Obstetrics and Gynaecology Cases - Reviews
Iatrogenic Myometrial Defect Following Fetoscopic Laser Therapy for Twin-Twin Transfusion Syndrome (TTTS)
Stephanie L Cooper1*, Sean Spence1, David Somerset1, Rory Windrim2 and Greg Ryan2
1Department of Obstetrics and Gynaecology, University of Calgary, Calgary, Canada
2Fetal Medicine Unit, Mount Sinai Hospital, University of Toronto, Toronto, Canada
*Corresponding author: Stephanie L Cooper, Department of Obstetrics and Gynaecology, University of Calgary, Calgary, Canada, E-mail: Stephanie.cooper3@albertahealthservices.ca
Obstet Gynecol Cases Rev, OGCR-3-069, (Volume 3, Issue 1), Case Report; ISSN: 2377-9004
Received: August 22, 2015 | Accepted: January 19, 2016 | Published: January 23, 2016
Citation: Cooper SL, Spence S, Somerset D, Windrim R, Ryan G (2016) Iatrogenic Myometrial Defect Following Fetoscopic Laser Therapy for Twin-Twin Transfusion Syndrome (TTTS). Obstet Gynecol Cases Rev 3:069. 10.23937/2377-9004/1410069
Copyright: © 2016 Cooper SL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Monochorionic twin pregnancies have significantly increased risk of fetal loss, perinatal mortality and morbidity compared to dichorionic twin and singleton gestations [1]. Twin to twin transfusion syndrome (TTTS) occurs in 10-15% of these twins, and is the most important cause of mortality [2]. Fetoscopic laser coagulation of selective vascular anastomosis of the monochorionic placenta is associated with the best outcomes for mid trimester TTTS [3]. Nonetheless, the risk of adverse pregnancy outcomes remains significant following treatment, and the pregnancy is monitored closely until delivery. This case represents an unusual sonographic finding and rare complication following fetoscopic laser coagulation for TTTS.
Keywords
Monochorionic twins, Twin-twin transfusion syndrome (TTTS), Fetoscopic laser coagulation
Introduction
A 33-year-old G2 P1 patient with a monochorionic diamniotic twin pregnancy was noted to have an amniotic fluid volume (AFV) discrepancy and nuchal translucency (NT) discordance on ultrasound (US) at 13+0 weeks gestation. The patient had no significant medical or surgical history and, specifically, no previous uterine surgery. One year previously, she had delivered her first child vaginally at 41 weeks gestation, after an uncomplicated pregnancy.
US at 15+3 weeks showed no evidence of growth discordance, but persistence of the AFV discrepancy, with a maximal vertical pocket (MVP) of 6.3 cm around twin A and 2.0 cm around twin B, whose bladder did not fill throughout the US. All Doppler studies (umbilical and middle cerebral arteries and ductus venosus) were normal and there were no hydropic changes. Stage II Twin-Twin Transfusion Syndrome (TTTS) was diagnosed and the patient was referred to the main fetal therapy program in Canada.
By 16+6 weeks, there was anhydramnios around the donor twin (B) whose bladder persistently remained empty and the deepest pool of amniotic fluid around the recipient was 9.4 cm. All Doppler's were normal and the placenta was anterior. The patient underwent fetoscopic laser ablation of the placental anastomosis at 16+6 weeks gestation. The trochar was inserted directly transamniotically without incident under continuous US guidance, taking care to avoid traversing the placenta or any maternal vessels. A 12F sheath (Cook Medical, Bloomington, IN, USA) and a 2 mm fetoscope were used (Storz GmbH, Tüttlingen, Germany). A total of 9 anastomosis were ablated using a diode laser (Dornier MedTech, Kennesaw, GA, USA) at a setting of 30W, aided by an US guided amnioinfusion of1, 900 mL followed by an amnioreduction of 1,100 mL, for an overall positive balance 800 mL. The deepest amniotic fluid pocket the recipient was 6 cm at the end of the procedure, which was 51 minutes in duration, with the laser portion lasting 18 mins. The surgery was well tolerated by the patient and was felt to be free of any complications by the surgical teams. The team was also confident that a septostomy had not occurred.
