Obstetrics and Gynaecology Cases - Reviews
Breus Mole: A Placental Anomaly in a Patient Undergoing a Dilation and Evacuation
Navdeesh Reiners1*, Victor Sai2, Nagesh Ragavendra2, Aparna Sridhar3 and Angela Chen3
1Department of Obstetrics and Gynecology, Kaiser Permanente Medical Center, Santa Clara, CA, USA
2Department of Radiology, David Geffen School of Medicine, University of California, Los Angeles, CA, USA
3Department of Obstetrics and Gynecology, Division of Family Planning, David Geffen School of Medicine, University of California, Los Angeles, CA, USA
*Corresponding author: Navdeesh Reiners, MD, MPH, Department of Obstetrics and Gynecology, Kaiser Permanente Medical Center, Santa Clara, 710 Lawrence Expressway Department 386 #M3179, CA 95051, USA, Tel: 408-851-3131, E-mail: navdeesh.k.reiners@kp.org
Obstet Gynecol Cases Rev, OGCR-3-093, (Volume 3, Issue 4), Case Report; ISSN: 2377-9004
Received: February 26, 2016 | Accepted: August 04, 2016 | Published: August 06, 2016
Citation: Reiners N, Sai V, Ragavendra N, Sridhar A, Chen A (2016) Breus Mole: A Placental Anomaly in a Patient Undergoing a Dilation and Evacuation. Obstet Gynecol Cases Rev 3:093. 10.23937/2377-9004/1410093
Copyright: © 2016 Reiners N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: A Breus mole, a massive subchorionic hematoma, can be associated with adverse outcomes including bleeding. There are no reports on outcomes in patients with a Breus mole undergoing second trimester surgical abortion.
Case: A 22-year-old woman presented at 21+1 weeks for dilation and evacuation. Sonographic features were consistent with a Breus mole. Intraoperatively, traction and massage were used to deliver the placenta; the patient quickly achieved hemostasis. Final pathology showed a fibrin lined intervillous cystic structure compatible with a Breus mole.
Conclusion: In this case, surgical termination of a pregnancy complicated by a Breus mole proceeded without complications. Maternal blood loss into the hematoma was self-limited and the placenta was removed without difficulty. Caution should be exercised for potential bleeding with a Breus mole.
Keywords
Breus mole, Placental anomaly, Dilation and evacuation
Introduction
A Breus mole is a massive subchorionic tuberous hematoma, first described by Breus in 1892. It is a rare occurrence, with one study suggesting an incidence of 1:1200 placentas [1]. Breus moles are often found in the placenta of demised fetuses, but they have also been reported in the placenta of live-born neonates [2-4]. The hematoma is maternal in origin [5], as shown by DNA molecular analysis [6], and occurs when maternal blood flows into the subchorionic space, separating the villous chorion from the chorionic plate. The etiology of a Breus mole remains unclear, but it can be associated with maternal conditions such as vascular disease including hypertension, heart disease and diabetes [1,7]. A Breus mole can be diagnosed prenatally using imaging techniques such as ultrasound, pulse Doppler imaging and magnetic resonance imaging, but there are reports of the diagnosis being missed during pregnancy and only made after inspection of the placenta at time of delivery [8-10]. A massive Breus mole or one located near the umbilical cord (causing compression of the cord) can be associated with adverse pregnancy outcomes such as spontaneous abortion, intrauterine growth restriction, preterm delivery, placental abruption and intrauterine fetal death due to a disturbance in blood flow to the fetus [5,7,9,11]. Case reports regarding antepartum or postpartum bleeding in patients with a Breus mole vary, with reports of both patients with significant intrapartum bleeding [7] and others without [2].
This is a case report of a Breus mole diagnosed on ultrasound during evaluation for surgical abortion. Review of the literature revealed no case reports on the presence of a Breus mole in a patient undergoing dilation and evacuation (D&E) for surgical abortion and maternal outcome during and after the procedure.
