Obstetrics and Gynaecology Cases - Reviews
Leiomyosarcoma of the Right Iliac Veins Presenting as a Pelvic Mass: A Case Report
E.Tripodi1, V. Zanfagnin1, C. Fava2, P. Zola1 and A. Ferrero1*
1Academic Division of Gynecologic Oncology, Mauriziano Hospital Turin, Italy
2Pathology Department, Mauriziano Hospital Turin, Italy
*Corresponding author: Annamaria Ferrero, Academic Division of Gynecologic Oncology, Mauriziano Hospital Turin, Largo Turati 62, 10128 Torino, Italy, Tel: +39 011 5082764, E-mail: a.ferrero@katamail.com/annamaria.ferrero@unito.it
Obstet Gynecol Cases Rev, OGCR-2-040, (Volume 2, Issue 3), Case Report; ISSN: 2377-9004
Received: May 23, 2015 | Accepted: May 27 2015 | Published: May 30, 2015
Citation: Tripodi E, Zanfagnin V, Fava C, Zola P, Ferrero A (2015) Leiomyosarcoma of the Right Iliac Vein Presenting as a Pelvic Mass: A Case Report. Obstet Gynecol Cases Rev 2:040. 10.23937/2377-9004/1410040
Copyright: © 2015 Tripodi E. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Leiomyosarcoma of the iliac veins is a very uncommon tumour. Prognosis is usually poor and the best treatment is unknown.
Case report: We report the case of a 74-year-old woman presenting a right leg oedema. Venous colour doppler was normal. Abdominal ultrasound and magnetic resonance scanning demonstrated a 70 mm mass in the right pelvis with a well-defined profile, which was not homogeneous after contrast enhancement. The lesion was in close contact with the iliac vessels and the right iliac veins profile was inside the mass. Serum markers were in the normal range. The patient underwent an exploratory laparotomy by a team of Gynecologic Oncologists for the suspicion of ovarian cancer, but a retroperitoneal tumour on the wall of the right common iliac and external iliac veins was found. With the help of a vascular surgeon the tumour was resected en bloc and polytetrafluoroethylene grafts were used to reconstruct the vessels. The postoperative course was uneventful. On histological examination a leiomyosarcoma of the iliac veins was found. The patient received adjuvant chemotherapy. Three years after surgical resection no signs of recurrence or postoperative complications were detected.
Conclusion: Leiomyosarcoma of the iliac veins is a rare option to consider in the management of a pelvic mass. Radical surgical excision with polytetrafluoroethylene grafts reconstruction followed by adjuvant chemotherapy was feasible and effective.
Keywords
Leiomyosarcoma, Pelvic mass, Iliac veins, Polytetrafluoroethylene grafts
Introduction
Leiomyosarcomas are a relatively rare group of smooth muscle soft tissue sarcomas. Leiomyosarcomas involving large blood vessels are quite unusual, comprising of less than 2% of all leiomyosarcomas [1]. Vascular leiomyosarcomas originate five times more often in arteries than in veins. Primary venous leiomyosarcomas are rare slow-growing tumours that originate from the smooth muscle tissue of vessels, usually the inferior vena cava. Since the first case reported by Perl in 1871, few cases (mostly single case reports or small series) have been described, with little information on follow-up [2]. This type of tumour has late diagnosis because of the varying clinical presentation and generally has a poor prognosis. Data on optimum treatment is limited due to the paucity of cases. However, radical surgical excision appears to offer the best chance of cure. The possible benefits of adjuvant therapy have not been proven.
We report the case of a primary leiomyosarcoma of the right iliac veins presenting as a pelvic mass.
Case Report
A 74-year-old woman presented an oedema of the right lower limb. She was not a smoker and had no risk factors for venous thrombosis.
