Journal of Family Medicine and Disease Prevention
Provider's Perspectives on Cultural Competence in Ethnically Diverse Primary Care Practices
Mary A Matteliano1* and Debra Street2
1School of Public Health and Health Professions, University at Buffalo, USA
2Department of Sociology, University at Buffalo, USA
*Corresponding author: Mary A Matteliano, Clinical Assistant Professor, Rehabilitation Science, School of Public Health and Health Professions, University at Buffalo, 515 Kimball Tower, 3435 Main St., Buffalo, NY 14214, USA, Tel: 716-829-6728, E-mail: mmatte@buffalo.edu
J Fam Med Dis Prev, JFMDP-1-013, (Volume 1, Issue 3), Research article; ISSN: 2469-5793
Received: August 24, 2015 | Accepted: October 11, 2015 | Published: October 14, 2015
Citation: Matteliano MA, Street D (2015) Provider's Perspectives on Cultural Competence in Ethnically Diverse Primary Care Practices. J Fam Med Dis Prev 1:013. 10.23937/2469-5793/1510013
Copyright: © 2015 Matteliano MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
This study explores how frontline healthcare providers describe and understand the delivery of culturally competent care to underserved groups in three neighborhood primary health care practices. Data from fifty intensive interviews and observations at three field sites in a multi-year study are analyzed using grounded theory techniques. Findings show that providers used a range of deliberate strategies-from establishing provider/patient concordance, to finessing language issues, practicing cultural humility, being in the trenches and enacting patient advocacy-to bridge cultural gaps with their patients. Medical directors modeled culturally competent care within each practice, contributing to organizational unity. Frontline providers' practices demonstrate some of the complexities of enacting culturally competent care and provide evidence for techniques that could be used to improve healthcare encounters with culturally diverse patients.
Keywords
Health disparities, Cultural competence, Primary care, Healthcare providers
Introduction
The individuals and institutions that oversee the distribution of healthcare and the organizations that provide healthcare face exceptional challenges as they struggle to meet the unique needs of diverse populations. Although health disparities are more prevalent among individuals from minority groups, the proportion of minority frontline providers is much smaller than the proportion of culturally distinctive patients who seek care in neighborhood primary care clinics. Health disparities arise from a complex combination of factors that range from low socioeconomic status to language barriers to differences in cultural beliefs and values about healthcare [1]. Understanding structural, cultural, and knowledge barriers that limit access and participation in healthcare involves activities enacted at multiple levels, from clinical to legislative [2]. Advocates of culturally competent healthcare highlight its potential to help close the gaps when cultural barriers in health care contribute to health disparities [3,4]. The assumption is that health gaps experienced by culturally distinctive groups can be bridged, in part, when providers deliver healthcare in culturally competent ways. But what is cultural competence?.
Cultural competency describes a process whereby healthcare providers consider and understand how structural, financial, social, and cultural factors affect individuals' health and attitudes toward illness and disability, and the ways they access services [5-7]. Culturally competent providers, in theory, deliver better care when each new patient encounter improves their understanding of the patient and their context [8]. Healthcare providers are encouraged to abandon counterproductive stereotyping and to alter the power differential between the patient and provider [4,6,9,10] to achieve culturally competent healthcare. Understanding the strategies healthcare providers used to provide culturally competent care to their diverse patients is the empirical focus of the present research.
Literature Review
The United States faces the challenge of providing healthcare to an increasingly multi-cultural community of patients. According to the U.S. Census Bureau [11] recent immigration trends have contributed to a broad range of ethnic diversity in the United States including the surpassing growth of Hispanics and Asians among ethnic populations [11]. Meeting the unique needs of diverse populations, whether native or foreign-born, is both a current and future challenge, as the system strives to meet healthcare needs for ethnically diverse groups that are both growing and aging. Foreign-born and minority persons may experience exceptional healthcare needs throughout their entire lives [12,13] underscoring the importance of the research on cultural aspects of healthcare disparities.
While the size of foreign-born and/or minority groups have grown in the United States, the ethnic characteristics of healthcare professionals has remained predominately homogenous and dominantly white [14]. For example, Blacks, Hispanics, and Native Americans make up 26% of the U.S. population, but only 6% of practicing physicians are from minority groups [15,16]. As for nurses, 82.3% of RNs are from white, non-Hispanic backgrounds while many ethnic groups continue to be underrepresented [17]. Approximately 81% of physical therapy graduates are white [18] as are 90% of occupational therapists, and similar patterns of ethnicity are reflected among audiology and speech-language pathologists [19]. In addition, white, middle-aged individuals from middle class socioeconomic backgrounds comprise the majority of faculty for most university and college health care and public health programs [20,21].
Not only are there relatively few ethnically diverse healthcare professionals, many medical students are choosing specialty careers over primary care [16]. Although studies show that the overall health of a community improves in proportion to the number of primary care physicians available [22-24], medical schools and the structural arrangements of the U.S. healthcare system promote an orientation towards specialization. This devalues the position of primary care physician in medicine [25] and directly affects the sustainability of primary care in communities.
There are also wide socioeconomic status (SES) gaps between healthcare providers and their patients [26]. Healthcare providers, especially physicians, enjoy the social and economic benefits that accompany high levels of education [27] and occupational prestige. Without being fully conscious of the gap between their patients' lives and their own, physicians and other healthcare providers may distance themselves from their patients or stereotype those from lower SES as the "other" [26]. If the patient's cultural background also differs, additional distancing may occur, particularly if providers have stereotypical views of other cultures [28]. Although often unrecognized, social distance between the provider and the patient can hinder communication and rapport, variables that are crucial to the delivery of equitable healthcare [8,26,28]. For these and the other aforementioned reasons, the way healthcare providers understand and experience their own efforts to provide healthcare that bridges cultural gaps, framed within the contexts where their work is performed, is an important area for research.
