Obstetrics and Gynaecology Cases - Reviews
Uterine Artery Embolisation for the Treatment of Large Submucosal Fibroid (Clinical Case)
Dobrokhotova J1*, Grishin I1, Khachatryan A1, Causeva O2, Zlatovratsky A2 and Rogovskaya S1
1Department of Obstetrics and Gynecology, N.I. Pirogov Russian National Research Medical University, Moscow, Russia
2City Clinical Hospital No 1 N.I. Pirogov, Russia
*Corresponding author: Dobrokhotova Julia, MD, Ph. D, Professor, Head of Department of Obstetrics and Gynecology, Medical Faculty, N.I. Pirogov Russian National Research Medical University, Moscow, Russia, E-mail: pr.dobrohotova@mail.ru
Obstet Gynecol Cases Rev, OGCR-2-023, (Volume 2, Issue 1), Case Report; ISSN: 2377-9004
Received: November 04, 2014 | Accepted: February 06, 2015 | Published: February 09, 2015
Citation: Dobrokhotova J, Grishin I, Khachatryan A, Causeva O, Zlatovratsky A, etal. (2015) Uterine Artery Embolisation for the Treatment of Large Submucosal Fibroid (Clinical Case). Obstet Gynecol Cases Rev 2:023. 10.23937/2377-9004/1410023
Copyright: © 2015 Dobrokhotova J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Article is devoted to the problem of endovascular treatment of uterine fibroids - Uterine Artery Embolization (UAE). A number of researches do not promote to use UAE technique when the uterine fibroid has submucosal position, considering the conservative transcervical myomectomy to be more accessible. In the article, based on clinical case, indication of EMA at the large submucous uterine fibroid among women that are still in their reproductive age as an alternative to a hysterectomy is discussed.
Keywords
Uterine artery embolization, Uterine fibroids, Embolization, Large fibroids, Myomectomy
Introduction and Background
Uterine Artery Embolization (UAE) is a uterine-sparing procedure that is used for the treatment of uterine fibroids. The indications for UAE include all symptomatic fibroids i.e. fibroids accompanied with menometrorrhagia, pain, heaviness, frequent urination, dyspareunia, etc., as well as rapidly growing fibroids, and large fibroids [1-5]. Spies say that the indications for UAE include virtually all the indications for the surgical treatment for the uterine fibroids [6].
The narrow-stalked, pedunculated subserous and submucosal fibroids come under the contraindications for UAE as in the former case the risk of fibroid expulsion into the abdominal cavity after endovascular intervention is high; whereas an alternative of minimally invasive hysteroscopic resection is available in the latter case1. It is sensible to carry out UAE with a subsequent myomectomy for the treatment of most uterine fibroids, when one of the tumours has a subserous or submucosal position [7].
Based on the above-stated case, UAE is proved clinically appealing and effective procedure for the treatment of large submucosal uterine fibroids.
Clinical Case
A 33-year-old woman was admitted to N.I. Pirogov City Clinical Hospital No.1, being diagnosed with Submucous leiomyoma of uterus, passed through the cervix fibroid, severe chronic posthaemorrhagic anemia. The patient complained of weakness, dizziness, losing consciousness during the last year, and heavy menstrual bleedings.
Anamnesis did not reveal any chronic disease of the extravaginal region. The first pregnancy in 2007 was a missed abortion at 8-9 weeks, whereas the second pregnancy in 2009 ended up with a successful delivery. The last normal menstrual period was noticed in August 2012. Menorrhagia was observed during the last year.
She was fully investigated in the gynecology unit. Low hemoglobin up to 76 g/l was seen in the clinical blood analysis. There were no abnormalities found in the biochemical analysis of blood, blood coagulogram, and urinalysis. The ultrasound investigation revealed that the size of body of the uterus was increased corresponding to 15-16 weeks of pregnancy. The submucosal fibroid (13.5cm�9.3cm�10.9cm) completely occupying the uterine cavity had mixed type of blood circulation. Uterine appendages were normal. There were no other pathological changes revealed in the organs of the abdominal cavity and lesser pelvis.