Venous colour doppler displayed no signs of deep veins thrombosis. Abdominal ultrasound showed a hypo-anechoic image of 46x45mm at the level of the uterus, in the right paramedian position of the pelvis. Magnetic resonance imaging of the inferior abdomen and pelvis showed a 70mm mass localised at the right side of the pelvic cavity with a well-defined but irregular profile. At contrast enhancement the mass impregnation was not homogeneous. The lesion was in close contact with the iliac vessels with an apparent greater involvement of the right iliac veins that presented themselves as incorporated in the context of the mass. A modest extrinsic compression of the iliac muscle was observed, but the lesion seemed to be cleavable. The radiologists hypothesized an adnexal tumour, so CT/MR angiogram was not performed. The patient also underwent a computerised tomography of the thorax and upper abdomen as preoperative staging: metastatic lesions were not found. Laboratory findings, including the serum concentration of the oncologic markers (Ca125, Ca15.3, CEA and Ca19.9), were in the normal range.
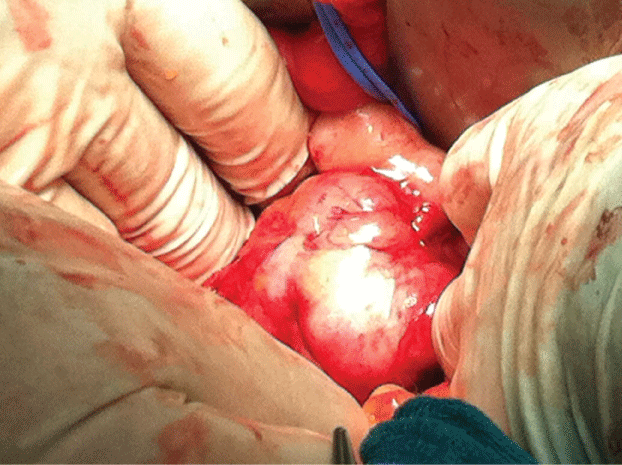
The patient underwent an exploratory laparotomy by a team of Gynecologic Oncologists for the suspicion of ovarian cancer. At the exploration of the abdominal cavity both the uterus and adnexi were regular and no adnexal masses had been detected. A large retroperitoneal tumour on the wall of the right common iliac and external iliac veins was found (Figure 1). With the help of a vascular surgeon they proceeded to separate the right iliac vessels (common iliac, external iliac and internal iliac veins). Then they isolated and removed the mass, which was well encapsulated and dissociable from the surrounding plans (Figure 2). At frozen section examination a leiomyosarcoma of the common and external iliac veins was detected. Polytetrafluoroethylene grafts were used to reconstruct the vessels.
.
Figure 1: Intraoperative finding: a large retroperitoneal tumor adherent to the right iliac vessels.
View Figure 1
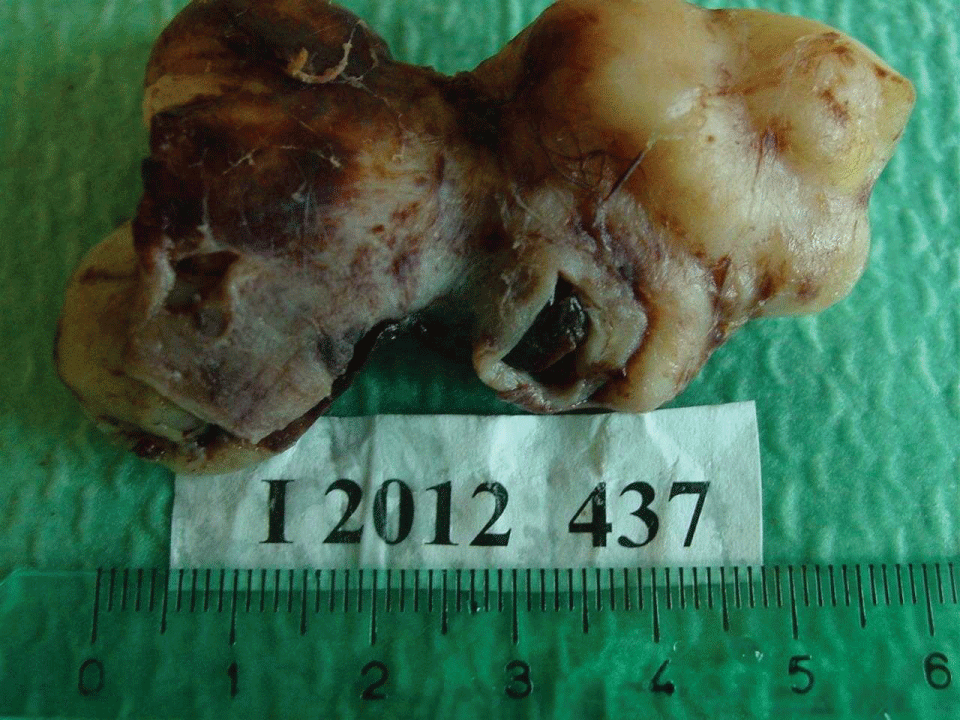
.
