Journal of Otolaryngology and Rhinology
Killian-Jamieson Diverticulum: A Case Report and Argument for Transcervical Diverticulectomy
Susannah Orzell1*, Todd Falcone2 and Gregory Grillone3
1Department of Otolaryngology, SUNY Upstate Medical Center, USA
2Division of Otolaryngology, University of Connecticut School of Medicine, USA
3Department of Otolaryngology, Boston University School of Medicine, USA
*Corresponding author:
Susannah Orzell, MD, MPH, Department of Otolaryngology, SUNY Upstate Medical University, 750 East Adams St, Syracuse, NY, 13202, USA, Tel: (315) 464-4636, Fax: (315) 464-7282, E-mail: goulds@upstate.edu
J Otolaryngol Rhinol, JOR-2-025, (Volume 2, Issue 4), Clinical Study
Received: May 29, 2016; Accepted: October 03, 2016; Published: October 05, 2016
Citation: Orzell S, Falcone T, Grillone G (2016) Killian-Jamieson Diverticulum: A Case Report and Argument for Transcervical Diverticulectomy. J Otolaryngol Rhinol 2:025.
Copyright: © 2016 Orzell S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Killian-Jamieson Diverticulum (KJD) is a rare type of cervical esophageal diverticulum. It originates inferior to the cricopharyngeal muscle and lateral to the longitudinal muscle of the esophagus, and is closely associated with the recurrent laryngeal nerve (RLN). We report a case of KJD in a 78-year-old man treated with an open diverticulectomy with a nerve integrity monitor (NIM), and present a comprehensive literature review. Our case supports the intimate relationship of the RLN to a KJD, and therefore we recommend open diverticulectomy with the use of a NIM as the treatment of choice for KJD to minimize risk of injury to the RLN.
Keywords
Killian jamieson diverticulum, Lateral cervical esophageal diverticulum, Dysphagia, Globus sensation
Introduction
Killian-Jamieson Diverticulum (KJD) is a rare type of esophageal diverticulum with uncertain pathophysiology. It originates inferior to the cricopharyngeal muscle and lateral to the longitudinal muscle of the cervical esophagus [1]. This area of weakness, referred to as the Killian-Jamieson space, contains penetrating branches of the recurrent laryngeal nerve (RLN) [2,3]. Like Zenker's diverticulum (ZD), KJDs are believed to be pulsion diverticula that are acquired due to a combination of age related changes on the musculature of the esophagus and swallowing dysfunction. The observation that KJDs are seen almost exclusively in middle age or elderly patients supports this claim [4]. KJD is often asymptomatic [4], but can be associated with symptoms similar to ZD, including dysphagia, cough, and regurgitation. Other less common symptoms have been described as well, including foreign body entrapment [5] or cervical cellulitis [6]. Diagnosis of KJD is based on radiographic evaluation, specifically CT scan and barium esophagography. Differentiation from the more common ZD is based on the findings of a diverticulum in the lateral wall of the esophagus approximately 2 cm below the upper esophageal sphincter without an obstructing cricopharyngeal bar [4,7]. Treatment has traditionally consisted of an open diverticulectomy with or without esophagomyotomy [6,8-11], however, there have been recent reports of KJDs successfully repaired with endoscopic methods [7,12]. We present a case of a symptomatic KJD that demonstrates the utility of an open excision and the potential dangers of endoscopic repair with regard to the RLN, and report the findings of a literature review.
