Obstetrics and Gynaecology Cases - Reviews
Arteriovenous Malformation of the Cervix: A Rare Cause of Vaginal Bleeding after Supracervical Hysterectomy
Nigel Pereira1*, Kayla M Wishall1, Gabrielle M Hawkins2, Nima R. Patel3 and Carl R. Della Badia DO3
1Department of Obstetrics and Gynecology, Drexel University College of Medicine, Philadelphia, USA
2Drexel University College of Medicine, Philadelphia, USA
3Division of Minimally Invasive Gynecologic Surgery, Drexel University College of Medicine, Philadelphia, USA
*Corresponding author: Nigel Pereira, MD, Department of Obstetrics and Gynecology, 245 N 15th Street, MS 495, 16th Floor, New College Building, Philadelphia, PA, 19102. USA, Tel: 215-762-8292, Fax: 215-762-1470, E-mail: nigelepereira@gmail.com
Obstet Gynecol Cases Rev, OGCR-2-021, (Volume 2, Issue 1), Case Report; ISSN: 2377-9004
Received: October 22, 2014 | Accepted: January 28, 2015 | Published: January 30, 2015
Citation: Pereira N, Wishall KM, Hawkins GM, Patel NR, Badia DO (2015) Arteriovenous Malformation of the Cervix: A Rare Cause of Vaginal Bleeding after Supracervical Hysterectomy. Gynecol Cases Rev 2:021. 10.23937/2377-9004/1410021
Copyright: © 2015 Pereira N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Cyclic vaginal bleeding is a well-known complication after a supracervical hysterectomy; however, severe delayed vaginal bleeding occurs infrequently.
Case: A 29-year-old woman underwent a supracervical hysterectomy for dysmenorrhea and pelvic pain refractory to multiple medical modalities. Eight weeks after surgery, the patient began to experience persistent heavy vaginal bleeding that continued in spite of application of silver nitrate to the cervical stump. The patient subsequently underwent vaginal trachelectomy for definitive management of the bleeding.
Results: Histologic and immunohistochemical evaluation of the excised cervical stump revealed chronic cervicitis and an arteriovenous malformation of the cervix confirmed by elastic staining.
Conclusions: Our case highlights that an arteriovenous malformation of the cervix can be an exceedingly rare cause of severe delayed vaginal bleeding after a supracervical hysterectomy, and should be considered in the differential diagnosis of vaginal bleeding after a supracervical hysterectomy.
Keywords
Arteriovenous malformation, Vaginal bleeding, Supracervical hysterectomy, Complications
Introduction
Hysterectomy is one of the most commonly performed gynecologic surgeries worldwide, with several variations in surgical technique [1,2]. Supracervical hysterectomy is one such technique, which can be performed either through the laparoscopic or abdominal approach. With an estimated incidence of 5-25%, cyclic vaginal bleeding is a frequently encountered complication after a supracervical hysterectomy [3-5]. Severe delayed vaginal bleeding after a supracervical hysterectomy, however, occurs rarely. Here, we report the case of 29-year-old woman with severe delayed vaginal bleeding after a supracervical hysterectomy due to an arteriovenous malformation (AVM) of the cervix.
Case Report
A 29-year-old nulliparous woman, with a history of menorrhagia, dysmenorrhea, and chronic pelvic pain presented for definitive surgical therapy. Various medical modalities had previously failed, including oral contraceptives and the levonorgestrel intrauterine device. Ablation of the endometrial lining was also performed 1-year prior, which alleviated her menorrhagia but not her dysmenorrhea or pelvic pain. She elected to undergo a laparoscopic supracervical hysterectomy. An uncomplicated laparoscopic supracervical hysterectomy was performed using a LiNA loop (LiNA Medical ApS, Glostrup, Denmark) to separate the uterine corpus from the cervix. The upper canal of the cervical stump was cauterized to minimize any residual endometrial tissue. Pathologic examination of the hysterectomized specimen revealed an atrophic and denuded endometrium, and unremarkable myometrium, fallopian tubes and utero-cervical junction. The patient made an uneventful recovery, with no complaints during her postoperative office visits 2 and 6 weeks later.
Eight weeks after surgery, the patient complained of heavy and persistent vaginal bleeding. The patient denied sexual activity, trauma, pelvic pain, or abdominal pain. The patient returned to the office for an examination. Her vital signs were within normal limits and her abdomen had well-healed surgical scars, without tenderness or guarding. Speculum examination revealed scant blood in the vaginal vault, a grossly normal appearing cervix, with minimal cervical bleeding. The endocervical canal was cauterized using silver nitrate following which no cervical bleeding was noted. A bimanual exam was performed, which was significant for cervical motion tenderness, and the patient was prescribed a week-long course of oral doxycycline 100mg two times a day for a presumptive diagnosis of cervicitis.
