Journal of Otolaryngology and Rhinology
A Rare Clinical Presentation of a Somewhat Common Lesion
Steve Manzon1, Malcolm Zola1*, Jared S Weiner2, Rawle F Philbert3, Kevin R. Torske4, Donald B MacDougall5, and Daniel Nadeau6
1Department of Dentistry and Oral & Maxillofacial Surgery, Attending Oral & Maxillofacial Surgeon, Lincoln Medical Center, 234 East 149th St, The Bronx, NY 10451, USA
2Department of Dentistry and Oral & Maxillofacial Surgery, Chief Resident, Lincoln Medical Health Center, 234 East 149th St, The Bronx, NY 10451, USA
3Department of Dentistry and Oral & Maxillofacial Surgery, Director, Lincoln Medical Center, 234 East 149th St, The Bronx, NY 10451, USA
4Department of Pathology, Naval Medical Center, Portsmouth, 620 John Paul Jones Circle, Portsmouth, VA 23708, USA
5Department of Pathology and Laboratory Medicine, Newport Hospital, 11 Friendship St., Hazard Bldg-Third floor, Newport RI 02840, USA
6Private Practice limited to Otolaryngology, 845 North Main Street, Providence, RI, USA
*Corresponding author:
Malcolm Zola, Attending Oral & Maxillofacial Surgeon, Department of Dentistry and Oral & Maxillofacial Surgery, Lincoln Medical Center, 234 East 149th Street, The Bronx, New York City, NY, Assistant Professor of Clinical Surgery Weill Cornell Medical College, (Dentistry, Oral & Maxillofacial Surgery), Tel: 718-579-5682, 203-767-6091, Fax: 718-579-4781, E-mail: Malcolm.Zola@nychhc.org, mbzola@optonline.net
J Otolaryngol Rhinol,
JOR-1-006, (Volume 1, Issue 1),
Case Report
Received: August 29, 2015: Accepted: September 16, 2015: Published: September 18, 2015
Citation: Manzon S, Zola M, Weiner JS, Philbert RF, Torske KR, et al. (2015) A Rare Clinical Presentation of a Somewhat Common Lesion. J Otolaryngol Rhinol 1:006
Copyright: © 2015 Manzon S. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Clinicians are often faced with diagnosing routine oral and maxillofacial pathology. Experience and training make such tasks relatively easy. Establishing differential diagnoses, and ruling out the most unlikely, usually will lead to an appropriate treatment plan. Occasionally, a pathologic presentation may significantly differ from the expected [1], and stump even an experienced clinician. It is imperative, when encountering an unknown or unusual lesion, to return to basics and approach the entity with the same systematic work-up approach we were trained to perform since entering residency training programs [2].
Case Report
A sixty year old Caucasian woman, wife of a retired United States Navy Master Chief, originally presented to the Ear, Nose and Throat clinic at Groton Naval Station for evaluation of what appeared to be a "huge lesion of my tongue." The patient reported the lesion had been slowly growing for the past year; however, "fear of cancer" overrode her normal inclination to present for treatment.
She denied recent weight loss or constitutional symptoms, such as fevers, chills or night sweats. Past medical history was significant for hypertension, which was well controlled with beta blockers. She denied tobacco and alcohol use. Chest x-ray was normal, and peripheral blood laboratory values were all within normal limits. She had no previous surgeries except dental extractions.
