. In addition, because the family is valued worldwide [60], a family-oriented approach could be implemented cross culturally, providing important population benefits across gender, race and national divides, where today's health challenges are particularly relevant.
Future Directions
Implementing a family approach in health promotion and disease prevention requires a shift from the biomedical to a biopsychosocial approach to health [61,62]. Health care professionals, healthcare managers, researchers, and policy makers must consider the context where health risk behaviors develop, maintain and change, and examine the interconnectedness among the physiological, psychological and social influences upon these behaviors. This broader approach starts with the recognition that individuals are members of families, and that families have major influence on health-related behaviors.
Implications for Clinical Practice
Improving family relations has important health implications, equivalent to reduction of risk factors for chronic disease by promoting exercise or diet [61-65]. Thus, offering early family interventions is clinical prevention, not just crisis management.
Family interventions are often overlooked because clinicians may not be familiar with the family research literature. Additionally, the health care system is generally structured for individuals, not for families. Working to strengthen family resilience and favoring positive family coping mechanisms, however, offers new avenues for preventive health care.
In general practice, clinicians need to be open to assess the context in which people find themselves, and be willing to incorporate this evaluation in diagnostic and treatment plans. Also, providers can conduct family assessments of patients with chronic disease and mental illnesses to detect problematic areas of family functioning which could therefore be improved. Patients and their families can be educated about how family factors are related in the treatment of the chronic disease or mental illness that one of them faces. Providers can involve family members in the care of patients, and give recommendations regarding what constitutes healthy family functioning, and how to improve their relational competence. If serious family problems are detected, according to their personal skills clinicians can provide services to solve these issues or refer the patient and their relatives to family therapists. These professionals are increasingly becoming part of the medical team in primary care, bridging the gap between the health professionals and the family's needs, providing what has bee n named Medical Family Therapy [66].
Using the contextual approach of the biopsychosocial model [67], helps the clinician appreciate the difficulties of changing lifestyles, and the patience required in helping people. Personal and familial habits are established over many years, and are unlikely to change overnight. This can be difficult to understand for health providers trained in hospitals where changes occur in minutes or hours. Instead, this approach requires valuing the importance of advancing one step at a time, accepting failure, and being willing to start all over the behavioral change process.
Also, the biopsychosocial model [67], requires that the health provider consider him/herself as a supporter in the change that the patient and the family need to perform, favoring a provider-patient/family relationship more cooperative and participatory, and less paternalistic and authoritative [66]. As well, clinicians are members of a multi professional healthcare team oriented to providing comprehensive care to patients and families. Each member contributes in a different way on fostering wellbeing within families, and working collaboratively will achieve better health results in clients. The goal is to collectively assist the patient and their family to make the lifestyle changes they need, want and agree to make, and by doing that help all their members achieve better health behaviors.
A different clinical approach involves operational and financial requirements to maintain sustainability [68]. From an operational perspective, interdisciplinary health teams will need to develop strategies to work together, new infrastructure will need to be considered and family- including clinical records systems will need to be developed to organize a real family oriented care. From a financial perspective, indicators, payment and incentive systems that incorporate the family approach will need to be developed to sustain this practice, and the required changes that need to be made.
Implications for Research
There is a tremendous need for clinicians and researchers to develop research on families and health, particularly designing and evaluating clinical trials. Family protective and risk factors have been identified, but theoretical frameworks that guide research in this area are missing.
Theories on how families affect health outcomes need to be developed to direct future studies. These frameworks should report the concepts and measurements needed to be evaluated in prospective clinical trials, and determine the types of interventions and specific populations for whom the interventions are most effective. However, these models should be flexible enough to incorporate the particular needs of the individual families receiving the interventions, and to adapt according to particular family characteristics.
High quality randomized controlled trials need to be conducted to assess the effectiveness of family interventions. Because of the high burden of disease of health behaviors, family- oriented research directed towards these outcomes is particularly interesting. Other areas of interest where family-centered trials need to be conducted are the prevention and control of chronic disease during adulthood: overweight/obesity, hypertension, diabetes, asthma/COPD, where research is limited. However, as discussed in the previous sections, clinical trials should also be aimed at targeting several risk factors and diseases, especially if they share pathophysiological commonalities.
