Obstetrics and Gynaecology Cases - Reviews
A Case of Arthrogryposis Multiplex Congenita in One Identical Twin Pregnancy
Ulas Fidan, Fahri Bur�in Firatligil*, Kazim Emre Karasahin, Mustafa Ulubay, Ugur Keskin and Ali Erg�n
Gulhane Military Medical Academy, Obstetrics and Gynecology Department, Turkey
*Corresponding author: Fahri Bur�in Firatligil, M.D., Gulhane Military Medical Academy, Obstetrics and Gynecology Department, Ankara, Turkey, Tel: +90 312 3045810, Fax: +90 312 3045800, E-mail: md.fahri@gmail.com
Obstet Gynecol Cases Rev, OGCR-2-037, (Volume 2, Issue 3), Case Report; ISSN: 2377-9004
Received: April 08, 2015 | Accepted: May 03, 2015 | Published: May 06, 2015
Citation: Fidan U, Firatligil FB, Karasahin KE, Ulubay M, Keskin U, et al. (2015) A Case of Arthrogryposis Multiplex Congenita in One Identical Twin Pregnancy. Obstet Gynecol Cases Rev 2:037. 10.23937/2377-9004/1410037
Copyright: © 2015 Fidan U, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Arthrogryposis multiplex congenita, is a developmental deformation characterized with multiple joint contructures that is seen in one delivery out of 3000 in average. The limitation of fetal movements which start in early pregnancy weeks especially at the 7th or 8th gestastional week, is the most important factor in etiology. That deformation, causes fetal morbidity, mortality and economic burden in postnatal period. In this case, an arthrogryposis in one identical twin, which was diagnosed during a routine 2nd trimester 2D ultrasound examination in which the pregnancy was terminated because of the misdiagnosis with twin- to twin transfusion syndrome, was reported.
Keywords
Arthrogryposis, Twin to twin transfusion, Twin pregnancy
Introduction
Arthrogryposis multiplex congenita (AMC), is a developmental deformation characterized with multiple joint contructures that is seen in one delivery out of 3000 in average [1]. Especially, the limitation of fetal movements which start in early pregnancy weeks, is the most important factor in etiology [2]. Especially, the factors such as muscular (muscular dystrophia, myastenia gravis disease in mother), neurologic (brain, spinal cord and peripheric nerve abnormalities), connective tissue diseases (distrophic displasia, marfan syndrome), the cases causing intrauterine space limitation (twin pregnancy, myomas, uterus abnormalities) can cause AMC by preventing fetal movements [3,4]. The etiologic factor that causes AMC, can generally be observed after autopsy [5]. In AMC patients, beside contructure abnormalities seen especially in distal joints; micrognathia, low- located ears, short neck, smooth- wide nose root and various muscular- skeletal system changes can be observed [5,6].
The early diagnosis and treatment of external factors causing AMC, can provide the prevention of deformation or can facilitate the treatment of deformation in postnatal period and thus can speed up the recovery [5].
In this case, an AMC in one identical twin, which was diagnosed during a routine 2nd trimester 2D ultrasound examination, was reported
Case Report
A female patient aged 36, G3P1, who had one normal vaginal delivery and an abortion previously, applied to our clinics for routine control examination. From the patient�s history, it was understood that the current pregnancy was a spontaneous twin pregnancy, within 17th gestational age by last menstrual period. It was determined in the anamnesis of the patient that she had no known chronic disease or gynecologic operation history. Beside that, there was no history of previous congenital deformations in the family.