Figure 2: The resected specimen: a segment of the iliac veins wall excised en bloc with the tumor.
View Figure 2
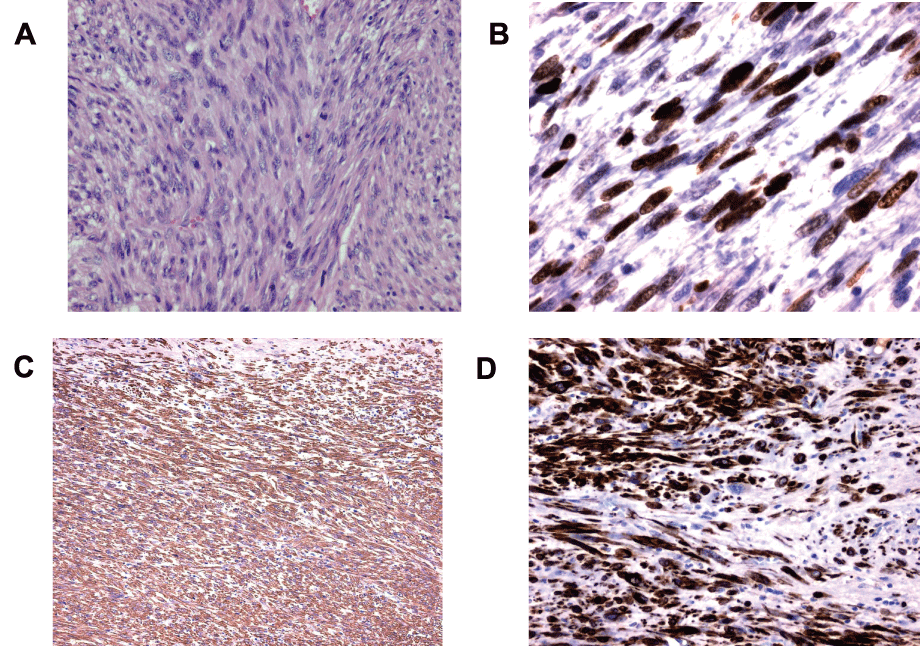
Post-surgery evaluation of the pathology specimen confirmed a leiomyosarcoma originating from the right iliac veins, positive for actin and desmin at immunochemistry (Figure 3A-3D). The lesion was 7,2cm large, and grade 3 according FNCLCC (score 7). Lymphovascular space involvement and perineural invasion were negative. Resection margins were free from tumour.
.
Figure 3: Pathological features. A: proliferation of atypical spindle cells with elongated, blunt-ended, or cigar-shaped nuclei and densely eosinophilic cytoplasm arranged in interlacing bundles, admixed with scattered bizarre cells and mitotic figures (H&E, �20). B: high expression of Ki-67 (x40). C: strong reactivity for smooth muscle actin (�10). D: strong reactivity for desmin (x20).