By measuring short-, medium-, and long-term outcomes in several dimensions, such as metabolic control, emotional distress, quality of life, and in multiple family members, a better understanding of the opportunities for health improvement with this type of approach will be provided. Cost-effectiveness evaluations of these interventions should also be conducted to determine the financial benefits of this health care model.
Family-oriented research should include diverse types of families. Little is known about the health effects of diverse family configurations, and if these are similar cross culturally. To generalize the benefits of this approach, real world effectiveness-research needs to be conducted considering a wide array of populations and family arrangements. Including minorities and underserved populations in research trials could be an effective strategy to respond to the burden of disease in these groups.
To address all these research requirements, an interdisciplinary approach is fundamental.
Future research on families and health should consider establishing partnerships among health providers, health researchers, healthcare managers, social scientists, and public health experts. Transdisciplinary research teams will study the family and health issues from diverse perspectives, developing comprehensive interventions tested in methodologically sound trials. This strategy will produce strong research reports, highly applicable to the current healthcare environment, including on the clinical, operational and economical sustainability of the interventions.
Implications for Policy
At this moment research is inconclusive on the benefits of family-oriented care. However, family-oriented health promotion and disease prevention are promising strategies to improve the health status of populations, and policy makers should be aware of these emerging findings.
With today's knowledge regarding the relationship of family and health outcomes, the assessment of familial protective and risk factors should be included in the clinical guidelines of multiple disorders. However, the involvement of family members in treatment, and the development of family psychoeducational activities or relational improvement programs should be considered.
Policy makers should also be aware of the requirements for the successful implementation of the family-centered biopsychosocial model [67], in case that cost-effectiveness is proved.
Healthcare systems are usually designed for individual care and switching to a broader and more comprehensive care delivery system has barriers that will need to be addressed. These barriers include clinical, operational, financial, educational, ethical, and legal challenges that have been ignored by the current biomedical approach. Policy makers should initiate discussions on the role of the family on the decision making processes and the implications that this can have in the healthcare system.
Limitations of a Family Approach in Health Promotion and Disease Prevention
Several factors limit the implementation of this approach at this moment. As stated previously, to date there has not been robust evidence to support the implementation of this approach in preventive care. Further research trials will contribute more and higher-quality evidence to address this issue.
Also, the eventual economic benefits need to be tested. Some concerns exist if the implementation of this approach requires longer clinical visits [53], or if the complexity of these interventions could produce more costs than savings [69]. Again, at this moment, there is insufficient research addressing these issues and future trials should incorporate these components into assessment.
Finally, because this approach requires different clinical skills, current providers might not provide care using this approach. Training curricula of healthcare professionals needs to incorporate family interviewing and assessment skills, and if demonstrated effective, ways to deliver basic family interventions. Preparing future clinicians in family-oriented health collaboration should also contribute to providing and delivering a more comprehensive and integrated care in our medical system.
Conclusions
Health promotion and disease prevention is fundamental nowadays, where disease burden is mostly derived from current life styles. Thus, new alternatives to overcome the current health problems need to be developed, implemented and assessed. Because the family is the place where health behaviors are developed, maintained and changed, incorporating this approach in clinical preventive care could dramatically improve the people's health.
In this article, we have reviewed the benefits of having a family oriented clinical approach, providing suggestions for clinicians, managers, researchers, and policy makers on the challenges to come. Because research on how family interventions improve health is limited, strong conclusions about the benefit of this clinical model cannot be made. However, enhancing family relationships and developing family-strengthening activities appears to be effective on several physical and mental health outcomes, in multiple diseases, across the human lifespan. Future trials are required to verify these findings, and guide the implementation of this promising clinical approach.
References
-
World Health Organization (2008) The global burden of disease 2004: an update. 1-146.
-
Mathers CD, Loncar D (2006) Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med 3: e442.
-
Mathers CD, Boerma T, Ma Fat D (2009) Global and regional causes of death. Br Med Bull 92: 7-32.
-
World Health Organization (2009) Global Health Risks: Mortality and burden of disease attributed to selected major risks. Switzerland: WHO Press.