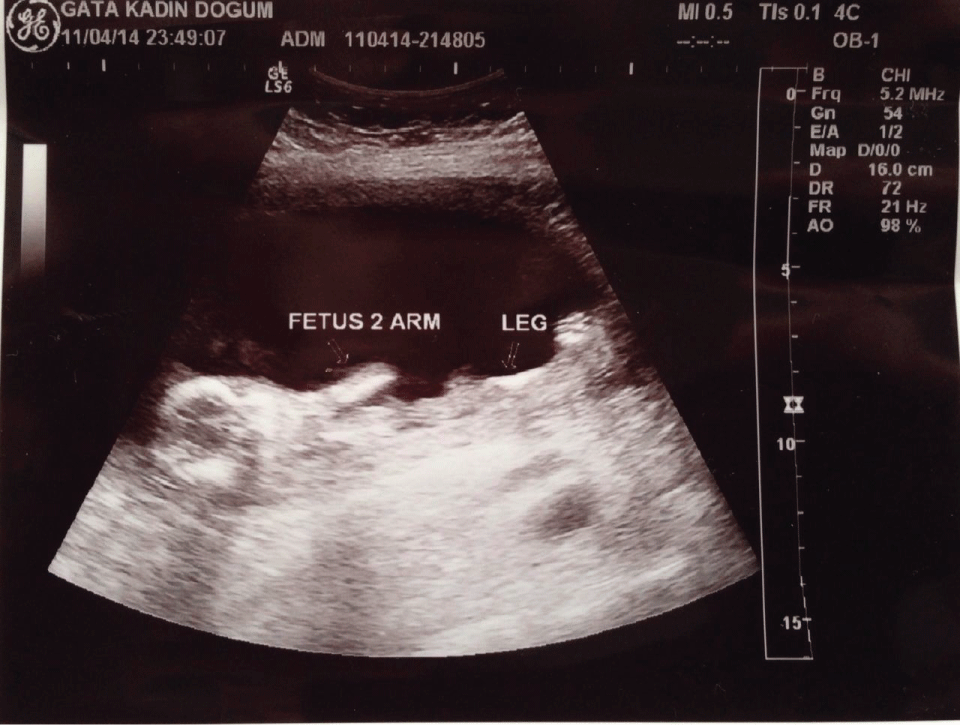
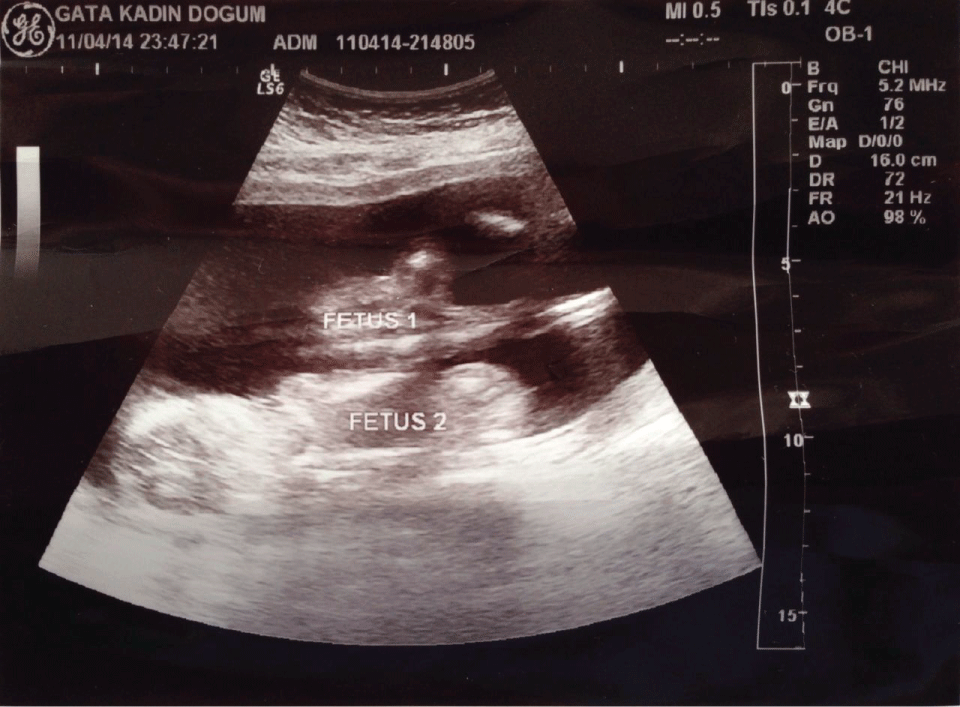
In routine prenatal ultrasound examination, there was a single placenta with thin dividing membranes (monochorionic and diamniotic), the examiner noted the absence of fetal movements, fixed flexion deformities and small chest deformity in one identical twin within 30 minutes observation period (Figure 1). Fetal biometric measurements were assessed for that fetus as 16th gestational week with normal amniotic fluid index (AFI). The other fetus was actively moving (Figure 2) and fetal biometric measurements were in agreement with the gastastional age with normal AFI. By the ultrasonographic findings, immobilized twin was accepted with a pre-diagnosis of AMC.