Clinical Presentation
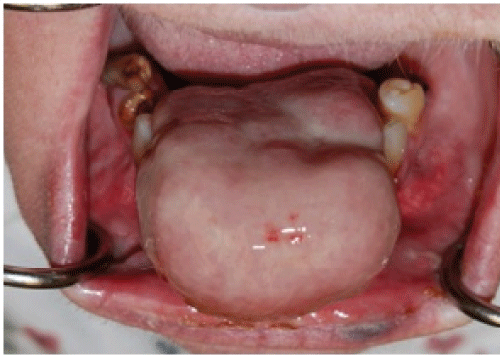
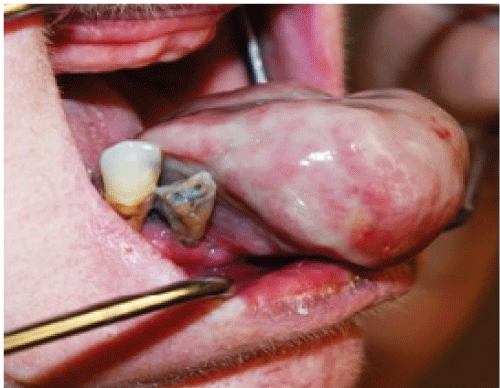
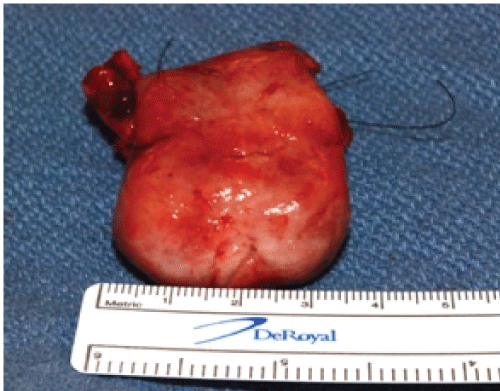
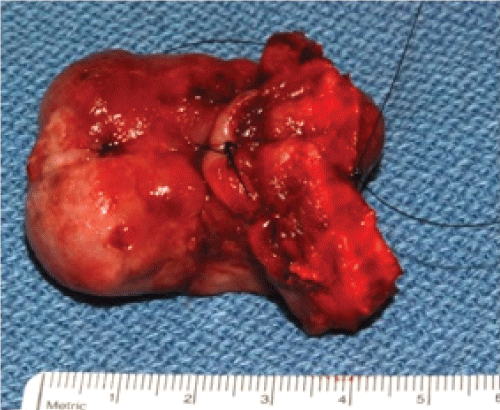
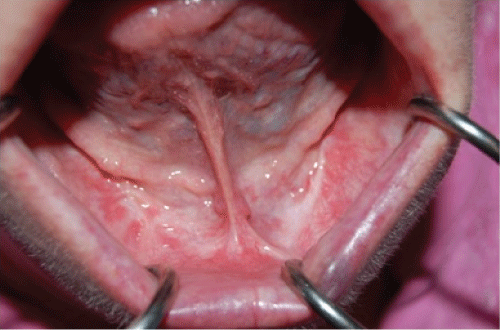
On physical exam the patient appeared as a heavy set woman of stated age. Head and neck exam revealed a large purplish lesion of approximately 5 cm. in diameter attached to the anterior portion of the mandibular alveolus, which protruded dramatically from the oral cavity upon forward motion of the tongue. (Figure 1 and Figure 2) The lesion was firm, fibrous, non-tender and non-ulcerated, positioned adjacent to remaining grossly carious and periodontally involved mandibular teeth. It was soon apparent that the tongue was freely mobile and not at all involved. Airway was patent; neck was supple with no palpable lymphadenopathy.