View Figure 3
The patient tolerated the surgery well and had an uneventful recovery. Venous thrombus-embolic prophylaxis with low molecular weight heparin was performed (6000 UI twice a day).
It was considered greater the risk of distant relapse than local recurrence, so she received three cycles of adjuvant treatment with Epirubicin (50mg/mq) and Ifosfamide (1800mg/mq in 5 days).
The patient undergoes lower limb venous colour doppler and clinical examinations every six months. Three years from surgery she has no recurrence and remains without signs of lower extremity venous congestion. Polytetrafluoroethylene grafts are patent.
Discussion
Leiomyosarcomas represent 10% to 15% of connective tissue sarcomas, 45% of retroperitoneal tumours [3] and 0.5% of sarcomas in adults [4]. Primary veins leiomyosarcoma is a rare type of vascular sarcoma that arises from the spindle cells of the venous wall; growth pattern may progress from intramural to endoluminal, extraluminal, or mixed forms [5]. Approximately half of primary venous leiomyosarcomas originate in the inferior vena cava [6]. Less frequently, great saphenous veins (25%), femoral veins, internal jugular veins, and iliac veins involvement have been reported [7]. Primary venous leiomyosarcoma of the inferior vena cava is more frequent in women in their sixth decade [7] although reports of younger patients are found [8]. Pathological classification follows retroperitoneal leiomyosarcoma criteria based upon mitotic figure count [9]. There are less than 250 cases reported to date, with a 60 % 5 year overall survival rate [10].
Clinical presentation is usually aspecific and physical examination yields normal findings. Thus, its diagnosis is frequently overlooked. However, at time of diagnosis, more than one half of the cases already present pulmonary metastases [11]. When symptoms are present, they depend on the location, size and growth rate. Acute venous thrombosis is the most common presentation of the iliac veins leiomyosarcoma. Other symptoms may occur due to compression of the iliac artery and pelvic organs. Primary venous leiomyosarcomas are clinically divided into non-occlusive, occlusive or terminal [12]. Other frequent clinical presentations include abdominal pain [13], consumptive symptoms (loss of weight, anorexia, or asthenia), fever, night sweats, nausea, vomiting, and dyspnoea [14]. On physical examination an abdominal mass may be detected. Other less frequent presentations include haematuria [15], a renal mass [16], or a cardiac tumour [17]. In most cases, the tumours are diagnosed in the occlusive stage. In our case, the patient had only an aspecific like symptom as oedema of the right lower limb, so it was difficult to reach the correct diagnosis. Preoperative imaging techniques were not definitive in identifying the origin of the mass in our patient.
Although hematogenous spread commonly leads to secondary deposits in the lung, liver, and brain in primary venous leiomyosarcoma and in later stages, lymphatic pathways may be involved in metastisation [18]; in our patient no metastatic lesions have been found.
Due to the limited cases of primary venous leiomyosarcoma, optimal treatment is yet to be established [19]. However, an aggressive surgical approach assuring a free margin en bloc tumour resection can be curative [19] despite reported local recurrence rates in selected cases of 40 to 60% [17]. Our patient underwent radical surgery and 3 years after, the local response is excellent.
The tumour may present difficulty of vascular reconstruction after en block resection. [20,21] The controversy in these types of cases was whether to reconstruct the iliac veins and how it could be done. The veins can be managed with primary repair, ligation, or prosthetic graft. The current published data suggests a high rate of polytetrafluoroethylene graft occlusion, with a patency of 62% at 3 years reported by Jost and 60% at 12 months in case series by Caldarelli [22,23]. At the same time, patency of the autologous veins graft appears to be higher [22]. Postoperative morbidity such as leg oedema with pain and tenderness, ulcerative sequelae, and venous claudication has been documented in a number of cases [21,23]. Reconstruction using a polytetrafluoroethylene graft can be indicated to bridge wide gaps in the veins, but clinical outcomes with prosthetic grafts in peripheral vascular reconstruction are inferior to those with autologous veins bypass grafts, in part because of anastomotic neointimal hyperplasia. Polytetrafluoroethylene grafts were used to reconstruct the vessels in our case, the patient had no postoperative complications and after 3 years there are no signs of obstruction or evidence of neointimal hyperplasia.