The present research tackles a particular component within the health disparities puzzle-efforts by frontline primary healthcare providers to minimize culturally-influenced causes of health disparities, by delivering culturally competent care. Our research explores how healthcare providers in three inner-city practices characterize the strategies they use in health provision for culturally diverse primary care settings. Using data from a multi-year interview and observational study, we identify key themes associated with health providers' attempts to provide culturally competent care.
Methods
The principal investigator conducted interviews and observations at three primary health care practices located in inner city neighborhoods in a mid-size city in the northeastern United States. Findings are reported using pseudonyms (both of field sites and the individuals within them) to maintain confidentiality of the participants in the research. The sites provide primary healthcare through three different organizations, each serving a distinctive vulnerable patient population. Two sites are private practices, while the third is affiliated with the city's largest not-for profit corporate hospital group. Each practice is located in a different inner city neighborhood with racially and ethnically diverse and, typically, low-income residents.
The first site, Washington Family Medicine (Washington), serves a patient base comprised almost entirely of African Americans. The second site, Centro de Asistencia Medica (Centro), serves a large Hispanic community and a smaller sub-population of refugees. The third site, Good Samaritan Family Practice (Good Samaritan) has two locations. The larger Good Samaritan site is in a very diverse transitional neighborhood comprised of an aging generation of Italian residents, a more recent influx of Hispanic residents, African Americans, plus a sizeable refugee population. The smaller Good Samaritan site serves one of the city's almost exclusively African American neighborhoods.
Data consist of interviews and observations of individuals working at three different health practice organizations. Intensive interviews with healthcare providers and staff elicited their perspectives on: (1) cultural competence in treating patients; (2) the influences of organizations and institutions that accommodate healthcare services; and (3) their own attempts to be culturally competent providers. Site selection was purposive, to maximize the cultural variation in patient groups and practice types. Interviewees were also sampled purposively, including physicians, nurse practitioners, nurses, and supportive office staff to ensure a full range of perspectives from different professional vantage points. The medical directors allowed all interviewees to take time from work to be interviewed and none of the healthcare providers or office staff who was approached, refused to be interviewed. Once a rapport was established and the initial interviews were conducted, healthcare providers and staff made recommendations for future interviewees, allowing us to use snowball sampling to obtain additional respondents. The PI conducted the interviews at the family practice locations, the interview times ranged from 30 to 60 minutes, and the interviews were conducted from September 2007 to March 2009. Several respondents were interviewed multiple times. Consequently, the data includes perspectives from a spectrum of healthcare providers and staff working at three distinctive practices serving cultural minority and impoverished patient communities.
Data
The complexities of professional socialization and practice characteristics makes a qualitative approach to data collection and analysis most appropriate [29]. Data validity was enhanced by direct observational access to the environment and interactions with research participants [30,31] and cross-checking analytic points with both respondents and experts in the field.
Data are from field notes, observations, and transcripts of intensive formal interviews with 41 healthcare providers (physicians, nurses, and members of other allied health professions) and supportive office staff who worked in three culturally diverse neighborhood primary health care practices. Triangulation of findings from the field data was achieved through analysis of nine additional interviews with experts in the field on cultural competence. These included interviews with administrators, social workers, and healthcare providers at centers that provide services for refugees and asylum seekers, and with professors in nursing and medical schools who teach cultural competency in their curricula.
Analysis
We developed a set of tables and working figures/diagrams to organize data under broad thematic headings by analyzing the transcribed interview data until thematic saturation was achieved. Descriptive code words were developed for recurring concepts, and analytic choices determined where these more refined concepts fit or overlapped within the overarching categories developed initially. The last analytic step compared across conceptual categories using axial coding. The initial process of creating concepts (open-coding) transitioned to examining the relationship between the concepts within the categories and sub-categories that were created [32]. Further data were acquired from nine additional interviews with key informants/experts after the interviews at the three sites were conducted. These data, too, were used to saturate core and related categories as recommended by Glaser in describing grounded theory methods [33].
Demographic characteristics of interviewees at three sites
Table 1 shows the demographic characteristics of the healthcare providers interviewed for this research. Thirteen physicians were interviewed, seven had minority backgrounds. Although the proportion was higher in this small sample, the pattern of higher concentrations of minority physicians in inner city practices is observed across the U.S. [34]. Thirteen non-physician healthcare providers included nurse practitioners (NPs), nurses, a social worker, and a physical therapist. Three of the five nurses were African, African American, or Hispanic; all five NPs were white. Most of the non-physician professional healthcare workers were women. Age range for healthcare providers was between 29 to 60 plus years. Although income level was not verified among physicians and healthcare providers, all physicians and most of the other healthcare providers would have had incomes substantially higher than the average income among the population they served.
![]()
Table 1: Healthcare Providers by Age, Ethnicity and Gender.
View Table 1
Fifteen office and support staff were interviewed including, business managers, receptionists, medical clerks, filing clerks, billers, insurance facilitators, and a maintenance worker. There was a high rate of ethnic concordance between office workers and staff and the communities each practice served and their ages ranged from early 20's to 60 plus years. Findings discussed in this paper focus on the ways healthcare providers talked about cultural competence in three inner city primary healthcare settings.
