Journal of Family Medicine and Disease Prevention
Improving Conceptual Clarity of Antenatal Interventions: A Scoping Review
Melissa Buultjens1*, Gregory Murphy1, Jeannette Milgrom2 and Darren Poinen3
1School of Psychology and Public Health, La Trobe University, Australia
2Professor of Psychology, Melbourne School of Psychological Sciences, University of Melbourne and Director of Clinical and Health Psychology at Austin Health, Melbourne, Australia
3Melbourne Institute of Technology and Kaplan Business School, Australia
*Corresponding author: Melissa Buultjens, School of Psychology and Public Health, La Trobe University, Melbourne (Bundoora), VIC 3086, Australia, Tel: +613 9479 6502, Fax: +613 9479 1783, E-mail: M.Buultjens@latrobe.edu.au
J Fam Med Dis Prev, JFMDP-2-043, (Volume 2, Issue 3), Review Article; ISSN: 2469-5793
Received: June 01, 2016 | Accepted: August 31, 2016 | Published: September 02, 2016
Citation: Buultjens M, Murphy G, Milgrom J, Poinen D (2016) Improving Conceptual Clarity of Antenatal Interventions: A Scoping Review. J Fam Med Dis Prev 2:043. 10.23937/2469-5793/1510043
Copyright: © 2016 Buultjens M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective:There is increasing awareness of perinatal health as a public health issue, while the antenatal period is a transitional time for parents-to-be and presents various opportunities to maximize health outcomes. The objectives of this scoping review were to identify non-pharmacological interventions in antenatal care, to examine the health outcomes and reductions of perinatal morbidity occurring in childbearing women as a result of these interventions, to explore the mechanisms of intervention effect, and overall, highlight where further development and research into perinatal health practice and service delivery may be warranted.
Design:The literature search was conducted using Medline and CINAHL for peer-reviewed research reported in journals using the English language. Studies that reported randomised controlled trials of universal interventions (i.e. that target all childbearing women that have not been identified on the basis of individual risk) initiated from conception up to, and including, the intrapartum period that were designed to improve maternal and perinatal health outcomes were included in the search. Study selection, data extraction and data analyses were performed by two investigators. Effect sizes at post-intervention were calculated and studies were categorised into key dependent-variable categories.
Findings:Thirty-one papers that examined universal non-pharmacological interventions that aimed to facilitate maternal health during the antenatal period and/or intrapartum period were identified. Findings suggested that skill-based interventions, particularly those with a physical component, (e.g., exercise), produced positive results on a number of outcome variables (e.g. emotional health and wellbeing). Further, interventions comprising dual-application (i.e. instruction and/or practice of a certain behaviour coupled with individual consultation) are even more likely to produce favorable outcomes.
Conclusion:This scoping review identified key areas in antenatal care for which randomised controlled trials have been conducted and identified that specific non-pharmological interventions were effective for obtaining a number of positive outcomes in antenatal care. Of these studies, mechanisms correlated with positive effect included timing of initiation, i.e., beginning at the start of pregnancy, as well as programs supervised by suitably qualified perinatal health professionals. These findings suggest a guide for future research and service development in the area of antenatal health promoting evidence-based clinical practice, education and health promotion initiatives for women and their families.
Keywords
Transition to parenthood, Scoping review, Midwifery, Antenatal, Intervention, Biopsychosocial, Universal
Introduction
For the expectant parent, the childbearing period has been identified as a major life event that is associated with many potentially distressing challenges [1-3]. Evidence further suggests that morbidity associated with childbirth and its impact on women's health is an area of real concern [4,5]. Despite this, there is a paucity of research examining the scope, content and range of non-pharmacological interventions that may collectively assist all childbearing women. Specifically few studies have explored the breadth, mechanisms of intervention effect, and effectiveness of non-pharmacological interventions that target potentially modifiable risk factors for poor maternal health outcomes [6].
Investment in strategies to promote 'a healthy start to life' has been identified as having the greatest potential to reduce health inequalities across the life course. To date, researchers have systematically examined health promotion before pregnancy, and the contribution of interventions concerning a number of potentially modifiable risk factors that are known to be associated with poor pregnancy outcomes, i.e. smoking, poor nutrition, and alcohol abuse [7]. There have also been reviews of health care interventions to improve clinical outcomes for targeted women, e.g., women with a disability [8] or overweight women [9]. However, little research has been conducted to explore the breadth and efficacy of antenatal interventions designed to prepare and facilitate both clinical (e.g. caesarean section rates, incontinence, gestational diabetes) and psychosocial (e.g. depression, parenting knowledge) aspects that are known to influence perinatal outcomes. Such variables are of importance given the effects and influence they can have on best-practice maternal and child health outcomes. For example, depressive symptomatology in the postpartum period negatively influences infant-feeding outcomes [10] and breastfeeding is widely acknowledged as being a best-practice outcome, with many health benefits [11,12]. Consideration of such variables is also of benefit from an economic stance, as has been illustrated by an Australian analysis estimate that reports the cost of postpartum depression and anxiety in mothers [13,14]. Likewise, the direct economic consequence of not breastfeeding has been well examined [11].
Prevention, promotion and facilitation are important concepts from both a public health and scientific perspective. Researchers posit that prevention "is inversely related to outcome so that by the time cases come to the attention of practitioners, they are harder to treat [15]". While the antenatal period represents an important point of contact with the health care system [16], and there is widespread agreement of the need to improve maternity care services and optimize accessibility to these services, there is a paucity of research that focuses on how this might be implemented and evaluated.
A scoping review provides a summary of the main trends in research in a field, rather than a comprehensive account of all the research such as would be available from a systematic review [17]. If considerable resources are to be devoted to providing models of quality care, education and preventative resources, then it is important to contextually identify interventions and appraise the mechanisms of positive intervention effect. Therefore, the aims of this scoping review were to explore the extent of the literature around perinatal non-pharmacological interventions delivered in the antenatal period as well as appraise if increases in health outcomes and reductions of perinatal morbidity occurred in childbearing women as a result of identified interventions.
With the purpose of a scoping exercise to map a wide range of literature and identify where innovative approaches may lie [18], the current review was undertaken in order to help identify appropriate parameters for further, more rigorous reviews (i.e. systematic), as well as disseminate evidence of a range of interventions specific to the antenatal period. Awareness of health promotion initiatives and interventions serve to strengthen evidence-based clincial care guidelines and education practices, thus reducing well known causes of maternal morbidity and facilitating the overall transition to parenthood.