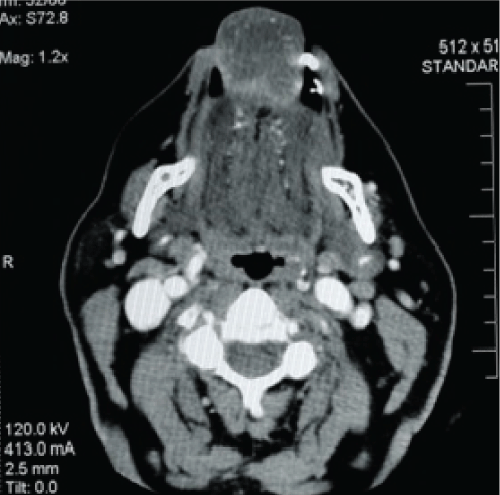
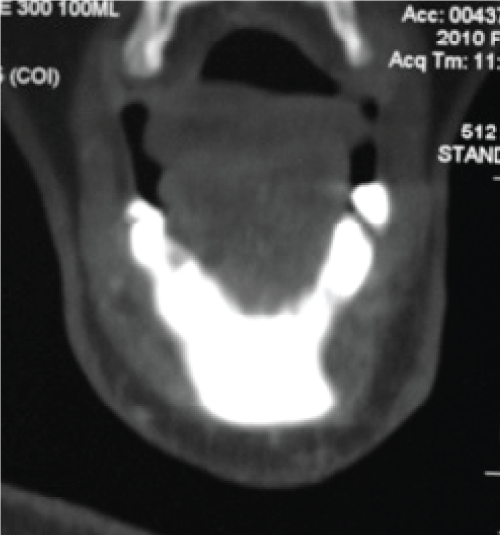
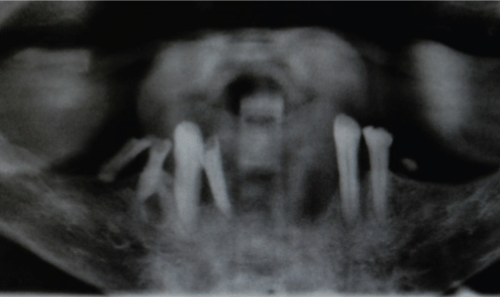
Panoramic x-ray revealed marked alveolar resorption associated with the overlying mass (Figure 3). CT scan further confirmed intimate relationship of the lesion to the mandibular alveolus. The mandible, however, appeared grossly intact without intrabony masses or lesions (Figure 4 and Figure 5).
.
Figure 3: Panoramic x-ray showing poor periodontal condition of teeth, and anterior spacing.
View Figure 3
Differential Diagnoses
Benign-appearing exophytic masses on the gingiva include pyogenic granuloma, peripheral odontogenic fibroma, peripheral ossifying fibroma, peripheral giant cell granuloma [3], peripheral ameloblastoma and of course primary vs. secondary malignancy.
With no history of previous malignancy, a metastatic lesion could be most likely ruled out, while a primary malignancy of the gingiva in the midline is very unusual.
The peripheral ameloblastoma is rare and usually presents as a sessile red mass in the posterior mandibular alveolar mucosa with little or no bony erosion [4,5].
Distinguishing the other four entities -- pyogenic granuloma, peripheral odontogenic fibroma, peripheral ossifying fibroma and peripheral giant cell granuloma -- from each other clinically is problematical (Table 1).
![]()
Table 1: Comparison of clinical and microscopic findings of the four entities most likely to be listed in the differential diagnosis of the lesion.
View Table 1
Color varies from pale to red [6] for each - in various stages of development [7]. The earlier the life of the lesion, the redder the apparent color will be. Pain [5] may not be a presenting factor, unless ulceration secondary to local or occlusal trauma occurs - and then pain may be present in any or all.
The ages of appearance of each of the lesions overlap considerably: "child bearing age," "age of pregnancies," "adolescence","mean age of occurrence 30," "50% of cases between ages 5 - 25," [4,5,8,9] making it difficult to rule in or rule out a diagnosis based on age - especially if, as in our case, the lesion is of long standing (and may have been present even longer than the patient described).
Pathogenesis of each seem to be intertwined; the pyogenic granuloma with a histologic appearance of heavily vascularized fibrous connective tissue seems to be an early stage of each of the other entities, and cross over in descriptive terminology between the four is almost interchangeable exept for differences in inclusion into the fibrous stroma of odontogenic epithelium, multinucleated giant cells, osteoid, or calcification [10].
Clinical Course
With no clear-cut diagnosis, incisional biopsy was carried out.