Results
Healthcare providers' strategies for culturally competent care
Ethnic Concordance and Language: Power differentials may be less intimidating when at least some of the healthcare providers' personal characteristics are concordant with patients, with patients reporting higher levels of satisfaction from office visits with providers of similar ethnicity and according concordant physicians more respect [26]. For example, the African woman physician at Centro said her ethnicity helped her develop rapport with African refugee patients more easily than with some patients from other backgrounds. Centro had the most ethnically diverse physicians, an advantage given its focus on serving refugees, immigrants, and members of the Hispanic community. Obviously, language matters, too, as two physicians at Centro noted.
...when patients find out that I am Puerto Rican and Dominican they identify with that ... they really like it when you speak their dialect and you understand them [Physician, Centro, 4/8/2008].
Being Hispanic and understanding other peoples' culture, especially the Hispanic culture, it makes it a lot easier to provide them information that is tangible to them and that's why it is important to hook up physicians and patients who are the same cultural background if possible.... The patient can relate to the physician a lot better and as a result trust them more. [Physician, Centro, 4/8/2008].
Both physicians expressed the conviction that physicians need to be involved in the communities they serve and regarded their participation in community health fairs and neighborhood health promotions as important contributions to their patients' cultural communities. Similarly, a Hispanic physician from Washington noted she was in high demand with its Hispanic patients, but not only due to her cultural background. She was also popular with the young patients-whether African American and Hispanic-because she was younger and had children, which resonated with their life experiences (Physician, Washington, 11/27/2007). Providers with similar ethnicity or background alleviate some patients' fears-no matter how broadly based the similarity.
For example, a nurse in her twenties, originally from Sierra Leone, explained that although patients from Africa spoke several different languages, her African background made it easier to overcome obstacles of trust [Nurse, Good Samaritan, 6/25/08]. Several constructs help to bridge the gap when providers try to achieve cultural competence, including language, shared cultural knowledge, and sometimes both. A Puerto Rican nurse in her thirties, with children of her own, certainly thought so. She used shared language, alongside her distinct advantage of shared cultural knowledge, to work effectively with young Hispanic mothers in the pre- and peri-natal programs [Nurse, Centro, 2/12/08]. She was able to help women patients feel comfortable discussing their most intimate health problems, bridging part of the provider/patient gap. A NP also observed the importance of her fluent Spanish in providing good care:
A lot of my patients actually do understand English... but they are more comfortable explaining their needs in Spanish because the small nuances of how they describe symptoms is very specific in a language and sometimes when you don't have good command of the language you miss all that [NP, Centro, 3/12/2008].
Although not Hispanic, her Spanish proficiency and desire to understand the cultural needs of Hispanic patients created a patient following. Shared language and respect for patients' culture overrides ethnic non-concordance in this case, and allows the NP to broker understanding between two cultures.
Cultural Humility: Sharing common ethnic heritage and languages were not the only ways care providers could establish rapport. In fact, proponents of culturally competent care direct their focus toward healthcare providers whose cultural backgrounds differ from their patients. A non-Hispanic NP at Centro said "I think my Spanish patients like me because I share a lot of myself and my family" [NP, 3/12/2008]. While ethnic concordance in some cases and gender or age in others may help establish good relationships between providers and patients, concordance is not possible in all settings. Providers then must establish rapport and trust using other interactional strategies that enable them to pursue cultural competence. These strategies, which include an openness and willingness to learn important patient cultural practices, are ways of practicing cultural humility. A practitioner who practices cultural humility acknowledges that they will never achieve perfect cultural competence, but by being open to patients' cultural beliefs and understanding the social and contextual factors that influence adherence to medical regimens, non-concordant providers can develop partnerships with patients who are culturally different [35-37].
A white physician at Washington family medicine, whose patients were mainly African American, thought best to get differences out right away.
Experience is significantly different from my patients and um...I know sometimes I don't understand all the challenges they face in a day... I deal with that by confessing that and bring the elephant into the room and make it a part of the conversation and they can contrast with that... [Physician, Washington, 2/26/2009].
Presenting and emphasizing his humble roots to patients and confessing imperfect knowledge rather than his professional stature, this seasoned physician tried to minimize social distance, opening the door to learn about patients' different life experiences-experiences that are often unfamiliar to physicians [38. This style of interaction, using cultural humility, reduces some of the power differential between provider and patient, opens up communication, and acknowledges patients' areas of expertise-their own lived experiences [35,36].
Physicians in this study advocated formal educational training that could make medical students more culturally sensitive. A woman physician at Centro, actively involved with medical students' training in cultural competence said:
Compassion helps but it is not the whole shot. We need to give them [medical students] techniques and training...you can't ever be culturally competent. The students really know that. Giving them some techniques about checking, asking, and the whole power differential, you are already a power authority and if you are a refugee who has been abused in any way, you might see that power differential as threatening. ...try to sort of get rid of that and your patient may be more likely to talk to you, no matter what culture they are from [Physician, Centro, 4/22/2008]
As a medical educator, her perspective reflects the current stance in medical training: culturally competent care requires more than a few simple mechanized steps or a standardized response to culturally unique patients [10,38]. She emphasizes that cultural competence-as an ideal type-is a goal to aim for but almost impossible to achieve. Health providers cannot entirely remove themselves from their background, power relationships and experiences that include stereotypes of others, nor can they immerse themselves completely in a different culture. Again, maintaining the stance of cultural humility and acknowledging that cultural competence is a lifelong process helps physicians and other healthcare providers close the gap between patient and professional [35].