Methods
A comprehensive literature search was conducted in 2013/14 to identify studies that reported on interventions initiated and implemented during the antenatal to intrapartum periods. Studies that had been published were identified by searching comprehensive electronic databases, Medline and CINAHL. More than one database was used so that the risk of introducing a database bias was minimised and the yield of relevant studies maximised [19]. Databases were searched and reviewed by MB and GM using a combination of terms, including transition to parenthood, childbirth education, maternal, psychological, training during pregnancy, healthy pregnant women, prenatal, antenatal preparation, birth/labour outcomes, antenatal education and randomised control* trial.
Selection inclusion and exclusion criteria
The relevance screening criteria [20] that were used to screen abstracts to identify papers relevant to this scoping review included the following: 1. Does that title/abstract describe a primary research study (as opposed to a review), 2. Does the title/abstract describe an intervention for antenatal childbearing women, and 3. Does the title/abstract include a health and wellbeing outcome to support antenatal childbearing women?
Following the initial screening stage, papers were further reviewed and deemed eligible based on the following: (a) the study evaluated a non-pharmacological intervention, (b) the intervention targeted best-practice outcomes (e.g. breastfeeding), as well as clinical (e.g., labour and birth outcomes), physical (e.g., incontinence), and/or psychological (e.g., depressive symptoms) (c) they were reporting results from a Randomised Controlled Trial (RCT) (d) the intervention was initiated and implemented in the antenatal to intrapartum period only, (e) effect sizes were reported or could be computed from available statistical information, and (f) the intervention was designed to be offered to all childbearing women that have not been identified on the basis of individual risk - i.e. was ‘universal' in the terminology of Mrazek and Haggerty [21].
Data collection and analyses
Two reviewers (MB, GM) collected data and assessed the appropriateness of the studies. All citations were independently reviewed by MB and GM. Titles and abstracts were screened (December 2012 - March 2013) and full texts were obtained for all articles that met the criteria, or if reviewers were uncertain of a particular study's applicability. MB and GM independently assessed research articles (March 2013 - September 2013) for potential selection, performance, and attrition bias. The Jadad scale [22] was applied to evaluate the methodological quality of each study. This scale assigns a numeric score for randomization, blinding and description of dropouts. Twenty-three of the 31 studies scored 3 or greater out of 5. It is worth noting that none of the studies were double blinded, though given the nature of most interventions, double blinding would not be feasible. All calculations and statistics, including the Jadad score and Cohen's d ("d"), were reviewed by an independent statistics consultant.
Search summary
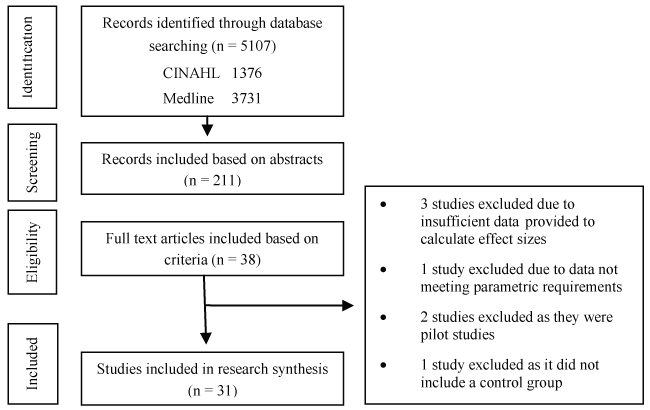
The search identified 5107 abstracts which were screened for relevance. Of the 211 papers included based on the abstracts, a review of the full text articles identified 38 as examining universal non-pharmacological interventions. Based on the selection inclusion and exclusion criteria, 31 RCT studies were included in the final review. Effective percentage agreement between the two authors independently rating the papers (MB; GM) was 82%. Full details of the search can be found in the schematic diagram outlining the review process in figure 1.
Indices of effect size
In preparing information for this review, the measure of effect size used was Cohen's d ("d") [23,24]. Using Cohen's recommendation, [25] effect sizes of 0.20 are considered to be small, 0.50 are medium, and 0.80 are large. The subsequent selection of research articles were reviewed (September 2013 - May 2014) to ascertain, post-test, mean and standard deviation information for both the experimental and the control groups. However, where this basic information was not reported the study was still retained for analysis if it contained statistical data suitable for calculating an effect size. While there are a variety of effect size indices, Cohen's d was judged to be the most useful effect size statistic to employ when interpreting these results [26].
Results
Table 1 summarises the design, intervention, results and effect size of 31 "Antenatal - Universal" studies which compared outcomes of women experiencing preparatory interventions thought likely to benefit childbearing women. It is important to note that because some studies had more than one relevant dependent variable, the number of effect sizes reported from these universal studies is more than 31.
![]()
Table 1: Antenatal - randomised controlled trial universal interventions.
View Table 1
Table 1 show that the main research foci have been on interventions that include education, skills-based practice, and intrapartum support. Table 1 illustrates that the interventions targeted a range of dependent variables. Generally, these interventions can be categorised as follows:
a.) improving aspects of labour and birth outcomes (n = 14);
b.) improving psychological wellbeing (n = 15);
c.) improving physiological functioning (n = 4);
d.) improving physical wellbeing (n = 6);
e.) strengthening couple relationships (n = 1);
f.) improving general maternal and child health outcomes (n = 4);
Improving aspects of labor and birth outcomes
The first group of effect sizes achieved on indicators of labour and birth outcomes (i.e. labour pain, pharmacological analgesia use, type of birth, and duration of labour) varied widely.
Labor pain, five studies in total: Five studies were noted here [27-31], with effect sizes ranging from 0.00 to -1.42, and a median "d" = -0.63.