-
Kochanek K, Xu J, Murphy S, Miniño A, Kung H (2011) Deaths: preliminary data for 2009. Hyattsville, MD: National Center for Health Statistics.
-
Anderson G (2004) Chronic conditions: making the case for ongoing care. Baltimore, MD: John Hopkins University.
-
Remington PL, Brownson RC; Centers for Disease Control and Prevention (CDC) (2011) Fifty years of progress in chronic disease epidemiology and control. MMWR Surveill Summ 60 Suppl 4: 70-77.
-
Freedman DS; Centers for Disease Control and Prevention (CDC) (2011) Obesity - United States, 1988-2008. MMWR Surveill Summ 60 Suppl: 73-77.
-
Centers for Disease Control and Prevention. National diabetes fact sheet: national estimates and general information on diabetes and prediabetes in the United States, 2011. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention.
-
Beckles GL, Zhu J, Moonesinghe R; Centers for Disease Control and Prevention (CDC) (2011) Diabetes - United States, 2004 and 2008. MMWR Surveill Summ 60 Suppl: 90-93.
-
Keenan NL, Rosendorf KA; Centers for Disease Control and Prevention (CDC) (2011) Prevalence of hypertension and controlled hypertension - United States, 2005-2008. MMWR Surveill Summ 60 Suppl: 94-97.
-
Garrett BE, Dube SR, Trosclair A, Caraballo RS, Pechacek TF; Centers for Disease Control and Prevention (CDC) (2011) Cigarette smoking - United States, 1965-2008. MMWR Surveill Summ 60 Suppl: 109-113.
-
World Health Organization (2005) Preventing chronic diseases: a vital investment. Switzerland: WHO Press.
-
Woolf S, Johnson R, Phillips RJ, Philipsen M (2007) Giving everyone the health of the educated: an examination of whether social change would save more lives than medical advances. Am J Public Health 97: 679-683.
-
Weihs K, Fisher L, Baird M (2002) Families, health, and behavior: A section of the commissioned report by the Committee on Health and Behavior: Research, Practice, and Policy Division of Neuroscience and Behavioral Health and Division of Health Promotion and Disease Prevention Institute of Medicine, National Academy of Sciences. Fam Syst Health 20: 7-46.
-
Fisher L (2006) Research on the family and chronic disease among adults: Major trends and directions. Fam Syst Health 24: 373-380.
-
McClellan CB, Cohen LL (2007) Family functioning in children with chronic illness compared with healthy controls: a critical review. J Pediatr 150: 221-223, 223.
-
García-Huidobro D, Puschel K, Soto G (2012) Family functioning style and health: opportunities for health prevention in primary care. Br J Gen Pract 62: e198-203.
-
Pereira MG, Berg-Cross L, Almeida P, Machado JC (2008) Impact of family environment and support on adherence, metabolic control, and quality of life in adolescents with diabetes. Int J Behav Med 15: 187-193.
-
Fiese B, Everhart R (2006) Medical adherence and childhood chronic illness: family daily management skills and emotional climate as emerging contributors. Curr Opin Pediatr 18: 551-557.
-
Sleddens EF, Gerards SM, Thijs C, de Vries NK, Kremers SP (2011) General parenting, childhood overweight and obesity-inducing behaviors: a review. Int J Pediatr Obes 6: e12-27.
-
Cerezo MA, Pons-Salvador G, Trenado RM (2008) Mother-infant interaction and children's socio-emotional development with high- and low-risk mothers. Infant Behav Dev 31: 578-589.
-
Deault LC (2010) A systematic review of parenting in relation to the development of comorbidities and functional impairments in children with attention-deficit/hyperactivity disorder (ADHD). Child Psychiatry Hum Dev 41: 168-192.
-
Petitclerc A, Tremblay RE (2009) Childhood disruptive behaviour disorders: review of their origin, development, and prevention. Can J Psychiatry 54: 222-231.
-
Bloomberg GR, Banister C, Sterkel R, Epstein J, Bruns J, et al. (2009) Socioeconomic, family, and pediatric practice factors that affect level of asthma control. Pediatrics 123: 829-835.