An US on post-operative day (POD) 1 showed a small amount of membrane separation in the upper right fundal area (close to the trochar insertion site), and a "simple right ovarian cyst" (5 × 2 cm) with a small amount of maternal ascites. The MVP for the recipient was 1.9 cm and was still unmeasureable around the donor. Both fetuses were healthy and some fluid accumulation was noted around the donor twin. The MVP for the donor twin was 0.8 cm. An US on POD 2 noted less membrane separation, and all Doppler waveforms were normal in both twins. The MVP for the recipient was 1.9 cm and 1.7 for the donor and both bladders were of a normal size. The patient denied any abdominal pain or fluid leakage per vagina. After one week, she returned to her referring institution for ongoing pregnancy care and US surveillance.
At 18+5 weeks, US demonstrated normal anatomy and Doppler studies for both fetuses. However, the recipient twin (A) who previously had polyhydramnios, was noted to have subjectively reduced amniotic fluid, although a 2.2 cm pocket could still be measured. The donor amniotic fluid pocket measured 1.5 cm.
There was also a new finding: a large hypoechoic cystic lesion (9.8 × 3.4 × 1.1 cm) adjacent to the uterus, lying between the fundus and the right lobe of the liver. This was separate and 'very different' from a previously identified right ovarian cyst that had pre-dated the pregnancy. The impression on imaging was of an extra-uterine collection of amniotic fluid trapped underneath the peritoneum. It was felt by the fetal surgeon that if such a collection was secondary to fluid leakage post-fetoscopy, it should disperse within a short time. An alternate explanation could be the incidental finding of an adnexal mass unrelated to the procedure.
At 19+3 weeks, both fetuses were noted to have oligohydramnios. The recipient twin (A) had a MVP of 1.4 cm, but its bladder was filling and emptying appropriately. The donor twin (B) had a MVP of 1.5 cm and also had a normal bladder size. The cystic area superior to the right uterine fundus had enlarged and remained well circumscribed (10 × 6.5 × 5.6 cm). By 21+5 weeks, this cyst had enlarged to 19 × 50 × 13 cm.
Magnetic Resonance Imaging (MRI) at 20.5 weeks reported no definite tract or extension of fluid collection relating to either the uterus or abdominal wall. The cyst was described as "thin walled with scant dependent debris".
At 23+3 weeks, the amniotic fluid volume had normalized around both twins. At 26+3 wks, MVP's for both fetuses were 4 cm and the abdominal cyst remained unchanged. However, at this time the myometrium immediately adjacent to the cystic lesion was noted to be strikingly thin, measuring only 1 mm.
The option of a premature Caesarean section in light of the uterine thinning was discussed with the patient. A plan was formulated to continue with weekly US monitoring until the pregnancy was more advanced.
Follow-up US's at 31+3, 32+3 and 33+3 weeks showed appropriate interval growth of both twins, all Doppler's remained normal and there were no signs of recurrence of TTTS or the development of TAPS. The cystic fluid collection remained stable in size, and the adjacent myometrium did increase slightly in thickness to 4-6 mm.
Healthy male infants were delivered by elective caesarean section at 33+5 weeks, due to concerns of preterm labour in the setting of a possible uterine fundal defect. Both twins were delivered intact without incident.
The cystic mass was determined to an amniotic fluid-containing sac exterior to the uterus (Figure 1) that had herniated through the original fetoscopic entry site. The sac had torted on its pedicle as it penetrated the uterine wall (Figure 2), thereby explaining why the cystic mass had remained relatively stable in size since it was first identified. This could also explain why there was transient oligohydramnios around the recipient twin (A), despite normal fetal urination, as an amniotic fluid sac had herniated through the defect (Figure 3). After extensive torsion (Figure 4), this mass was no longer in continuity with the amniotic cavity and amniotic fluid was thus able to reaccumulate around twin A.