These studies produced a large spread of effects in reducing pain scores, though the end-point and type of measure were not identical among identified studies. More specifically, Chang, et al. (2002) [27] measured pain at the transitional phase (8-10 cm dilation) using the Present Behavior Intensity Scale (as rated by the nurse); Chuntharapat, et al. (2008) [28] measured 4 hours after the woman had reached 3-4 cm in dilation and was contracting at 30-60 seconds using both the Visual Analogue Sensation of Pain Scale and Patient Observed Labor Pain scales; Wan-Yim, et al. (2009) [31] also used the Visual Analogue Scale measuring pain at the last third of the duration of the first stage of labor (the time which begins with the onset of regular contractions and ends with full dilation of the cervix); Gau, et al. (2011) [29] assessed labor pain by using the Short Form McGill Pain Questionnaire (SF-MPQ) which is a multidimensional assessment combining a Visual Analogue Scale, Verbal Response Scale and a Present Pain Intensity Scale, measuring a 8 cm dilation; and finally Gedde-Dahl and Fors (2012) [30] used a Numeric Rating Scale 0-10 to measure pain at delivery.
The lowest "d" of 0.00 was observed in both an efficacy-enhancing educational intervention [31] and self-administered CD with booklet intervention [30]. While the efficacy enhancing intervention [31] successfully promoted women's self-reported ability to cope in labour (decreased perception of pain) in the early and middle stages (-0.63; -0.46), results were not sustained in the last stage of labor. Perhaps the strongest result, (triangulated by several pain measures), was noted , for example, in a birth ball exercise programme [29], and produced an effect of -1.42 as measured by the Visual Analogue Scale at 8 cm dilation. Together, this intervention included a multimedia education component and periodic follow ups during prenatal checks. Following this, large effects were noted in a massage therapy intervention during labor [27] (transitional phase = -1.05; average "d" of -0.99 across the three phases), that was closely followed by a skills-based yoga intervention [28] ("d" of -0.54), though it is not clear at what dilation each woman would have been at time point three, and this potentially confounds the accurate comparison of effectiveness between interventions.
Pharmacological analgesia use, four studies in total: Epidural analgesia use was an outcome measure in four interventions, of which effect sizes typically produced small effect [29,32-34] and ranged from -0.05 to -0.20, with a median "d" = -0.06.
The most encouraging results in reducing epidural anesthesia came from Gau, et al. (2011) [29] (d = -0.20) by means of a birth-ball exercise programme, including a multimedia education component as well as periodic follow ups during prenatal checks.
Type of birth, three studies in total: Three studies which focused on types of birth (i.e. cesarean and instrumental deliveries) [29,35,36] produced weak results with "d" ranging from -0.32 to -0.03.
These studies yielded small effects. The largest effect was found in the research which comprised a structured, moderate intensity exercise program that was undertaken the entire pregnancy [35] and yielded an effect of -0.23 when measuring caesarean deliveries between exercise and control groups.
Duration of labour, two studies in total: One investigation [37] produced a strong "d" with regards to the duration of active labor in minutes (d = -0.53), whilst at the 2nd and 3rd stages produced weak results, with an average "d" = -0.03.
One study [29] produced a moderate effect size result for the duration of the first stage of labour, "d" = -0.45, whilst in the second stage of labour there was a weaker result, "d" = -0.22.
In the second stage of labour, both studies produced minimal effects, though the birth-ball exercise programme [29] illustrated stronger outcomes in comparison to the psychosocial intervention that involved support from a close female relative [37].
Improving psychological wellbeing
The literature search produced a number of psychological outcome variables for examination (i.e. anxiety, depression, self-efficacy, stress, and wellbeing after birth).
Anxiety, five studies in total: Five studies measured the effects of the interventions on the women's experiences of anxiety. The results of the interventions varied greatly.
Two studies [31,38] produced "d" values ranging from -0.45 to 0.18 for reduced anxiety scores, with a median "d" = -0.32, while Chang, et al. (2002) [27] produced an average "d" of -0.46 across three phases for the Visual Analogue Scale for Anxiety.
Gedde-Dahl and Fors (2012) [30] measured anxiety at delivery, following the use of a self-administered CD (with relaxation techniques) practiced in the final part of pregnancy. A "d" of -0.36 was calculated between the CD intervention and no intervention, showing relatively small effects on reducing anxiety.
Conversely, measuring anxiety in the antenatal period, similar results were noted in a research paper examining anxiety levels following a mobile phone service as prenatal support [36], which produced a "d" of -0.40.
Overall these varying effect sizes illustrate an inconsistency in reducing anxiety levels among the different interventions. These differences may be accounted for by differing methodologies in measuring the variables. Three of the aforementioned studies used the Visual Analogue Scale (VAS) during labor [27,30,31], while the most favorable result measured at delivery (-0.36) was noted in an intervention that comprised a self-administered practice of relaxation techniques, positive affirmation and guided imagery [30]. The findings from a massage intervention undertaken by Chang, et al. (2002) [27] followed with an effect size of -0.24, as measured in the transitional phase of labour. Finally, Wan-Yim, et al. (2009) [31] found no effect in the last stage of labour (0.18), and overall limited results using an educational programme to reduce anxiety across the three stages of labour, average "d" = -0.26.
The two remaining studies examined general anxiety in pregnant women [36,38], producing high variability in the results in reducing anxiety levels, with the highest "d" = -0.40 for Jareethum, et al. (2008) [36] and lowest "d" = -0.19 for Chang, et al. [38]. However, the findings from Jareethum, et al. (2008) [36] need to be interpreted with caution as anxiety is stated as being measured on a VAS, though there is no reference to validate the questionnaire.
Depression, four studies in total: Two studies used the EPDS scale producing "d" = -0.44 [38] and a "d" = -0.56 [39], illustrating a moderately strong effect on reducing symptoms of depression.
One examination [40] applied the CES-D scale, producing strong results with a "d" of -0.86.
One investigation [41], produced weak results with a "d" = -0.09 (for those with EPDS < 10) in comparison to those who did not exercise before pregnancy (EPDS < 10), "d" = -0.50.
Results showed that all studies produced advantageous findings. All studies were practical in their application, i.e. learning through practice with a skills-based supervised intervention. The strongest result was found in a 12-week supervised exercise program that commenced approximately 16-20 weeks' gestation [40], yet results from a similar exercise program (with a considerably larger sample) did not find a lower prevalence of high EPDS scores among women randomised to regular exercise during pregnancy. Although the present scoping review wasn't examining ‘select' populations, it is worth noting that women in the intervention group who did not exercise regularly prior to pregnancy had a reduced risk of postnatal depression.
Of the remaining two studies, a six-session hypnotherapeutic program showed benefit with a moderate to high effect of -0.56 [39], followed by a two-week self-directed, non-invasive music therapy intervention [38].