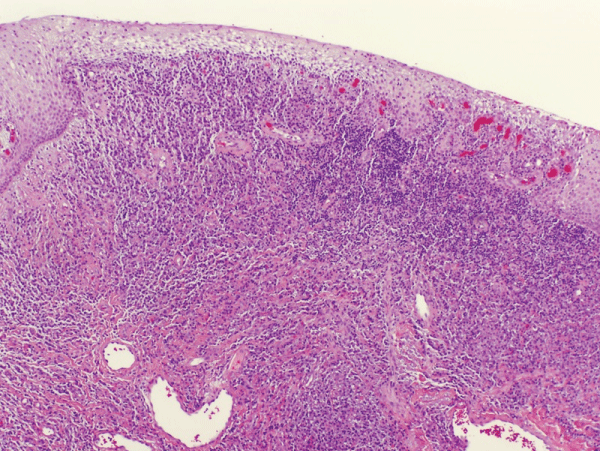
Incisional biopsy was performed in the mid portion of the lesion. Results were inconclusive. The staff general pathologist could only identify connective tissue pattern without being able to identify the histologic diagnosis of such lesion. A second opinion was sought. The lesion was re-biopsied under conscious sedation and 5mm diameter cores were obtained from the lesion in the area adjacent to the alveolus. The specimen was submitted to Department of Oral Pathology, National Naval Medical Center (NNMC), Bethesda. Once again the diagnosis was not clearly established due to significant inflammatory infiltrate and non-specific fibrous tissue. (Figure 6 and Figure 7) The Oral Pathologist did note, however, spindle cell proliferation - altered by myxoid degeneration and chronic inflammation (Figure 8) - which could be consistent with extra abdominal desmoid tumor or fibromatosis any growing mass will have a ring of fibrosis that looks like scar tissue and has features of a desmoid. Thus it is sometimes unclear whether a mass biopsied was inadequately biopsied (i.e., the fibrous ring surrounding the mass, not the mass itself, was taken) or is in fact a desmoid. Therefore, since malignancy was not apparent, recommendation was made to excise the lesion in entirety for thorough microscopic examination.
.
Figure 6: Photomicrograph - Incisional biopsy: dense chronic inflammation (H & E Stain; low power).
View Figure 6
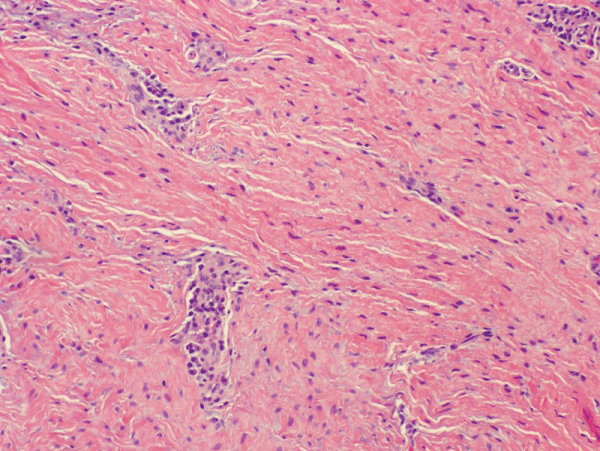
.
Figure 7: Photomicrograph - Incisional biopsy: Fibrous component (H & E Stain; medium power).
View Figure 7
The patient subsequently was taken to the operating room at Newport Hospital where the lesion (Figure 9) was excised under general anesthesia with a generous soft tissue margin. The tumor was found to be well adherent to crestal portion of the mandible, so 0.5 cm of the alveolar bone was excised with the soft tissue mass. 3 mm. of residual soft tissue were also excised and sent out for verification of free margins, the five remaining mandibular teeth were extracted and the wound closed in layered fashion.
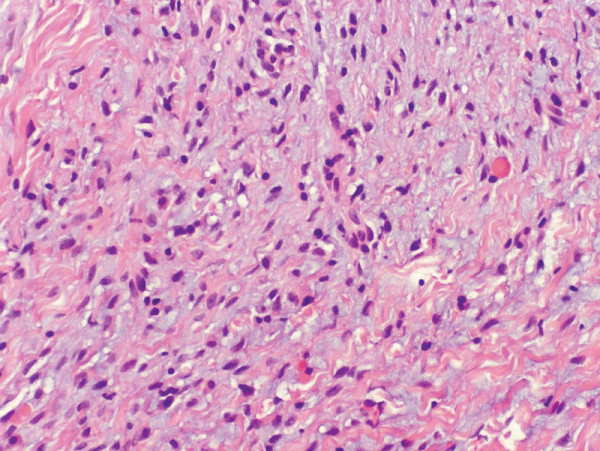
.