Case Report
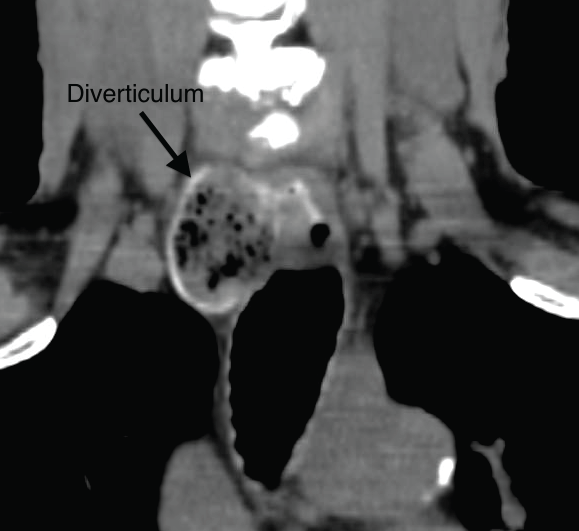
A 78-year-old male presented to an outpatient clinic with a history of persistent dysphagia, globus sensation, cough during deglutition, gastro-esophageal reflux disease (GERD) and occasional regurgitation. His physical exam, including fiberoptic laryngoscopy, was normal but a barium esophogram and subsequent Computed Tomography (CT) scan demonstrated a right-sided esophageal diverticulum inferior to the cricopharyngeus and anterolateral to the esophagus, consistent with a Killian-Jamieson Diverticulum (KJD) (Figure 1). The patient was then taken to the operating room for definitive open diverticulectomy given the concern for the potential intimate relationship between the recurrent laryngeal nerve (RLN) and the diverticulum. Following induction of general anesthesia with insertion of a NIM endotracheal tube (Medtronic), a Weerda diverticuloscope was introduced to visualize the diverticulum, which was found to be distal to the cricopharyngeus muscle and projecting anterolaterally to the patient's right, thus confirming the diagnosis of KJD. A cervical rigid esophagoscopy was performed. The pouch was fully impacted with food debris (Figure 2). Following disimpaction and irrigation, an orogastric tube was used to cannulate the esophagus and strip gauze was packed into the pouch to aid in identification of the sack once the neck was opened. A right-sided horizontal neck incision was used to expose the diverticulum, which measured 3.5 cm in length. The RLN was found to be adherent to the medial neck of the diverticulum (Figure 3), and was carefully dissected away prior to excision of the pouch with an Endo GIA articulating stapler. A myotomy of the circular muscle fibers immediately inferior to the diverticulum was also performed. The incision was closed in layers and a small penrose drain was left in situ and removed on postoperative day 1. A follow up gastrograffin swallow study on post-operative day 5 demonstrated an intact staple line and the patient was started on a liquid diet. He was advanced to a soft diet and discharged on postoperative day 6.
.
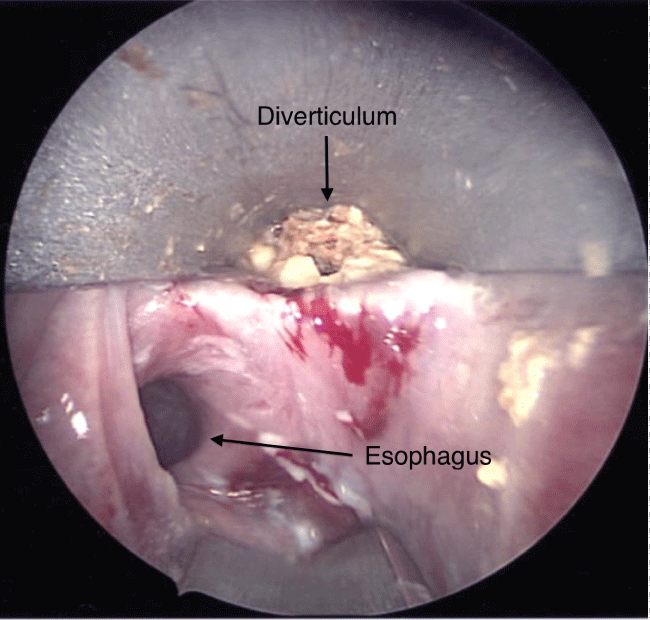
Figure 2: Esophagoscopy showing a right-sided cervical diverticulum with food impaction anterior and lateral to the esophagus.
View Figure 2
Discussion
Many comparisons have been made between ZD and KJD due to the fact they have similar symptoms, more often occur in the elderly, and are believed to have similar etiologies. An association between GERD and ZD has been previously described [8], and although an association between KJD and GERD has not yet been demonstrated, there are case reports relating the presence of KJDs with heartburn [8] and erosive gastritis [13]. The subject in our case report had poorly controlled GERD, further supporting a possible association. Hypotheses for the association of ZD with GERD include longitudinal muscle contraction leading to separation of muscle fibers in an area of weakness [15] and inappropriate contraction of the upper esophageal sphincter during swallowing [16]. A significant number of patients are asymptomatic and diverticula are found during workups for presumed thyroid nodules or other neck masses (Table 1). The belief that a significant number of patients with ZD are asymptomatic has lead to theories proposing a functional, and not just structural, component of the pathology, which may also be true for KJD [4,17]. Unlike ZD, which affects males slightly more than females, KJDs reported in the literature are most often found in middle-aged women followed by elderly men. Interestingly, while KJDs are typically larger in men they are less often symptomatic in males when compared to their female counterparts (Table 1).