-
Morisky DE, Levine DM, Green LW, Shapiro S, Russell RP, et al. (1983) Five-year blood pressure control and mortality following health education for hypertensive patients. Am J Public Health 73: 153-162.
-
Armour TA, Norris SL, Jack L Jr, Zhang X, Fisher L (2005) The effectiveness of family interventions in people with diabetes mellitus: a systematic review. Diabet Med 22: 1295-1305.
-
Weich S, Patterson J, Shaw R, Stewart-Brown S (2009) Family relationships in childhood and common psychiatric disorders in later life: systematic review of prospective studies. Br J Psychiatry 194: 392-398.
-
Marshall AJ, Harper-Jaques S (2008) Depression and family relationships: ideas for healing. J Fam Nurs 14: 56-73.
-
Thomas J, Patten C, Mahnken J, O fford K, Hou Q, et al. (2009) Validation of the support provided measure among spouses of smokers receiving a clinical smoking cessation intervention. Psychol Health Med 14: 443-453.
-
Shoham V, Rohrbaugh MJ, Trost SE, Muramoto M (2006) A family consultation intervention for health-compromised smokers. J Subst Abuse Treat 31: 395-402.
-
Leonard KE, Eiden RD (2007) Marital and family processes in the context of alcohol use and alcohol disorders. Annu Rev Clin Psychol 3: 285-310.
-
Velleman R1, Templeton LJ, Copello AG (2005) The role of the family in preventing and intervening with substance use and misuse: a comprehensive review of family interventions, with a focus on young people. Drug Alcohol Rev 24: 93-109.
-
Quinn C, Clare L, Woods B (2009) The impact of the quality of relationship on the experiences and wellbeing of caregivers of people with dementia: a systematic review. Aging Ment Health 13: 143-154.
-
Bisschop M, Kriegsman D, van Tilburg T, Penninx B, van Eijk J, et al. (2003) The influence of differing social ties on decline in physical functioning among older people with and without chronic diseases: the Longitudinal Aging Study Amsterdam. Aging Clin Exp Res 15: 164-173.
-
Fletcher J (2009) All in the Family: Mental Health Spillover Effects between Working Spouses. B E J Econom Anal Policy 9: 1.
-
Robles TF, Kiecolt-Glaser JK (2003) The physiology of marriage: pathways to health. Physiol Behav 79: 409-416.
-
Wright RJ (2011) Epidemiology of stress and asthma: from constricting communities and fragile families to epigenetics. Immunol Allergy Clin North Am 31: 19-39.
-
Golden SH (2007) A review of the evidence for a neuroendocrine link between stress, depression and diabetes mellitus. Curr Diabetes Rev 3: 252-259.
-
Gregor MF, Hotamisligil GS (2011) Inflammatory mechanisms in obesity. Annu Rev Immunol 29: 415-445.
-
Samek D, Rueter M, Koh B (2013) Overview of Behavioral Genetics Research for Family Researchers. J Fam Theory Rev 5: 214-233.
-
Campbell TL (2003) The effectiveness of family interventions for physical disorders. J Marital Fam Ther 29: 263-281.
-
Pachucki MA, Jacques PF, Christakis NA (2011) Social network concordance in food choice among spouses, friends, and siblings. Am J Public Health 101: 2170-2177.
-
Scragg R, Reeder AI, Wong G, Glover M, Nosa V (2008) Attachment to parents, parental tobacco smoking and smoking among Year 10 students in the 2005 New Zealand national survey. Aust N Z J Public Health 32: 348-353.
-
Greenberg RS, Ariza AJ, Binns HJ (2010) Activity and dietary habits of mothers and children: close ties. Clin Pediatr (Phila) 49: 1026-1032.
-
Falba TA, Sindelar JL (2008) Spousal concordance in health behavior change. Health Serv Res 43: 96-116.
-
Pilowsky DJ, Wickramaratne P, Talati A, Tang M, Hughes CW, et al. (2008) Children of depressed mothers 1 year after the initiation of maternal treatment: findings from the STAR*D-Child Study. Am J Psychiatry 165: 1136-1147.