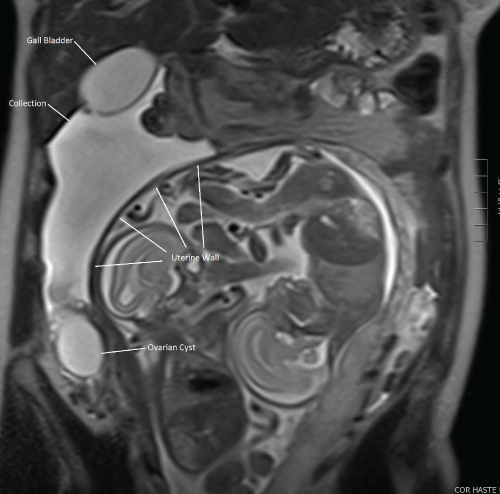
.
Figure 1: MRI of extrauterine cystic mass, described as thin walled with scant dependent debris.
View Figure 1
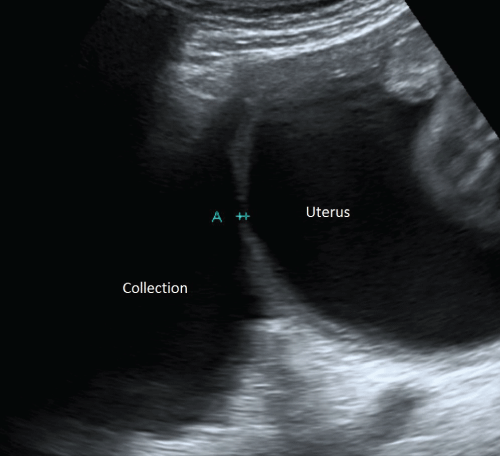
.
Figure 2: Extrauterine cystic mass observed on ultrasound at 26 weeks gestation following prior laser coagulation of TTTS with additional finding of myometrial thinning.
View Figure 2
The twins were transferred to the neonatal intensive care (NICU). The recipient had some significant respiratory concerns, and the attending NICU team felt that there might have been an element of pulmonary hypoplasia clinically. It was postulated that oligohydramnios due to leakage into the defect at a critical stage of pulmonary development might have contributed.
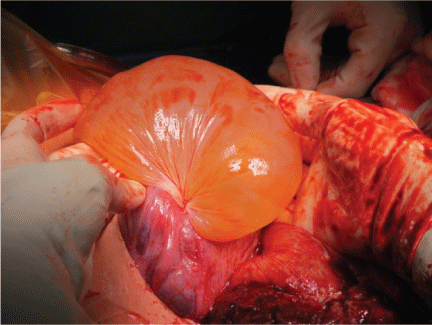
.
Figure 3: Finding at Cesarean Section: Fluid-containing sac demonstrating herniation through the port site created at the time of laser anastomotic ablation.
View Figure 3
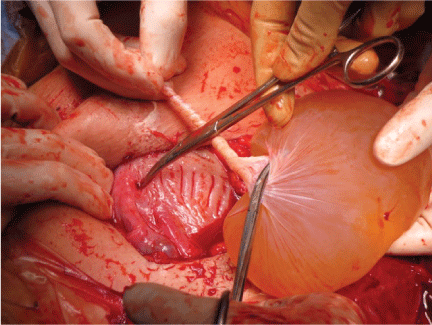
.
Figure 4: Finding at Cesarean Section: Amniotic sac of recipient twin had torted on a pedicle penetrating through the uterine wall.
View Figure 4
This is a very rare previously unrecognized complication of fetoscopy. And should be considered whenever a "new" cystic lesion is noted after fetoscopy. Its presence should impact on the fetal monitoring and timing of elective delivery.
References
-
Lewi L, Van Schoubroeck D, Gratacos E, Witters I, Timmerman D, et al. (2003) Monochorionic diamniotic twins: complications and management options. Curr Opin Obstet Gynecol 15: 177-194.
-
Acosta-Rojas R, Becker J, Munoz-Abellana B, Ruiz C, Carreras E, et al. (2007) Twin chorionicity and the risk of adverse perinatal outcome. Int J Gynaecol Obstet 96: 98-102.
-
Rossi AC, D'Addario V (2008) Laser therapy and serial amnioreduction as treatment for twin-twin transfusion syndrome: a metaanalysis and review of literature. Am J Obstet Gynecol 198: 147-152.