Case
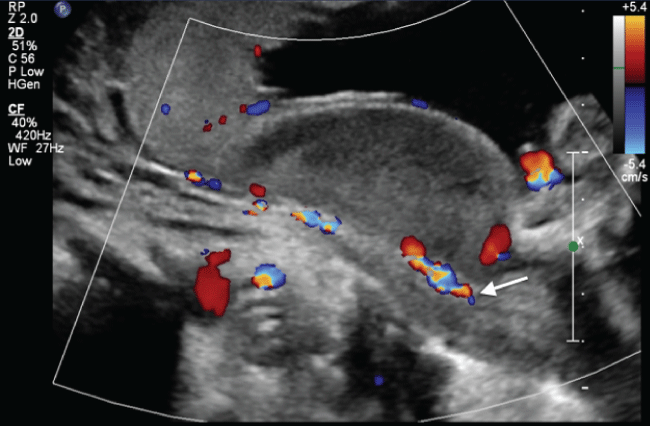
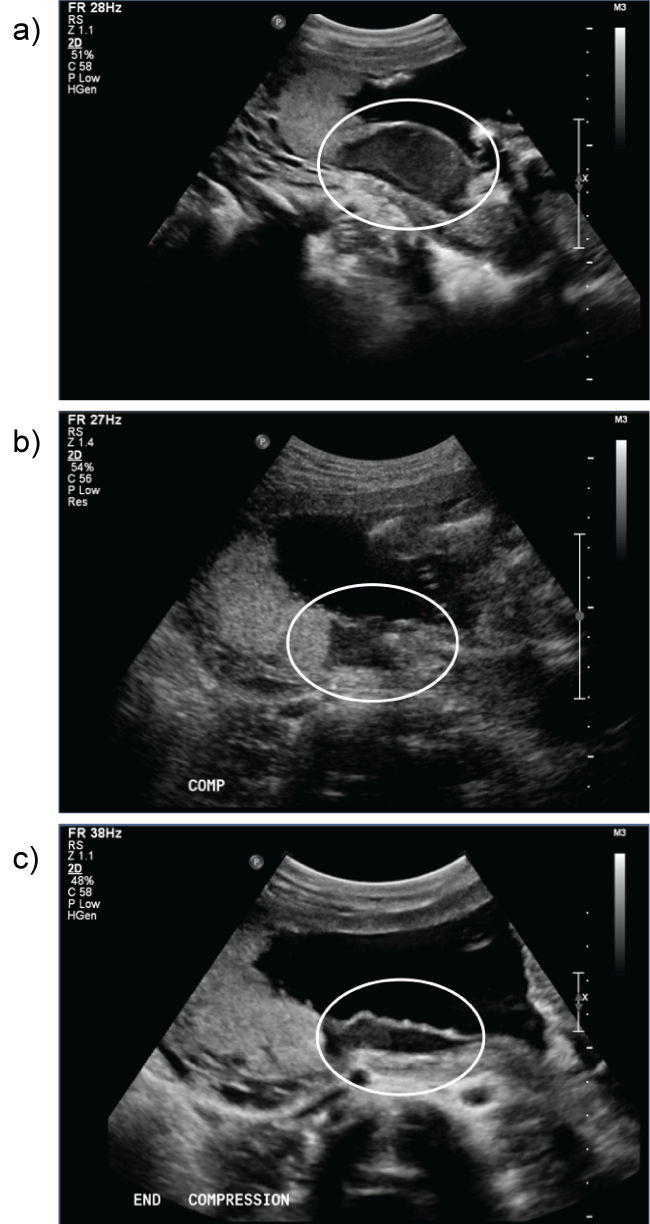
A 22-year-old woman, with a history of prior dilation and curettage for a first trimester abortion followed 1 year later by an uncomplicated term vaginal delivery, presented with an unplanned, undesired pregnancy at 21 weeks and 1 day by ultrasound dating. The patient had an uncomplicated prenatal course prior to presentation. Her past medical and surgical history was otherwise unremarkable. On initial ultrasound, the patient had a posterior fundal placenta with a subchorionic venous lake inferior to the lower margin of the placenta approximately 5 to 7 cm in diameter (Figure 1). Doppler examination suggested that the blood was venous in origin and continuous with the maternal circulation. Blood efflux into the maternal circulation out of the blood filled space was noted with the application of pressure on the maternal abdomen (Figure 2). The sonographic features were consistent with a Breus mole, thought to be a cystic degeneration of a subchorionic intervillous thrombus with subsequent connection to the maternal venous circulation. There was no evidence of an arteriovenous malformation.