Gynecological Investigations: The external genital organs were of a normal growth. Pubic hair was of the female pattern. Vaginal examination revealed the walls of the vagina to be clear and pink in color. The cervix was round in shape, narrow with no hypertrophy. A finger could pass through the external os of the cervix with the lower edge of the fibroid had been being palpable. There was observed a bloody discharge through the cervical canal. Bimanual vaginal examination with abdominal palpation revealed the uterus to be in the anteflexed position. The body of the uterus was balloon shaped. It was increased in size, relatively corresponding to 15-16 weeks of pregnancy. It was slightly dense and painless on palpation. Uterine appendages were normal. Fornices of the vagina were deep and empty. There was no infiltration to the parametrium.
The diagnosis of submucous leiomyoma of uterus with anemia of moderate degree was established based on the anamnesis data, clinical blood analysis, ultrasound investigation, and the clinical picture. Despite the large size of the fibroid, its submucosal position, a bright clinical picture, and taking into consideration patient's reproductive age, it was decided to refrain from hysterectomy. Carrying out its resection through a resectoscope was not an option as the fibroid was large. Thus, a decision was made to perform uterine artery embolization.
Arteriography and uterine artery embolization were performed in the radio-endovascular surgery department of N.I. Pirogov City Clinical Hospital No.1. Blood transfusion with 323mLs of erythrocyte suspension was carried out to the patient. Antibacterial, anti-inflammatory, and analgesic medicines were administered along with the infusion therapy. An ultrasound investigation was carried out after UAE. It showed increased size of the body of the uterus, relatively corresponding to 15-16 weeks of pregnancy (13.5 cm�9.3 cm�10.9 cm) and was shown as avascular on the Color Doppler scan.
Under our observation, the patient was discharged from the hospital on the 8th day. The patient was provided with directions regarding the further continuation of treatment of her anemia by keeping the blood hemoglobin level under control. She was asked to carry out planned ultrasound investigations in the period of 1, 3, 6, and 12 months.
Three months later a recurrent hospitalization in N.I. Pirogov City Clinical Hospital No.1 was followed due to a heavy bloody discharge from the genital tract. The patient complained of two heavy menstrual periods after UAE. According to the ultrasound investigation of the organs of lesser pelvis, the submucosal fibroid was descended to the lower third of the uterus. This time it was 10.5cm�6.5cm�7.9 cm in size. Intranodular and perinodular blood flow were well pronounced on the Colour Doppler scan (Figure1).
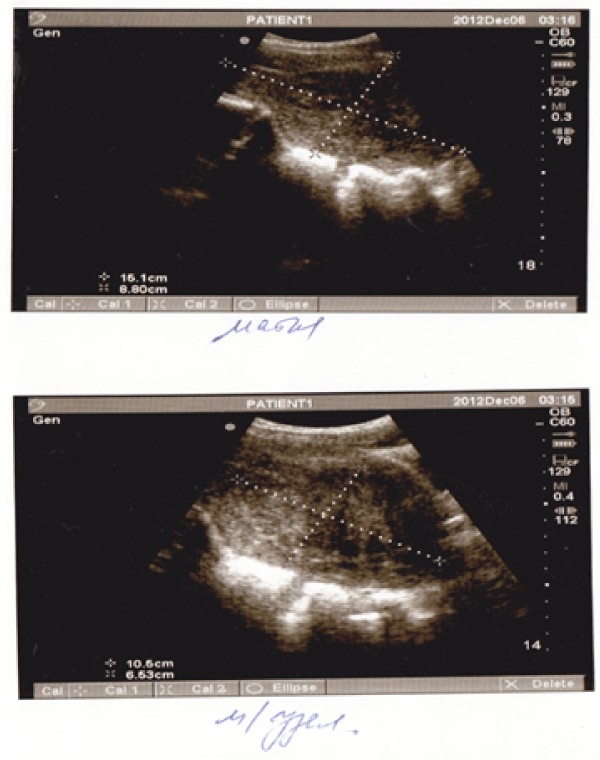
Figure 1: Ultrasound investigation of the uterus and uterine fibroid after using UAE for the first time
View Figure 1
Gynecological Investigations: the cervix was round in shape, narrow with no hypertrophy. External os of the cervix measured between 3 and 4 cm. There was observed a bloody discharge through the cervical canal. Bimanual vaginal examination with abdominal palpation revealed the uterus to be in the anteflexed position. The body of the uterus was balloon shaped. It was increased in size, relatively corresponding to 11-12 weeks of pregnancy. It was slightly dense and painless on palpation. Fornices of the vagina were deep and empty. There was no infiltration to the parametrium.