Self-efficacy, two studies in total: Two studies [31,34] produced similarly strong results. In Svensson, et al. (2009) [34] the "d" was calculated at 0.74, while Wan-Yim, et al. (2009) [31] used the Chinese Childbirth Self-efficacy Inventory, in particular the two subscales, OE-16, 0.80 and EE-16, 0.89.
Both these studies of group interactive education yielded strong results in improving self-efficacy. While the intervention conducted by Wan-Yim, et al. (2009) [31] focused towards the intrapartum period, i.e. promoting women's self-efficacy for childbirth, Svensson, et al. (2009) [34] measured self-efficacy eight weeks postnatal.
Stress, two studies in total: The two studies that tested for intervention effects on stress [38,42] produced differing "d" = -0.09 and -1.25 respectively.
Results of the two interventions designed to reduce stress were both measured using the Perceived Stress Scale (PSS). Music therapy illustrated minimal reduction in stress level [38], while a skills-based intervention comprising yoga and guided relaxation [42] provided a very large effect size.
Wellbeing after birth, two studies in total: One study [30] produced a medium effect with a "d" of -0.65 between the intervention and no intervention group (assessing a CD intervention (self-administered practice of relaxation techniques). Wellbeing was measured one day after birth using the Edmonton Scale, where 0 is the best possible feeling of wellbeing and 10 is the worst possible feeling of wellbeing.
Similarly, Rakhshani, et al. (2010) [43] assessed well being, however this was measured using the World Health Organization Quality of life (WHOQOL - 100). Results showed a "d" ranging from 0.23 to 0.74, with a median "d" = 0.68. This research, comprising integrated yoga, yielded significant results demonstrating that the intervention improved women's wellbeing after birth. The WHOQOL encompasses many psychosocial components and all yielded strong effects; psychological (0.74); social relationships (0.60); and general health quality (0.72).
Improving physiological functioning
Effect sizes achieved on indicators of physiological outcomes (i.e. physiological functioning, maternal glucose tolerance and gestational diabetes) produced differing results.
Improving physiological functioning (cardiovascular) was assessed in two studies: One study [44] produced a median "d" = -0.47 with a decline on the cardiovascular index. Whilst the other investigation [42], produced an average value of "d" = -0.22 with a range from -0.18 - -0.24 (autonomic responses).
Interventions consisted a single-visit relaxation intervention [44] and integrated yoga practice and relaxation which measured autonomic response [42], together typically producing low to moderate results as shown by the median "d" of 0.37.
The RCT by Satyapriya, et al. (2009) [42], illustrated that practicing yoga and relaxation could reduce autonomic responses, while measures at the 36th week for Heart Rate Variability for Low Frequency (LF), showed small effect sizes, d = -0.24, High Frequency (HF), d = -0.24; and LF/HF, d = -0.18. In contrast, another skills-based study [44] examining the effects of brief progressive muscle relaxation and guided imagery (GI) relaxation exercise on cardiovascular activity, indicated that GI was effective in inducing self-reported relaxation while also producing moderate (-0.47) effect in reducing cardiovascular activity.
Improving maternal glucose tolerance, one study in total: One study (Barakat, et al. 2012) [35] produced a strong result, "d" = -0.90.
This research explored the influence of an exercise program on maternal glucose tolerance, illustrating significant differences between study groups on the 50 g maternal glucose screen (MGS).
Gestational diabetes, one study in total: One investigation [45] produced weak results, "d" = -0.11.
This research objective was to assess whether exercise during pregnancy could prevent gestational diabetes and improve insulin resistance [45]. Results showed that at 32-36 weeks of gestation there were no differences between groups in prevalence of gestational diabetes.
Improving physical wellbeing
Effect sizes achieved on indicators of physical wellbeing constructs (i.e. Pelvic Girdle Pain, Lower Back Pain and/or Lumbopelvic Pain and Urinary and/or Faecal incontinence) produced very weak results.
Pelvic girdle pain, lower back pain and/or lumbopelvic pain, was assessed in two studies: One study [46] produced a low "d" for both Pelvic Girdle Pain (d = -0.02) and Lower Back Pain (d = -0.07).
One examination [47] produced a weak result in relation to Lumbopelvic pain, "d" = -0.03.
Both of the studies examined exercise programs. Results were of minimal impact, suggesting that supervised group exercise did not reduce the prevalence of low back pain or pelvic girdle pain [46], nor could regular exercise significantly influence the prevalence of lumbopelvic pain in pregnant women [45].
Urinary and/or faecal incontinence, four studies in total: Four studies [48-51] produced overall weak results with "d" ranging from -0.07 to -0.33.
All of the above studies primary outcome measure was based on self-reported symptoms. Further, all study interventions involved pelvic floor muscle training and exercise. The largest effect (-0.29) was noted in the earliest investigation [50] which illustrated significantly fewer women reporting urinary incontinence three months after delivery. Subsequent studies demonstrated lesser effect. While the examination by Mason, et al. (2010) [49] demonstrated fewer episodes of incontinence in the pelvic exercise group, the differences were not statistically significant. Similarly, Bø and Haakstad (2011) [48] found no significant differences in the number of women reporting incontinence at six weeks postpartum. However, it is worth noting that the exercises in this intervention were taught in general fitness classes without instruction of correct pelvic floor muscle contraction. Extraneous variables were also cited, being low adherence and a small sample size. The final investigation [51], while also evaluating the outcomes of a general exercise course, differed in that it measured results of incontinence in late pregnancy, but again produced negligible effect (urinary, -0.16; faecal, -0.04).
Strengthening couples' relationship
In the current scoping review, only one study was identified for transitioning parents, which was developed to prevent a deterioration in couples' relationship. This examination focusing on 155 married couples [52] produced moderate "d" values. There were several outcome variables assessed, with a minimum "d" = -0.19 for the Instructor Encouraged Treatment as measured by the Transition Adjustment Scale, and a maximum "d" = -0.54 for the Self-guided treatment as measured by the Marital Virtues profile. Examining two psycho-educational interventions (a self-guided group - (SG), and an instructor-encouraged group - (IE) and a comparable control group - (CG)), findings showed that despite positive formative evaluation results from participants, there were limited positive intervention effects (Transition Adjustment Scale - IE vs. CG, "d" = -0.19; SG vs. CG, "d" = -0.23). The largest effect was noted in the Marital Virtues Profile measure amongst the SG group, d = -0.54 and Relationship Evaluation Measure, d = -0.41.