The role of chemotherapy and radiation therapy for all retroperitoneal sarcomas in general and for venous sarcoma in particular is not clear [24]. In our case the patient received 3 cycles of chemotherapy with Epirubicin (50mg/mq) and Ifosfamide (1800mg/m in 5 days), the treatment was well tolerated with no toxicity greater than grade 2.
Patients with primary venous leiomyosarcoma have a mean survival of 3.5 years, and a favourable outcome relies greatly upon eligibility and achievement of a free-margin resection [25], as has been achieved in the patient that we treated at our centre. Comparatively to other sarcomas, primary venous leiomyosarcoma has a shorter metastases free interval and survival [26].
Conclusion
Primary malignant tumours of vascular origin are rare. Leiomyosarcoma of the iliac veins is a rare option to consider in the management of a pelvic mass and is important to know in the differential diagnosis of gynecologic pelvic diseases. A mass causing venous stasis, with oedema, swelling, or thrombosis of the lower limbs, is frequently the manifestation of a leiomyosarcoma of the iliac veins. Preoperative diagnostic procedures may not always successfully identify the origin. Therefore, definitive diagnosis can only be possible with surgery and subsequent histopathologic examination.
Optimal treatment strategies are unclear. Complete surgical resection with negative margins offers the only chance of long-term survival [24]. The reported case concerns a leiomyosarcoma of the right iliac veins with extraluminal growth. Radical surgical excision of the lesion with polytetrafluoroethylene grafts to reconstruct the vessels and adjuvant chemotherapy allowed our patient to have three year without recurrence.
References
-
Le Minh T, Cazaban D, Michaud J, Ginestet-Auge MC, Laporte MH, et al. (2004) Great saphenous veins leiomyosarcoma: a rare malignant tumor of the extremity--two case reports. Ann Vasc Surg 18: 234-236.
-
Prandi M, Scabini S, Taviani MP (2001) An extraluminal leiomyosarcoma of the iliac veins without thrombosis--a case report. Vasc Surg 35: 311-314.
-
Gurleyik G, Aktekin A, Arman A, Muftuoglu T, Saglam A (2005) Leiomyosarcoma of the inferior vena cava: report of a case. Indian Journal of Surgery 67: 320-322.
-
Laskin WB, Fanburg-Smith JC, Burke AP, Kraszewska E, Fetsch JF, et al. (2010) "Leiomyosarcoma of the inferior vena cava: clinicopathologic study of 40 cases. American Journal of Surgical Pathology 34: 873- 881.
-
Ceyhan M, Danaci M, Elmali M, Ozmen Z (2007) Leiomyosarcoma of the inferior vena cava. Diagn Interv Radiol 13: 140-143.
-
Hilliard NJ, Heslin MJ, Castro CY (2005) Leiomyosarcoma of the inferior vena cava: three case reports and review of the literature. Ann Diagn Pathol 9: 259-266.
-
Fischer MG, Gelb AM, Nussbaum M, Haveson S, Ghali V (1982) Primary smooth muscle tumors of venous origin. Ann Surg 196: 720-724.
-
Hines OJ, Nelson S, Quinones-Baldrich WJ, Eilber FR (1999) Leiomyosarcoma of the inferior vena cava: prognosis and comparison with leiomyosarcoma of other anatomic sites. Cancer 85: 1077-1083.
-
Tameo MN, Calligaro KD, Antin L, Dougherty MJ (2010) Primary leiomyosarcoma of the inferior vena cava: reports of infrarenal and suprahepatic caval involvement. J Vasc Surg 51: 221-224.