Figure 8: Photomicrograph - Incisional biopsy: Fibrous tissue, spindle cells, inflammation & myxoid degeneration
(H & E Stain; high power).
View Figure 8
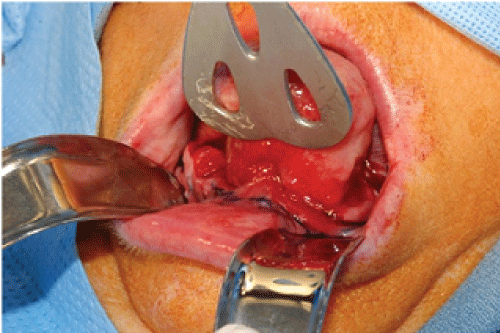
.
Figure 9: Clinical view prior to excision showing attachment of the lesion to the alveolar gingival.
View Figure 9
The lesion, measuring approximately 3x5 cm. (Figure 10 and Figure 11), was submitted for general pathology examination at Newport hospital and slides mailed out for second opinion to a soft tissue pathologist expert at Emory University.
Finally, after some deliberation, diagnosis was established and confirmed by NNMC specialists. Recovery was uneventful and the patient was discharged home on the following day. The healing process was unremarkable and at one year follow up no recurrence was noted (Figure 12).
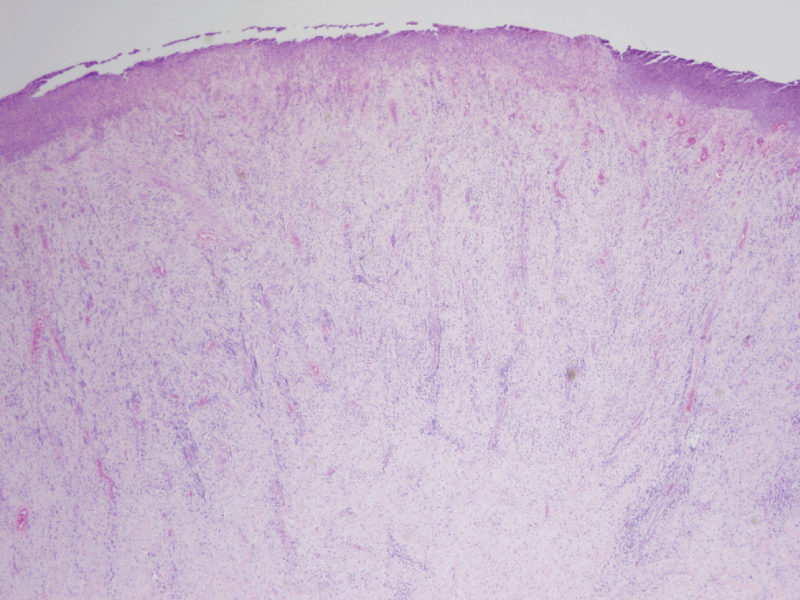
.
Figure 13: Photomicrograph - Excised specimen: Ulcerated and inflamed mass composed primarily of fibrous connective tissue. (H & E Stain; medium power).
View Figure 13
Microscopic examination of the excisional biopsy is presented.