.
Figure 2: Fetus 1 was actively moving; fetus 2 was in stuck position (immobilized)
View Figure 2
The family was informed about the situation by multidisciplinary approach with genetic and orthopedic counselor. It was explained that even if the fetus having AMC is born, he can expose to several orthopedic surgical examination after newborn period, and it can be possible not to get the level for pursuing normal daily life even with the physical treatment procedures. After prenatal diagnosis with amniocentesis, umbilical cord clamp procedure together with fetoscope was suggested to the family for termination that fetus. However, the family decided to continuation of the pregnancy without prenatal diagnosis. Then, when communicated with the family for examining the progress of pregnancy it was understood that the patient was pre-diagnosed as twin to twin transfusion syndrome (TTTS) in external clinics and thus the fetus was terminated by laser coagulation process accompanied with ultrasonography in 20th pregnancy week, then after the process, at the 23th hour of the clinical pursuit of the patient, amniotic membrane rupture happened and the pregnancy was completely ended by complete abortus. In autopsy report; in gross fetal examination in one identical twin, fixed flexion contractures in both extremities without any other external findings and estimated gestational age based on autopsy measurements of 18 weeks were observed. In histopathologic examination, pulmoner hypoplasia and myofiber hypoplasia in muscles were observed with normal myelination of nerves. Other abdominal organs and brain were also in normal position and sizes consistent with gestational age. The other identical twin was estimated in 20th gestasyonel age with no congenital or structural anomalies based on autopsy measurements. The plasental gross and histopathologic examination was normal.
Discussion
AMC is a developmental deformation that is characterized with several joint contructures [1]. However, although joint contructures are considered as the common ultrasonographic findings for AMC cases, these findings were determined as clinical findings rather than certain diagnosis [7]. By this time, the confession of missing the diagnosis of arthrogryposis is useful since 75% of cases of arthrogryposis are missed, so care should be taken when examing ultrasound and the diagnosis [7].
In AMC cases, when the other ultrasonographic findings are examined, immobilization, abnormal position, cerebral ventriculomegali, dismorphic findings, growth retardation, increased nuchal translucency, scoliosis, cystic hygroma, small chest, thin ribs can be observed [8]. These findings observed by ultrasonography should be carefully evaluated.
The connection of AMC cases with other trisomy cases especially with trisomy 18 (Edwards� syndrome) is present [5,9]. Edwards� syndrome is the most abundant trisomy syndrome after Down syndrome, that show major abnormalities [5]. That is why, in the case of necessity, prenatal diagnosis can be done to these patients.
When etiology is examined; it is seen that the factors especially muscular (muscular dystrophia, myastenia gravis disease in mother), neurologic (brain, spinal cord and peripheric nerve abnormalities), connective tissue diseases (distrophic displasia, marfan syndrome), the cases causing intrauterine space limitation (twin pregnancy, myomas, uterus abnormalities) can cause AMC [3]. Particularly twin pregnancy out of these factors, as in our case, caused AMC by restricting intrauterine space.