-
Cocieru A, Dietzek A, Saldinger PF (2010) Internal Iliac Vein Transposition for Vascular reconstruction after resection of an external iliac veins leiomyosarcoma. Ann Vasc Surg 24: 693.e9-10.
-
da Gama AD, Cabral G, Ministro A, Evangelista A, Dami�ao A, et al. (2009) Leiomyosarcoma of the superficial femoral veins. Case report. Revista Portuguesa de Cirurgia Cardio-Tor�acica e Vascular 16: 97-101.
-
Valverde FM, Ramos MJ, Torregrosa N, Molto M, Rojas JL (2009) Leiomyosarcoma of the iliac veins," Ann Vasc Surg 23: 536.e5-536.e8.
-
Kieffer E, Alaoui M, Piette JC, Cacoub P, Chiche L (2006) Leiomyosarcoma of the inferior vena cava: experience in 22 cases. Ann Surg 244: 289-295.
-
Abisi S, Morris-Stiff GJ, Scott-Coombes D, Williams IM, Douglas-Jones AG, et al. (2006) Leiomyosarcoma of the inferior vena cava: clinical experience with four cases. World J Surg Oncol 4: 1.
-
Lang EK, Rudman E, Colon I, Macchia RJ (2009) Hematuria: the presenting symptom of an angiosarcoma of the inferior vena cava. J Urol 182: 2470.
-
Shvarts O, Han KR, Lam JS, Belldegrun AS (2004) Primary leiomyosarcoma of the inferior vena cava presenting as a renal mass. Rev Urol 6: 39-42.
-
Fonseca N, Silvestre I, Bernardino L, Augusto S, Ferreira M, et al. (2002) Leiomiossarcoma da Veia Cava Inferior a prop�osito de um caso cl�inico muito raro. Rev Port Cardiol 21: 1469-1478.
-
Ahluwalia A, Saggar K, Sandhu P, Gupta K (2002) Primary leiomyosarcoma of inferior vena cava: an unusual entity," Indian Journal of Radiology and Imaging 12: 515-516.
-
Reddy VP, VanVeldhuizen PJ, Muehlebach GF, Dusing RW, Birkbeck JP, et al. (2010) Leiomyosarcoma of the inferior vena cava: a case report and review of the literature. Cases Journal 3: 71.
-
Valverde FM, Ramos MJ, Torregrosa N, Molto M, Rojas JL (2009) Leiomyosarcoma of the iliac veins. Ann Vasc Surg 23: 536.
-
Fung TM, Wong WS, Lam YH, Lau JY (2005) Resection of leiomyosarcoma arising from the iliac veins. J Am Coll Surg 200: 136-137.
-
Jost CJ, Gloviczki P, Cherry KJ Jr, McKusick MA, Harmsen WS, et al. (2001) Surgical reconstruction of iliofemoral veinss and the inferior vena cava for nonmalignant occlusive disease. J Vasc Surg 33: 320-327.
-
Caldarelli G, Minervini A, Guerra M, Bonari G, Caldarelli C, et al. (2002) Prosthetic replacement of the inferior vena cava and the iliofemoral veins for urologically related malignancies. BJU Int 90: 368-374.
-
Mingoli A, Cavallaro A, Sapienza P, Di Marzo L, Feldhaus RJ, et al. (1996) International registry of inferior vena cava leiomyosarcoma: analysis of a world series on 218 patients. Anticancer Res 16: 3201-3205.
-
Dzsinich C, Gloviczki P, van Heerden JA, Nagorney DM, Pairolero PC, et al. (1992) Primary venous leiomyosarcoma: a rare but lethal disease. J Vasc Surg 15: 595-603.
-
Italiano A, Toulmonde M, Stoeckle E, Kind M, Kantor G, et al. (2010) Clinical outcome of leiomyosarcomas of vascular origin: comparison with leiomyosarcomas of other origin. Ann Oncol 21: 1915-1921.