Improving general maternal and child health outcomes
Effect sizes achieved on indicators of general maternal and child health outcomes (i.e. increasing parenting knowledge and breastfeeding practices) produced mixed results.
Increasing parenting knowledge, one study in total: Increasing parenting knowledge was assessed in one study [34], "d" = 0.33, suggesting modest results. This research design was educational in composition, presented in the antenatal period by means of seven two-hour sessions. As highlighted by the researchers, a feature of the programme was the recognition that pregnancy, labour, birth and early parenting are a microcosm of the childbearing experience, rather than separate topics.
Improving breastfeeding practices, three studies in total: Breastfeeding practices were assessed in three studies [53-55]. The range of values for the "d" was between 0.00 and 0.37.
Two interventions were educational in form, and findings illustrated that those receiving an individual education session with a lactation counselor [56] showed better outcomes (d = 0.37) compared to the structured antenatal education group training program [54]. The study by Forster, et al. (2004) [53] differed in that it compared two strategies for increasing the initiation and duration of breastfeeding in comparison to the control group. The interventions were a 1.5 hour class on practical aspects of breastfeeding, and two one-hour classes exploring family and community attitudes and experiences of breastfeeding. Neither intervention increased breastfeeding initiation or duration.
Discussion
Main findings
From this set of experimental studies, the results produced data across a range of domains that were grouped into six main categories for analysis of post intervention effects. Consecutively, the largest numbers of interventions were noted in the categories of: improving psychological wellbeing, improving aspects of labour and birth outcomes, and improving physical wellbeing; highlighting a wide range of areas for development and thus prevention of maternal morbidity. Maternal morbidity has been conceptualized as including rare, severe, and potentially life-threatening obstetric complications, but less severe health problems are highly prevalent and meaningful to childbearing women [56]. Further, as evidence suggests, even when the processes of pregnancy and childbirth are normal, maternal functional health is affected [57].
The analysis revealed numerous examples of supportive care interventions which were undertaken by a range of perinatal clinicians that were designed to address risk factors and thus decrease perinatal morbidity. Three major considerations were noted. Firstly, the capacity of learning through practice with ‘skills-based' or ‘physical' interventions: the effects of exercise were noted in a number of study domains that achieved large effect and reached statistical significance. The tangible benefits of exercise included improvements in labour and birth outcomes such as self-efficacy, pain and use of analgesia; maternal glucose levels; psychological health and physical health. This result was supported by a review examining the effects of exercise on pregnancy outcome which found that it could limit adverse maternal and fetal morbidities and provide reduction of maternal weight gain during pregnancy and improvement in cardiovascular fitness [58]. This shows that opportunities to "learn through doing" in active practice can be valuable. When individuals engage in tasks, they are learning through practice, as they construe and construct the capacities to undertake the activities and interactions arising from what they experience [59]. The mechanism of positive effect for physical exercise-based studies [60] could also be interpreted as being successful due to the timing of initiation, i.e., beginning at the start of pregnancy. Other prominent features of studies illustrating significant results included those with tailored programs which accommodate individual flexibility, as well as those with suitably qualified and constantly supervised programs (e.g. obstetricians and sport science professionals and/or allied health teams).
Secondly, many of the successful interventions consisted of dual-application, in that they involved instruction, either in a group educational setting or by distributed educational material, followed up with individual consultation/s. Other reviews in comparable fields support these findings. Using the example of depression in adults, evidence indicates that while purely self-guided Web-based interventions benefit depressed individuals, effect sizes are enhanced when online programs are facilitated by a live coach [61]. To some extent this also supports the principle of adult learning theory which proposes that adults have well-differentiated learning styles which should be accommodated by multiple learning strategies [62]. Perhaps most importantly, it is the authors' opinion that participants, regardless of intervention target, need to be proficiently educated on the rationale of the program objectives. If a woman understands the putative benefits of the targeted outcomes, she may be more motivated to initiate participation and adhere to the intervention.
Finally, social support is considered to play a contemporaneous, positive role in the identified interventions. Participants may indirectly acquire social benefit from participating in a group setting [63]. Future research could examine the broader perspective of the types of positive outcomes for parents and their infant, beyond the clinical realms, e.g. social capital [64].
Strengths and limitations
Although this review explored a very broad topic scope, this provides an evidence-based for a series of robust (but more focused) systematic review [65]. Additionally, only high-level evidence, i.e. RCTs, were included in the scoping review. This comprehensive synthesis identified interventions that could be implemented antenatally as preventative measures to complement current antenatal midwifery education, individual intervention results should be interpreted with caution as many samples were small which make it difficult to generalize obtained results. A more basic limitation of the current study derives from the use of only two databases (Medline and CINAHL). While both were checked for their well-recognised breadth of coverage, the use of additional more maternity-focused databases may well have yielded additional research studies.
While the broad range of international literature included in this scoping review illustrates promise for future service provision, the cross-cultural nature of the study populations was not taken into consideration. Competence to act according to one's cultural and situational context (e.g. traditional practices) means that it is possible that not all interventions and/or results could be transferable across all ethnicities. For example, confinement following birth for Chinese women may impact on their ability to adhere to interventions conducted postnatally (as Chinese women are expected to remain indoors and follow a complex set of rules), and thus this can impact the extensiveness and delivery of antenatal interventions to ensure the needs of women are met. To enhance the mechanism of intervention effect, interventions may work best if tailored to local circumstances rather than being completely standardized, particularly when there are several interacting components [66].
Further, the inconsistent follow-up periods across the studies constitutes a limitation, as does the lack of any economic analysis of particular interventions; there is broad consensus that cost-effectiveness analysis and cost-benefit analysis are necessary to inform resource allocation decisions [67]. Despite this, a number of interventions were highlighted that warrant further consideration. It may also be useful to consider whether such interventions that may be viewed as preventative interventions actually reduce the incidence, or only delay the onset of negative outcomes such as depression. Given the follow up period in most studies did not go beyond the postpartum phase, it cannot be concluded that incidence was actually prevented among all variables in the long term.
Perhaps another limitation of the current review, is the varying outcome measures which reduce accurate transference of the research results to clinical practice and service delivery. For example, in measuring depression, more than one scale was applied across the intervention studies, i.e. Centre for Epidemiological Studies Depression scale (CES-D) and Edinburgh Postnatal Depression Scale (EPDS).