Despite these measures, the patient continued to experience heavy vaginal bleeding, and a trachelectomy was performed for definitive management. Intraoperative examination revealed a few blood clots in the vaginal vault, without active bleeding from the cervical stump. An uneventful vaginal trachelectomy with minimal blood loss was performed.
Results
Gross pathology of the surgical specimen showed a cervix measuring 3.4 � 2.7 � 3 cm, with an os measuring 1.3 � 0.6 cm. A large tortuous vessel near the posterior-superior resection margin was also noted (Figure 1). Serial sections of the cervix with the vessel were submitted for immunohistochemical examination. The cervix showed histologic signs of chronic cervicitis, and the vessel was confirmed to be an arteriovenous malformation by elastic staining (Figure 2). At her 2-week postoperative office visit, the patient denied any recurrence of symptoms.
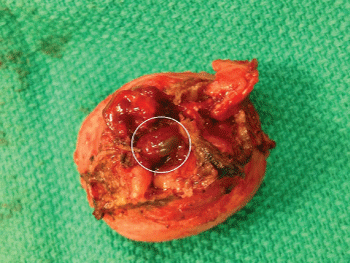
Figure 1: Surgically excised cervical stump revealing a large tortuous vessel (white circle) at the cut surface
View Figure 1
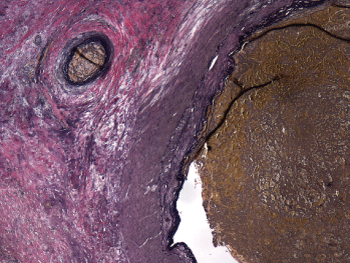
Figure 2: Photomicrograph showing a cut section of the cervical AVM, with elastic stain highlighting the elastic lamia of the AVM (4x magnification, elastic stain)
View Figure 2
Discussion
Supracervical or subtotal hysterectomy was first carried out at the turn of the last century to reduce total hysterectomy-related complications, particularly ureteral injuries [6]. During the past decade, laparoscopic supracervical hysterectomy has become an increasing popular hysterectomy technique in the management of benign uterine pathology, primarily due to decreased operative time [2,3]. Initially thought to be superior to other modes of hysterectomy, current data indicate no difference in complications, pelvic support, sexual, and urinary function in patients undergoing laparoscopic supracervical hysterectomy [2]. The decision to leave behind a cervical stump is therefore debated, posing risks of cervical neoplasia and cyclic vaginal bleeding [3,6].
A lack of consensus exists about the incidence of cyclic vaginal bleeding after a supracervical hysterectomy; however, some studies estimate this complication to occur in up to 25% of cases [3,6]. Cyclic stimulation of remnant endometrial tissue in the upper cervical canal is posited to be cause of such vaginal bleeding [7]. Improper surgical technique leading to uterine amputation above the level of the internal os has frequently been blamed for remnant endometrial tissue in the cervical stump, though vaginal bleeding may still occur even when amputation of the uterus below the level cervical os has been performed [4,7]. Therefore, intraoperative ablation or coring of the endocervical canal is frequently performed to reduce the possibility of postoperative bleeding [6-8].
Severe delayed vaginal bleeding from the cervical stump after a supracervical hysterectomy is a rare complication [6,9]. We searched PubMed, Ovid, EMBASE, Google Scholar for all English-language articles published from January 1990 to August 2014 with search terms including �supracervical hysterectomy,� �vaginal bleeding,� �vaginal hemorrhage,� �delayed bleeding,� and �complications.� Our search returned only one publication reporting the case of a patient who presented on postoperative day 15 after a LSH with severe vaginal bleeding [9]. The bleeding in this case was thought to be due to cautery-induced tissue necrosis of the cervical stump. Our search, however, did not reveal any reports of severe vaginal bleeding related to vascular malformations of the cervix.
Vascular malformations, specifically AVMs, constitute a very small portion of all tumors of the female genital tract [10]. AVMs may occur in isolation or as a part of a syndrome, and may be congenital or acquired [11]. In general, vascular lesions may be classified based on the main channel type, that is, arterial, venous, capillary, lymphatic, or mixed [12,13]. They can be further subdivided based on flow characteristics into slow-flow or fast-flow lesions [12,13]. Slow-flow lesions include venous, capillary, and lymphatic vascular malformations, and fast-flow lesions include arterial, arteriovenous, and arteriovenous fistula vascular malformations [12,13].
The majorities of AVMs of the female genital tract are asymptomatic and found incidentally; however, when symptomatic, they can cause profuse bleeding and hemodynamic changes, both of which are related to the size of the AVM [10]. Historically, the diagnosis of an AVM was made by histopathologic analysis of the surgical specimen [9]. Most recently, however, non-invasive diagnostic modalities such as ultrasonography with color Doppler, magnetic resonance imaging and angiography have been utilized as adjuncts in the diagnosis of AVMs [11,12].