-
Schwandt P, Bertsch T, Haas GM (2011) Sustained lifestyle advice and cardiovascular risk factors in 687 biological child-parent pairs: the PEP Family Heart Study. Atherosclerosis 219: 937-945.
-
Pyke SD, Wood DA, Kinmonth AL, Thompson SG (1997) Change in coronary risk and coronary risk factor levels in couples following lifestyle intervention. The British Family Heart Study. Arch Fam Med 6: 354-360.
-
Stanton B, Cole M, Galbraith J, Li X, Pendleton S, et al. (2004) Randomized trial of a parent intervention: parents can make a difference in long-term adolescent risk behaviors, perceptions, and knowledge. Arch Pediatr Adolesc Med 158: 947-955.
-
Young KM, Northern JJ, Lister KM, Drummond JA, O'Brien WH (2007) A meta-analysis of family-behavioral weight-loss treatments for children. Clin Psychol Rev 27: 240-249.
-
Sacher PM, Kolotourou M, Chadwick PM, Cole TJ, Lawson MS, et al. (2010) Randomized controlled trial of the MEND program: a family-based community intervention for childhood obesity. Obesity (Silver Spring) 18 Suppl 1: S62-68.
-
García-Huidobro D, Bittner M, Brahm P, Puschel K (2011) Family intervention to control type 2 diabetes: a controlled clinical trial. Fam Pract 28: 4-11.
-
Keogh KM, Smith SM, White P, McGilloway S, Kelly A, et al. (2011) Psychological family intervention for poorly controlled type 2 diabetes. Am J Manag Care 17: 105-113.
-
Martire LM (2005) The " Relative" Efficacy of Involving Family in Psychosocial Interventions for Chronic Illness: Are There Added Benefits to Patients and Family Members?. Fam Syst Health 23: 312.
-
Martire LM, Lustig AP, Schulz R, Miller GE, Helgeson VS (2004) Is it beneficial to involve a family member? A meta-analysis of psychosocial interventions for chronic illness. Health Psychol 23: 599-611.
-
Chesla CA (2010) Do family interventions improve health? J Fam Nurs 16: 355-377.
-
Hartmann M, Bäzner E, Wild B, Eisler I, Herzog W (2010) Effects of interventions involving the family in the treatment of adult patients with chronic physical diseases: a meta-analysis. Psychother Psychosom 79: 136-148.
-
Martire LM, Schulz R, Helgeson VS, Small BJ, Saghafi EM (2010) Review and meta-analysis of couple-oriented interventions for chronic illness. Ann Behav Med 40: 325-342.
-
World Values Survey Association (2008) World Values Survey 2005 Official Data File v.20081015.
-
Doherty W, Boss P, LaRossa R, Schumm W, Steinmetz S (1993) Family Theories and Met hods: A Contextual Approach. In: Boss P, Doherty W, LaRossa R, Schumm W, Steinmetz S Source book of Family Theories and Methods: A Contextual Approach: Springer 3-30.
-
Doherty WJ, Campbell TL (1988) Families and health. Newbury Park, CA: Sage.
-
Heru AM (2006) Family psychiatry: from research to practice. Am J Psychiatry 163: 962-968.
-
Rozanski A, Blumenthal JA, Davidson KW, Saab PG, Kubzansky L (2005) The epidemiology, pathophysiology, and management of psychosocial risk factors in cardiac practice: the emerging field of behavioral cardiology. J Am Coll Cardiol 45: 637-651.
-
Dimsdale JE (2008) Psychological stress and cardiovascular disease. J Am Coll Cardiol 51: 1237-1246.
-
McDaniel SH, Doherty, Hepworth J (2013) Medical Family Therapy and Integrated Care. (2nd Edn) New York: American Psychological Association.
-
Engel GL (1977) The need for a new medical model: a challenge for biomedicine. Science 196: 129-136.
-
Peek CJ (2008) Planning care in the clinical, operational, and financial worlds. In: Kessler R, Stafford D, editors. Collaborative medicine case studies New York: Springer 25-38.
-
Ficher L, Weihs KL (2000) Can addressing family relationships improve outcomes in chronic diseases? Report of the National Working Group on Family-Based Intervention in Chronic disease. J Fam Pract 49: 561-566.