In applying the contemporary approach of calculating effect size across the reviewed set of studies, not all demonstrated large effects. Despite this, small effects can still deliver practical benefits. Using the example of childbirth, if it could be shown that in making a small and inexpensive change to antenatal educational practices would increase the rates of normal birth by an effect size of even as little as 0.1, then this could be a useful, meaningful improvement [23]; particularly if the improvement applied to all childbearing women, and even more so if the effect were cumulative over time. Discussion relating to the potential importance of small effects has been previously reported in the existing literature, in that small effects may have enormous implication in a practical context, and small effects in ongoing processes may accumulate over time to become large effects [26,68].
Interpretation
Awareness of risk factors that predispose to adverse outcomes, in addition to preparatory approaches as identified throughout this review, can guide policy, midwifery practices and education. In light of this scoping review, one can identify strategies of favorable outcomes that may not only provide direct benefit to childbearing women (clinically and economically), but may also decrease the burden placed on the health care system. As evidence suggests, there are correlations between health issues and if we modify one risk factor, it can lead to further health benefit. As noted in earlier literature, women with perinatal depression have been shown to suffer more frequently from diabetes mellitus and gestational diabetes [69]. Further, women with adverse perinatal outcomes [70] have been shown to suffer more frequently from postpartum depression. If universal, multidisciplinary evidence-based interventions can be implemented into routine antenatal midwifery care, there is potential to modify behavior and/or prevent known risk factors that threaten perinatal outcomes. For example, exercise during pregnancy can evidently improve the level of maternal glucose tolerance - and this may be viewed as a protective factor for gestational diabetes [35], as well as other pregnancy associated health risks and pregnancy complications linked with gestational diabetes, including fetal overgrowth and thus shoulder dystocia [71].
Many of the identified interventions could be produced cost effectively in group settings (e.g. yoga, structured exercise training), and implemented into existing midwifery education practice. The use of groups as a mode of service delivery is well supported by the findings of Scott, et al. (2001) [72]. Group dynamics are thought to provide several benefits, while there are many factors that enable group members to change behaviors as a result of facilitated group interaction, including receiving and offering of support and advice and interpersonal learning [73]. Beyond this, groups may also increase social networks, facilitating the development of ongoing support groups outside of the immediate health service. In addition to this, it is our opinion that participating in a social and collegial environment with other pregnant women could also generate an important level of adherence to programs. Identification and initiation of support in the antenatal period could further generate ongoing informal social and professional connections (including informational resources) that may not otherwise be established in the postnatal period when a woman is adjusting to the demands of early parenthood. Thus, identification of any potential difficulties may be managed early and reduce adverse perinatal biopsychosocial health outcomes.
As discussed by earlier researchers, universal approaches in health care are most beneficial, in that the alternate pathway of targeting services for a small number high-risk people will have little impact on the total burden of ill health and social problems in a population [74]. Consistent with the current research, The National Health and Hospitals Reform Commission Report [75] further recommends an integrated strategy for the health system to nurture a healthy start to life for all Australian children and that services should focus on health promotion and prevention in the form of an early ‘progressive universalism' approach (p.20).
Conclusion
There are many interventions delivered in the antenatal period which appear promising, as outlined above. These bear further investigation as the many differences in content, reporting, outcome measures and implementation of engagement make it challenging to undertake systematic comparisons. Additionally, a lack of commonly-agreed evaluation time-points constrains our ability to say that the current evidence accurately supports any particular intervention over another.
Nevertheless, this scoping review was a first step by the authors towards the enhancement of maternity service care and provision in the antenatal period. The exploratory study shows where further development and research into perinatal health practice and service delivery may be warranted, while several diverse intervention compositions were identified. The next step forward is to develop parameters around each identified intervention to identify clinical guidelines (e.g. number of sessions, individual or group consultations and time points for delivery) to maximise perinatal health outcomes. Further, a combination of both quantitative and qualitative measures are important. Not all research studies report non-participation or reasons for drop out and this is important as good patient compliance is important for interventions to be effective.
Finally, this scoping review not only indirectly highlights the diversity of perinatal morbidity, but also the invaluable potential of multidisciplinary health practitioners in the care of childbearing women. Collectively, the ultimate step forward is to design and evaluate a robust multidisciplinary health promotion intervention combining several strategies and components (e.g. yoga, education, exercise) to address protective factors and modifiable risk components, as well as evaluate cumulative effect and cost benefit. Results from such a study would make a valuable contribution to the quality of health service managers' decision making regarding where to invest in order to optimize perinatal health outcomes [76,77].
References
-
Darvill R, Skirton H, Farrand P (2010) Psychological factors that impact on women's experiences of first-time motherhood: a qualitative study of the transition. Midwifery 26: 357-366.
-
Nelson AM (2003) Transition to motherhood. J ObstetGynecol Neonatal Nurs 32: 465-477.
-
Nicolson P (1998) Post-natal Depression: Psychology, Science and Transition to Motherhood. London: Routledge.
-
Buultjens M, Murphy G, Robinson P, Milgrom J (2013) The perinatal period: A literature review from the biopsychosocial perspective. Clinical Nursing Studies 1: 19.
-
Fenwick J, Butt J, Dhaliwal S, Hauck Y, Schmied V (2010) Western Australian women's perceptions of the style and quality of midwifery postnatal care in hospital and at home. Women Birth 23: 10-21.
-
Brown SJ, Yelland JS, Sutherland GA, Baghurst PA, Robinson JS (2011) Stressful life events, social health issues and low birthweight in an Australian population-based birth cohort: challenges and opportunities in antenatal care. BMC Public Health 11: 196.
-
Whitworth M, Dowswell T (2009) Routine pre-pregnancy health promotion for improving pregnancy outcomes. Cochrane Database Syst Rev, CD007536.
-
Malouf R, Redshaw M, Kurinczuk JJ, Gray R (2014) Systematic review of heath care interventions to improve outcomes for women with disability and their family during pregnancy, birth and postnatal period. BMC Pregnancy Childbirth 14: 58
-
Dodd JM, Grivell RM, Crowther CA, Robinson JS (2010) Antenatal interventions for overweight or obese pregnant women: a systematic review of randomised trials. BJOG 117: 1316-1326.
-
Dennis CL, McQueen K (2009) The relationship between infant-feeding outcomes and postpartum depression: a qualitative systematic review. Pediatrics 123: e736-751.