.
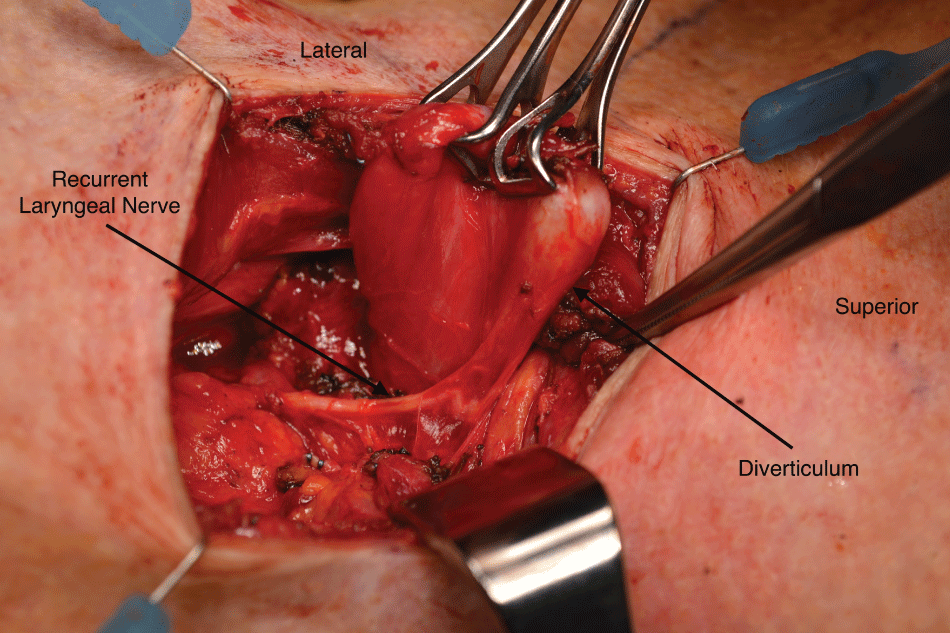
Figure 3: Intra-operative photo showing the recurrent laryngeal nerve coursing along the neck of the diverticulum.
View Figure 3
![]()
Table 1: Characteristics of KJD in published reports.
View Table 1
While the majority of KJDs described in the literature are left-sided and unilateral, a small number of variances have been described in the literature, including bilateral KJDs [4,11,19], and 2 KJDs occurring on the same side [1]. Right-sided KJDs, like the one seen in our case, are exceedingly rare, and approximately half of subjects in the literature with a right-sided KJD also had a left sided KJD. The disproportionate number of right-sided KJDs may be in part due to the differences in anatomy between the left and right neck. In particular, the more lateral location of the carotid artery on the left may result in an area of relatively low resistance compared to the right. Data on the anatomical relationship of the RLN to the KJD is limited to a few reports, but studies that do describe the location, including this case report, note that the KJD projects posterolaterally to the RLN [6,8,31].
The majority of symptomatic KJD described in the literature were treated with open excision with or without esophagomyotomy [9,11,14]. This is largely due to the close relationship of the RLN, the relative rarity of KJD's, and the amount of transoral manipulation required for endoscopic repair. In recent years however, successful cases of endoscopic repair have been reported without serious adverse effects [7,12]. Both Lee, et al. and Tang, et al. performed endoscopic distal vertical diverticulotomies (DVD) to disrupt the circular muscle of the esophagus inferior to the diverticulum to widen the opening and allow for drainage of its contents into the esophagus. Both studies reported resolution of symptoms in their subjects at their post-operative clinic visits and had no serious adverse outcomes.