We were uncertain about the cause of this patient�s severe delayed vaginal bleeding 8 weeks after the laparoscopic supracervical hysterectomy, but given her pattern of delayed, non-cyclic and heavy vaginal bleeding, we remained suspicious about a vascular lesion of the cervical stump. Radiologic imaging may have aided in diagnosing a vascular lesion; however, we decided not to undertake any radiologic investigation as we considered a trachelectomy to be the best diagnostic and therapeutic strategy for this patient, especially given her desire for definitive therapy. Rapid enlargement or bleeding of AVMs has known to occur in the setting of trauma, thrombosis, infection, or hormonal changes [10-13]. In the absence of vaginal trauma and acute changes in hormonal status, and in the presence of cervical motion tenderness on pelvic examination, we postulate that the triggering event for severe vaginal bleeding in our patient was likely infectious or inflammatory in nature. This is further corroborated by the histologic findings of cervicitis in the trachelectomy specimen. It is also possible that thermal injury to the AVM may have occurred during cauterization of the cervical stump during the original laparoscopic supracervical hysterectomy, making bleeding more likely to occur from the AVM in an infectious or inflammatory setting. The lack of histologic findings of thermal artifact in the trachelectomy specimen, however, makes this hypothesis less likely. Finally, the possibility that the AVM was merely an incidental finding cannot be ruled out confidently.
The treatment of cervical AVMs is typically a hysterectomy, or as highlighted in our case, a trachelectomy if a supracervical hysterectomy has previously been performed [8]. Alternatives including embolization of the feeding vessel with coils or polyvinyl alcohol particles mixed with thrombin have been described [8]. Radiation treatment with brachytherapy has also proven too effective in some cases [8].
Conclusions
When severe delayed vaginal bleeding occurs after a LSH, or when vaginal bleeding remains refractory to routine therapeutic measures such as cauterization of the cervical stump, the possibility of an AVM of the cervix should be considered [9]. Despite its rarity, early recognition of a cervical AVM is imperative to enable timely diagnosis and intervention [9].
References
-
Wu JM, Wechter ME, Geller EJ, Nguyen TV, Visco AG (2007) Hysterectomy rates in the United States, 2003. Obstet Gynecol 110: 1091-1095.
-
American College of Obstetricians and Gynecologists (2007) ACOG Committee Opinion No. 388 November 2007: supracervical hysterectomy. Obstet Gynecol 110: 1215-1217.
-
Huang JY, Ziegler C, Tulandi T (2005) Cervical stump necrosis and septic shock after laparoscopic supracervical hysterectomy. J Minim Invasive Gynecol 12: 162-164.
-
Ghomi A, Hantes J, Lotze EC (2005) Incidence of cyclical bleeding after laparoscopic supracervical hysterectomy. J Minim Invasive Gynecol 12: 201-205.
-
van der Stege JG, van Beek JJ (1999) Problems related to the cervical stump at follow-up in laparoscopic supracervical hysterectomy. JSLS 3: 5-7.
-
Kho RM, Magrina JF (2011) Removal of the retained cervical stump after supracervical hysterectomy. Best Pract Res Clin Obstet Gynaecol 25: 153-156.
-
Berner E, Qvigstad E, Langebrekke A, Lieng M (2013) Laparoscopic Supracervical Hysterectomy Performed With and Without Excision of the Endocervix: A Randomized Controlled Trial. J Minim Invasive Gynecol 20:368-375.
-
Lowenstein L, Solt I, Deutsch M, Kerner H, Amit A (2004) A life-threatening event: uterine cervical arteriovenous malformation. Obstet Gynecol 103: 1073-1075.
-
Holloran-Schwartz MB, Potter SJ, Kao MS (2012) Massive delayed vaginal hemorrhage after laparoscopic supracervical hysterectomy. Case Rep Obstet Gynecol 2012:871041.
-
Gupta R, Singh S, Nigam S, Khurana N (2006) Benign vascular tumors of female genital tract. Int J Gynecol Cancer 16: 1195-1200.
-
Brotherton J, Yazdany T (2010) Resection of a vulvar arteriovenous malformation in a premenarchal patient. Obstet Gynecol 115: 426-429.
-
Herman AR, Morello F, Strickland JL (2004) Vulvar venous malformations in an 11-year-old girl: a case report. J Pediatr Adolesc Gynecol 17: 179-181.
-
Pereira N, Dormosh M, Mirmanesh M, Guilfoil DS (2014) Arteriovenous malformation of the vulva: a case report. J Low Genit Tract Dis 18: 12-15.