.
Figure 1: Subchorionic blood filled space along lower margin of placenta continuous with maternal circulation at the base of the placenta (arrow).
View Figure 1
.
Figure 2: Emptying of the blood filled space with gentle pressure as a result of efflux of blood into the maternal circulation. a) Without compression; b) With compression; c) End of compression.
View Figure 2
After thorough discussion of risks, benefits and alternatives including continuing the pregnancy and induction of labor, the patient chose to proceed with surgical abortion for this unwanted pregnancy. The patient's preoperative hemoglobin and hematocrit were 10.8 g/dL and 33.0%, respectively, likely due to her pregnant state and unrelated to the placental abnormality. The patient was cross matched for 2 units of packed red blood cells and consented for possible Interventional Radiology (IR)-guided embolization. Fetal demise was induced with intra-amniotic digoxin to decrease placental blood flow two days prior to the procedure.
On the morning of the D&E, the patient had rupture of membranes in the preoperative holding area. Her case was rescheduled as the first case of the day. Fetal demise was confirmed at the start of the D&E by ultrasound, and the placenta was noted to have a subchorionic blood-filled space. The patient underwent an uncomplicated dilation and evacuation under ultrasound guidance. The placenta was grasped with forceps, causing the blood-filled space to compress, and then it was removed mostly intact. The patient was given Pitocin 40 units IV and Methergine 0.2 mg IM at the time of placental separation. Suction was performed at the end of the procedure to ensure that all remaining products of conception were evacuated. No blood transfusion or IR intervention was indicated. Ultrasound confirmed a thin endometrial stripe at the end of the procedure.
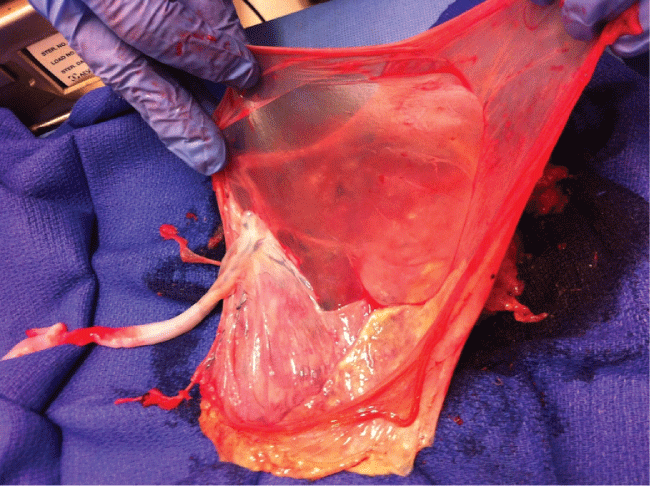
The placenta was sent to Pathology (Figure 3). Grossly, the placenta weighed 119 g when stripped of fetal membranes and the umbilical cord. The placental disc was 12.3 × 9.8 × 2.1 cm with an attached trivascular umbilical cord eccentrically inserted and measuring 29.0 cm in length and 1.0 cm in diameter with approximately 2 coils per 10 cm. The chorionic surface was markedly disrupted (approximately 60%). No subchorionic hematoma or potential space was noted, but the large area of disc disruption did not preclude this. The maternal surface was also markedly disrupted with fragmented placental disc. No hematomas or infarcts were noted. The final pathologic diagnosis was "Mature singleton placenta. Fibrin lined intervillous cystic structure, compatible with clinical finding of Breus mole".
.
Figure 3: Photograph of the placenta demonstrating the cystic sac of the Breus mole.
View Figure 3
The patient had an uncomplicated postoperative course.