Root Causes: In some cases, health providers made repeated efforts to find out the root causes of a patient's illness-beyond its medical diagnoses-in an attempt to understand either why their patients did not adhere to treatment regimens or why no biological cause could be linked to physical complaints. Providers reported that, in some cases, physical complaints were a pretext for an underlying mental health issue-a phenomenon referred to as somatization [39]. Good Samaritan and Centro providers identified this as a frequent phenomenon among refugee patients. When diagnostic tests revealed no identifiable physical cause for a particular problem, several physicians took time to try to find the root cause. One medical director described such a case:
I took care of this Somali woman ...I realized there was no physical cause for these complaints; she kept coming in and at some point you have to think about depression. It was pretty obvious to me she was depressed and you have to start thinking this is the cause of her symptoms that the interpreter and I ...there is no word for depression in their language so how do you even begin to get at that...the closest we could get to was the word "to break my heart" and we tried, we tried to get there [Medical Director, Good Samaritan, 11/8/2007].
Eventually providers and patients have to negotiate and agree upon treatment, but it can be difficult for both parties. Despite explanations about the cause of their illness or physical symptoms, patient comprehension of processes and treatment of any illness, and particularly mental illness, is not guaranteed [40]. Providers emphasized that it took extra time to develop the quality of patient/practitioner relationships to manage gaps arising from patient cultural realities-and that even then, some cultural issues and medical problems seemed difficult or impossible to resolve.
Patient Advocacy: A physician at Centro found that effectively advocating for her patients were necessary, but also a source of constant frustration.
... you have to keep fighting, fighting, fighting for what is out of the norm and the norm is you [meaning herself, or other providers] are in America you can speak English, ...this would not happen to you or me. ...this system does not treat them commensurate with how you or I would be treated [Physician, Centro, 4/22/2008].
She worried that her disadvantaged patients were either incapable or unlikely to advocate effectively to get the healthcare they needed, leaving them perpetually on a lower rung of the healthcare ladder than more sophisticated or savvy patients. Other physicians echoed her concerns about patient advocacy. For example, one physician used his professional reputation to help reverse a specialist's office decision not to perform an urgent colonoscopy. He circumvented office staff gate keeping by advocating for his patient directly with the physician.
Beyond the Call of Duty: Many providers and clinic staff interviewed for this research routinely went "beyond the call of duty" to provide culturally competent services to their patients. One NP drew the sun and the moon on prescription bottles to help an illiterate mother and her daughter take medications at the right time of day. She also created a Spanish/English handout chart on medication management that patients could refer to in their native language for dosages [NP, Centro, 3/12/2008]. In another example of effort beyond the call of duty, the African-born physician at Centro calls patients some evenings. She goes home, thinks about them, and checks up if she realizes they might have unresolved issues, or as she put it, she "gets personal" with her patients, she can relate to young mothers and the problems they face [Physician, Centro, 4/1/2008].
Gender: Women physicians and other healthcare providers frequently mentioned deploying advantages normatively associated with their gender when forming relationships with patients.
I think...um, that female physicians are different and you take time with your patients-whether it is true or not they perceive us as being more nurturing and more...um just you know that we take more time with them so I think that there is that aspect [Physician, Centro, 4/08/2008].
Whether woman physicians are more nurturing or not, this physician remarked that patients perceive them to be. Such gendered assumption aided in her establishing rapport with patients. Many women providers talked about "scolding" their patients or being "motherly." Combining the professional and mother role seemed to inspire trust in patients. A possible explanation for this, especially at Centro, is that the mother archetype, Marianismo, is a predominant theme among many cultures, especially the Hispanic community [41]. Being "motherly" seemed to work well in gaining respect not only among patients in the Hispanic community, but also among African American patients and other groups as well [42].
Both men and women providers discussed the need for patience, taking time, and careful listening as components of cultural competence. Further, many men physicians said they deliberately incorporated empathetic and rapport-building strategies into their practices. These characteristics may be less an issue of gendered characteristics of providers than familiar attributes cultivated among family physicians, who are socialized in ways that contribute to building and sustaining long-term relationships with patients [43-45].
Niches: Many providers at Centro and Good Samaritan worried about providing culturally competent care for Muslim patients, a growing part of patient caseload. However, some providers established relationships of trust with Muslim patients and managed to deal with some of the predictably sensitive gender relationship issues that arose, with little fuss. For example, the Good Samaritan medical director did not seem to find the same culturally specific gender relationships as bothersome as some others-he simply took them in stride. He emphasized the broad variations among Muslim patients' beliefs, reinforcing the principle that various ethnic and religious groups are heterogeneous. In fact, strict adherence to gender relationships may vary among Muslim individuals depending on age, gender, and length of stay in the U.S. [46]. In another case, a woman NP at Centro established a niche treating Muslim patients and carried a proportionately higher amount of Muslim patients than other providers [37]. Her colleague stated:
I know they [Muslim patients] like [NP xxx] a lot...she has many Muslim patients and they love her and they love Dr. xxx... and you have to look at the husband and talk to the husband...so even the kids you are asking the father and I will be asking Mom...it is hard for me to not ask the Mom and that I have to ask the Dad...it is really hard [NP, Centro 3/12/2008].