-
Rollins NC, Bhandari N, Hajeebhoy N, Horton S, Lutter CK, et al. (2016) Why invest, and what it will take to improve breastfeeding practices? Lancet 387: 491-504.
-
Victora CG, Bahl R, Barros AJ, França GV, Horton S, et al. (2016) Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet 387: 475-490.
-
Beyondblue (2012) Valuing perinatal health: The consequences of not treating perinatal depression and anxiety.
-
Madeleine M (Writer) (2014) Perinatal depression estimated to cost $535 million a year if left untreated: report ABC News Australia.
-
Cuijpers P, van Straten A, Smit F, Mihalopoulos C, Beekman A (2008) Preventing the onset of depressive disorders: a meta-analytic review of psychological interventions. Am J Psychiatry 165: 1272-1280.
-
Lassi ZS, Haider BA, Bhutta ZA (2010) Community-based intervention packages for reducing maternal and neonatal morbidity and mortality and improving neonatal outcomes. Cochrane Database Syst Rev 11.
-
Arksey H, O'Malley L (2005) Scoping studies: towards a methodological framework. International journal of social research methodology 8: 19-32.
-
Ehrich K, Freeman GK, Richards SC, Robinson IC, Shepperd S (2002) How to do a scoping exercise: continuity of care. Research Policy and Planning 20: 25-29.
-
Schlosser RW, Wendt O, Sigafoos J (2007) Not all systematic reviews are created equal: Considerations for appraisal. Evidence-Based Communication Assessment and Intervention 1: 138-150.
-
Meade MO, Richardson WS (1997) Selecting and appraising studies for a systematic review. Ann Intern Med 127: 531-537.
-
Mrazek PJ, Haggerty RJ (1994) Reducing risk for mental disorders: Frontiers for preventative intervention research. Washington DC: National Academy Press.
-
Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJM, et al. (1996) Assessing the quality of reports of randomized clinical trials: is blinding necessary? Controlled clinical trials 17: 1-12.
-
Coe R (2002) It's the Effect Size, Stupid. What effect size is and why it is important Paper presented at the Annual Conference of the British Educational Research Association, University of Exeter, England.
-
Cohen J (1988b) Statistical power analysis for the behavioural sciences, 2nd ed. Hillsdale, NJ: L Erlbaum Associates.
-
Parker RI, Hagan-Burke S (2007) Useful effect size interpretations for single case research. Behav Ther 38: 95-105.
-
Rubin A (2012) Statistics for evidence-based practice and evaluation: Cengage Learning.
-
Chang MY, Wang SY, Chen CH (2002) Effects of massage on pain and anxiety during labour: a randomized controlled trial in Taiwan. J Adv Nurs 38: 68-73.
-
Chuntharapat S, Petpichetchian W, Hatthakit U (2008) Yoga during pregnancy: Effects on maternal comfort, labor pain and birth outcomes. Complement Ther Clin Pract 14: 105-115.
-
Gau ML, Chang CY, Tian SH, Lin KC (2011) Effects of birth ball exercise on pain and self-efficacy during childbirth: a randomised controlled trial in Taiwan. Midwifery 27: e293-300.
-
Gedde-Dahl M, Fors EA (2012) Impact of self-administered relaxation and guided imagery techniques during final trimester and birth. Complementary Therapies in Clinical Practice 18: 60-65.
-
Ip WY, Tang CS, Goggins WB (2009) An educational intervention to improve women's ability to cope with childbirth. J Clin Nurs 18: 2125-2135.
-
Campbell DA, Lake MF, Falk M, Backstrand JR (2006) A randomized control trial of continuous support in labor by a lay doula. J Obstet Gynecol Neonatal Nurs 35: 456-464.
-
Salvesen KA, Mørkved S (2004) Randomised controlled trial of pelvic floor muscle training during pregnancy. BMJ 329: 378-380.
-
Svensson J, Barclay L, Cooke M (2009) Randomised-controlled trial of two antenatal education programmes. Midwifery 25: 114-125.
-
Barakat R, Pelaez M, Lopez C, Montejo R, Coteron J (2012) Exercise during pregnancy reduces the rate of cesarean and instrumental deliveries: results of a randomized controlled trial. J Matern Fetal Neonatal Med 25: 2372-2376.
-
Jareethum R, Titapant V, Chantra T, Sommai V, Chuenwattana P, et al. (2008) Satisfaction of healthy pregnant women receiving short message service via mobile phone for prenatal support: A randomized controlled trial. J Med Assoc Thai 91: 458-463
-
Yuenyong S, O'Brien B, Jirapeet V (2012) Effects of labor support from close female relative on labor and maternal satisfaction in a Thai setting. J Obstet Gynecol Neonatal Nurs 41: 45-56.
-
Chang MY, Chen CH, Huang KF (2008) Effects of music therapy on psychological health of women during pregnancy. J Clin Nurs 17: 2580-2587.
-
Guse T, Wissing M, Hartman W (2006)The effect of a prenatal hypnotherapeutic programme on postnatal maternal psychological well-being. Journal of Reproductive and Infant Psychology 24: 163-177.
-
Robledo-Colonia AF, Sandoval-Restrepo N, Mosquera-Valderrama YF, Escobar-Hurtado C, Ramírez-Vélez R (2012). Aerobic exercise training during pregnancy reduces depressive symptoms in nulliparous women: a randomised trial. Journal of Physiotherapy 58: 9-15.
-
Songøygard KM, Stafne SN, Evensen KA, Salvesen KÅ, Vik T, et al. (2012) Does exercise during pregnancy prevent postnatal depression? A randomized controlled trial. Acta Obstet Gynecol Scand 91: 62-67.
-
Satyapriya M, Nagendra HR, Nagarathna R, Padmalatha V (2009) Effect of integrated yoga on stress and heart rate variability in pregnant women. Int J Gynaecol Obstet 104: 218-222.
-
Rakhshani A, Maharana S, Raghuram N, Nagendra HR, Venkatram P (2010) Effects of integrated yoga on quality of life and interpersonal relationship of pregnant women. Qual Life Res 19: 1447-1455.
-
Urech C, Fink NS, Hoesli I, Wilhelm FH, Bitzer J, et al. (2010) Effects of relaxation on psychobiological wellbeing during pregnancy: a randomized controlled trial. Psychoneuroendocrinology 35: 1348-1355.