Endoscopic repair for ZD has been enormously successful, and has become the preferred method of treatment for ZD over the past decade. Although associated with a greater rate of recurrence, it is also associated with decreased operative times, hospital length of stay, rate of major complications, and time to oral intake [32]. Overall, the low incidence of adverse events while still achieving significant symptom resolution highlight it's utility, particularly for high-risk patients. Although the results of the studies by Lee and Tang appear encouraging for the future of endoscopic repair for KJD, significant questions regarding the protection of the RLN during diverticulotomy were not answered by these studies. Attempting endoscopic repair in patients with KJD puts the RLN at high risk of injury since it does not currently provide visualization of the RLN and does not allow for gentle dissection away from the diverticulum. The studies on endoscopic repair acknowledge the possibility of RLN transection, but neither offers much direction on how to avoid this major complication [7,12]. Tang, et al. do encourage avoiding lateral diverticulotomies to avoid the RLN [7], however during this case, the RLN was observed to course over the medial aspect of the KJD. The proximity of the RLN to the diverticulumnot only puts it at risk of transection, but also potentially put it at risk for thermal injury if electrocautery devices are used [33,34]. Additionally, current methods do not reliably assess individual RLN monitoring during endoscopic repair. In addition to direct visualization of the RLN, the judicious use of the NIM during this case helped confirm the location of the right RLN and its branches, and helped guide the dissection and stapling of the diverticulum. As demonstrated in this case as well as several other cases of KJD repaired with open diverticulectomy, the RLN is closely associated with the neck of the diverticulum and may need gentle dissection prior to excision of the diverticulum [9].
Conclusion
This case of a symptomatic KJD intimately associated with the RLN illustrates the importance of performing an open diverticulectomy. Although endoscopic repair of ZD has likely surpassed open diverticulectomy as a preferred method of repair, it should not become standard of care for KJD. Attempting endoscopic repair in patients with KJD puts the RLN at high risk of injury since it does not provide visualization or monitoring of the RLN and does not allow for dissection away from the diverticulum. We therefore recommend open diverticulectomy with intraoperative RLN monitoring as the treatment of choice for KJD.
The authors of this manuscript have no financial disclosures, conflicts of interest or sources of funding to disclose.
References
-
Ekberg O, Wahlgren L (1985) Dysfunction of pharyngeal swallowing. A cineradiographic investigation in 854 dysphagia patients. Acta Radiol Diagn (Stockh) 26: 389-395.
-
Killian G (1908) Über den Mund der Speiseröhre. Zeitschrift für Ohrenheilkunde 55: 1-44.
-
Jamieson EB (1934) Illustrations of regional anatomy Edinburgh: E&S Livingstone Ltd 44.
-
Rubesin SE, Levine MS (2001) Killian-Jamieson diverticula: radiographic findings in 16 patients. AJR Am J Roentgenol 177: 85-89.
-
Jung WS, Cho JH (2014) Incidentally Found Killian-Jamieson Diverticulum Due to an Embedded Fishbone. J Craniofac Surg.
-
Kitazawa M, Koide N, Saito H, Kamimura S, Uehara T, et al. (2010) Killian-Jamieson diverticulitis with cervical cellulitis: report of a case. Surg Today 40: 257-261.
-
Tang SJ, Tang L, Chen E, Myers LL (2008) Flexible endoscopic Killian-Jamieson diverticulotomy and literature review. Gastrointest Endosc 68: 790-793.
-
Siow SL, Mahendran HA, Hardin M (2015) Transcervical diverticulectomy for Killian–Jamieson diverticulum. Asian J Surg.
-
Undavia S, Anand SM, Jacobson AS (2013) Killian-Jamieson Diverticulum: A case for open transcervical excision. Laryngoscope 123: 414-417.
-
Chea CH, Siow SL, Khor TW, Nik Azim NA (2011) Killian-Jamieson diverticu- lum: the rarer cervical esophageal diverticulum. Med J Malaysia 66: 73-74.
-
Boisvert RD, Bethune DC, Acton D, Klassen DR (2010) Bilateral Killian-Jamieson diverticula: a case report and literature review. Can J Gastroenterol 24: 173-174.
-
Lee CK, Chung IK, Park JY, Lee TH, Park SH, et al. (2008) Endoscopic diverticulotomy with an isolated-tip needle-knife papillotome (Iso-Tome) and a fitted overtube for the treatment of a Killian-Jamieson diverticulum. World J Gastroenterol 14: 6589-6592.
-
Resouly A, Braat J, Jackson A, Evans H (1994) Pharyngeal pouch: link with reflux and oesophageal dysmotility. Clin Otolaryngol Allied Sci 19: 241-242.