While her colleague could effectively communicate within traditional Muslim protocols for communication with both women and men, one particular NP acknowledged she had problems doing so, finding it difficult to overcome her own cultural beliefs about appropriate gender relationships in clinical encounters. When that happens, the availability of a team of healthcare providers is an important component of culturally competent care. Reliance on others who have developed expertise or understanding with particular groups, or who have overcome their own cultural prejudices, may help an entire practice function in a more cohesive and culturally sensitive manner. The development of niche or cultural specialties within the healthcare teams at practice sites means all members' talents can be used most effectively, minimizing the shortcomings of single or particular members [37].
Preserving Dignity: Providers observed that developing rapport and a therapeutic relationship with a patient takes time. Yet, physicians are trained to process patients quickly and efficiently regardless of patient personal characteristics, expecting patients to answer personal questions during the first visit, and to divulge personal information without an opportunity to develop a participatory relationship [36]. Even patients who are familiar with U.S. healthcare and conditioned to provide physicians with personal information on demand, often find the medical interview stressful [10,47,48].
Central to the development of patient and provider rapport is building trust; a precarious process for providers working with patients whose experiences had bred mistrust with many authority figures [40]. Preserving dignity was one trust-building tactic that meant that the provider did not ask questions based on personal curiosity, but rather encouraged patients to maintain their dignity in the midst of the medical encounter. The medical director at Good Samaritan remarked that medical students are not always socialized to maintain patient dignity and build trust.
...They [patients] have to get to know us before they're going to trust us... medical students were taught we have this right as a doctor to just go into a room and ask someone how many sexual partners they have and who they sleep with, do you sleep with men or women, and um... and what do you believe in, does your husband beat you up or to refugees, what kind of trauma, what was it like, that comes and that information has to come at some point but I don't think we have the right to ...to go there, and I try to build a relationship and then all that stuff will come out in time...[Medical Director, Good Samaritan,11/8/07].
Compounding the power differential between patient and physician is that medical students' socialization experiences often desensitize them to different patients' personal, contextual, and cultural needs for privacy or circumspection [36]. When that happens, providers may be culturally inept in maintaining patients' dignity, a particular risk among refugees who have experienced physical and mental anguish associated with their ordeals [40]. For example, a Centro nurse told me about a group of women who were illegal immigrants, held against their will and forced to work as prostitutes at local massage parlors. After police raided the massage parlors, the women were referred to Centro for medical care. According to her, the women made little eye contact and did not want to engage in conversation with the healthcare providers [Centro nurse, 3/26/2008]. The stigma and shame of their situation seemed too much for some to bear. The nurse decided the best route was to safeguard these women's dignity by avoiding direct discussion of their recent ordeal and giving them time to adjust to their change in circumstances.
Voyeurism, as described by a Centro physician, is fascination with patient details that are not clinically important and serve mainly to satisfy curiosity about cultural differences. Several providers who worked with refugees articulated similar sentiments. Allowing the patient to open up over time and maintain their dignity, while preserving a core of privacy, was a strategy that provider's at all three sites mentioned to help build trust. One discussed the sensitivities of patient disclosure:
...you don't have to delve into every single thing and you do need to maintain objectivity-the same with the refugees- fascinating to hear about the culture but ...maybe you don't have to strip away everything and maybe it isn't your right to know everything...you have to leave them defenses... if you strip away everything then the patient has nothing left to protect themself with [Physician, Centro, 4/22/2008].
In the Trenches: Despite the emphasis many of the healthcare providers in this study placed on enacting cultural competence, not every physician interviewed attributed equivalent importance to devising culturally specific ways to interact with patients. As one physician from Washington remarked:
...we spend a lot of time talking about culture but that sort of gets around the whole culture issue-everybody is an individual and there is more difference in individuals in a culture than there is between cultures and so we kind of figure out what that individual needs-sometimes you don't do a good job and sometimes you never figure it out and the patient has to go see someone else ... [Physician, Washington, 2/26/2009].
While the physician acknowledged that he might not understand all patients' needs and that another provider might end up providing better care, he did not place much credence in the focus on culture per se. Instead he emphasized heterogeneity within cultural groups as a reminder not to stereotype patients. Treating the patient as an individual, rather than focusing on the characteristics of their cultural group, was another way some providers talked about clinical relationships with patients. They explained procedures and changed approaches with particular patients in mind-but they did that whether the changed approaches were interpreted as demanded by the cultural position of their patient, or not.
An older white physician thought that despite current heightened interest in the role cultural competence plays in healthcare encounters, there really was not all that much new about cultural competence:
There is not a great deal of difference between cultural competency and common courtesy. "Ask me what I want", it does not matter what nationality I am, asking and educating ourselves... You're in a community long enough you get to know the culture of the community [Physician, Washington, 10/31/07].