-
Stafne SN, Salvesen KÅ, Romundstad PR, Eggebø TM, Carlsen SM, et al. (2012) Regular Exercise During Pregnancy to Prevent Gestational Diabetes: A Randomized Controlled Trial. Obstet Gynecol 119: 29-36.
-
Eggen M, Stuge B, Mowinckel P, Jensen K, Hagen K (2012) Can supervised Group Exercise Including Ergonomic Advice Reduce the Prevalence and Severity of Low Back Pain and Pelvic Girdle Pain in Pregnancy? A Randomized Controlled Trial. Phys Ther 92: 781-790.
-
Stafne SN, Salvesen KÅ, Romundstad PR, Stuge B, MØRkved S (2012) Does regular exercise during pregnancy influence lumbopelvic pain? A randomized controlled trial. Acta Obstet Gynecol Scand 91: 552-559.
-
Bø K, Haakstad LA (2011) Is pelvic floor muscle training effective when taught in a general fitness class in pregnancy? A randomised controlled trial. Physiotherapy 97: 190-195.
-
Mason L, Roe B, Wong H, Davies J, Bamber J (2010)The role of antenatal pelvic floor muscle exercises in prevention of postpartum stress incontinence: a randomised controlled trial. J Clin Nurs 19: 2777-2786.
-
Morkved S, Bo K, Schei B, Salvesen KA (2003) Pelvic floor muscle training during pregnancy to prevent urinary incontinence: a single-blind randomized controlled trial. Obstet Gynecol 101: 313-319.
-
Stafne SN, Salvesen K, Romundstad PR, Torjusen IH, Mørkved S (2012)Does regular exercise including pelvic floor muscle training prevent urinary and anal incontinence during pregnancy? A randomised controlled trial. BJOG 119: 1270-1280.
-
Hawkins AJ, Fawcett EB, Carroll JS, Gilliland TT (2006) The marriage moments program for couples transitioning to parenthood: divergent conclusions from formative and outcome evaluation data. J Fam Psychol 20: 561-570.
-
Forster D, McLachlan H, Lumley J, Beanland C, Waldenström U, et al. (2004) Two mid-pregnancy interventions to increase the initiation and duration of breastfeeding: a randomized controlled trial. Birth 31: 176-182.
-
Kronborg H, Maimburg RD, Væth M (2012) Antenatal training to improve breast feeding: a randomised trial. Midwifery 28: 784-790.
-
Mattar CN, Chong YS, Chan YS, Chew A, Tan P, et al. (2007) Simple antenatal preparation to improve breastfeeding practice: a randomized controlled trial. Obstet Gynecol 109: 73-80.
-
Ansara D, Cohen MM, Gallop R, Kung R, Schei B (2005) Predictors of women's physical health problems after childbirth. J Psychosom Obstet Gynaeco l26: 115-125.
-
Webb DA, Bloch JR, Coyne JC, Chung EK, Bennett IM, et al. (2008) Postpartum physical symptoms in new mothers: their relationship to functional limitations and emotional well-being. Birth 35: 179-187.
-
Gavard JA, Artal R (2008) Effect of exercise on pregnancy outcome. Clin Obstet Gyneco l51: 467-480.
-
Valsiner J (2000) Culture and human development: Sage.
-
Barakat R, Cordero Y, Coteron J, Luaces M, Montejo R (2012) Exercise during pregnancy improves matenal glucose screen at 24 - 28 weeks: a randomised controlled trial. Br J Sports Med 46: 656 - 661.
-
Mohr DC, Cuijpers P, Lehman K (2011) Supportive accountability: a model for providing human support to enhance adherence to eHealth interventions. J Med Internet Res 13: e30.
-
Knowles MS, Holton III EF, Swanson RA (2012) The adult learner: Routledge.
-
Weiss JA, Viecili MA, Sloman L,Lunsky Y (2013) Direct and Indirect Psychosocial Outcomes for Children with Autism Spectrum Disorder and their Parents Following a Parent-involved Social Skills Group Intervention. J Can Acad Child Adolesc Psychiatry 22: 303-309.
-
Schultz J, Corman H, Noonan K, Reichman NE (2009) Effects of child health on parents' social capital. Soc Sci Med 69: 76-84.
-
Armstrong R, Hall BJ, Doyle J, Waters E (2011) Cochrane Update. 'Scoping the scope' of a cochrane review. J Public Health (Oxf) 33: 147-150.
-
Craig P, Dieppe P, Macintyre S, Michie S, Nazareth I, et al. (2008) Developing and evaluating complex interventions: the new Medical Research Council guidance. BMJ 337: a1655.
-
Drummond M, Weatherly H, Ferguson B (2008) Economic evaluation of health interventions. BMJ 337: a1204.
-
Prentice DA, Miller DT (1992) When small effects are impressive. Psychological bulletin 112: 160-164.
-
Bansil P, Kuklina EV, Meikle SF, Posner SF, Kourtis AP, et al. (2010) Maternal and fetal outcomes among women with depression. J Womens Health (Larchmt) 19: 329-334.
-
Barbadoro P, Cotichelli G, Chiatti C, Simonetti ML, Marigliano A, et al. (2012) Socio-economic determinants and self-reported depressive symptoms during postpartum period. Women Health 52: 352-368.
-
Landon MB, Gabbe SG (2011) Gestational diabetes mellitus. Obstet Gynecol 118: 1379-1393.
-
Scott D, Brady S, Glynn P (2001) New mother groups as a social network intervention: consumer and maternal and child health nurse perspectives. Aust J Adv Nurs 18: 23-29.
-
Novick G (2004) CenteringPregnancy and the current state of prenatal care. J Midwifery Womens Health 49: 405-411.
-
Rose G (2008) Rose's strategy of preventive medicine: the complete original text (Vol. 1): Oxford University Press.
-
National Health and Hospitals Reform Commission (2009) A healthier future for all Australians: final report.
-
Lorgelly PK, Lawson KD, Fenwick EAL, Briggs AH (2010) Outcome Measurement in Economic Evaluations of Public Health Interventions: a Role for the Capability Approach? Int J Environ Res Public Health 7: 2274-2289.
-
Mihalopoulos C, Vos T, Pirkis J, Carter R (2011) The economic analysis of prevention in mental health programs. Annu Rev Clin Psychol 7: 169-201.