Comment
Our patient presented with a rare finding in a viable pregnancy. A Breus mole was first suspected based upon ultrasound findings and ultimately confirmed with pathologic examination. The patient had no risk factors for the vascular abnormality, and although she had had a prior dilation and curettage, there is no known association between a Breus mole and prior uterine instrumentation. The patient desired termination, and as it was unclear what the potential for bleeding during or after the case was, precautions were taken in the case of difficulty delivering the placenta and devastating bleeding. Pre-procedure fetal demise was induced to decrease placental blood flow. The patient was typed and crossed for blood and arrangements had been made for possible IR intervention if needed.
The extraction of the placenta was without complication: the placenta delivered easily without any additional instrumentation. Uterotonics were prophylactically used at removal of the placenta. There was no significantly increased bleeding after the procedure attributable to the placenta anomaly. The placenta was sent to Pathology for tissue examination, and the pathologic examination confirmed the prenatal diagnosis of a Breus mole.
Given the patient's decision to end the pregnancy, it is unknown what potential complications could have arisen from the placenta anomaly. If the patient desired to continue the pregnancy, further imaging evaluation could have been done to support the diagnosis of a Breus mole with appropriate fetal surveillance.
Our experience shows that surgical abortion of a pregnancy complicated by a Breus mole can proceed without complications, as it appears that maternal blood loss into the hematoma is self-limited and the placenta can deliver without difficulty. Other clinical scenarios reported, although none utilizing a dilation and evacuation as the mode of delivery, have noted both uncomplicated outcomes and complications such as significant hemorrhage [2,7,10]. Based upon this, the risk of hemorrhage and poor outcomes is present during a surgical abortion due to the placental anomaly. Precautionary measures should be taken for potential bleeding, similar to those taken for a patient at increased risk of a postpartum hemorrhage.
It is unknown if the patient has an increased risk of recurrence in a subsequent pregnancy, but detailed ultrasound evaluation of the placenta could be justified with preparations made for potential abnormal bleeding at time of abortion or live birth.
References
-
Benirschke K (1981) Abortions and moles. Monogr Pathol 23-48.
-
Koçak M, Kandemir O, Sen S, Başkan B, Demir OF (2006) A rare form of abruptio placenta and clinical presentation in a preterm labor case: Breus' mole. Fetal Diagn Ther 21: 540-543.
-
Shanklin DR, Scott JS (1975) Massive subchorial thrombohaematoma (Breus' mole). Br J Obstet Gynaecol 82: 476-487.
-
Fox H, Elston CW (1978) Pathology of the placenta. Major Probl Pathol 7: 1-491.
-
Kim DT, Riddell DC, Welch JP, Scott H, Fraser RB, et al. (2002) Association between Breus' mole and partial hydatidiform mole: chance or can hydropic villi precipitate placental massive subchorionic thrombosis? Pediatr Pathol Mol Med 21: 451-459.
-
Wright JR, Samson KA, Cooper-Rosen E, Riddel DC (1998) Breus' Mole: DNA Shows Massive Subchorionic Hematoma is Maternal in Origin. Fetal Pediatr Pathol 18: 151-156.
-
Giri V, Cheema Q, Mulay A (2011) Early-onset severe growth restriction and placental abruption associated with Breus mole. Int J Gynaecol Obstet 113: 81-82.
-
Kojima K, Suzuki Y, Makino A, Murakami I, Suzumori K (2001) A case of massive subchorionic thrombohematoma diagnosed by ultrasonography and magnetic resonance imaging. Fetal DiagnTher 16: 57-60.
-
Madu AE (2006) Breus' mole in pregnancy. J Obstet Gynaecol 26: 815-816.
-
Alanjari A, Wright E, Keating S, Ryan G, Kingdom J (2013) Prenatal diagnosis, clinical outcomes, and associated pathology in pregnancies complicated by massive subchorionic thrombohematoma (Breus' mole). Prenat Diagn 33: 973-978.
-
Nishida N, Suzuki S, Hamamura Y, Igarashi K, Hayashi Z, et al. (2001) Massive subchorionic hematoma (Breus' mole) complicated by intrauterine growth retardation. J Nippon Med Sch 68: 54-57.