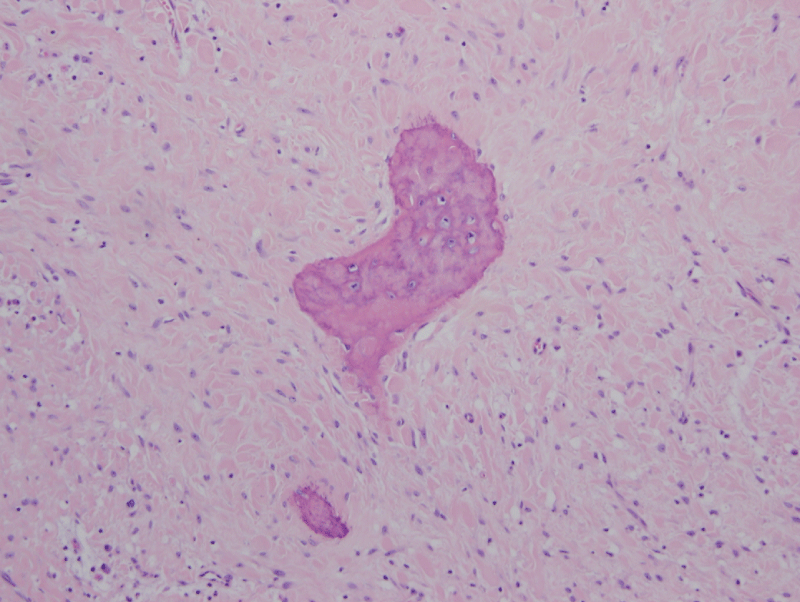
.
Figure 14: Photomicrographs - Excised specimen: Fibrous connective tissue with multiple, scattered osseous
Calcifications composed primarily of woven bone. Focal lamellar bone also observed. (H & E Stain; high power).
View Figure 14
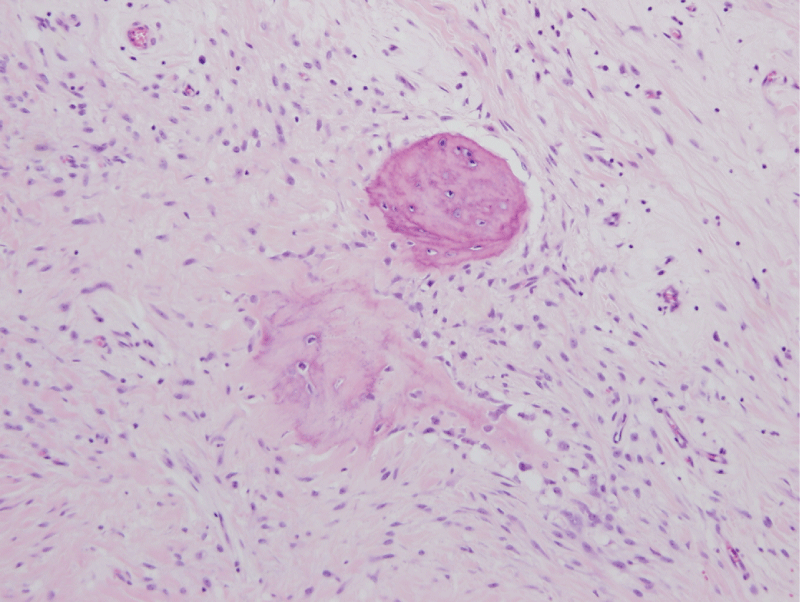
.
Figure 15: Photomicrographs - Excised specimen: Fibrous connective tissue with multiple, scattered osseous
Calcifications composed primarily of woven bone. Focal lamellar bone also observed. (H & E Stain; high power).
View Figure 15
The final diagnosis by the reporting pathologist was 'Peripheral Ossifying Fibroma'.
Discussion
Peripheral ossifying fibromas aka "bump on the gum" are very common benign tumors. They are considered to be reactive lesions rather than neoplastic [11], arising secondarily to irritation by plaque micro-organisms and other irritants such as calculus within the gingival crevice [12]. The peripheral ossifying fibroma more often than not is noted to have a mineralized component [13], which most likely originates from the periosteum or periodontal ligament, and may be merely a pyogenic granuloma that has undergone maturation and calcification. These lesions are found more often in females than in males [4]. They arise more commonly in the maxilla than - as in this case - the mandible.