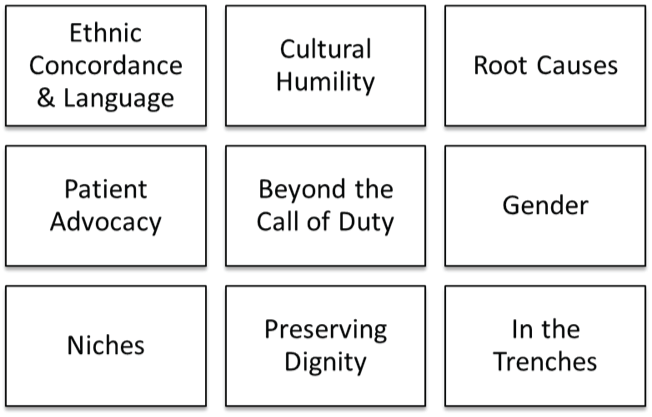
Perhaps good listening skills, changing approaches according to patient needs, and understanding the culture of the community are ways of showing common courtesy to patients and going beyond the precursory history and physical. Yet, researchers argue that reaching cultural proficiency is more-a process that requires awareness, knowledge, skill, and desire [4,49]. Perhaps common courtesy is a beginning and an attribute that has been underused among some healthcare providers in their pursuit of efficiency and medical competence, no matter which cultural group they serve. However, this physician notes that understanding the culture of a community is a process and a long-term commitment, which showed a commitment to cultural proficiency, albeit defined in his own way. This physician may view the term cultural competency as jargon, yet perhaps shares the view of cultural competency proponents that, in order to learn culture competence, it must be practiced in the trenches. Figure 1 summarizes individual strategies to achieve cultural competence.
Discussion
Professional and personal socialization experiences and the particular characteristics of organizations appear to influence healthcare providers' propensity and proficiency for culturally competent care. Ethnic concordance and shared language between providers on the one hand and patients on the other helped providers in different roles in these practices to develop rapport and build trusting relationships with their culturally diverse patients. Providers who did not match the ethnic or cultural characteristics of their patients used techniques such as cultural humility to help develop trustful and sustained relationships with their patients over time. Women physicians, nurse practitioners, and nurses frequently referred to their gender and their status as mothers as traits that helped them develop trustful relationships with their patients.
Many providers and professional staff described their work at the practice sites as a calling or a vocation, confirming that they perceived their interest in providing healthcare for underserved groups as altruistic, not exclusively motivated by profit or gain. Shared values in the importance of providing healthcare for the underserved were common themes in the interview data and according to many providers and staff, the medical directors were a source of inspiration in modeling these values. The medical directors served as organizational role models who inspired the group culture at each specific site. These leadership traits motivated the professionals and many office workers to strive to provide culturally competent care to their patients, despite obstacles, frustrations, and lack of resources.
Providers admitted that there were times when they could not meet patients' needs due to communication problems or because they failed to fully understand a patient's customs and culture. When that happened, resources available in other components of the healthcare team could compensate. For example, several providers developed niches and specialties within the practice. This suggests that interdisciplinary healthcare teams within these practices evolved in many ways that improved the overall efficiency of the practice, and that the individuals who comprise effective teams have talents and propensities that are uniquely valuable.
Providers emphasized the importance of building trustful relationships and preserving dignity as strategies they used to deliver culturally competent care to patients. Providers developed trustful relationships by learning more about patients, their family members, and the cultural and socioeconomic needs of the community, using strategies that took them beyond the call of duty. However, providers realize that optimizing the relationship between provider and patient is an ongoing challenge. There are times that probing might lead to undue distress for patients who have survived difficult and possibly horrendous circumstances. Most providers preferred not to probe so deeply that they might be viewed as demanding answers to questions; rather, a gentler and more oblique route allowed patients to reveal what was necessary over time and at their own pace. One outgrowth of preserving patients' dignity may be that patients become more self-efficacious regarding their own healthcare. Although providers were often strong patient advocates for patients who lacked self-efficacy or had difficulty navigating the U.S. healthcare system, most regarded it as important for the patient to transition to self-initiated health behaviors. Providers and office workers who went too far, did "too much" for patients may have unintentionally enabled dependence.
This raises a question: Does providing culturally competent care follow a curvilinear relationship to the outcomes providers hope to achieve for their patients, or that providers believe patients should want to accomplish? The relationships between health care providers and patients are fragile and must be closely monitored by the provider (and patients as they become more self-efficacious). There is not a clear line of demarcation between enabling versus promoting self-efficacy and wherever the line is, it may differ for each patient depending on his or her age, gender, socioeconomic condition, and ethnicity. The process of negotiation, with a clear understanding of the patient's contextual considerations, will promote partnerships between patient and provider and hopefully aid in patients adapting self-efficacious health behaviors [8,50,51].
Limitations and directions for future research
This research provides insight into the perspectives of healthcare providers and their capacities to enact culturally competent healthcare within underserved community settings. While the richness of qualitative data provides contextual depth associated with interactional processes, the research has some limitations. Although numerous safeguards were implemented to enhance the reliability and validity of the data, there are always possibilities for human bias and misrepresentation by respondents in a small sample. Nonetheless, purposive sampling maximized variation; thematic saturation established confidence in the scope of the study and cross-checking the analysis with respondents and experts produced confidence in the authenticity of the findings. The potential for bias due to primary healthcare providers self-selecting into settings that provided care to ethnically diverse individuals may create the impression of such healthcare providers being more likely to embrace the values of culturally competent healthcare than would be typical of physicians in other types of settings. Nonetheless, providing empirical verification of multiple strategies deployed to enact culturally competent care-strategies that likely reflect provider/patient encounters in many diverse cultural settings-underscores the transferability of the findings.
Future avenues for research about the delivery of culturally competent care are varied. Inclusion of more in-depth data about the roles office staff play in practice teamwork would establish when their actions contribute to cultural competence at the practice level, and highlight similarities and differences between healthcare providers and other staff. How patients in healthcare settings experience cultural competence or incompetence is another fruitful direction for additional research. Finally, a research design that features sustained observation and interviews incorporating providers, office staff, and patients would represent an important extension to this exploratory research.