After taking into consideration the clinical picture and ultrasound investigation of the lesser pelvis, including the Colour Doppler scan that marked well pronounced intranodular and perinodular blood flow, a decision was made to perform UAE for the second time. Arteriography and uterine artery embolization were performed in the radio-endovascular surgery department of N.I. Pirogov City Clinical Hospital No.1. An ultrasound investigation showed the uterus to be 6.2cm�3.8cm�5.9cm in size. A wide-stalked tumour mass of heterogeneous echogenicity (12.0 cm�7.0 cm�8.6 cm) had grown out from the posterior wall. It was considered as an interstitial-submucosal fibroid with signs of detachment. The mass was shown as avascular on the Colour Doppler scan.
Gynecological Investigations revealed narrow cervix. External os of the cervix measured between 3 and 4cm. The lower edge of the fibroid was soft on palpation. There was observed a bloody discharge through the cervical canal. Bimanual vaginal examination with abdominal palpation revealed the uterus to be increased in size, relatively corresponding to 11-12 weeks of pregnancy.
After taking into consideration the large size of the fibroid and its soft consistency, a decision was made to carry out transcervical myomectomy. Transcervical myomectomy with hysteroscopy was performed on the 7th day after UAE. Blood loss was about 50mLs (Figure 2).
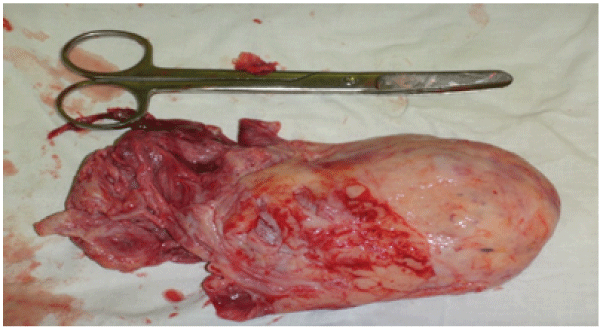
Figure 2: Gross appearance of the submucosal fibroid
View Figure 2
According to the postoperative ultrasound investigation, the uterus measured 6.0cm�4.4cm�4.8cm. Its borders were regular with no evidence of myomata. Endometrium was 0.8 cm thick with regular and clear borders.
The condition of the patient was satisfactory. Under our observation, the patient was discharged from the hospital on the 10th day. The patient was provided with directions regarding the further continuation of treatment of her anemia by keeping the blood hemoglobin level under control. She was asked to carry out planned ultrasound investigations in the period of 1, 3, 6, and 12 months.
One month after the transcervical myomectomy, an ultrasound investigation of the organs of lesser pelvis was carried out as it had been planned. The uterus measured 6.7cm�4.2cm�5.6cm. Its borders were regular, but the myometrium was heterogeneous. No evidence of myomata. A hypoechoic tumour bed (2.3cm�0.8cm�1.2cm) was revealed on the middle third of posterior wall of the uterus. Thickness of endometrium was 0.5cm on the upper third and 0.2cm on the lower third (Figure 3).