-
Kim DC, Hwang JJ, Lee WS, Lee SA, Kim YH, et al. (2012) Surgical treatment of Killian-Jamieson Diverticulum. Korean J Thorac Cardiovasc Surg 45: 272-274.
-
Sasaki CT, Ross DA, Hundal J (2003) Association between Zenker diverticulum and gastroesophageal reflux disease: development of a working hypothesis. Am J Med 115: 169S-171S.
-
Veenker E, Cohen JI (2003) Current trends in management of Zenker diverticulum. Curr Opin Otolaryngol Head Neck Surg 11: 160-165.
-
Siddiq MA, Sood S, Strachan D (2001) Pharyngeal pouch (Zenker's diverticulum). Postgrad Med J 77: 506-511.
-
Kim Th, Kim S, Chang KS (2015) Simple method of using soda for distinguishing Killian-Jamieson diverticulum from a thyroid nodule. Endocrine 48: 351-352.
-
Kim HK, Lee JI, Jang HW, Bae SY, Lee JH, et al. (2012) Characteristics of Killian-Jamieson diverticula mimicking a thyroid nodule. Head Neck 34: 599-603.
-
Udare A, Mondel P, Badhe P (2014) Killian-Jamieson diverticulum. Indian Journal of Gastroenterology 33: 98-98.
-
Lee F, Leung CH, Huang WC, Cheng SP (2012) Killian-Jamieson diverticulum masquerading as a thyroid mass. Intern Med 51: 1141-1142.
-
Mimatsu K, Oida T, Kano H, Kawasaki A, Fukino N, et al. (2013) Killian-Jamieson Diverticula Presenting Synchronously with Thyroid Adenoma. Case Rep Gastroenterol 7: 188-194.
-
Kim MH, Kim EK, Kwak JY, Kim MJ, Moon HJ (2010) Bilateral Killian-Jamieson diverticula incidentally found on thyroid ultrasonography. Thyroid 20: 1041-1042.
-
Pang JC, Chong S, Na H, Kim YS, Park SJ, et al. (2009) Killian-Jamieson diverticulum mimicking a suspicious thyroid nodule: Sonographic diagnosis. Journal of Clinical Ultrasound 37: 528-530.
-
Mercer D, Blachear A, Khafif A, Weiss J, Kessler A (2005) Real-time sonography of Killian-Jamieson diverticulum and its differentiation from thyroid nodules. J Ultrasound Med 24: 557-560.
-
Rekhtman N, Rekhtman K, Sheth S, Ali SZ (2005) A 62-year-old woman with a suspected thyroid nodule. Arch Pathol Lab Med 129: 1497-1498.
-
O'Rourke A, Weinberger PM, Postma GN (2012) Killian-Jamieson diverticulum. Ear, nose and throat journal 91: 196.
-
Huang YC, Chen JW, Chang CH (2013) Is It Really a Thyroid Nodule? Gastroenterology 145: 726-913.
-
Yang CW, Yen Hh, Choo Ch (2013) Hematemesis in a Man With Longstanding Esophageal Globus Sensation. Gastroenterology 144: e11-e12.
-
Donnellan F, Al-Qarshoubi IS, Kortan PP (2010) A Rare Cause of Food Bolus Obstruction. Gastroenterology 139: e7-e8.
-
Rodgers PJ, Armstrong WB, Dana E (2000) Killian-Jamieson diverticulum: a case report and review of the literature. Ann Otol Rhinol Laryngol 109: 1087-1091.
-
Koch M, Mantsopoulos K, Velegrakis S, Iro H, Zenk J (2011) Endoscopic laser-assisted diverticulotomy versus open surgical approach in the treatment of Zenker's diverticulum. Laryngoscope 121: 2090-2094.
-
Beriat GK, Akmansu SH, Ezerarslan H, Dogan C, Han U, et al. (2012) The comparison of thermal tissue injuries caused by ultrasonicscalpel and electrocautery use in rabbit tongue tissue. Bosn J Basic Med Sci 12: 151-157.
-
Lin YC, Dionigi G, Randolph GW, Lu IC, Chang PY, et al. (2015) Electrophysiologic monitoring correlates of recurrent laryngeal nerve heat thermal injury in a porcine model. Laryngoscope 125: E283-E290.