This research has important practice and educational implications. Perhaps a good start in teaching cultural competence to healthcare providers is to complement classroom instruction with actual experiences with diverse patients. Students who participate in structured encounters with diverse individuals tend to develop self-awareness, confidence, and advocacy characteristics that will assist them in their future delivery of healthcare services [36,52,53]. Treating patients with cultural competence means understanding the impact that culture, social interactions, living environments, and socioeconomic status have on individual health. Successful, culturally competent patient encounters may not seem efficient at first, but they may be in the long run-instrumental for the implementation of healthier lifestyles in the future. If that is true, the time and effort invested in providing culturally appropriate care might pay off in economic efficiency if, for example, providing care that way slows the onset of chronic conditions. At the organizational level, effective training among all healthcare team members will also improve operational efficiency and create more capacity for culturally responsive care.
Statement of Ethnical Research
The University at Buffalo Internal Review Board approved the research conducted for this study. All participants were fully informed of the research process and signed consent to participate, confidentiality was stringently adhered. Participants' identity was protected and the names of the clinical sites were changed.
References
-
Craddock-Lee SJ (2009) Science, surveillance, and the politics of redress in health disparities research. Race/Ethnicity 3: 51-74.
-
Carrillo JE, Victor AC, Hector RP, Debbie SL, Ana NP, Alex TB (2011) Defining and Targeting Health Care Access Barriers. J Health Care Poor Underserved 22: 562-575.
-
(2001) Crossing the Quality Chasm: A New Health System for the 21st Century. Institute of Medicine, National Academy Press.
-
Sotnik P, Jezewski MA (2005) Disability Service Providers as Culture Brokers. In: Stone JH, Culture and Disability: Providing Culturally Competent Services. Sage, Thousand Oaks, CA, USA 37-64.
-
Berlin EA, Fowkes WC (1983) A Teaching Framework for Cross-Cultural Health Care: Application in Family Practice. West J Med 139: 934-938.
-
Black J, Purnell L (2003) Cultural Competence for the Physical Therapy Profession. J Phys Therapy Educ16: 3-10.
-
Rorie JL, Paine LL, Barger MK (1996) Primary Care for Women, Cultural Competency in Primary Care Services. J Nurse Midwifery 41: 92-100.
-
Langer N (1999) Culturally Competent Professionals in Therapeutic Alliances Enhance Patient Compliance. J Health Care Poor Underserved 10: 19-26.
-
Betancourt JR (2006) Cultural Competence and Medical Education: Many Names, Many Perspectives, One Goal. Acad Med 81: 499-501.
-
Ayonrinde O (2003) Importance of Cultural Sensitivity in Therapeutic Transactions: Considerations for healthcare providers. Dis Manag Health Outcomes 11: 234-246.
-
Grieco EM, Acosta YD, Patricia de la Cruz G, Gambino C, Gryn T, et al. (2012) The Foreign Born Population in the United States: 2010. Census Bureau, US.
-
Geronimus AT, Hicken M, Keene D, Bound J (2006) Weathering and Age Patterns of Allostatic Load Scores among Blacks and Whites in the United States. Am J Public Health 96: 826-833.
-
Zuvekas SH, Taliaferro GS (2003) Pathways to access: Health Insurance, the Health Care Delivery System, and Racial/Ethnic Disparities, 1996-1999. Health Aff 22: 139-153.
-
Jones ME, Cason CL, Bond ML (2004) Cultural Attitudes, Knowledge, and Skills of a Health Workforce. J Transcult Nurs 15: 283-290.
-
Bazemore LD, Bowman R, Petterson S, Greene LA, Phillips RL (2007) Will Medical School Expansion Help Diversify the Physician Workforce? Am Fam Physician 76: 38.
-
Turner EJ, Bazemore AW, Phillips RL, Green LA (2008) Will Patients Find Diversity in the Medical Home? Am Fam Physician 78: 183.
-
(2008) National sample survey of registered nurses: New careers in nursing. Robert Wood Johnson Foundation.
-
Lattanzi JB, Purnell LD (2006) Introducing Cultural Concepts: Developing Cultural Competency in Physical Therapy Practice. F.A. Davis, Philadelphia, USA 7: 4.
-
McGruder J (2003) Culture, Race, Ethnicity, and Other Forms of Human Diversity. In: E. Crepeau, Cohn E, Schell BA (eds) Willard & Spackman's Occupational Therapy 10th (edn) Lippincott Williams & Wilkins, Philadelphia, USA 81-95.
-
Kardong-Edgren S (2007) Cultural Competence of Baccalaureate Nursing Facility. J Nurs Educ 46: 360-366.
-
Murray-Garcia J (1999) The Public's Health, Its National Identity, and the Continuing Dilemma of Minority Status. J Health Care Poor Underserved 10: 397-408.
-
Beal AC, Doty MM, Hernandez SE, Shea KK, Davis K. (2007) Closing the Divide: How Medical Homes Promote Equity in Health Care. The Common wealth Fund.
-
Shi L, Starfield B (2001) The Effect of Primary Care Physician Supply and Income Inequality on Mortality Among Blacks and Whites in US Metropolitan Areas. Am J Public Health 91: 1246-1250.
-
Starfield B, Shi L, Macinko J (2005) Contribution of Primary Care to Heatlh Systems and Health. The Milbank Quarterly 83: 457-502.
-
Fry J, Light D, Rodrick J, Orton P (1997) The US Health Care System. In: Conrad P (ed) The Sociology of Health and Illness 5th (edn), Clinical Perspectives, St. Martin's Press, New York, USA 206-214.
