Obstetrics and Gynaecology Cases - Reviews
McLeod Ob/Gyn Dillon, South Carolina 29536, USA
*Corresponding author: Iacob Marcovici, FACOG, Assistant Professor of Ob/Gyn McLeod Health - Dillon Ob/Gyn 705 N, 8th Ave., Suite 3B Dillon, South Carolina 29536, USA, Fax: 843-841-3830, Tel: 843-472-7825, E-mail: DrIMarcovici@Yahoo.com
Obstet Gynecol Cases Rev, OGCR-3-073, (Volume 3, Issue 1), Case Report; ISSN: 2377-9004
Received: April 23, 2015 | Accepted: January 28, 2016 | Published: January 30, 2016
Citation: Marcovici I (2016) Vulvar Abcess due to Actinomyces Meyerii. Obstet Gynecol Cases Rev 3:073. 10.23937/2377-9004/1410073
Copyright: © 2016 Marcovici I. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Vulvar Abscess, Actinomyces meyerii
Introduction
A case of Vulvar Abscess due to Actinomyces meyerii is presented. Actinomyces meyerii-a gram positive rod has not been previously described as causing vulvar abscess.
Case
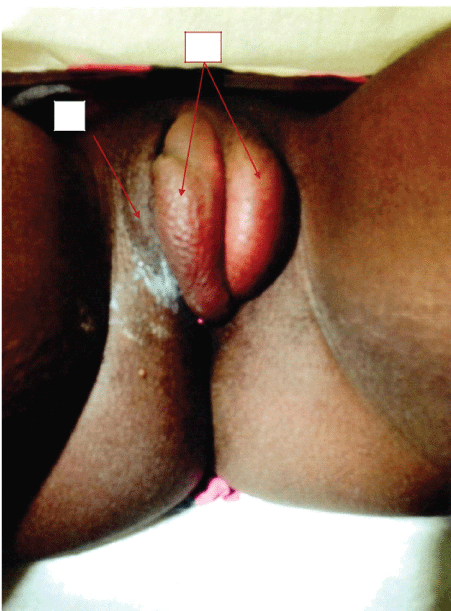
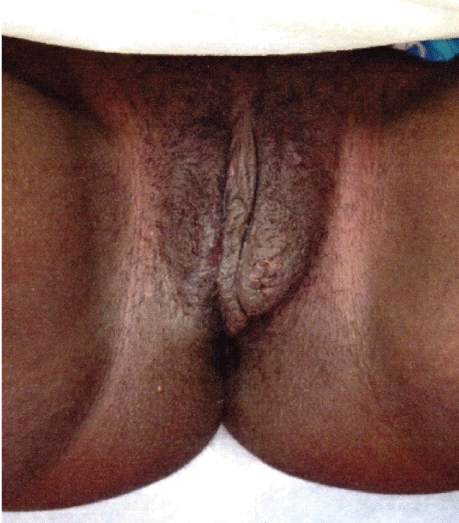
A 14 years old girl presented with vulvar swelling, pain, and difficulty to walk. Her examination showed a tender and large left labial abscess (Figure 1). In OR, the patient underwent incision and drainage. Large amounts of puss were evacuated. Aerobic and anaerobic cultures were obtained. The patient's postoperative recovery was unremarkable and she was discharged on oral Ciprofloxacin 250 mg twice a day and Cephalexin 500 mg twice a day for 7 days. One week later the cultures were positive for Actinomyces meyerii: Infectious disease specialist on consult recommended Amoxicillin 875 mg orally, every 12 hours for at least 4 weeks based upon clinical resolution. Four weeks later patient had complete resolution (Figure 2).
Discussion
Human actinomycosis is a rare infection caused by a gram positive, anaerobic bacterial rod of the genus Actinomyces that is colonizing the mouth, gastrointestinal tract, and vagina in healthy individuals. Some members of the order are: Actinomyces israelii, A. odontolyticus, A. naeslundii, A. meyerii, A. viscosus, Rothia dentocariosa, and Propionibacterium propionicus [1]. The four major types of human actinomycosis are: Cerebral, cervico-facial, thoracic, abdomino-pelvic [2]. The gynecologist is more likely to encounter abdominal and/or pelvic actinomycosis. Weight loss and chronic low-grade fever are symptoms common to all of the different presentations of actinomycosis it is thought to be underdiagnosed due to the indolent nature of the complaints.
The classic symptoms of abdominal actinomycosis are diffuse abdominal pain, nausea, vomiting and diarrhea. Some classical studies have documented genital/pelvic actinomycosis, a rare infection, in women with IUD [3]. Actinomyces israelii was almost exclusively found in those women with IUD or in vaginal pessary users. The pathogenesis of actinomycosis infection starts at the site of disruption of the mucosal barrier. There is penetration of organisms into deeper tissues. Solitary or multiple abscesses develop, with slowly progressive induration, fluctuation, central suppuration, and a fibrotic texture develops that can be easily mistaken for carcinoma. The primary abscess enlarges and develops a fibrotic capsule that, after further growth, breaks down with the formation of sinus tracts.
Vulvar Actinomycosis
It has been rarely described before. McElroy and colleagues described a case of vulvar actinomycosis mimicking a vulvar malignancy [4].
The present report is about Actinomyces meyerii causing a Vulvar Abscess. A search of English literature on the Medline did not produce any additional cases associating actinomyces myerii with vulvar abscess.
References
-
Russo TA (1995) Agents of actinomycosis. In: Mandell GL, Bennett JE, Dolin R (eds) Principles and Practice of Infectious Diseases. (4th ed.), New York, NY: Churchill Livingstone: 2280-2288.
-
Schaal KP, Lee HJ (1992) Actinomycete infections in humans--a review. Gene 115: 201-211.
-
Persson E, Holmberg K, Dahlgren S, Nilsson L (1983) Actinomyces israelii in the genital tract of women with and without intra-uterine contraceptive devices. Acta Obstet Gynecol Scand 62: 563-568.
-
Jennifer Y McElroy, Marsha E Gorens, Lisa N Jackson, Danielle Stigger, Teresa Becker, et al. (2006) Actinomyces israelii May Produce Vulvar Lesions Suspicious for Malignancy. Infect Dis Obstet Gynecol 2006: 48269.