Amyoplasia is the most frequent form of AMC and has a markedly increased occurrence in one of the monozygotic twins [10,11]. The another issue that is related to the AMC cases seen in twin pregnancy is the diagnosis complication by TTTS. In our case, the patient pursued with AMC diagnosis, was pre-diagnosed as TTTS in external clinics and thus one of the twins was terminated. That is why, we would like to mention about some strategies for avoiding misdiagnosis with TTTS. TTTS occurs when the blood supply of one twin moves to the other through the shared placenta. The twin that loses the blood is called the donor twin - becomes dehydrated. The twin that receives the blood is called the recipient twin - develops high blood pressure and produces too much urine and over fills the amniotic sac (polyhydramnios) [12]. On the other hand, general findings such as discordant amniotic fluid volume and abnormalities in fetal Doppler flow patterns could be observed via ultrasound in TTTS [13]. Through these abnormalities observed by Doppler flow patterns, it can be determined that the donor twin can become smaller and immobile [12]. However, since the ultrasonographic findings were not encountered for explaining TTTS case in our first evaluation of the case, we kept away from TTTS diagnosis.
In conclusion, AMC is a multifactorial disease that is characterized with multiple joint contructures in more than one area of the human body that causes fetal morbidity, mortality and economic burden in postnatal period. A broad range of counseling should be given to parents with pregnancies complicated by AMC including natural history of the disease, as well as management options and their risks and benefits. In addition, because of the similarity of AMC cases particularly seen in twin pregnancy with TTTS, the patients should be evaluated carefully and the symptomatology of TTTS should be known.
Acknowledgements
Written consent was obtained from the patient and her husband for publication of this case report.
Disclosure Statement
Presented at Fetus as a Patient 2014, 30th Anniversary Congress St. Stefan / Budva, Montenegro as a oral presentation.
References
-
Lowry RB, Sibbald B, Bedard T, Hall JG (2010) Prevalence of multiple congenital contractures including arthrogryposis multiplex congenita in Alberta, Canada, and a strategy for classification and coding. Birth Defects Res A Clin Mol Teratol 88: 1057-1061.
-
Hall JG (1997) Arthrogryposis multiplex congenita: etiology, genetics, classification, diagnostic approach and general aspects. J Pediatr Orthop B 6: 159-166.
-
Bonilla-Musoles F, Machado LE, Osborne NG (2002) Multiple congenital contractures (congenital multiple arthrogryposis). J Perinat Med 30: 99-104.
-
Hoff JM, Daltveit AK, Gilhus NE (2006) Artrogryposis multiplex congenita -- a rare fetal condition caused by maternal myasthenia gravis. Acta Neurol Scand Suppl 183: 26-27.
-
Hoff JM, Loane M, Gilhus NE, Rasmussen S, Daltveit AK (2011) Arthrogryposis multiplexa congenita: an epidemiologic study of nearly 9 million births in 24 EUROCAT registers. Eur J Obstet Gynecol Reprod Biol 159: 347-350.
-
Banker BQ (1986) Arthrogryposis multiplex congenita: spectrum of pathologic changes. Hum Pathol 17: 656-672.
-
Filges I, Hall JG (2013) Failure to identify antenatal multiple congenital contractures and fetal akinesia--proposal of guidelines to improve diagnosis. Prenat Diagn 33: 61-74.
-
Kalampokas E, Kalampokas T, Sofoudis C, Deligeoroglou E, Botsis D (2012) Diagnosing arthrogryposis multiplex congenita: a review. ISRN Obstet Gynecol 2012: 264918.
-
Naguib KK, Al-Awadi SA, Moussa MA, Bastaki L, Gouda S, et al. (1999) Trisomy 18 in Kuwait. Int J Epidemiol 28: 711-716.
-
Hall JG, Reed SD, McGillivray BC, Herrmann J, Partington MW, et al. (1983) Part II. Amyoplasia: twinning in amyoplasia--a specific type of arthrogryposis with an apparent excess of discordantly affected identical twins. Am J Med Genet 15: 591-599.
-
Hall JG, Aldinger KA, Tanaka KI (2014) Amyoplasia revisited. Am J Med Genet A 164A: 700-730.
-
Wong HS, Kidd A, Zuccollo J, Parker S, Richardson V, et al. (2009) A case of amyoplasia in a monochorionic twin pregnancy: a sequela from twin-twin transfusion syndrome? Fetal Diagn Ther 25: 31-35.
-
Society for Maternal-Fetal Medicine, Simpson LL (2013) Twin-twin transfusion syndrome. Am J Obstet Gynecol 208: 3-18.