-
Malat J (2001) Social Distance and Patients' Rating of Healthcare Providers. J Health Soc Behav 42: 360-372.
-
White K (2002) An Introduction to the Sociology of Health and Illness. Sage Publications, London.
-
Cooper-Patrick L, Gallo JJ, Gonzales JJ, Vu HT, Powe NR, et al. (1999) Race, Gender, and Partnership in the Patient-Physician Relationship. JAMA 282: 583-589.
-
Guba EG, Lincoln YS (1994) Competing Paradigms in Qualitative Research. In: Denzin NK, Lincoln YS (ed) Handbook of Qualitative Research. Sage Publications, Thousand Oaks, CA, USA 105-117.
-
Altheide DL, Johnson JM (1994) Criteria for Assessing Interpretive Validity in Qualitative Research. In: Denzin NK, Lincoln YS, Handbook for Qualitative Research. Sage Publications, Thousand Oaks, CA, USA 485-499.
-
Babbie E (2004) The Practice of Social Research (10th edition) Belmont, Wadsworth/Thompson Learning, CA, USA.
-
Strauss A, Corbin J (1998) Basics of Qualitative Research, Techniques and Procedures for Developing Grounded Theory 2nd (edn). Sage Publications, Thousand Oaks, CA, USA.
-
Glaser BG (2005) The Grounded Theory Perspective III: Theoretical Coding. Sociology Press. Mill Valley, CA, USA.
-
Reschovsky JD, O'Malley AS (2008) Do Primary Care Physicians Treating Minority Patients Report Problems Delivering High-Quality Care? Health Affairs 26: 222-231.
-
Tervalon M, Murray-Garcia J (1998) Cultural Humility Versus Cultural Competence: A Critical Distinction in Defining Physician Training Outcomes in Multicultural Education. J Health Care Poor Underserved 9: 117-125.
-
Griswold K, Zayas LE, Kernan JB, Wagner CM (2007) Cultural Awareness through Medical Student and Refuee Patient Encounters. J Immigrant Health 9: 55-60.
-
Matteliano MA, Street D (2012) Nurse practitioners' contributions to cultural competence in primary care settings. J Am Acad Nurse Pract 24: 425-435.
-
Betancourt JR, Green AR, Carrillo JE, Ananeh-Firempong O (2003) Defining Cultural Competence: A Practical Framework for Addressing Racial/Ethnic Disparities in Health and Health Care. Public Health Rep 118: 293-302.
-
Helman CG (2007) Culture, Health, and Illness (5th edition). Hodder Arnold, London.
-
Asgary R, Segar N (2011) Barriers to Health Care Access among Refugee Asylum Seekers. J Health Care Poor Underserved 22: 506-522.
-
Santana-Martin S, Santana FO (2005) An Introduction to Mexican Culture for Service Providers. In: Stone JH (ed) Culture and Disability: Providing Culturally Competent Services. Sage publication, Thousand Oaks, CA, USA, 161-186.
-
Blanchard S, Jenkins C (2006) African Americans. In: Royeen M, Crabtree JL (ed) Culture in Rehabilitation: From Competency to Proficiency. Pearson Prentice Hall, Upper Saddle River, New Jersey, USA 103-130.
-
Aita V, McIlvain H, Backer E, McVea K, Crabtree B (2005) Patient-Centered Care and Communication in Primary Care Practice: What is involved? Patient Educ Couns 58: 296-304.
-
Paasche-Orlow M, Roter D (2003) The Communication Patterns of Internal Medicine and Family Practice Physicians. J Am Board Fam Prac 16: 485-493.
-
Ross M, Willer B (1982) Primary Care and Medical Education. Medical Care 20: 235-241.
-
Ahmad SO, Alsharif NZ, Royeen M. Arab Americans (2006). In: Royeen M, Crabtree JL (ed) Culture in Rehabilitation: From Competency to Proficiency. Pearson Prentice Hall, Upper Saddle River, New Jersey, USA 181-202.
-
Kleinman A, Eisenberg L, Good B (1978) Culture, illness, and care: Clinical Lessons from Anthropologic and Cross-Cultural Research. Ann Intern Med 88: 251-258.
-
Waitzkin H (2000) Changing Patient-Physician Relationships in the Changing Health-Policy Environment. In: Bird CE, Conrad P, Fremont AM (ed) Handbook of Medical Sociology. Prentice Hall, Upper Saddle River, New Jersey, USA 271-283.
-
Campinha-Bacote J (2002) The Process of Cultural Competence in the Delivery of Healthcare Services: A Model of Care. J Transcult Nurs 13: 181-184.
-
Martin DR, O'Brien JL, Heyworth JA, Meyer NR (2005) The Collaborative Healthcare Team: Tensive Issues Warranting Ongoing Consideration. J Am Acad Nurse Pract 17: 325-330.
-
Philips R, Green L, Fryer G, Dovey S (2001) Trumping professional roles: collaboration of nurse practitioners and physicians for a better U.S. health care system. Am Fam Physician 64: 1325.
-
Jeffreys MR (2006) Teaching Cultural Competence in Nursing and Health Care: Inquiry, Action, and Innovation. Springer Publishing Co, New York, USA.
-
Mays VM, Ly L, Allen E, Young S (2009) Engaging Student Health Organizations in Reducing Health Disparities in Underserved Communities through Volunteerism: Developing a Student Health Corps. J Health Care Poor Underserved 20: 914-928.