The peripheral ossifying fibroma, pedunculated or sessile, appears exclusively on the gingiva, with peak prevalence stated in the literature to be between 10 and 19 years of age [8]. Most of these lesions originate and extend from the interdental papilla [14]. Most lesions are small, usually less than 2 cm. in size, but some believe these lesions have the potential to grow into "gigantiform" size. Routine oral examinations allow for early detection of these lesions, hypothesized to be one of the reasons for the usual small size of this entity. Our patient delayed presenting for evaluation due to fear. We postulate that the larger size of this lesions is secondary not only to the delayed presentation but also to the edentulous aspect of the anterior mandible, where the lesion had unopposed growth restriction.
Conclusion
We have presented a rare clinical manifestation of a somewhat common lesion, and its diagnostic and surgical management. The training of a surgeon is long, tedious, demanding and varied. Included is training in surgical skills, patient management, operating room techniques, historical perspective of the specialty; in all, a common thread exists. The resident is taught to think; think of what he proposes; think of differential diagnoses; think of possible complications; think of the handling of tissues; think of the patient; think of his colleagues and their possible contribution to the care of his patients.
As part of this thinking process, the resident is taught to evaluate the diagnosis and care of lesions of the head and neck. It is this aspect of his/her training that will permit, in an orderly fashion, the diagnosis and recommended treatment of usual, but more importantly, unusual lesions which their patient may present to them [1,2]. Not always do the clinical, radiographic and pathologic evaluations coincide. Those guidelines taught during residency permit the practitioner to formulate treatment plans that result in appropriate, timely care for his patient.
Acknowledgement
The authors wish to express their gratitude to:
Sharon Weiss, MD, Director, Expert Consultation Service in Anatomic Pathology, Professor of Pathology, Emory University Hospital H180, Atlanta, GA 30322, Tel: 404-712-0708 For her expertise and help in finalizing the micro-pathological diagnosis for this interesting case.
References
-
Sacks HG, Amrani S, Anderson K (2012) Gigantiform Periferal Ossifying fibroma. J Oral Maxillofac Surg 70: 2610-2613.
-
Carlson ER, Sims PG (2012) AAOMS Parameters of Care. J Oral Maxillofac Surg 70.
-
Trasad VA, Devarsa GM, Subba Reddy VV, Shashikiran ND (2011) Peripheral ossifying fibroma in the maxillary arch. J Indian Soc Pedod Prev Dent 29: 255-259.
-
Kerpel, Freedman, Reich (2008) A comprehensive review course in oral pathology.
-
Regezi, Sciubba (1989) Oral pathology; clinical-pathologic correlations. W.B Saunders 187-88.
-
Bhaskar (1961) Synopsis of Oral Pathology. C V Mosby.
-
Poonacha KS, Shigli AL, Shirol D (2010) Peripheral ossifying fibroma: A clinical report. Contemp Clin Dent 1: 54-56.
-
Mishra MB, Bhishen KA, Mishra S (2011) Peripheral ossifying fibroma. J Oral Maxillofac Pathol 15: 65-68.
-
Jaffe (1958) Tumors and tumerous conditions of the Bones and Joints. Lea & Febiger, Philadelphia, Pa.
-
Chatterjee A, Ajmera N, Singh A (2010) Peripheral cemento-ossifying fibroma of maxilla. J Indian Soc Periodontol 14: 186-189.
-
Yadav R, Gulati A (2009) Peripheral ossifying fibroma: a case report. J Oral Sci 51: 151-154.
-
Kolte AP, Kolte RA, Shrirao TS (2010) Focal fibrous overgrowths: a case series and review of literature. Contemp Clin Dent 1: 271-274.
-
Neville, Damm, Allen, Bouquot Oral and Maxillofacial Pathology. 521-523.
-
Kumar SK, Ram S, Jorgensen MG, Shuler CF, Sedghizadeh PP (2006) Multicentric peripheral ossifying fibroma. J Oral Sci 48: 239-243.