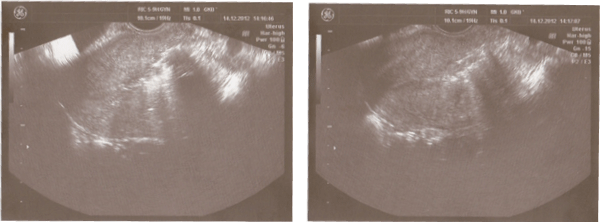
Figure 3: Ultrasound investigation of the uterus after myomectomy (The arrow points to the tumour bed)
View Figure 3
Discussion
UAE is successfully used in the treatment of most uterine fibroids [1]. A number of researches do not promote to use UAE technique when the uterine fibroid has submucosal position, considering the conservative transcervical myomectomy to be more accessible [8]. As the authors mention [8-10], 5% of the patients with submucosal uterine fibroid may face both early as well as late transvaginal expulsion. In most cases, the detaching fibroid expulses in the early days once the symptoms appear.
In some observations noted the myometrial migration of submucosal fibroids to be accompanied by their subsequent volume reduction or fibrosis and followed by their volume retention in absence of clinical manifestations of the uterine fibroid [3,7]. In these cases it becomes possible to perform resectoscopy, however early it was impossible because of the size of fibroids.
However, the indications for UAE are considerably more in number than those for the surgical treatment for the uterine fibroids; besides the endovascular intervention eliminates the need of a hysterectomy in patient, avoiding the use of anaesthesia, surgical trauma, as well as severe early and late postoperative complications in case of surgical treatment [2,11]. Thus UAE can be carried out among women with submucosal uterine fibroid of type 0, I, and II [12] as an alternative to hysterectomy, as well as when the transcervical myomectomy cannot be carried out immediately [13,14]. UAE is the method of choice unlike the surgical interventions especially among patients with high surgical and anesthesiological risk [5,12].
According to the literature in recent years, UAE doesn't effect significant on menstrual function and fertility among women. Tropeano et al. [15,16] established no effect UAE on the level of follicle-stimulating hormone (FSH), estradiol, the number of antral follicles and ovarian volume within 1 year of observation for women after UAE [15,16].
Kim et al. evaluated the effectiveness of UAE in young women taking into account peculiarities of blood supply to the uterus and ovaries describe three clinical cases of amenorrhea in patients with uterus-ovarian anastomoses [17].
Most researchers noted a significant success in the treatment of UAE of uterine fibroids in patients interested in the reproductive function [18-20]. Walker et al published data on 56 pregnancies that ended in the birth of 33 (58,9%) cases [21].
Conclusion
According to Marret et al. such complications as endometritis and pyometra may occur due to a late fibroid expulsion [10].
Although in this particular case, the fibroid was trapped in the uterus; and we do not count it as a complication. UAE can be used as a part of the overall treatment that a patient needs for the uterine fibroids, thereby called as UAE-assisted transcervical myomectomy.
This case illustrates the uterine-sparing importance of UAE in patients with large and submucosal uterine fibroid. Thus, as an alternative to a hysterectomy, it is sensible and effective to perform uterine artery embolisation for the treatment of large submucosal fibroid among women that are still in their reproductive age with subsequent myomectomy possible.
References
-
Belenky A, Cohen M, Bachar GN (2001) Uterine arterial embolization for the management of leiomyomas. Isr Med Assoc J 3: 719-721.
-
Itkin M, Shlansky-Goldberg R (2002) Uterine Fibroid Embolization for the Treatment of Symptomatic Leiomyomata. Applied Radiology 31: 9-17.
-
Saveleva GM, Breusenko VG, Kapranov CA, Kurcer MA, Krasnova IA, et al. (2007). Uterine artery embolization in the treatment of uterine fibroids: achievements and prospects. Obstetrics and Gynecology 5: 54-59.
-
Ravina JH, Merland JJ, Ciraru-Vigneron N, Bouret JM, Herbreteau D, et al. (1995) [Arterial embolization: a new treatment of menorrhagia in uterine fibroma]. Presse Med 24: 1754.
-
Worthington-Kirsch RL, Siskin GP (2004) Uterine artery embolization for symptomatic myomata. J Intensive Care Med 19: 13-21.
-
Spies JB, Ascher SA, Roth AR, Kim J, Levy EB, et al. (2001) Uterine artery embolization for leiomyomata. Obstet Gynecol 98: 29-34.
-
Dobrokhotova JE, Kapranov SA, Alieva AA (2005) New method of treatment of uterine leiomyomas-uterine artery embolization. Medicine (periodic textbook of RSMU 2: 24-27.
-
Mara M, Fucikova Z, Kuzel D, Maskova J, Dundr P, et al. (2007) Hysteroscopy after uterine fibroid embolization in women of fertile age. J Obstet Gynaecol Res 33: 316-324.
-
Mara M, Horak P, Kubinova K, Dundr P, Belsan T, et al. (2012) Hysteroscopy after uterine fibroid embolization: evaluation of intrauterine findings in 127 patients. J Obstet Gynaecol Res 38: 823-831.
-
Marret H, Keris Yle B, Acker O, Cottier JP, Herbreteau D (2004) Late leiomyoma expulsion after uterine artery embolization. J Vasc Interv Radiol 15: 1483-1485.
-
Al-Mahrizi S, Tulandi T (2007) Treatment of uterine fibroids for abnormal uterine bleeding: myomectomy and uterine artery embolization. Best Pract Res Clin Obstet Gynaecol 21: 995-1005.
-
Wamsteker K, Emanuel MH, de Kruif JH (1993) Transcervical hysteroscopic resection of submucous fibroids for abnormal uterine bleeding: results regarding the degree of intramural extension. Obstet Gynecol 82: 736-740.
-
Agdi M, Tulandi T (2010) Minimally invasive approach for myomectomy. Semin Reprod Med 28: 228-234.
-
Berkowitz RP, Hutchins FL Jr, Worthington-Kirsch RL (1999) Vaginal expulsion of submucosal fibroids after uterine artery embolization. A report of three cases. J Reprod Med 44: 373-376.
-
Tropeano G, Di Stasi C, Litwicka K, Romano D, Draisci G, et al. (2004) Uterine artery embolization for fibroids does not have adverse effects on ovarian reserve in regularly cycling women younger than 40 years. Fertil Steril 81: 1055-1061.
-
Tropeano G, Di Stasi C, Amoroso S, Gualano MR, Bonomo L, et al. (2010) Long-term effects of uterine fibroid embolization on ovarian reserve: a prospective cohort study. Fertil Steril 94: 2296-2300.
-
Kim HS, Paxton BE, Lee JM (2008) Long-term efficacy and safety of uterine artery embolization in young patients with and without uteroovarian anastomoses. J Vasc Interv Radiol 19: 195-200.
-
Knisheva IG (2012) Analysis of the clinical course of pregnancy, especiality of fetoplacentar complex, hemostatic systems and function of endometrium in patients after uterine artery embolization for myomas. Medicine 3: 50-56.
-
Kim MD, Kim NK, Kim HJ, Lee MH (2005) Pregnancy following uterine artery embolization with polyvinyl alcohol particles for patients with uterine fibroid or adenomyosis. Cardiovasc Intervent Radiol 28: 611-615.
-
Redecha M Jr, Mizickova, Javorka V, Redecha M Sr, Kurimska S, et al. (2013) Pregnancy after uterine artery embolization for the treatment of myomas: a case series. Arch Gynecol Obstet 287: 71-76.
-
Walker WJ, McDowell SJ (2006) Pregnancy after uterine artery embolization for leiomyomata: a series of 56 completed pregnancies. AJOG 195: 1266-1271.





